Abstract
The concept of oral health-related quality of life (OHRQoL) delineates how oral outcomes impact on an individual’s physical, psychological, and social functioning and hence overall quality of life. It explains how compromised oral health can negatively impact on quality of life through impairing daily activities, social interactions, and self-esteem. Factors that contribute to OHRQoL are in the areas of: oral health (mostly tooth loss, periodontal disease, and pain), general health (especially chronic conditions and cognitive impairments causing deficient oral health behaviour), personal traits (including the ability to cope and adapt), demographic factors (age, gender, socioeconomic status, ethnicity, culture), social (support, integration), and environmental factors (lifestyle, place of residence). In order to assess OHRQoL outcomes, a number of specific instruments, mostly questionnaires, have been developed.
Medical practitioners can make a major contribution towards improvement of OHRQoL and thereby the overall quality of life of their patients, and the public at large, through including oral health-related questions in holistic medical assessments, promotion of good oral hygiene practices, and increasing the awareness of the importance of good oral health to maintaining overall quality of life.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
FormalPara Learning ObjectivesAfter reading this chapter, readers should be able to:
-
Understand the concept of oral health-related quality of life.
-
State the dimensions measured in different methods of measuring oral health-related quality of life.
-
Argue on the importance of good oral health in maintaining overall quality of life.
6.1 OHRQoL: The Concept, Its Relation to General Health, Assessment
Quality of life (QoL) is defined as ‘an individual’s perception of their position in life in the context of the culture and value systems in which they live and in relation to their goals, expectations, standards, and concerns’ [1]. As such, QoL is closely related to well-being [2], and is both multidisciplinary and subjective in nature. QoL is affected through complex interactions between an individual’s physical and psychological health, personal beliefs, social relationships, and their environment, and can only be understood from a personal perspective. This can help to explain why persons with similar health status can have different QoL perspectives based on differing experiences, expectations, and perceptions.
Oral health is understood to be integral to both general health and quality of life [3]. As such, the concept of oral health-related QoL (OHRQoL) delineates how oral outcomes impact on an individual’s overall QoL. Many definitions of OHRQoL have been suggested since Locker first described the concept and illustrated the pathways involved [4, 5]. This description captured all of the important aspects of oral health which contribute to QoL including function (chewing, biting, speaking, swallowing), psychological factors (aesthetics, self-esteem, appearance), social factors (relating to interactions with others), and the experience of pain and discomfort. A recent definition by the FDI World Dental Federation closely reflects the dynamic, multidimensional, and subjective nature of the concept: ‘OHRQoL is a multidimensional construct that reflects (among other things) people’s comfort when eating, sleeping and engaging in social interaction; their self-esteem; and their satisfaction, with respect to their oral health’ [6].
In the last two decades, the concept of OHRQoL has helped to shift the emphasis of clinicians and researchers from purely focusing on objective measures of oral health to adopting a more holistic and patient-centred approach. It acknowledges that the ultimate goal of dental care, good oral health, is not the mere absence of oral disease or disorders. Although these clinical oral outcomes remain relevant, the experienced functional, psychological, and social impacts of oral outcomes on a person’s QoL are arguably more important. This is especially true in an era where a patient’s values, preferences, and context play a central role in clinical decision-making and where personalized healthcare is the dominant healthcare paradigm [7, 8]. Thus, OHRQoL outcomes are vital not only to the delivery of oral healthcare, but also to shape oral health promotion and prevention programmes, allocate resources, develop oral health policies, and organize oral healthcare. Documented uses of OHRQoL outcomes are listed in Table 6.1.
In aspects of healthcare, a series of Patient Reported Outcome Measures (PROMs) have been developed to measure outcomes which matter to patients. In order to assess OHRQoL outcomes, a number of specific instruments have also been developed. These instruments utilize a variety of methodologies, of which the self-administered individual questionnaire is the most popular [10]. Table 6.2 lists the most often used questionnaires and their characteristics. Although such questionnaires differ in underlying theory, focus, and length they all attempt to capture the constituent elements of OHRQoL (functional, psychological, social, pain/discomfort). It is important to note that the way in which these factors contribute to an individual’s OHRQoL depends on the person, the situation, and the interaction between that person and the situation. These relationships are dynamic and can change significantly over time, in particular when patients become frail or care dependent [12], as demonstrated through the case of ‘Mrs. Brown’.
