Abstract
Although allergic diseases were historically reported more commonly in industrialized populations, in the past decades, their rates have been on the rise globally, especially in developing countries. Trends observed in various developing countries in Africa, the Middle East, Asia, and Latin America show this increasing prevalence has been attributed to the effects of modernization in those countries. Multiple risk factors of allergic diseases, such as obesity, tobacco exposure, living in close proximity of factories, or simply overcrowding, are linked to urbanization and modern life styles. It is important to note that despite lower disease rates, the impact of allergic diseases is potentially higher in developing countries with limited resources than that observed in developed countries. This is at least partly due to a lack of knowledge and inadequate access to health care. The lack of awareness about the rise of allergies must be addressed in order to decrease the burden of these diseases.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
Allergic diseases are defined as a hypersensitivity or overreaction of the immune system to seemingly harmless substances in the environment. While being impacted by the environment, they are also closely linked to the genetic background of the individuals affected. A number of allergic conditions can be observed as a result of this altered immune response, such as atopic dermatitis, asthma, allergic rhinitis, and food sensitivity/allergy. Although allergens are different throughout the world and in different environments, some are more commonly known to cause an allergic response in many populations; these include pollens, dust mites, animal dander, insect bites, and certain foods such as nuts and seafood.
Historically, allergic diseases were seen more commonly in industrialized populations and more so in urban areas compared to rural regions. However, in the past few decades, a changing trend has been witnessed, and higher incidence of allergic diseases is observed in developing countries as well. This rise has been attributed to the effects of modernization, industrialization, and improved sanitation in those countries, as well as greater access to various foods. Modern life changes such as overcleaning, access to filtered and sanitized water, use of pesticides, detergents and cleaners, as well as food storage and transportation have decreased exposure to many antigens that individuals would previously be in contact with on a daily basis. But how does this affect allergic diseases? The answer is described by the “hygiene hypothesis,” which is, perhaps, the most credible explanation for the observed change caused by modernization [1, 2]. The hygiene hypothesis states that decreased exposure to bacteria early on in life inhibits full immune system development, making individuals prone to allergic diseases [1]. Therefore, the more sterile the living environment in early life, the higher the incidence of allergic diseases. The hygiene hypothesis is supported by migration studies where individuals from developing countries with low incidence of allergic and autoimmune diseases who migrated to developed countries with high incidence of these diseases acquired these conditions at rates similar to that of natives of the developed country, emphasizing the role of modern lifestyles and the environment in the development of these conditions [3]. With that said, two important factors influencing this observation are the length of stay of migrants and their age at the time of migration. This reinforces the idea that the lack of exposure to bacteria in early childhood is what leads to the exacerbated immune response.
Some of the consequences of this altered immune function have a greater impact on individuals’ lives than others. Asthma, for example, characterized by inflammation and narrowing of the airways, affected 339 million people worldwide in 2018. Although its exact cause is not known, there is strong evidence linking atopy and asthma to the hygiene hypothesis [4]. However, most observations of asthma as an allergic disease come predominantly from high-income, developed countries, and the association of the two is weaker in low- and middle-income or developing countries. Could this be a truly weak association though? Or is it simply because data are lacking from developing countries?
Although it is speculated that the prevalence of allergic diseases in developing countries is growing, data is lacking on the exact rates of these conditions in various parts of the world. What is certain, however, is that prevalence rates are still lower than those observed in developed countries. With that said, because of poorer economic conditions and lack of access to appropriate medical care, the health and economic impact of these diseases appear to be higher in developing and underprivileged countries [5].
In the following sections, we will first review the available data on the prevalence of allergic diseases in developing countries and discuss trends and patterns seen over the past few decades, and then, we will discuss the overall risk factors and common allergens, followed by the burden caused by allergic diseases in these countries.
Prevalence of Allergic Diseases: An Overview
The International Study of Asthma and Allergies in Childhood (ISAAC) is the largest worldwide collaborative epidemiological research project investigating asthma, rhinitis, and eczema, including data from over 100 countries. The study started in 1991 and has had several phases carried out thus far. Early data from the study reported an astounding 20-fold to 60-fold difference in asthma, allergic rhinoconjunctivitis, and atopic dermatitis (eczema) among children in different parts of the world [6]. As expected, these diseases were highest in developed countries, such as the United Kingdom, Australia, New Zealand, and Ireland, and lowest in developing countries, such as Indonesia, China, Taiwan, Uzbekistan, India, and Ethiopia [7]. But prevalence rates increased throughout the world from Phase I to Phase III studies, with 6- to 7-year-old children of Jodhpur, India, experiencing the lowest rates (2.4%) and those in Costa Rica experiencing the highest (37.6%).
Asthma trends: The rates of asthma are markedly varied across the globe. Adolescents (13–14 years of age) in Tibet and New Zealand experienced the lowest and highest rates of asthma, respectively (0.8% vs. 32.6%) [5]. The countries experiencing the highest rates of asthma most often had higher rates of allergic rhinoconjunctivitis as well.
Atopic dermatitis followed different patterns, with African countries being among those with higher prevalence rates. Studies on atopic dermatitis revealed rates as low as <2% in Iran to over 16% in Japan and Sweden in 6–7 year olds. The rates were also varied in older children in different parts of the world with rates of <1% in Albania and over 17% in Nigeria in 13- to 14-year-old children [7]. Phase III data from ISAAC in 2008 showed the increasing trend in atopic dermatitis with the highest rates being in Asia and Latin America. In children 13–14 years of age, atopic dermatitis ranged from 0.2% in China to 24.6% in Columbia with the highest rates again in Africa and Latin America [8].
Food allergies are another major category of allergic diseases, and although there is a lack of high-quality studies using gold standard techniques of diagnosing food allergies, the available data still shows an increasing trend in developed and developing countries, with some developing countries showing rates as high as developed countries [9, 10]. Genome–environment interactions are evidenced by studies investigating food allergies in migrants or descendants of low- and middle-income countries growing up in developed countries. These studies have shown that the rates of food allergies in these immigrant populations are even higher than that observed in natives of those developed countries [10].
One very important factor when comparing prevalence rates among different countries is having the same diagnostic criteria for a disease, as different criteria in the same population can give varying results, let alone in different populations around the world. And while not all studies published in the past few decades use the same diagnostic criteria, many are either part of the ISAAC project or have adopted its protocols and questionnaires, performing the same study in 6-to 7-year-old and 13- to 14-year-old children, making their results ideal for comparison. Although all relevant studies have been included in the sections presented in this chapter, for the sake of convenience, studies using ISAAC guidelines are marked in the tables associated with each section.
Prevalence and Trends of Allergic Diseases: Africa
The prevalence of allergic diseases varies widely between African countries and even within different regions of one country. Data from selected countries are presented in Table 2.1. The lowest rates of asthma are reported in children from a low socioeconomic region of Nigeria (0.9%), while highest rates are observed in South Africa and Congo (20.3% and 19.9%, respectively) [11, 12]. Allergic rhinitis rates as high as 38.5% and 61.7% have been reported in the general population of South Africa and Benin, respectively [13, 14]. Data from African countries is very limited, and it is hard to pinpoint exact high and low regions, but even with the scarce amount of data available, the increasing trend in allergic diseases over the past few decades is evident. The same survey repeated 6 years apart in Kenyan adolescents showed significant changes over time. The rate of asthma increased from 6.6% to 12.6%, while allergic rhinitis increased from 14.9% to 38.6% and atopic dermatitis increased from 13.9% to 28.5% [15]. South Africa also showed similar trends with a 1–8.5% increase in different allergic diseases over a 7-year period [14].
Food allergies also appear to be on the rise in African countries with highest rates reported in Zimbabwe (10%) and Morocco (9.5%) [16]. Self-reported food reactions are as high as 28% in Nigeria [17]. Forty percent of children with atopic dermatitis in South Africa have a peanut allergy, one of the most common allergens [18, 19]. Other foods known to cause allergic reactions in various African countries include apples, tomatoes, soy, crab, egg whites, and milk. Sea food allergy is also high in certain regions of South Africa [20].
Prevalence and Trends of Allergic Diseases: Middle East
Most data in the Middle East come from studies performed in Turkey followed by Iran and Saudi Arabia. Before talking about individual countries, however, it would be best to get an overall picture of asthma status in that region by noting the meta-analysis performed in 2018 in the Eastern Mediterranean Region countries (Afghanistan, Bahrain, Djibouti, Egypt, Iran, Iraq, Jordan, Kuwait, Lebanon, Libya, Morocco, Oman, Pakistan, Palestine, Qatar, Saudi Arabia, Somalia, Sudan, Syria, Tunisia, United Arab Emirates (UAE), Yemen, and Cyprus). Using the World Health Organization definition of asthma, Masjedi et al. reported a pooled asthma prevalence of 9.38% (confidence interval: 9.20–9.55) [21]. While not all countries had the same amount of data to be reflected in this analysis equally, the highest prevalence rate was observed in Kuwait and the lowest in Syria. Another systematic review from the Arabian Peninsula including seven countries (Kuwait, UAE, Bahrain, Qatar, Oman, Kingdom of Saudi Arabia, and Yemen) reported a prevalence range of 8–23%, while the SNAPSHOT program reported lower prevalence rates of 3.6%, 6.4%, and 6.4% in Egypt, Turkey, and the Gulf Cluster (Kuwait, Saudi Arabia, and the UAE) [22, 23].
