Abstract
Brentuximab vedotin (BV) and the PD-1 inhibitors have dramatically expanded options and improved outcomes for patients with relapsed or refractory Hodgkin lymphoma (HL). For patients with disease progression following BV, PD-1 inhibitors, and autologous stem cell transplant (ASCT), treatment options are limited. Additional classes of drugs have been found to be effective for HL, including drugs that target the PI3-kinase (PI3K) pathway, histone deacetylase (HDAC) inhibitors, as well as immune modulatory agents. These agents target both the Hodgkin Reed-Sternberg cells as well as the tumor microenvironment. While these targeted drugs are options for patients who have progressed after BV or PD-1 inhibitors, there is good rationale for combining some of these agents with either BV or PD-1 inhibitors to improve response rates or durability. Such combinations are under investigation in clinical trials. Emerging therapies for HL include the anti-CD25 antibody drug conjugate, camidanlumab, as well as other therapies that target CD30 such as anti-CD30 chimeric antigen receptor (CAR)-T cells and the bispecific antibody, AFM-13. Newer targeted agents, emerging therapies, as well as studies evaluating novel combinations will be reviewed.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
1 PI3K/Akt/mTOR Pathway
Constitutive activation of the PI3K/Akt/mTOR pathway is present in both HL cell lines and primary tissue [1, 2]. The significance of this pathway in HL was demonstrated by the efficacy of everolimus, an mTOR inhibitor, in patients with relapsed or refractory (rel/ref) HL. In the phase II study evaluating everolimus in rel/ref HL, patients received 10 mg/day until progression of disease [3]. Among the 57 patients enrolled, the overall response rate (ORR) and complete response (CR) rate were 45.6% and 8.8%, respectively. Seven (12%) patients were long-term responders (lasting >12 months). Treatment was well tolerated with grade 3 or 4 thrombocytopenia and anemia occurring in 21% and 14%, respectively. Furthermore, only 3.5% of patients experienced grade 3 stomatitis, and pneumonitis occurred in 10.5% (all grade 1 or 2).
The value of targeting this pathway in HL was further tested through a phase II study evaluating idelalisib, a delta-specific PI3 kinase (PI3Kδ) inhibitor. PI3Kδ is preferentially expressed in cells of hematopoietic origin, particularly B cells, and is highly expressed in HL cell lines compared to other PI3K isoforms [4]. Twenty-five patients with rel/ref HL enrolled on this study and were treated with idelalisib 150 mg BID until progression, with the option to increase to 300 mg BID. The ORR was 20% with one complete response and four partial responses [5]. As was seen with everolimus, a few prolonged responses were observed and median duration of response was 8.4 months. Adverse events typically seen with this drug class were observed and included grade ≥ 3 elevations in alanine aminotransferase and/or aspartate aminotransferase in five patients, colitis (grade 1 or 2) in three patients, and grade 2 pneumonitis in one patient.
Preclinical studies have led to several clinical trials evaluating novel regimens involving drugs affecting the PI3K pathway. For example, the demonstration of synergy between everolimus and panobinostat in HL cell lines led to a phase I/II study evaluating this combination [6, 7]. This combination, however, did not appear to be more efficacious than observed with either drug alone. There is also rationale for combining PI3K pathway inhibitors and immunotherapeutic agents. PI3K blockade inhibits regulatory T cells and reduces anti-inflammatory cytokines; therefore PI3K inhibitors likely function in part through promotion of antitumor immunity and have potential to synergize with PD-1 blockade [8, 9]. Pembrolizumab plus idelalisib is being evaluated in a study for chronic lymphocytic leukemia and indolent B-cell non-Hodgkin lymphomas (NCT02332980). In addition, a study evaluating PD-1 blockade plus everolimus for solid tumors is underway (NCT02890069). If these combinations are found to be safe, it would be reasonable to evaluate them in HL as well.
2 HDAC Inhibitors
The histone deacetylase (HDAC) inhibitors target both HL Reed-Sternberg (RS) cells and their tumor microenvironment and therefore are particularly attractive agents for HL. Their epigenetic effects on gene expression support apoptosis of RS cells and cause disruption of the cytokine- and chemokine-mediated interactions between the RS cells and their microenvironment [10, 11]. The available HDAC inhibitors differ by their specificity for particular HDAC isotypes, and the more selective HDAC inhibitors may have the advantage of causing less hematologic toxicity.