Case. Mrs. Brown
Mrs. Brown has always cared a lot about her appearance, as shown through her immaculate clothing, well-manicured fingers, well-groomed hairstyle, and neat facial make-up. She has always visited the dentist twice a year and her oral self-care has always been perfect. At the age of 82, she still has all of her natural teeth. However, she has progressive Parkinson’s disease. Her joints are increasingly painful and have started to impede her dexterity. Handling a toothbrush is increasingly difficult for her. Since she is aware that her toothbrushing efforts are not effective, she has decided—also because she feels tired almost throughout the day—to give up brushing. As a result, she develops a number of carious lesions and ends up losing five teeth in 6 months’ time. Now, several scenarios are possible, e.g.:
-
(a)
She cannot bite hard food anymore and she minds—her OHRQoL is negatively affected in the oral function domain.
-
(b)
She does not mind her oral functions, but cares a lot about her mutilated dentition, she hates the ways she looks now and does not dare to go out anymore (her OHRQoL is negatively affected in the psychological and social domain)
-
(c)
She adapts to the new situation by eating only soft foods and not looking in the mirror anymore—impacts on her OHRQoL are nil.
-
(d)
She decides to have her teeth replaced by full dental prostheses and adapts to wearing these; she likes the look of her new teeth even more than her natural teeth and is satisfied with the oral functions—impacts on her OHRQoL are positive.
Reported OHRQoL outcomes of older people almost exclusively result from quantitative surveys which utilize the questionnaires in Table 6.2. One major drawback of these OHRQoL questionnaires is that they generally only measure negative oral health impacts without considering the potentially positive or neutral experiences of such negative oral impacts. For instance, not all patients are concerned that they cannot bite an apple because of loose teeth. Such a response could be a result of coping and adaptation [13, 14] and altered health expectations in old age [15]. These neutral or positive responses to negative QoL impacts could help to clarify the discrepancy between self-rated oral health status and related OHRQoL found in older people [15,16,17]. In this light, it is important to notice that existing evidence on the associations between OHRQoL and oral health of older people is controversial, with several studies indicating that the OHRQoL remains stable or even improves despite decreasing oral health [15,16,17,18,19], while others show a negative effect of decreasing OH on OHRQoL [20,21,22,23].
Since OHRQoL is highly dependent on a context that is rapidly changing in old age, this context should be queried by care providers and researchers, ideally through open questions (e.g. What is important to you in life? What activities do contribute to your well-being? How does your oral health support or impede engagement in such activities?), and possibly in addition to OHRQoL self-administered questionnaires. Such questioning can also help to identify older people who do not prioritize oral health, thus enabling appropriate preventative and educational regimes to be implemented.
6.2 Factors Contributing to OHRQoL
Since the development of the first OHRQoL instruments, hundreds of studies have assessed the factors that contribute to OHRQoL. These factors can be divided into several categories: oral health, general health, personal traits, demographic factors, and social and environmental factors. Which factors have the strongest predictive value depends primarily on characteristics of the target population and, to a lesser extent, to the used instruments. In older populations, oral health factors often appear to have relatively less predictive value than, for instance, social factors and personal traits. Moreover, none of the factors associated with OHRQoL are evidenced consistently in scientific studies, nor are their effects consistent across similar populations and, at individual and population level, over time.
Oral health: A systematic review and meta-analysis has indicated that loss of natural teeth is directly and negatively associated with OHRQoL [24]. Analysed evidence was derived from all parts of the world, including Europe, North and Southern America, Southeast Asia (China, Japan, South Korea, Sri Lanka), and Africa (Tanzania). This review included a study from Finland which used nationally representative population datasets to explore the relationship between age, tooth loss, and OHRQoL. The authors reported that age and tooth loss are closely associated, but have independent effects on OHRQoL [25]. Tooth loss (which is associated with increasing age) is associated with more negative impacts, while increasing age independently results in fewer. In all of the populations and sub-populations studied, a complete or almost complete natural dentition was associated with the best OHRQoL.