Selected data from different countries in addition to time trends are shown in Table 2.2. Based on these data, the highest reported prevalence of asthma in the years 2010–2019 was 35.4% in children (Iran—single-center study) and 15% in adults (Kuwait—national survey) [24, 25]. The lowest rates reported in children and adults were 8.9% (Turkey) and 1.9% (Kazakhstan), respectively [26, 27]. Given that allergic diseases are predominantly diagnosed for the first time in childhood, the majority of studies in the Middle East have focused on children, using ISAAC guidelines. While the rates of allergic diseases vary among different countries, they do show an anticipated rise in allergic diseases. In Turkey, the same survey repeated in 1994, 2004, and 2014 shows this trend well. The rate of allergic rhinitis, asthma, and atopic dermatitis increased from 8.8% to 15.6%, 5% to 8.9%, and 5% to 7%, respectively [27]. Other similar trends are seen in Oman, Iran, Saudi Arabia, and Lebanon (Table 2.2).
Of the different allergic diseases, the highest rates in all Middle Eastern countries belong to allergic rhinitis. In Iran, about 40% of children and 26–28% of adults experience allergic rhinitis independent from or along with asthma [28,29,30]. Rates as high as 20%, 30%, and 38% have also been reported in Kuwait, Qatar, and Saudi Arabia, respectively [31,32,33]. Data on food allergy prevalence is lacking in the Middle East; however, the available data show an increase in this category of allergic diseases as well. In Turkey, seafood, fermented drinks made with millets, and animal fats are among common food allergens reported [34]. Peanuts were the most common food allergen in Saudi Arabia, and in Israel, egg, cow’s milk, and sesame caused the most number of allergic reactions [35, 36].
Prevalence and Trends of Allergic Diseases: Asia
In general, asthma prevalence is lower in Asian developing countries compared to those in other regions of the world. A range of 1.1–11.0% was found in a systematic review of 74 studies in various regions of China, with the lowest prevalence being observed in Tibet and highest in Hong Kong [37]. Most studies performed in mainland China have used Chinese diagnostic guidelines, yielding a lower prevalence of 3% [37]. Crude prevalence of asthma in India, Sri Lanka, Bangladesh, Nepal, and Pakistan were found to be 6.3%, 5.3%, 5.2%, 4.2%, and 3.7%, respectively [38]. The highest rate of allergic rhinitis was reported for adults in Thailand (37.7%), followed by those in Vietnam (29.6%) [39, 40]. Food allergy prevalence appears to be comparable to prevalence rates observed in Europe and the West, even though the types of foods consumed vary widely [41, 42]. Various seafood are major allergens in the adult population, while eggs and milk commonly affect children. In India, beef and wheat allergies are reported as well. Table 2.3 summarizes results of selected studies performed throughout Asia. Similar to many other developing countries, data from most countries are insufficient, especially in the adult population.
Prevalence and Trends of Allergic Diseases: Latin America
Based on the data available, the highest rate of asthma in adults and children living in Latin American countries is 9.5% (Argentina) and 28.6% (Brazil), respectively, while the lowest rates reported are 4.4% (Brazil) and 6.1% (Mexico) [43,44,45,46]. The same increasing trend observed in other developing countries is reported in Latin America as well, although data from most countries excluding Mexico and Brazil are scarce. Selected data from these countries are shown in Table 2.4. As with other countries, allergic rhinitis is the most common allergic disease with rates as high as 43.2%, 42.6%, and 36.6% reported in Brazilian, Costa Rican, and Colombian youth [47,48,49]. Given the tropical climate of many Latin American countries, dampness, mold, and different fungi commonly trigger allergic reactions. Food allergies range from 0.8% in Argentina to 5.7% in El Salvador, where milk, shrimp, chili, chocolate, and nuts were the most common allergens [50, 51].
Risk Factors and Common Allergens in Developing Countries
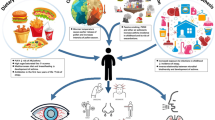
So there is evidently an increasing trend in allergic diseases in developing countries, and while risk factors such as gender, age, family history of atopic diseases, and socioeconomic status affect the development of allergic diseases [14, 19, 29, 33, 34, 52,53,54,55,56,57,58,59,60,61,62,63,64,65,66,67,68,69,70,71,72,73,74,75,76,77,78,79,80,81,82,83], these factors have been present at times of lower prevalence rates as well and do not contribute much to the increasing rates over the past few decades. What risk factors do affect allergic diseases then? Probably, those that have changed as a result of urbanization and modernization. Examples of these are increase in caesarian section rates, smoking, obesity, and exposure to air pollutants.
Mode of delivery
Birth delivery mode has been shown to affect the rate of allergic diseases [49, 72, 73, 84,85,86,87,88]. More caesarian sections are being performed now compared to past decades, since it seems to be the “modern” way of delivering a child in many countries where it is performed without adequate indication. In 2010, the World Health Organization reported over 6.2 million unnecessary caesarian sections being performed worldwide, 50% of which belonged to China and Brazil [89].
Obesity
Greater consumption of high-fat foods and lower physical activity leading to overweight and obesity are also common trends in urbanized societies. Fast food consumption, weight gain, and higher body mass index have been reported to be risk factors of asthma and its related symptoms as well [26, 65, 75, 78, 90,91,92,93,94,95,96,97,98,99,100,101,102,103,104,105].
Smoking
Most studies in different developing countries have reported higher rates of allergic diseases in urban vs. rural areas [62, 101, 106,107,108,109,110,111,112,113,114,115]. Furthermore, many reports have indicated that exposure to tobacco smoking is an important risk factor for asthma [55, 62, 73,74,75, 77, 78, 81, 90, 92, 93, 95, 96, 116,117,118,119,120,121,122,123,124,125,126,127,128,129,130,131,132,133,134,135]. One interesting observation made in several studies is the effects of maternal smoking on increased allergic diseases in children [72, 73, 88, 121, 136,137,138,139,140]. One possible explanation for this observation is that in many societies, female smoking was previously regarded as a taboo, but it appears that cultures have overcome this taboo and female smoking has become more common in developing countries. The effects of smoking during pregnancy and low-birth-weight children have been extensively studied and proven before, and now higher rates of allergic diseases are observed in children born underweight and to mothers who smoke.
Pet allergy
Many of the allergens reported in various countries also reflect modernization features. Pets are a common allergen in many developing countries, as having a pet inside the home (dogs and cats) is more common now [13, 34, 77, 92, 104, 116,117,118, 121, 127, 132, 134, 140,141,142,143,144,145,146,147,148]. This can contribute to the increased rate of pet allergy.
Industrial sites and pollution
Other allergens of urbanized living reported include living in close proximity of different industries such as cement or brick factories, air pollution, and chemical compounds and volatile fuel that individuals were less commonly exposed to prior to the increase in allergic diseases [13, 79, 82, 148,149,150,151,152]. Living conditions often experienced in urban societies such as apartment living, more crowding in small areas, and crowded day-care attendance have been shown to be associated with higher asthma and its related symptoms as well [56, 61, 68, 76, 151, 153,154,155,156,157,158].
Now not all modern techniques adversely affect allergic diseases. For example, use of electricity as a cooking method was shown to be a protective factor compared to wood, coal, and other smoke-producing biomass that were previously used for indoor cooking and heating [39, 126, 127, 134, 159].