Both pan-HDAC inhibitors (vorinostat and panobinostat) and more selective inhibitors (mocetinostat and entinostat) have been evaluated in HL. Vorinostat demonstrated only modest activity in rel/ref HL in a phase II study by the Southwest Oncology Group (SWOG), with only 1 out of 25 patients achieving PR [12]. Panobinostat demonstrated more promising activity in an international phase II study in rel/ref HL [13]. Of 129 patients, there were 35 (27%) responses, which included 5 (4%) CRs and 30 (23%) PRs. Furthermore, tumor reductions were observed in 74% of patients. Responses were durable with median duration of response of 6.9 months. Common toxicities seen with this agent were thrombocytopenia (79% grade 3/4), diarrhea, nausea, and fatigue.
Mocetinostat, which selectively inhibits class I and IV HDACs, was evaluated in 51 patients with HL and demonstrated an ORR of 33% [14]. In contrast to panobinostat, hematologic toxicity was rarely seen with mocetinostat; however, 6% of patients developed nonfatal pericardial effusions. Entinostat, a selective class I HDAC inhibitor, demonstrated an ORR of 12% (6 PRs among 49 patients) and tumor reductions in 58% of patients [15].
Overall, the HDAC inhibitors consistently demonstrate activity in HL and cause only moderate toxicity; therefore, they are good candidates for evaluation in combination with other agents for HL. Their role in enhancing antitumor immunity through activating natural killer cell-mediated cell killing provides rationale for combination with PD-1 blockade [16]. An ongoing phase II study with pembrolizumab plus entinostat in Hodgkin lymphoma and follicular lymphoma is testing this concept (NCT03179930).
3 Lenalidomide
The antitumor activity of lenalidomide in HL is potentially mediated through activation of the E3 ubiquitin ligase cereblon, resulting in direct cytotoxicity, alteration of tumor cell microenvironment, and/or antiangiogenesis [17, 18]. Evidence of activity of lenalidomide in HL was initially reported by Böll and colleagues among 12 patients with rel/ref HL treated on a named patient program; all of the patients achieved clinical benefit and 50% achieved objective responses [19]. One patient achieved a complete response which was ongoing after 2 years of therapy. In a larger phase II study of 36 patients with rel/ref HL, lenalidomide induced objective responses in seven (19%) patients. An additional five (14%) patients achieved stable disease for 6 months or more, and prolonged responses were observed yielding a median time to treatment failure of 15 months [20]. Although not tremendously active as a single agent in HL, lenalidomide produces durable responses and represents another good candidate for combination. Lenalidomide has been evaluated in combination with everolimus as well as panobinostat; however neither combination appears more active than the individual agents [21, 22]. Ongoing studies are evaluating lenalidomide in combination with nivolumab (NCT03015896) and brentuximab vedotin (NCT03302728).
4 Emerging Therapies
Newer methods for targeting CD30 are under investigation and include chimeric antigen receptor (CAR)-T cells and bispecific antibodies. An initial phase I study evaluating anti-CD30 CAR-T cells demonstrated only limited activity in HL, likely due to lack of pre-CAR-T lymphodepleting chemotherapy [23]. Lymphodepleting chemotherapy improves CAR-T cell expansion and is incorporated into two ongoing studies which show promising activity in small numbers of patients so far [24,25,26].
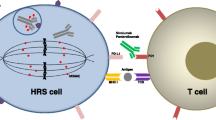
AFM13 is a bispecific antibody construct that binds CD30 on tumor cells as well as CD16A on NK cells. It works by enhancing NK cell-mediated tumor cell killing. A phase I study of AFM13 showed single-agent activity in relapsed and refractory HL and it is currently being evaluated in combination with pembrolizumab [27, 28]. The combination is well-tolerated and interim results show ORR and CR rates of 87% and 35% among 23 evaluable patients.
CD25 is another promising target for HL, given that it is expressed on both Hodgkin Reed-Sternberg cells and regulatory T cells. ADCT-301 (camidanlumab) is an antibody-drug conjugate comprised of an anti-CD25 monoclonal antibody conjugated to the pyrrolobenzodiazepine dimer (PBD) toxin. In a phase I study, 60 patients with HL were treated and ORR rate among evaluable patients (n = 55) was 69% with 43.6% achieving CR [29]. Furthermore, at the recommended dose for expansion (45 μg/kg), the ORR and CR rates among 26 patients were 80.8% and 50%, respectively. Notable toxicities observed with camidanlumab included Guillain Barre (3.3%), grade 3 transaminitis (10%), and grade 3 rash (13.3%). A phase II study further evaluating efficacy and toxicity of this agent in HL is planned (Table 24.1).