Tooth loss not only impairs chewing functions, speech, and appearance, it also negatively affects people’s self-worth, e.g. by hampering a person’s sense of intactness and pride, as well as interpersonal relationships [26]. Prosthodontic replacement of missing teeth can also impact on OHRQoL, with a generally positive impact reported for fixed prostheses [27] compared with mixed impacts for removable prostheses (Figs. 6.1, 6.2, 6.3, and 6.4). In older people ill- or loose fitting removable prostheses are often a source of pain and discomfort [28] and can severely impact OHRQoL. This point has been illustrated in work carried out by McKenna et al. who demonstrated significantly improved OHRQoL outcomes for partially dentate older patients restored to shortened dental arches (a specific type of a dentition with a reduced number of posterior teeth, often called functional dentition) with fixed prostheses compared to removable partial dentures (Figs. 6.3 and 6.4) [29]. A decreased number of teeth, as well as ill-fitting tooth replacements, lead to reduced chewing ability which in turn can result in a preference for foods that are softer and easier to chew. Typically, such foods are relatively low in nutrients and high in calories and complex carbohydrates [30], and hence induce poor nutritional status and subsequent health. It should thereby be noted that adequate masticatory function is a prerequisite but not sufficient condition for good nutrient intake [31]. Poor eating behaviour of the elderly people is also influenced by personal and contextual factors, such as depression, physical illness, tastiness of served meals, and social context (detailed discussion in Chap. 5).
A recent systematic review showed that periodontal diseases also seem to be associated with worse OHRQoL, with severe periodontitis exerting the most significant impact by compromising aspects related to oral function and aesthetics [32]. Evidence was derived from over 20 countries worldwide, including Brazil, the UK, the USA, Australia, India, China, Jordan, and Nigeria. The same review showed that gingivitis (inflammation of the gums) was associated with pain, discomfort, and with difficulties performing oral hygiene and wearing dentures.
Other oral health factors that are associated with OHRQoL, mostly through pain and discomfort or affecting appearance, are toothache, fractured or damaged teeth, oral cancer, mucositis, and xerostomia [33]. Caries, which is the most prevalent oral disease, eventually leading to tooth destruction, and tooth loss, is often unnoticed by the patient, and has therefore no or little impact on OHRQoL until it becomes severe and causes pain or discomfort. This illustrates why regular and systematic oral health assessments by care providers (dental and non-dental staff) are vitally important to detect carious lesions before they become symptomatic and potentially difficult to manage.
General health: Despite considerable evidence for significant associations between oral and systemic health conditions, evidence on associations between impaired general health and oral health-related quality of life (OHRQoL) offer contradicting results. For instance, Jensen et al. [34] found no association between OHRQoL and performance in activities of daily living (ADL), while Miura et al. [35] found a significant positive association between OHRQoL and ADL, especially communication. Ostberg et al. [36] showed that OHRQoL was significantly associated with self-rated general health and self-rated mental health, but not with self-rated physical health, whereas Hassel et al. [37] found a significant inverse association between physical pain and OHRQoL. Similar inconsistent findings have resulted from research on the associations between general health and quality of life. Clearly, the associations between impaired health, OH and OHRQoL are complex. Yet, evidence on links between impaired general health and disadvantageous oral health behaviour (oral self-care (e.g. toothbrushing) and dental service use) is less controversial: people with chronic conditions, pain, impaired dexterity or mobility, low energy, depression, and especially with impaired cognitive functions, show worse oral healthcare behaviour than healthy persons [38,39,40,41,42], with a proven negative effect on their oral health (e.g. [42]).
Personal, demographic, social, and environmental factors: As populations age and lose teeth, their quality of life may be expected to change, particularly with respect to the way that their oral condition impacts on day-to-day activities. This may happen as a direct result of altered function due to tooth loss, but possibly also as a result of changes in perceptions and values that occur with increasing age. Evidence has shown that experience of oral diseases has a more significant impact on subjective oral health when it occurs early in adulthood rather than in old age [16]. Other factors which may mediate the relationship between OH and QoL are personal traits, health beliefs, demographic factors, social and environmental factors. Personal traits include coping and adaptation ability, locus of control (the degree to which people believe that they have control over the outcome of events in their lives), self-efficacy (the degree to which people believe they can succeed in a specific situation or accomplish a task), neuroticism, extraversion, and optimism [43,44,45,46,47,48]. The fact that the above factors mitigate OHRQoL is, for instance, explained by the need for older people to adapt as an integral part of successful ageing and a means of coping with the impact of oral disorders, and by balancing gains and losses, adjusting expectations, and seeking social support [49, 50].
Demographic factors that have been shown to positively impact OHRQoL include higher age, being male, ethnicity (e.g. not belonging to ethnic minorities and being of Caucasian origin), higher socioeconomic status, and residing in an urban environment (e.g. [12, 42]).