The High Burden of Allergic Diseases in Developing Countries
As mentioned in the previous sections, the impact of allergic diseases appears to be higher in developing countries in comparison to developed countries, despite of their lower prevalence rates. But why so? There are several reasons for this phenomenon. Lack of knowledge by patients, caregivers, and most importantly physicians is one critical, influential, and preventable factor. Many studies evaluating physicians’ ability to identify and manage allergic diseases have reported poor and insufficient knowledge about asthma, its pathophysiology and related symptoms [160,161,162,163,164,165,166], delayed or inaccurate diagnosis [167, 168], lack of knowledge about standard medications and guidelines [160, 165, 168,169,170], and general mismanagement [160, 163,164,165, 171,172,173,174,175]. In one study evaluating the quality of asthma management, 40% of individuals diagnosed were not informed about their disease, and those who were informed were not given any educational materials [176]. Of course, these extreme cases are uncommon; however, poor physician–patient interactions further affect disease management. Given that the majority of allergic symptoms first develop in childhood, parental knowledge about these diseases and their management is critical, yet in many instances, missing [177,178,179,180,181]. In one study in Africa, parents perceived asthma to be contagious and transmitted from one person to another, while others believed it was transmitted through contaminated food [182]. In Brazil, some parents believed rescue medications may cause their children harm [44]. Research regarding psychosocial factors affecting asthma management in nine Arab countries has also shown parental knowledge to be generally insufficient [179]. Many parents perceive that their children cannot lead normal lives [175] and these misconceptions adversely affect their children’s quality of life as they are often passed down to them, making them believe that they cannot overcome and control their medical condition. Besides social pressures, lack of knowledge in patients leads to noncompliance with therapy [177, 178, 183, 184], exacerbating disease status.
Even when knowledge is adequate, however, other obstacles such as limited resources hinder better care in developing countries. Many times, the most appropriate medications and therapies are not readily available [168, 185], and even when they are, individuals from lower socioeconomic levels are not able to afford them. The economic burden of allergic diseases is a great concern for many countries. The highest costs in various countries are attributed to inpatient and emergency room visits as well as medications [186,187,188]. In Iran and India, where health care is mostly self-funded, the annual cost per child is very high compared to the average family incomes, draining on family resources [187, 189].
There is a low level of asthma control reported by many developing countries, even those with larger, more rapidly growing economies [184, 186, 187, 190,191,192,193]. In China, physicians reported 75% of patients to be well-controlled, while according to Global Initiative for Asthma (GINA) criteria , less than 15% of them were well-controlled [194].
In Qatar, a country with the highest gross domestic product per capita in the world and high health expenditure per capita, 31% and 26% of patients had uncontrolled and partly controlled asthma, respectively, most of which stemmed from incorrect use of inhalers and misunderstanding the role of reliever and controller medications, signifying that the effects of insufficient knowledge on asthma control are greater than the effects economic limitations may have [190]. Allergic diseases in general, but more so uncontrolled asthma, affect individuals’ quality of life and cause behavioral and emotional problems in children [44, 167, 179]. They cause school and work absences in 52% of children and 30% of adults in Oman, respectively, and similar patterns are observed in other countries as well [44, 179, 186, 191, 195]. Work productivity, daily activities, and sleep quality are also reported to be low by asthma patients in different developing countries. Although decreased quality of life does pertain not only to developing countries but also to anyone with uncontrolled asthma all over the world, the impact is more significant in low-income developing countries because of the higher rate of uncontrolled asthma observed in these populations.
Allergic Diseases: An Emerging Problem or an Overseen Issue?
So are allergic diseases an emerging problem in low-income and developing countries? Or are they an overseen issue in these populations? The answer appears to be both. Allergic diseases are an emerging problem because of changes in disease patterns and rates over the past few decades, caused by multiple risk factors mainly linked to modernization. The majority of the available data is very recent or only partial, indicating that the issue had been overlooked before and not anticipated in many populations. On the other hand, while there is still a substantial amount of work to be done, most developing countries are now aware of the increasing rate of allergic diseases and are trying to do something about it. For so many years, the greatest health obstacle in developing countries was controlling communicable diseases (still the greatest obstacle in underdeveloped countries), as they caused the highest rates of morbidity and mortality. However, with the global disease trends seen over the past decades, changing from high rates of communicable disease to high noncommunicable diseases, there is a need for change in public health policies in order to better control the burden associated with noncommunicable diseases, including allergic diseases. This change has not yet occurred in many developing countries. Medical and political authorities must get engaged in order to develop adequate resources to manage these problems. As with most things, education definitely plays a major role. Turkey has been a pioneer is conducting different educational workshops targeting different levels of care, from formal educational workshop for physicians to allergy camps for children, all of which have been found to be significantly effective and a great first step for combating the burden of allergic diseases in this country. Similar approaches for the development of infrastructures of education, research, and management are needed throughout the world. These programs need to be culturally sensitive and specific to each population in order to precisely address the needs of each group of people and impact their audience.
References
Bach J-F. The hygiene hypothesis in autoimmunity: the role of pathogens and commensals. Nat Rev Immunol. 2017;18:105.
Strachan DP. Hay fever, hygiene, and household size. BMJ. 1989;299(6710):1259–60.
Okada H, Kuhn C, Feillet H, Bach JF. The ‘hygiene hypothesis’ for autoimmune and allergic diseases: an update. Clin Exp Immunol. 2010;160(1):1–9.
The Global Asthma Report 2018. Auckland: Global Asthma Network; 2018.
Lai CK, Beasley R, Crane J, Foliaki S, Shah J, Weiland S. Global variation in the prevalence and severity of asthma symptoms: phase three of the International Study of Asthma and Allergies in Childhood (ISAAC). Thorax. 2009;64(6):476–83.
Worldwide variation in prevalence of symptoms of asthma, allergic rhinoconjunctivitis, and atopic eczema: ISAAC. The International Study of Asthma and Allergies in Childhood (ISAAC) Steering Committee. Lancet. 1998;351(9111):1225–32.
Williams H, Robertson C, Stewart A, Ait-Khaled N, Anabwani G, Anderson R, et al. Worldwide variations in the prevalence of symptoms of atopic eczema in the International Study of Asthma and Allergies in Childhood. J Allergy Clin Immunol. 1999;103(1 Pt 1):125–38.
Odhiambo JA, Williams HC, Clayton TO, Robertson CF, Asher MI. Global variations in prevalence of eczema symptoms in children from ISAAC Phase Three. J Allergy Clin Immunol. 2009;124(6):1251–8.e23.
Prescott SL, Pawankar R, Allen KJ, Campbell DE, Sinn J, Fiocchi A, et al. A global survey of changing patterns of food allergy burden in children. World Allergy Organ J. 2013;6(1):21.
Loh W, Tang MLK. The epidemiology of food allergy in the global context. Int J Environ Res Public Health. 2018;15(9):E2043.
Ait-Khaled N, Odhiambo J, Pearce N, Adjoh KS, Maesano IA, Benhabyles B, et al. Prevalence of symptoms of asthma, rhinitis and eczema in 13- to 14-year-old children in Africa: the International Study of Asthma and Allergies in Childhood Phase III. Allergy. 2007;62(3):247–58.
Adetoun Mustapha B, Briggs DJ, Hansell AL. Prevalence of asthma and respiratory symptoms in children in a low socio-economic status area of Nigeria. Int J Tuberc Lung Dis. 2013;17(7):982–8.
Flatin MC, Ade S, Hounkpatin SH, Ametonou B, Vodouhe UB, Adjibabi W. Symptoms of allergic rhinitis in Parakou, Benin: prevalence, severity and associated factors. Eur Ann Otorhinolaryngol Head Neck Dis. 2018;135(1):33–6.
Zar HJ, Ehrlich RI, Workman L, Weinberg EG. The changing prevalence of asthma, allergic rhinitis and atopic eczema in African adolescents from 1995 to 2002. Pediatr Allergy Immunol. 2007;18(7):560–5.
Esamai F, Ayaya S, Nyandiko W. Prevalence of asthma, allergic rhinitis and dermatitis in primary school children in Uasin Gishu district, Kenya. East Afr Med J. 2002;79(10):514–8.
Boye JI. Food allergies in developing and emerging economies: need for comprehensive data on prevalence rates. Clin Transl Allergy. 2012;2(1):25.
Achinewu SC. Food allergy and its clinical symptoms in Nigeria. Food and Nutrition Bulletin. 1983;5(3):18–19.
Frank L, Marian A, Visser M, Weinberg E, Potter PC. Exposure to peanuts in utero and in infancy and the development of sensitization to peanut allergens in young children. Pediatr Allergy Immunol. 1999;10(1):27–32.
Gray CL, Levin ME, du Toit G. Ethnic differences in peanut allergy patterns in South African children with atopic dermatitis. Pediatr Allergy Immunol. 2015;26(8):721–30.
Zinn C, Lopata A, Visser M, Potter PC. The spectrum of allergy to South African bony fish (Teleosti). Evaluation by double-blind, placebo-controlled challenge. S Afr Med J. 1997;87(2):146–52.
Masjedi M, Ainy E, Zayeri F, Paydar R. Assessing the prevalence and incidence of asthma and chronic obstructive pulmonary disease in the Eastern Mediterranean Region. Turk Thorac J. 2018;19(2):56–60.
Al-Herz W. A systematic review of the prevalence of atopic diseases in children on the Arabian Peninsula. Med Princ Pract. 2018;27(5):436–42.