5 Conclusion
Even with the availability of BV and anti-PD1 antibodies, there is considerable room for improvement in the treatment of HL. In the rel/ref setting, treatment options eventually become exhausted as patients ultimately progress following BV or anti-PD1-based treatment. Furthermore, more individualized and better-tolerated therapies are needed in the frontline and second-line treatment setting for HL. Therapies currently under investigation in HL target activated pathways within the RS cells, the HL microenvironment, or both, and the key challenge will be to identify markers that predict likelihood of response and to determine the optimal way to combine these agents to produce well-tolerated, effective regimens. As we continue to develop new effective agents for HL, emerging biomarkers, such as circulating tumor DNA [30], will undoubtedly aid us in identifying the right patient for the best treatment at the optimal time (Figs. 24.1 and 24.2).
References
Dutton A, Reynolds GM, Dawson CW, Young LS, Murray PG (2005) Constitutive activation of phosphatidyl-inositide 3 kinase contributes to the survival of Hodgkin’s lymphoma cells through a mechanism involving Akt kinase and mTOR. J Pathol 205:498–506
Georgakis GV, Li Y, Rassidakis GZ, Medeiros LJ, Mills GB, Younes A (2006) Inhibition of the phosphatidylinositol-3 kinase/Akt promotes G1 cell cycle arrest and apoptosis in Hodgkin lymphoma. Br J Haematol 132:503–511
Johnston PB, Pinter-Brown LC, Warsi G, White K, Ramchandren R (2018) Phase 2 study of everolimus for relapsed or refractory classical Hodgkin lymphoma. Exp Hematol Oncol 7:12
Meadows SA, Vega F, Kashishian A et al (2012) PI3Kdelta inhibitor, GS-1101 (CAL-101), attenuates pathway signaling, induces apoptosis, and overcomes signals from the microenvironment in cellular models of Hodgkin lymphoma. Blood 119:1897–1900
Gopal AK, Fanale MA, Moskowitz CH et al (2017) Phase II study of idelalisib, a selective inhibitor of PI3Kdelta, for relapsed/refractory classical Hodgkin lymphoma. Ann Oncol 28:1057–1063
Lemoine M, Derenzini E, Buglio D et al (2012) The pan-deacetylase inhibitor panobinostat induces cell death and synergizes with everolimus in Hodgkin lymphoma cell lines. Blood 119:4017–4025
Oki Y, Buglio D, Fanale M et al (2013) Phase I study of Panobinostat plus Everolimus in patients with relapsed or refractory lymphoma. Clin Cancer Res 19:6882–6890
Ali K, Soond DR, Pineiro R et al (2014) Inactivation of PI(3)K p110delta breaks regulatory T-cell-mediated immune tolerance to cancer. Nature 510:407–411
Marshall NA, Galvin KC, Corcoran AM, Boon L, Higgs R, Mills KH (2012) Immunotherapy with PI3K inhibitor and toll-like receptor agonist induces IFN-gamma+IL-17+ polyfunctional T cells that mediate rejection of murine tumors. Cancer Res 72:581–591
Buglio D, Georgakis GV, Hanabuchi S et al (2008) Vorinostat inhibits STAT6-mediated TH2 cytokine and TARC production and induces cell death in Hodgkin lymphoma cell lines. Blood 112:1424–1433
Buglio D, Khaskhely NM, Voo KS, Martinez-Valdez H, Liu YJ, Younes A (2011) HDAC11 plays an essential role in regulating OX40 ligand expression in Hodgkin lymphoma. Blood 117:2910–2917
Kirschbaum MH, Goldman BH, Zain JM et al (2007) Vorinostat (Suberoylanilide Hydroxamic acid) in relapsed or refractory Hodgkin lymphoma: SWOG 0517. ASH Annual Meeting Abstracts 110:2574
Younes A, Sureda A, Ben-Yehuda D et al (2012) Panobinostat in patients with relapsed/refractory Hodgkin’s lymphoma after autologous stem-cell transplantation: results of a phase II study. J Clin Oncol Off J Am Soc Clin Oncol 30:2197–2203
Younes A, Oki Y, Bociek RG et al (2011) Mocetinostat for relapsed classical Hodgkin’s lymphoma: an open-label, single-arm, phase 2 trial. Lancet Oncol 12:1222–1228