Social and environmental factors include social and lifestyle factors. More social support and a higher degree of social integration have been proven to increase OHRQoL [51, 52].
In general, social determinants of health (being ‘the conditions in which people are born, grow, work, live, and age, and the wider set of forces and systems shaping the conditions of daily life like economic policies and systems, development agendas, social norms, social policies and political systems’ (www.who.int/social_determinants/en/)), influence both oral health and OHRQoL throughout the life-course [53]. Improving OHRQoL therefore would ideally involve multifactorial life-course interventions. In any case, interventions aiming at (general) health promotion, development of positive health beliefs, and better access to healthcare from early childhood onwards, will also benefit OHRQoL. Therefore, oral health prevention and promotion should be a priority for all members of the care team (dental and non-dental members of staff).
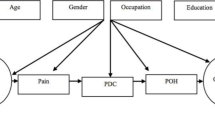
Figure 6.5 delineates the associations between evidenced factors and OHRQoL, and the mediating role of non-oral health factors (in the purple rectangle) on the links between oral impairments, experienced oral effects, and impacts on daily performance. To illustrate the tentative nature of associations and controversies about direction of found relations between the above factors, lines are dotted, and some lines double-arrowed.
Theorized pathways affecting OHRQoL. Dotted lines symbolize an evidenced possible effect. The model left from the purple rectangle is a modified version of the model from the WHO International Classification of Impairments, Disabilities, and Handicaps amended for dentistry [54]
6.3 Implications for Healthcare Practice
As demonstrated in this chapter, there are numerous ways that oral health can have significant impacts on quality of life. Moreover, poor oral health may be underreported by the older patients for the reasons previously explained. All members of the healthcare team should be aware of these threats and implications and strive to promote and deliver care which preserves and improves oral health-related quality of life.
Given that poor oral health has negative impacts on quality of life, it is essential that every effort is made to regularly evaluate oral health status and prevent chronic dental diseases and ultimately natural tooth loss. Dental care for older patients should have a preventative focus with attention given to clear and achievable messages. Where patients are dependent, these messages should be shared with carers and family members. Preventative advice should be tailored to take into account individual patients’ needs with adaptation of oral hygiene tools suggested for those with physical limitations. This advice should be emphasized regularly and checked to ensure understanding and implementation.
6.4 Conclusion
Regardless of the definition of OHRQoL, it is clear that oral conditions can have varied impacts on daily living and that the patients’ perceptions about their oral health and related QoL are significant in clinical practice and patient management. The extent of these impacts could be assessed by OHRQoL assessments, wherein standardized, validated instruments should ideally be complemented by open questions. Such assessments can be appropriately incorporated into oral healthcare practices, but also in general healthcare, e.g. through inclusion of such questions in comprehensive geriatric or medical assessments. As such, healthcare professionals play an important role in enhancing the OHRQoL, and thereby QoL of their patients and the public at large.
The importance of assessing both patients’ perceptions of health and presence or absence of disease lies in the need to have accurate data to promote health, disease prevention programmes, and for allocation of health resources. Furthermore, as patients’ assessment of their health-related quality of life is often markedly different to the opinion of healthcare professionals, patient assessment of healthcare interventions is warranted.
References
World Health Organization. WHOQOL: measuring quality of life. https://www.who.int/healthinfo/survey/whoqol-qualityoflife/en/.
Skevington SM, Bohnke JR. How is subjective well-being related to quality of life? Do we need two concepts and both measures? Soc Sci Med. 2018;206:22–30.
Baiju RM, Peter E, Varghese NO, Sivaram R. Oral health and quality of life: current concepts. J Clin Diagn Res. 2017;11(6):Ze21–ze26.
Locker D. Concepts of oral health, disease and the quality of life. In: Measuring oral health and quality of life. Chapel-Hill: Department of Dental Ecology, University of North Carolina; 1996.
Sischo L, Broder HL. Oral health-related quality of life: what, why, how, and future implications. J Dent Res. 2011;90(11):1264–70.
FDI World Dental Federation, Oral health and quality of life. https://www.fdiworlddental.org/resources/policy-statements-and-resolutions/oral-health-and-quality-of-life.
Blobel B, Ruotsalainen P. Healthcare transformation towards personalized medicine—chances and challenges. Stud Health Technol Inform. 2019;261:3–21.
Annadurai K, Danasekaran R, Mani G. Personalized medicine: a paradigm shift towards promising health care. J Pharm Bioallied Sci. 2016;8(1):77–8.