Al-Digheari A, Mahboub B, Tarraf H, Yucel T, Annesi-Maesano I, Doble A, et al. The clinical burden of allergic rhinitis in five Middle Eastern countries: results of the SNAPSHOT program. Allergy Asthma Clin Immunol. 2018;14:63.
Entezari A, Mehrabi Y, Varesvazirian M, Pourpak Z, Moin M. A systematic review of recent asthma symptom surveys in Iranian children. Chron Respir Dis. 2009;6(2):109–14.
Khadadah M. The cost of asthma in Kuwait. Med Princ Pract. 2013;22(1):87–91.
Nugmanova D, Sokolova L, Feshchenko Y, Iashyna L, Gyrina O, Malynovska K, et al. The prevalence, burden and risk factors associated with bronchial asthma in commonwealth of independent states countries (Ukraine, Kazakhstan and Azerbaijan): results of the CORE study. BMC Pulm Med. 2018;18(1):110.
Dogruel D, Bingol G, Altintas DU, Seydaoglu G, Erkan A, Yilmaz M. The trend of change of allergic diseases over the years: three repeated surveys from 1994 to 2014. Int Arch Allergy Immunol. 2017;173(3):178–82.
Salarnia S, Momen T, Jari M. Prevalence and risk factors of allergic rhinitis in primary school students of Isfahan, Iran. Adv Biomed Res. 2018;7:157.
Shokouhi Shoormasti R, Pourpak Z, Fazlollahi MR, Kazemnejad A, Nadali F, Ebadi Z, et al. The prevalence of allergic rhinitis, allergic conjunctivitis, atopic dermatitis and asthma among adults of Tehran. Iran J Public Health. 2018;47(11):1749–55.
Fazlollahi MR, Najmi M, Fallahnezhad M, Sabetkish N, Kazemnejad A, Bidad K, et al. The prevalence of asthma in Iranian adults: the first national survey and the most recent updates. Clin Respir J. 2018;12(5):1872–81.
Janahi IA, Bener A, Bush A. Prevalence of asthma among Qatari schoolchildren: international study of asthma and allergies in childhood, Qatar. Pediatr Pulmonol. 2006;41(1):80–6.
Al-Ghobain MO, Al-Moamary MS, Al-Hajjaj MS, Al-Fayez AI, Basha SI. Prevalence of rhinitis symptoms among 16 to 18 years old adolescents in Saudi Arabia. Indian J Chest Dis Allied Sci. 2013;55(1):11–4.
Ziyab AH. Prevalence and risk factors of asthma, rhinitis, and eczema and their multimorbidity among young adults in Kuwait: a cross-sectional study. Biomed Res Int. 2017;2017:2184193.
Tamay Z, Akcay A, Ergin A, Guler N. Effects of dietary habits and risk factors on allergic rhinitis prevalence among Turkish adolescents. Int J Pediatr Otorhinolaryngol. 2013;77(9):1416–23.
El-Rab MO. Foods and food allergy: the prevalence of IgE antibodies specific for food allergens in Saudi patients. Saudi J Gastroenterol. 1998;4(1):25–9.
Dalal I, Binson I, Reifen R, Amitai Z, Shohat T, Rahmani S, et al. Food allergy is a matter of geography after all: sesame as a major cause of severe IgE-mediated food allergic reactions among infants and young children in Israel. Allergy. 2002;57(4):362–5.
Yangzong Y, Shi Z, Nafstad P, Haheim LL, Luobu O, Bjertness E. The prevalence of childhood asthma in China: a systematic review. BMC Public Health. 2012;12:860.
Bishwajit G, Tang S, Yaya S, Feng Z. Burden of asthma, dyspnea, and chronic cough in South Asia. Int J Chron Obstruct Pulmon Dis. 2017;12:1093–9.
Lam HT, Van TTN, Ekerljung L, Ronmark E, Lundback B. Allergic rhinitis in Northern Vietnam: increased risk of urban living according to a large population survey. Clin Transl Allergy. 2011;1(1):7.
Bunjean K, Sukkasem K, Noppacroh N, Yamkaew N, Janthayanont D, Theerapancharern W, et al. Prevalence of allergic rhinitis and types of sensitized allergen in adult at Wat Intaram community, Hua Raeu, Phra Nakhon Si Ayutthaya District, Phra Nakhon Si Ayutthaya Province, Thailand. J Med Assoc Thail. 2012;95(Suppl 5):S63–8.
Lee AJ, Thalayasingam M, Lee BW. Food allergy in Asia: how does it compare? Asia Pac Allergy. 2013;3(1):3–14.
Tang R, Wang ZX, Ji CM, Leung PSC, Woo E, Chang C, et al. Regional differences in food allergies. Clin Rev Allergy Immunol. 2019;57(1):98–110.
Arias SJ, Neffen H, Bossio JC, Calabrese CA, Videla AJ, Armando GA, et al. Prevalence and features of asthma in young adults in urban areas of Argentina. Arch Bronconeumol. 2018;54(3):134–9.
Roncada C, de Oliveira SG, Cidade SF, Sarria EE, Mattiello R, Ojeda BS, et al. Burden of asthma among inner-city children from Southern Brazil. J Asthma. 2016;53(5):498–504.
Menezes AM, Wehrmeister FC, Horta B, Szwarcwald CL, Vieira ML, Malta DC. Prevalence of asthma medical diagnosis among Brazilian adults: National Health Survey, 2013. Rev Bras Epidemiol. 2015;18(Suppl 2):204–13.
Ramirez-Soto M, Bedolla-Barajas M, Gonzalez-Mendoza T. Prevalence of asthma, allergic rhinitis and atopic dermatitis in school children of the Mexican Bajio region. Rev Alerg Mex. 2018;65(4):372–8.
Luna Mde F, Almeida PC, Silva MG. Asthma and rhinitis prevalence and co-morbidity in 13-14-year-old schoolchildren in the city of Fortaleza, Ceara State, Brazil. Cad Saude Publica. 2011;27(1):103–12.
Soto-Martinez ME, Yock-Corrales A, Camacho-Badilla K, Abdallah S, Duggan N, Avila-Benedictis L, et al. The current prevalence of asthma, allergic rhinitis, and eczema related symptoms in school-aged children in Costa Rica. J Asthma. 2019;56(4):360–8.
Penaranda A, Aristizabal G, Garcia E, Vasquez C, Rodriguez-Martinez CE, Satizabal CL. Allergic rhinitis and associated factors in schoolchildren from Bogota, Colombia. Rhinology. 2012;50(2):122–8.
Cabrera-Chavez F, Rodriguez-Bellegarrigue CI, Figueroa-Salcido OG, Lopez-Gallardo JA, Aramburo-Galvez JG, Vergara-Jimenez MJ, et al. Food allergy prevalence in Salvadoran school children estimated by parent-report. Int J Environ Res Public Health. 2018;15(11):2446.
Mehaudy R, Parisi C, Petriz N, Eymann A, Jauregui MB, Orsi M. Prevalence of cow’s milk protein allergy among children in a university community hospital. Arch Argent Pediatr. 2018;116(3):219–23.
Bezzaoucha A. Epidemiology of asthma in children and young adults in Algiers. Rev Mal Respir. 1992;9(4):417–23.
Yemaneberhan H, Flohr C, Lewis SA, Bekele Z, Parry E, Williams HC, et al. Prevalence and associated factors of atopic dermatitis symptoms in rural and urban Ethiopia. Clin Exp Allergy. 2004;34(5):779–85.
Georgy V, Fahim HI, El-Gaafary M, Walters S. Prevalence and socioeconomic associations of asthma and allergic rhinitis in northern [corrected] Africa. Eur Respir J. 2006;28(4):756–62.
Desalu OO, Salami AK, Iseh KR, Oluboyo PO. Prevalence of self reported allergic rhinitis and its relationship with asthma among adult Nigerians. J Investig Allergol Clin Immunol. 2009;19(6):474–80.
Belyhun Y, Amberbir A, Medhin G, Erko B, Hanlon C, Venn A, et al. Prevalence and risk factors of wheeze and eczema in 1-year-old children: the Butajira birth cohort, Ethiopia. Clin Exp Allergy. 2010;40(4):619–26.
Gray CL, Levin ME, Zar HJ, Potter PC, Khumalo NP, Volkwyn L, et al. Food allergy in south African children with atopic dermatitis. Pediatr Allergy Immunol. 2014;25(6):572–9.
Kumah DB, Lartey SY, Yemanyi F, Boateng EG, Awuah E. Prevalence of allergic conjunctivitis among basic school children in the Kumasi Metropolis (Ghana): a community-based cross-sectional study. BMC Ophthalmol. 2015;15:69.
Kiboneka A, Levin M, Mosalakatane T, Makone I, Wobudeya E, Makubate B, et al. Prevalence of asthma among school children in Gaborone, Botswana. Afr Health Sci. 2016;16(3):809–16.