Batlevi CL, Kasamon Y, Bociek RG et al (2016) ENGAGE- 501: phase II study of entinostat (SNDX-275) in relapsed and refractory Hodgkin lymphoma. Haematologica 101:968–975
Skov S, Pedersen MT, Andresen L, Straten PT, Woetmann A, Odum N (2005) Cancer cells become susceptible to natural killer cell killing after exposure to histone deacetylase inhibitors due to glycogen synthase Kinase-3–dependent expression of MHC class I–related chain a and B. Cancer Res 65:11136–11145
Kotla V, Goel S, Nischal S et al (2009) Mechanism of action of lenalidomide in hematological malignancies. J Hematol Oncol 2:36
Gribben JG, Fowler N, Morschhauser F (2015) Mechanisms of action of Lenalidomide in B-cell non-Hodgkin lymphoma. J Clin Oncol Off J Am Soc Clin Oncol 33:2803–2811
Boll B, Borchmann P, Topp MS et al (2010) Lenalidomide in patients with refractory or multiple relapsed Hodgkin lymphoma. Br J Haematol 148:480–482
Fehniger TA, Larson S, Trinkaus K et al (2011) A phase 2 multicenter study of lenalidomide in relapsed or refractory classical Hodgkin lymphoma. Blood 118:5119–5125
Maly JJ, Christian BA, Zhu X et al (2017) A phase I/II trial of Panobinostat in combination with Lenalidomide in patients with relapsed or refractory Hodgkin lymphoma. Clin Lymphoma Myeloma Leuk 17:347–353
Padrnos L, Ernst B, Dueck AC et al (2018) A novel combination of the mTORC1 inhibitor everolimus and the immunomodulatory drug lenalidomide produces durable responses in patients with heavily pretreated relapsed lymphoma. Clin Lymphoma Myeloma Leuk 18:664–672.e2
Ramos CA, Ballard B, Zhang H et al (2017) Clinical and immunological responses after CD30-specific chimeric antigen receptor-redirected lymphocytes. J Clin Invest 127:3462–3471
Ramos CA, Rouce R, Robertson CS et al (2018) In vivo fate and activity of second- versus third-generation CD19-specific CAR-T cells in B cell non-Hodgkin’s lymphomas. Mol Ther 26:2727–2737
Ramos CA, Bilgi M, Gerken CP et al (2018) CD30-chimeric antigen receptor (CAR) T cells for therapy of Hodgkin lymphoma (HL). Blood 132:680
Grover NS, Park SI, Ivanova A et al (2018) Clinical responses to CAR.CD30-T cells in patients with CD30+ lymphomas relapsed after multiple treatments including Brentuximab Vedotin. Blood 132:681
Rothe A, Sasse S, Topp MS et al (2015) A phase 1 study of the bispecific anti-CD30/CD16A antibody construct AFM13 in patients with relapsed or refractory Hodgkin lymphoma. Blood 125:4024–4031
Bartlett NL, Chen RW, Domingo-Domenech E et al (2018) A phase 1b study investigating the combination of the tetravalent bispecific NK cell engager AFM13 and Pembrolizumab in patients with relapsed/refractory Hodgkin lymphoma after Brentuximab Vedotin failure: updated safety and efficacy data. Blood 132:1620
Hamadani M, Collins GP, Samaniego F et al (2018) Phase 1 study of Adct-301 (Camidanlumab Tesirine), a novel Pyrrolobenzodiazepine-based antibody drug conjugate, in relapsed/refractory classical Hodgkin lymphoma. Blood 132:928
Spina V, Bruscaggin A, Cuccaro A et al (2018) Circulating tumor DNA reveals genetics, clonal evolution, and residual disease in classical Hodgkin lymphoma. Blood 131:2413–2425
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2020 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Moskowitz, A.J., Younes, A. (2020). Other New Agents for Hodgkin Lymphoma. In: Engert, A., Younes, A. (eds) Hodgkin Lymphoma. Hematologic Malignancies. Springer, Cham. https://doi.org/10.1007/978-3-030-32482-7_24
Download citation
DOI: https://doi.org/10.1007/978-3-030-32482-7_24
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-32481-0
Online ISBN: 978-3-030-32482-7
eBook Packages: MedicineMedicine (R0)