Fitzpatrick R, Fletcher A, Gore D, Spiegelhalter D, Cox D. Quality of life measures in health care. I: application and issues in assessment. Br Med J. 1992;305:1074–7.
Abreu LG. An overview of oral health related quality of life. Oral Health Case Rep. 2015;1:e105.
Bennadi D, Reddy CV. Oral health related quality of life. J Int Soc Prev Community Dent. 2013;3(1):1–6.
Niesten D. Oral health care and oral health-related quality of life of frail and care-dependent older people, in medicine. Radboud University Nijmegen: Nijmegen; 2017.
Allison PJ, Locker D, Feine JS. Quality of life: a dynamic construct. Soc Sci Med. 1997;45(2):221–30.
von Faber M, Bootsma-van der Wiel A, van Exel E, Gussekloo J, Lagaay AM, van Dongen E, et al. Successful aging in the oldest old: who can be characterized as successfully aged? Arch Intern Med. 2001;161(22):2694–700.
Locker D, Gibson B. Discrepancies between self-ratings of and satisfaction with oral health in two older adult populations. Community Dent Oral Epidemiol. 2005;33(4):280–8.
Slade GD, Sanders AE. The paradox of better subjective oral health in older age. J Dent Res. 2011;90(11):1279–85.
Steele JG, Sanders AE, Slade GD, Allen PF, Lahti S, Nuttall N, et al. How do age and tooth loss affect oral health impacts and quality of life? A study comparing two national samples. Community Dent Oral Epidemiol. 2004;32(2):107–14.
Sanders AE, Slade GD, Lim S, Reisine ST. Impact of oral disease on quality of life in the US and Australian populations. Community Dent Oral Epidemiol. 2009;37(2):171–81.
Dahl KE, Wang NJ, Skau I, Ohrn K. Oral health-related quality of life and associated factors in Norwegian adults. Acta Odontol Scand. 2011;69(4):208–14.
Petersen PE, Kandelman D, Arpin S, Ogawa H. Global oral health of older people—call for public health action. Community Dent Health. 2010;27(4 Suppl 2):257–67.
Ettinger RL. Oral health and the aging population. J Am Dent Assoc. 2007;138(Suppl):5S–6S.
Locker D, Clarke M, Payne B. Self-perceived oral health status, psychological well-being, and life satisfaction in an older adult population. J Dent Res. 2000;79(4):970–5.
MacEntee MI. Missing links in oral health care for frail elderly people. J Can Dent Assoc. 2006;72(5):421–5.
Gerritsen AE, Allen PF, Witter DJ, Bronkhorst EM, Creugers NH. Tooth loss and oral health-related quality of life: a systematic review and meta-analysis. Health Qual Life Outcomes. 2010;8:126.
Lahti S, Suominen-Taipale L, Hausen H. Oral health impacts among adults in Finland: competing effects of age, number of teeth, and removable dentures. Eur J Oral Sci. 2008;116(3):260–6.
Niesten D, van Mourik K, van der Sanden W. The impact of having natural teeth on the QoL of frail dentulous older people. A qualitative study. BMC Public Health. 2012;12:839.
Ali Z, Baker SR, Shahrbaf S, Martin N, Vettore MV. Oral health-related quality of life after prosthodontic treatment for patients with partial edentulism: a systematic review and meta-analysis. J Prosthet Dent. 2019;121(1):59–68.e3.
MacEntee MI, Hole R, Stolar E. The significance of the mouth in old age. Soc Sci Med. 1997;45(9):1449–58.
McKenna G, Allen PF, Hayes M, DaMata C, Moore C, Cronin M. Impact of oral rehabilitation on the quality of life of partially dentate elders in a randomised controlled clinical trial: 2 year follow-up. PLoS One. 2018;13(10):e0203349.
Moynihan PJ. The relationship between nutrition and systemic and oral well-being in older people. J Am Dent Assoc. 2007;138(4):493–7.
Tada A, Miura H. Systematic review of the association of mastication with food and nutrient intake in the independent elderly. Arch Gerontol Geriatr. 2014;59(3):497–505.
Ferreira MC, Dias-Pereira AC, Branco-de-Almeida LS, Martins CC, Paiva SM. Impact of periodontal disease on quality of life: a systematic review. J Periodontal Res. 2017;52(4):651–65.