Arrais M, Lulua O, Quifica F, Rosado-Pinto J, Gama JMR, Taborda-Barata L. Prevalence of asthma and allergies in 13-14-year-old adolescents from Luanda, Angola. Int J Tuberc Lung Dis. 2017;21(6):705–12.
Zeyrek CD, Zeyrek F, Sevinc E, Demir E. Prevalence of asthma and allergic diseases in Sanliurfa, Turkey, and the relation to environmental and socioeconomic factors: is the hygiene hypothesis enough? J Investig Allergol Clin Immunol. 2006;16(5):290–5.
Selcuk ZT, Demir AU, Tabakoglu E, Caglar T. Prevalence of asthma and allergic diseases in primary school children in Edirne, Turkey, two surveys 10 years apart. Pediatr Allergy Immunol. 2010;21(4 Pt 2):e711–7.
Khan AA, Tanzil S, Jamali T, Shahid A, Naeem S, Sahito A, et al. Burden of asthma among children in a developing megacity: childhood asthma study, Pakistan. J Asthma. 2014;51(9):891–9.
Cobanoglu HB, Isik AU, Topbas M, Ural A. Prevalence of allergic rhinitis in children in the Trabzon Province of the Black Sea Region of Turkey. Turk Arch Otorhinolaryngol. 2016;54(1):21–8.
Masoompour SM, Mahdaviazad H, Ghayumi SMA. Asthma and its related socioeconomic factors: the Shiraz adult respiratory disease study 2015. Clin Respir J. 2018;12(6):2110–6.
Tarraf H, Aydin O, Mungan D, Albader M, Mahboub B, Doble A, et al. Prevalence of asthma among the adult general population of five Middle Eastern countries: results of the SNAPSHOT program. BMC Pulm Med. 2018;18(1):68.
Chan-Yeung M, Zhan LX, Tu DH, Li B, He GX, Kauppinen R, et al. The prevalence of asthma and asthma-like symptoms among adults in rural Beijing, China. Eur Respir J. 2002;19(5):853–8.
Hassan MR, Kabir AR, Mahmud AM, Rahman F, Hossain MA, Bennoor KS, et al. Self-reported asthma symptoms in children and adults of Bangladesh: findings of the National Asthma Prevalence Study. Int J Epidemiol. 2002;31(2):483–8.
Vichyanond P, Sunthornchart S, Singhirannusorn V, Ruangrat S, Kaewsomboon S, Visitsunthorn N. Prevalence of asthma, allergic rhinitis and eczema among university students in Bangkok. Respir Med. 2002;96(1):34–8.
Lao-araya M, Trakultivakorn M. Prevalence of food allergy among preschool children in northern Thailand. Pediatr Int. 2012;54(2):238–43.
Agrawal S, Pearce N, Ebrahim S. Prevalence and risk factors for self-reported asthma in an adult Indian population: a cross-sectional survey. Int J Tuberc Lung Dis. 2013;17(2):275–82.
Zhao K, Song GH, Gu HQ, Liu S, Zhang Y, Guo YR. Epidemiological survey and risk factor analysis of asthma in children in urban districts of Zhengzhou, China. Zhongguo Dang Dai Er Ke Za Zhi. 2014;16(12):1220–5.
Huang J, Huang DM, Xiao XX, Fu SM, Luo CM, Zeng G, et al. Epidemiological survey of asthma among children aged 0-14 years in 2010 in urban Zhongshan, China. Zhongguo Dang Dai Er Ke Za Zhi. 2015;17(2):149–54.
Shi JB, Fu QL, Zhang H, Cheng L, Wang YJ, Zhu DD, et al. Epidemiology of chronic rhinosinusitis: results from a cross-sectional survey in seven Chinese cities. Allergy. 2015;70(5):533–9.
Zhang F, Hang J, Zheng B, Su L, Christiani DC. The changing epidemiology of asthma in Shanghai, China. J Asthma. 2015;52(5):465–70.
Fu QL, Du Y, Xu G, Zhang H, Cheng L, Wang YJ, et al. Prevalence and occupational and environmental risk factors of self-reported asthma: evidence from a cross-sectional survey in seven Chinese cities. Int J Environ Res Public Health. 2016;13(11):E1084.
Hu SJ, Wei P, Kou W, Wu XF, Liu MY, Chen C, et al. Prevalence and risk factors of allergic rhinitis: a Meta-analysis. Lin Chung Er Bi Yan Hou Tou Jing Wai Ke Za Zhi. 2017;31(19):1485–91.
Ma Q, Yang T. Prevalence and influential factors for asthma among adults in Chinese. Zhong Nan Da Xue Xue Bao Yi Xue Ban. 2017;42(9):1086–93.
Bunyavanich S, Soto-Quiros ME, Avila L, Laskey D, Senter JM, Celedon JC. Risk factors for allergic rhinitis in Costa Rican children with asthma. Allergy. 2010;65(2):256–63.
Borges WG, Burns DA, Felizola ML, Oliveira BA, Hamu CS, Freitas VC. Prevalence of allergic rhinitis among adolescents from Distrito Federal, Brazil: comparison between ISAAC phases I and III. J Pediatr. 2006;82(2):137–43.
Chhabra SK, Gupta CK, Chhabra P, Rajpal S. Risk factors for development of bronchial asthma in children in Delhi. Ann Allergy Asthma Immunol. 1999;83(5):385–90.
Tomac N, Demirel F, Acun C, Ayoglu F. Prevalence and risk factors for childhood asthma in Zonguldak, Turkey. Allergy Asthma Proc. 2005;26(5):397–402.
Breda D, Freitas PF, Pizzichini E, Agostinho FR, Pizzichini MM. Prevalence of asthma symptoms and risk factors among adolescents in Tubarao and Capivari de Baixo, Santa Catarina State, Brazil. Cad Saude Publica. 2009;25(11):2497–506.
Sun Y, Hou J, Sheng Y, Kong X, Weschler LB, Sundell J. Modern life makes children allergic. A cross-sectional study: associations of home environment and lifestyles with asthma and allergy among children in Tianjin region, China. Int Arch Occup Environ Health. 2019;92(4):587–98.
Xu D, Wang Y, Chen Z, Li S, Cheng Y, Zhang L, et al. Prevalence and risk factors for asthma among children aged 0-14 years in Hangzhou: a cross-sectional survey. Respir Res. 2016;17(1):122.
Liu SJ, Wang TT, Cao SY, Tan YQ, Chen LZ. A Meta analysis of risk factors for asthma in Chinese children. Zhongguo Dang Dai Er Ke Za Zhi. 2018;20(3):218–23.
Chatkin MN, Menezes AM, Victora CG, Barros FC. High prevalence of asthma in preschool children in Southern Brazil: a population-based study. Pediatr Pulmonol. 2003;35(4):296–301.
Chatkin MN, Menezes AM. Prevalence and risk factors for asthma in schoolchildren in southern Brazil. J Pediatr. 2005;81(5):411–6.
Gibbons L, Belizán JM, Lauer JA, Betrán AP, Merialdi M, Althabe F. The global numbers and costs of additionally needed and unnecessary caesarean sections performed per year: overuse as a barrier to universal coverage. World Health Report Background Paper, 30. Geneva; 2010.
El Kettani S, Lotfi AB, Aichane A. Prevalence of allergic rhinitis in a rural area of Settat, Morocco. East Mediterr Health J. 2009;15(1):167–77.
Droma Y, Kunii O, Yangzom Y, Shan M, Pingzo L, Song P. Prevalence and severity of asthma and allergies in schoolchildren in Lhasa, Tibet. Clin Exp Allergy. 2007;37(9):1326–33.
Song N, Shamssain M, Zhang J, Wu J, Fu C, Hao S, et al. Prevalence, severity and risk factors of asthma, rhinitis and eczema in a large group of Chinese schoolchildren. J Asthma. 2014;51(3):232–42.
Nakao M, Yamauchi K, Ishihara Y, Omori H, Solongo B, Ichinnorov D. Prevalence and risk factors of airflow limitation in a Mongolian population in Ulaanbaatar: cross-sectional studies. PLoS One. 2017;12(4):e0175557.
Cassol VE, Rizzato TM, Teche SP, Basso DF, Centenaro DF, Maldonado M, et al. Obesity and its relationship with asthma prevalence and severity in adolescents from southern Brazil. J Asthma. 2006;43(1):57–60.
Soto-Martinez M, Avila L, Soto N, Chaves A, Celedon JC, Soto-Quiros ME. Trends in hospitalizations and mortality from asthma in Costa Rica over a 12- to 15-year period. J Allergy Clin Immunol Pract. 2014;2(1):85–90.
Guddattu V, Swathi A, Nair NS. Household and environment factors associated with asthma among Indian women: a multilevel approach. J Asthma. 2010;47(4):407–11.
Sousa CA, Cesar CL, Barros MB, Carandina L, Goldbaum M, Pereira JC. Respiratory diseases and associated factors: population-based study in Sao Paulo, 2008–2009. Rev Saude Publica. 2012;46(1):16–25.
Baumann LM, Romero KM, Robinson CL, Hansel NN, Gilman RH, Hamilton RG, et al. Prevalence and risk factors for allergic rhinitis in two resource-limited settings in Peru with disparate degrees of urbanization. Clin Exp Allergy. 2015;45(1):192–9.
Gonzalez-Garcia M, Caballero A, Jaramillo C, Maldonado D, Torres-Duque CA. Prevalence, risk factors and underdiagnosis of asthma and wheezing in adults 40 years and older: a population-based study. J Asthma. 2015;52(8):823–30.
Hijazi N, Abalkhail B, Seaton A. Diet and childhood asthma in a society in transition: a study in urban and rural Saudi Arabia. Thorax. 2000;55(9):775–9.
Norback D, Zhao ZH, Wang ZH, Wieslander G, Mi YH, Zhang Z. Asthma, eczema, and reports on pollen and cat allergy among pupils in Shanxi province, China. Int Arch Occup Environ Health. 2007;80(3):207–16.
Gutierrez-Delgado RI, Barraza-Villarreal A, Escamilla-Nunez MC, Solano-Gonzalez M, Moreno-Macias H, Romieu I. Food consumption and asthma in school children in Cuernavaca, Morelos, Mexico. Salud Publica Mex. 2009;51(3):202–11.
Farrokhi S, Gheybi MK, Movahhed A, Dehdari R, Gooya M, Keshvari S, et al. Prevalence and risk factors of asthma and allergic diseases in primary schoolchildren living in Bushehr, Iran: phase I, III ISAAC protocol. Iran J Allergy Asthma Immunol. 2014;13(5):348–55.
Alqahtani JM. Asthma and other allergic diseases among Saudi schoolchildren in Najran: the need for a comprehensive intervention program. Ann Saudi Med. 2016;36(6):379–85.
Poongadan MN, Gupta N, Kumar R. Dietary pattern and asthma in India. Pneumonol Alergol Pol. 2016;84(3):160–7.
Viinanen A, Munhbayarlah S, Zevgee T, Narantsetseg L, Naidansuren T, Koskenvuo M, et al. Prevalence of asthma, allergic rhinoconjunctivitis and allergic sensitization in Mongolia. Allergy. 2005;60(11):1370–7.
Nyembue TD, Jorissen M, Hellings PW, Muyunga C, Kayembe JM. Prevalence and determinants of allergic diseases in a Congolese population. Int Forum Allergy Rhinol. 2012;2(4):285–93.
Shimwela M, Mwita JC, Mwandri M, Rwegerera GM, Mashalla Y, Mugusi F. Asthma prevalence, knowledge, and perceptions among secondary school pupils in rural and urban coastal districts in Tanzania. BMC Public Health. 2014;14:387.
Morgan BW, Siddharthan T, Grigsby MR, Pollard SL, Kalyesubula R, Wise RA, et al. Asthma and allergic disorders in Uganda: a population-based study across urban and rural settings. J Allergy Clin Immunol Pract. 2018;6(5):1580–7.e2.
Ma Y, Zhao J, Han ZR, Chen Y, Leung TF, Wong GW. Very low prevalence of asthma and allergies in schoolchildren from rural Beijing, China. Pediatr Pulmonol. 2009;44(8):793–9.
Bartlett E, Parr J, Lindeboom W, Khanam MA, Koehlmoos TP. Sources and prevalence of self-reported asthma diagnoses in adults in urban and rural settings of Bangladesh. Glob Public Health. 2013;8(1):79–89.
Zheng M, Wang X, Bo M, Wang K, Zhao Y, He F, et al. Prevalence of allergic rhinitis among adults in urban and rural areas of China: a population-based cross-sectional survey. Allergy Asthma Immunol Res. 2015;7(2):148–57.
Wang XY, Zhuang Y, Ma TT, Zhang B, Wang XY. Prevalence of self-reported food allergy in six regions of inner Mongolia, northern China: a population-based survey. Med Sci Monit. 2018;24:1902–11.
Camargos PA, Castro RM, Feldman JS. Prevalence of symptoms related to asthma in school children of Campos Gerais, Brazil. Rev Panam Salud Publica. 1999;6(1):8–15.
Solis Soto MT, Patino A, Nowak D, Radon K. Prevalence of asthma, rhinitis and eczema symptoms in rural and urban school-aged children from Oropeza Province – Bolivia: a cross-sectional study. BMC Pulm Med. 2014;14:40.
Kalyoncu AF, Selcuk ZT, Enunlu T, Demir AU, Coplu L, Sahin AA, et al. Prevalence of asthma and allergic diseases in primary school children in Ankara, Turkey: two cross-sectional studies, five years apart. Pediatr Allergy Immunol. 1999;10(4):261–5.
Al Frayh AR, Shakoor Z, Gad El Rab MO, Hasnain SM. Increased prevalence of asthma in Saudi Arabia. Ann Allergy Asthma Immunol. 2001;86(3):292–6.
Ghozikali MG, Ansarin K, Naddafi K, Nodehi RN, Yaghmaeian K, Hassanvand MS, et al. Prevalence of asthma and associated factors among male late adolescents in Tabriz, Iran. Environ Sci Pollut Res Int. 2018;25(3):2184–93.
Razzaq S, Nafees AA, Rabbani U, Irfan M, Naeem S, Khan MA, et al. Epidemiology of asthma and associated factors in an urban Pakistani population: adult asthma study-Karachi. BMC Pulm Med. 2018;18(1):184.
Quah BS, Wan-Pauzi I, Ariffin N, Mazidah AR. Prevalence of asthma, eczema and allergic rhinitis: two surveys, 6 years apart, in Kota Bharu, Malaysia. Respirology. 2005;10(2):244–9.
Sharma SK, Banga A. Prevalence and risk factors for wheezing in children from rural areas of north India. Allergy Asthma Proc. 2007;28(6):647–53.
Pakhale S, Wooldrage K, Manfreda J, Anthonisen N. Prevalence of asthma symptoms in 7th- and 8th-grade school children in a rural region in India. J Asthma. 2008;45(2):117–22.
Agrawal S. Effect of indoor air pollution from biomass and solid fuel combustion on prevalence of self-reported asthma among adult men and women in India: findings from a nationwide large-scale cross-sectional survey. J Asthma. 2012;49(4):355–65.
Hong H, Yang Q, Zuo K, Chen X, Xia W, Lv M, et al. A hospital-based survey on the prevalence of bronchial asthma in patients with allergic rhinitis in southern China. Am J Rhinol Allergy. 2013;27(6):502–5.
Wang F, Wang M, Chen CB, Cai ZW, Wen DD, Chen FY, et al. Epidemiological analysis of childhood asthma in Yichang City, China. Zhongguo Dang Dai Er Ke Za Zhi. 2013;15(11):979–82.
Kumar P, Ram U. Patterns, factors associated and morbidity burden of asthma in India. PLoS One. 2017;12(10):e0185938.
Bhalla K, Nehra D, Nanda S, Verma R, Gupta A, Mehra S. Prevalence of bronchial asthma and its associated risk factors in school-going adolescents in Tier-III North Indian City. J Family Med Prim Care. 2018;7(6):1452–7.
Casagrande RR, Pastorino AC, Souza RG, Leone C, Sole D, Jacob CM. Asthma prevalence and risk factors in schoolchildren of the city of Sao Paulo, Brazil. Rev Saude Publica. 2008;42(3):517–23.
Soto-Quiros M, Bustamante M, Gutierrez I, Hanson LA, Strannegard IL, Karlberg J. The prevalence of childhood asthma in Costa Rica. Clin Exp Allergy. 1994;24(12):1130–6.
Dagoye D, Bekele Z, Woldemichael K, Nida H, Yimam M, Venn AJ, et al. Domestic risk factors for wheeze in urban and rural Ethiopian children. QJM. 2004;97(8):489–98.
Aggarwal AN, Chaudhry K, Chhabra SK, D’Souza GA, Gupta D, Jindal SK, et al. Prevalence and risk factors for bronchial asthma in Indian adults: a multicentre study. Indian J Chest Dis Allied Sci. 2006;48(1):13–22.
Dong GH, Ding HL, Ma YN, Jin J, Cao Y, Zhao YD, et al. Housing characteristics, home environmental factors and respiratory health in 14,729 Chinese children. Rev Epidemiol Sante Publique. 2008;56(2):97–107.