Skoskiewicz-Malinowska K, Malicka B, Zietek M, Kaczmarek U. Does oral dryness influence quality of life? Current perspectives in elderly dental care. Adv Clin Exp Med. 2019;28(9):1209–16.
Jensen PM, Saunders RL, Thierer T, Friedman B. Factors associated with oral health-related quality of life in community-dwelling elderly persons with disabilities. J Am Geriatr Soc. 2008;56(4):711–7.
Miura H, Yamasaki K, Morizaki N, Moriya S, Sumi Y. Factors influencing oral health-related quality of life (OHRQoL) among the frail elderly residing in the community with their family. Arch Gerontol Geriatr. 2010;51(3):e62–5.
Ostberg AL, Hall-Lord ML. Oral health-related quality of life in older Swedish people with pain problems. Scand J Caring Sci. 2011;25(3):510–6.
Hassel AJ, Koke U, Schmitter M, Rammelsberg P. Factors associated with oral health-related quality of life in institutionalized elderly. Acta Odontol Scand. 2006;64(1):9–15.
Dolan TA, Peek CW, Stuck AE, Beck JC. Functional health and dental service use among older adults. J Gerontol A Biol Sci Med Sci. 1998;53(6):M413–8.
Chalmers J, Pearson A. Oral hygiene care for residents with dementia: a literature review. J Adv Nurs. 2005;52(4):410–9.
Niesten D, Witter D, Bronkhorst E, Creugers N. Oral health-related quality of life and associated factors in a care-dependent and a care-independent older population. J Dent. 2016;55:33–9.
Niesten D, Witter DJ, Bronkhorst EM, Creugers NHJ. Oral health care behavior and frailty-related factors in a care-dependent older population. J Dent. 2017;61:39–47.
MacEntee MI, editor. Oral healthcare and the frail elder. Iowa: Wiley-Blackwell; 2011.
Ekback G, Persson C, Linden-Bostrom M. What factors can be protective for both self-rated oral health and general health? Swed Dent J. 2015;39(2):99–107.
Takeshita H, Ikebe K, Kagawa R, Okada T, Gondo Y, Nakagawa T, et al. Association of personality traits with oral health-related quality of life independently of objective oral health status: a study of community-dwelling elderly Japanese. J Dent. 2015;43(3):342–9.
Jamieson LM, Parker EJ, Roberts-Thomson KF, Lawrence HP, Broughton J. Self-efficacy and self-rated oral health among pregnant aboriginal Australian women. BMC Oral Health. 2014;14:29.
Schwartz CE, Bode R, Repucci N, Becker J, Sprangers MA, Fayers PM. The clinical significance of adaptation to changing health: a meta-analysis of response shift. Qual Life Res. 2006;15(9):1533–50.
Acharya S, Sangam DK. Oral health-related quality of life and its relationship with health locus of control among Indian dental university students. Eur J Dent Educ. 2008;12(4):208–12.
Miao L, Feng J, Wu L, Zhang S, Ge Z, Pan Y. The mediating role of general self-efficacy in the association between perceived social support and oral health-related quality of life after initial periodontal therapy. BMC Oral Health. 2016;16(1):68.
MacEntee MI. Quality of life as an indicator of oral health in older people. J Am Dent Assoc. 2007;138(Suppl):47S–52S.
Brondani M. The voice of the elderly in accepting alternative perspectives on oral health. Community Dent Health. 2010;27(3):139–44.
Maupome G, MacEntee MI. Prosthodontic profiles relating to economic status, social network, and social support in an elderly population living independently in Canada. J Prosthet Dent. 1998;80(5):598–604.
McGrath C, Bedi R. Influences of social support on the oral health of older people in Britain. J Oral Rehabil. 2002;29(10):918–22.
Watt RG. Emerging theories into the social determinants of health: implications for oral health promotion. Community Dent Oral Epidemiol. 2002;30(4):241–7.
Locker D. Measuring oral health: a conceptual framework. Community Dent Health. 1988;5:3–18.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2020 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Niesten, D., McKenna, G. (2020). Quality of Life and Oral Health in Older People. In: Kossioni, A. (eds) Gerodontology Essentials for Health Care Professionals. Practical Issues in Geriatrics. Springer, Cham. https://doi.org/10.1007/978-3-030-41468-9_6
Download citation
DOI: https://doi.org/10.1007/978-3-030-41468-9_6
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-41467-2
Online ISBN: 978-3-030-41468-9
eBook Packages: MedicineMedicine (R0)