Gonzalez-Diaz SN, Del Rio-Navarro BE, Pietropaolo-Cienfuegos DR, Escalante-Dominguez AJ, Garcia-Almaraz RG, Merida-Palacio V, et al. Factors associated with allergic rhinitis in children and adolescents from northern Mexico: international study of asthma and allergies in childhood phase IIIB. Allergy Asthma Proc. 2010;31(4):e53–62.
Dhabadi BB, Athavale A, Meundi A, Rekha R, Suruliraman M, Shreeranga A, et al. Prevalence of asthma and associated factors among schoolchildren in rural South India. Int J Tuberc Lung Dis. 2012;16(1):120–5.
Coelho MA, de Pinho L, Marques PQ, Silveira MF, Sole D. Prevalence and factors associated with asthma in students from Montes Claros, Minas Gerais, Brazil. Cien Saude Colet. 2016;21(4):1207–16.
Bolat E, Arikoglu T, Sungur MA, Batmaz SB, Kuyucu S. Prevalence and risk factors for wheezing and allergic diseases in preschool children: a perspective from the Mediterranean coast of Turkey. Allergol Immunopathol (Madr). 2017;45(4):362–8.
Celedon JC, Soto-Quiros ME, Silverman EK, Hanson L, Weiss ST. Risk factors for childhood asthma in Costa Rica. Chest. 2001;120(3):785–90.
Al-Kubaisy W, Ali SH, Al-Thamiri D. Risk factors for asthma among primary school children in Baghdad, Iraq. Saudi Med J. 2005;26(3):460–6.
Uthaisangsook S. Risk factors for development of asthma in Thai adults in Phitsanulok: a university-based study. Asian Pac J Allergy Immunol. 2010;28(1):23–8.
Juca SC, Takano OA, Moraes LS, Guimaraes LV. Asthma prevalence and risk factors in adolescents 13 to 14 years of age in Cuiaba, Mato Grosso State, Brazil. Cad Saude Publica. 2012;28(4):689–97.
Bener A, al-Jawadi TQ, Ozkaragoz F, al-Frayh A, Gomes J. Bronchial asthma and wheeze in a desert country. Indian J Pediatr. 1993;60(6):791–7.
Civelek E, Sahiner UM, Yuksel H, Boz AB, Orhan F, Uner A, et al. Prevalence, burden, and risk factors of atopic eczema in schoolchildren aged 10–11 years: a national multicenter study. J Investig Allergol Clin Immunol. 2011;21(4):270–7.
Stephen GA, McRill C, Mack MD, O’Rourke MK, Flood TJ, Lebowitz MD. Assessment of respiratory symptoms and asthma prevalence in a U.S.-Mexico border region. Arch Environ Health. 2003;58(3):156–62.
Vedanthan PK, Mahesh PA, Vedanthan R, Holla AD, Liu AH. Effect of animal contact and microbial exposures on the prevalence of atopy and asthma in urban vs rural children in India. Ann Allergy Asthma Immunol. 2006;96(4):571–8.
Ngui R, Lim YA, Chow SC, de Bruyne JA, Liam CK. Prevalence of bronchial asthma among orang asli in peninsular Malaysia. Med J Malaysia. 2011;66(1):27–31.
Li J, Wang H, Chen Y, Zheng J, Wong GW, Zhong N. House dust mite sensitization is the main risk factor for the increase in prevalence of wheeze in 13- to 14-year-old schoolchildren in Guangzhou city, China. Clin Exp Allergy. 2013;43(10):1171–9.
Kurt E, Metintas S, Basyigit I, Bulut I, Coskun E, Dabak S, et al. Prevalence and risk factors of allergies in Turkey: results of a multicentric cross-sectional study in children. Pediatr Allergy Immunol. 2007;18(7):566–74.
Dong GH, Ma YN, Ding HL, Jin J, Cao Y, Zhao YD, et al. Effects of housing characteristics and home environmental factors on respiratory symptoms of 10,784 elementary school children from Northeast China. Respiration. 2008;76(1):82–91.
Zhang Y, Zhang L. Prevalence of allergic rhinitis in China. Allergy Asthma Immunol Res. 2014;6(2):105–13.
Yoshihara S, Munkhbayarlakh S, Makino S, Ito C, Logii N, Dashdemberel S, et al. Prevalence of childhood asthma in Ulaanbaatar, Mongolia in 2009. Allergol Int. 2016;65(1):62–7.
Rojas Molina N, Legorreta Soberanis J, Olvera GF. Prevalence and asthma risk factors in municipalities of the State of Guerrero, Mexico. Rev Alerg Mex. 2001;48(4):115–8.
Sriyaraj K, Priest N, Shutes B. Environmental factors influencing the prevalence of respiratory diseases and allergies among schoolchildren in Chiang Mai, Thailand. Int J Environ Health Res. 2008;18(2):129–48.
Kurt E, Metintas S, Basyigit I, Bulut I, Coskun E, Dabak S, et al. Prevalence and Risk Factors of Allergies in Turkey (PARFAIT): results of a multicentre cross-sectional study in adults. Eur Respir J. 2009;33(4):724–33.
Wang HY, Chen YZ, Ma Y, Wong GW, Lai CK, Zhong NS. Disparity of asthma prevalence in Chinese schoolchildren is due to differences in lifestyle factors. Zhonghua Er Ke Za Zhi. 2006;44(1):41–5.
Benicio MH, Ferreira MU, Cardoso MR, Konno SC, Monteiro CA. Wheezing conditions in early childhood: prevalence and risk factors in the city of Sao Paulo, Brazil. Bull World Health Organ. 2004;82(7):516–22.
Al-Mazam A, Mohamed AG. Risk factors of bronchial asthma in Bahrah, Saudi Arabia. J Family Community Med. 2001;8(1):33–9.
Dela Bianca A, Wandalsen G, Mallol J, Sole D. Risk factors for wheezing disorders in infants in the first year of life living in Sao Paulo, Brazil. J Trop Pediatr. 2012;58(6):501–4.
Baccioglu A, Sogut A, Kilic O, Beyhun E. The prevalence of allergic diseases and associated risk factors in school-age children and adults in Erzurum, Turkey. Turk Thorac J. 2015;16(2):68–72.
Wong GW, Ko FW, Hui DS, Fok TF, Carr D, von Mutius E, et al. Factors associated with difference in prevalence of asthma in children from three cities in China: multicentre epidemiological survey. BMJ. 2004;329(7464):486.
Hesse IF. Knowledge of asthma and its management in newly qualified doctors in Accra, Ghana. Respir Med. 1995;89(1):35–9.
Abudahish A, Bella H. Primary care physicians perceptions and practices on asthma care in Aseer region, Saudi Arabia. Saudi Med J. 2006;27(3):333–7.
Bhulani N, Lalani S, Ahmed A, Jan Y, Faheem U, Khan A, et al. Knowledge of asthma management by general practitioners in Karachi, Pakistan: comparison with international guidelines. Prim Care Respir J. 2011;20(4):448–51.
Jumbe Marsden E, Wa Somwe S, Chabala C, Soriano JB, Valles CP, Anchochea J. Knowledge and perceptions of asthma in Zambia: a cross-sectional survey. BMC Pulm Med. 2016;16:33.
Kouotou EA, Nansseu JR, Ngangue Engome AD, Tatah SA, Zoung-Kanyi Bissek AC. Knowledge, attitudes and practices of the medical personnel regarding atopic dermatitis in Yaounde, Cameroon. BMC Dermatol. 2017;17(1):1.
Urrutia-Pereira M, Fernandez C, Valentin-Rostan M, Cruz A, Torres O, Simon L, et al. Primary care physicians’ knowledge about allergic rhinitis and its impact on asthma (ARIA guidelines): a comparative Brazilian/Paraguayan/Uruguayan pilot study. Rev Alerg Mex. 2018;65(4):321–30.
Yilmaz O, Reisli I, Tahan F, Orhan F, Boz AB, Yuksel H. Influence of education on primary care physicians’ knowledge on childhood allergy as a systemic disease and the atopic march. Allergol Immunopathol (Madr). 2011;39(2):73–8.
Hussein S, Partridge M. Perceptions of asthma in south Asians and their views on educational materials and self-management plans: a qualitative study. Patient Educ Couns. 2002;48(2):189–94.
Osaretin OW, Uchechukwu ND, Osawaru O. Asthma management by medical practitioners: the situation in a developing country. World J Pediatr. 2013;9(1):64–7.
Hussain SF, Zahid S, Khan JA, Haqqee R. Asthma management by general practitioners in Pakistan. Int J Tuberc Lung Dis. 2004;8(4):414–7.
Chan YC, Tay YK, Sugito TL, Boediardja SA, Chau DD, Nguyen KV, et al. A study on the knowledge, attitudes and practices of Southeast Asian dermatologists in the management of atopic dermatitis. Ann Acad Med Singap. 2006;35(11):794–803.
Neffen H, Baena-Cagnani CE, Malka S, Sole D, Sepulveda R, Caraballo L, et al. Asthma mortality in Latin America. J Investig Allergol Clin Immunol. 1997;7(4):249–53.
Hounkpati A, Hounkpati HY, Kpanla E, Balogou KA, Tidjani O. Evaluation of asthma care in Africa. Rev Mal Respir. 2009;26(1):11–20.
Opedun N, Ehlers VJ, Roos JH. Compliance amongst asthma patients registered for an asthma disease risk-management programme in South Africa. Curationis. 2011;34(1):E1–8.
Chima EI, Iroezindu MO, Uchenna NR, Mbata GO, Okwuonu CG. A survey of asthma management practices and implementation of global initiative for asthma guidelines among doctors in a resource-limited setting in Nigeria. Niger J Clin Pract. 2017;20(8):984–91.
Badoum G, Ouedraogo SM, Lankoande H, Ouedraogo G, Boncoungou K, Bambara M, et al. Knowledge, attitudes and practices of general practitioners about asthma in the city of Ouagadougou. Mali Med. 2012;27(1):10–3.
Kotwani A, Chhabra SK, Tayal V, Vijayan VK. Quality of asthma management in an urban community in Delhi, India. Indian J Med Res. 2012;135:184–92.
Justin-Temu M, Risha P, Abla O, Massawe A. Incidence, knowledge and health seeking behaviour for perceived allergies at household level: a case study in Ilala district Dar es Salaam Tanzania. East Afr J Public Health. 2008;5(2):90–3.
Zhao J. Asthma control status in children and related factors in 29 cities of China. Zhonghua Er Ke Za Zhi. 2013;51(2):90–5.
Al-Khateeb AJ, Al Khateeb JM. Research on psychosocial aspects of asthma in the Arab world: a literature review. Multidiscip Respir Med. 2015;10(1):15.
Alzaabi A, Idrees M, Behbehani N, Khaitov MR, Tunceli K, Urdaneta E, et al. Cross-sectional study on asthma insights and management in the Gulf and Russia. Allergy Asthma Proc. 2018;39(6):430–6.
Urrutia-Pereira M, Mocellin LP, de Oliveira RB, Simon L, Lessa L, Sole D. Knowledge on asthma, food allergies, and anaphylaxis: assessment of elementary school teachers, parents/caregivers of asthmatic children, and university students in Uruguaiana, in the state of Rio Grande do Sul, Brazil. Allergol Immunopathol (Madr). 2018;46(5):421–30.
Mavale-Manuel S, Duarte N, Alexandre F, Albuquerque O, Scheinmann P, Poisson-Salomon AS, et al. Knowledge, attitudes, and behavior of the parents of asthmatic children in Maputo. J Asthma. 2004;41(5):533–8.
Sy DQ, Thanh Binh MH, Quoc NT, Hung NV, Quynh Nhu DT, Bao NQ, et al. Prevalence of asthma and asthma-like symptoms in Dalat Highlands, Vietnam. Singapore Med J. 2007;48(4):294–303.
Rastogi D, Gupta S, Kapoor R. Comparison of asthma knowledge, management, and psychological burden among parents of asthmatic children from rural and urban neighborhoods in India. J Asthma. 2009;46(9):911–5.
Salama AA, Mohammed AA, El Okda el SE, Said RM. Quality of care of Egyptian asthmatic children: clinicians adherence to asthma guidelines. Ital J Pediatr. 2010;36:33.
Al-Busaidi N, Habibulla Z, Bhatnagar M, Al-Lawati N, Al-Mahrouqi Y. The burden of asthma in Oman. Sultan Qaboos Univ Med J. 2015;15(2):e184–90.
Rezvanfar MA, Kebriaeezadeh A, Moein M, Nikfar S, Gharibnaseri Z, Abdollahi-Asl A. Cost analysis of childhood asthma in Iran: a cost evaluation based on referral center data for asthma and allergies. J Res Pharm Pract. 2013;2(4):162–8.
Chuesakoolvanich K. Cost of hospitalizing asthma patients in a regional hospital in Thailand. Respirology. 2007;12(3):433–8.
Handa S, Jain N, Narang T. Cost of care of atopic dermatitis in India. Indian J Dermatol. 2015;60(2):213.
Ibrahim WH, Suleiman NN, El-Allus F, Suleiman J, Elbuzidi AA, Guerrero MD, et al. The burden of adult asthma in a high GDP per capita country: the QASMA study. Ann Allergy Asthma Immunol. 2015;114(1):12–7.
Ding B, DiBonaventura M, Karlsson N, Ling X. A cross-sectional assessment of the prevalence and burden of mild asthma in urban China using the 2010, 2012, and 2013 China National Health and Wellness Surveys. J Asthma. 2017;54(6):632–43.
Mungan D, Aydin O, Mahboub B, Albader M, Tarraf H, Doble A, et al. Burden of disease associated with asthma among the adult general population of five Middle Eastern countries: results of the SNAPSHOT program. Respir Med. 2018;139:55–64.
Bavbek S, Mungan D, Turktas H, Misirligil Z, Gemicioglu B. A cost-of-illness study estimating the direct cost per asthma exacerbation in Turkey. Respir Med. 2011;105(4):541–8.
Ding B, Small M. Disease burden of mild asthma in China. Respirology. 2018;23(4):369–77.
Civelek E, Yavuz ST, Boz AB, Orhan F, Yuksel H, Uner A, et al. Epidemiology and burden of rhinitis and rhinoconjunctivitis in 9- to 11-year-old children. Am J Rhinol Allergy. 2010;24(5):364–70.
Nafti S, Taright S, El Ftouh M, Yassine N, Benkheder A, Bouacha H, et al. Prevalence of asthma in North Africa: the Asthma Insights and Reality in the Maghreb (AIRMAG) study. Respir Med. 2009;103(Suppl 2):S2–11.
Belhocine M, Ait-Khaled N. Prevalence of asthma in a region of Algeria. Bull Int Union Tuberc Lung Dis. 1991;66(2–3):91–3.
Arrais M, Lulua O, Quifica F, Rosado-Pinto J, Gama JMR, Taborda-Barata L. Prevalence of asthma, allergic rhinitis and eczema in 6–7-year-old schoolchildren from Luanda, Angola. Allergol Immunopathol (Madr). 2019;47(6):523–534.
Miningou SD, Zoubga AZ, Meda H, Meda N, Tiendrebeogo H. Prevalence of asthma in subjects aged 15-64 years in Bobo-Dioulasso (Burkina Faso) in 1998. Rev Pneumol Clin. 2002;58(6 Pt 1):341–5.
Pefura-Yone EW, Kengne AP, Balkissou AD, Boulleys-Nana JR, Efe-de-Melingui NR, Ndjeutcheu-Moualeu PI, et al. Prevalence of asthma and allergic rhinitis among adults in Yaounde, Cameroon. PLoS One. 2015;10(4):e0123099.
Mbatchou Ngahane BH, Afane Ze E, Nde F, Ngomo E, Mapoure Njankouo Y, Njock LR. Prevalence and risk factors for allergic rhinitis in bakers in Douala, Cameroon. BMJ Open. 2014;4(8):e005329.
Mugusi F, Edwards R, Hayes L, Unwin N, Mbanya JC, Whiting D, et al. Prevalence of wheeze and self-reported asthma and asthma care in an urban and rural area of Tanzania and Cameroon. Trop Dr. 2004;34(4):209–14.
Hailu S, Tessema T, Silverman M. Prevalence of symptoms of asthma and allergies in schoolchildren in Gondar town and its vicinity, northwest Ethiopia. Pediatr Pulmonol. 2003;35(6):427–32.
Melaku K, Berhane Y. Prevalence of wheeze and asthma related symptoms among school children in Addis Ababa, Ethiopia. Ethiop Med J. 1999;37(4):247–54.
Adeyemi AS, Akinboro AO, Adebayo PB, Tanimowo MO, Ayodele OE. The prevalence, risk factors and changes in symptoms of self reported asthma, rhinitis and eczema among pregnant women in Ogbomoso, Nigeria. J Clin Diagn Res. 2015;9(9):Oc01–7.
Hogewoning AA, Bouwes Bavinck JN, Amoah AS, Boakye DA, Yazdanbakhsh M, Kremsner PG, et al. Point and period prevalences of eczema in rural and urban schoolchildren in Ghana, Gabon and Rwanda. J Eur Acad Dermatol Venereol. 2012;26(4):488–94.
Roudaut M, Meda AH, Seka A, Fadiga D, Pigearias B, Akoto A. Prevalence of asthma and respiratory diseases in schools in Bouake (Ivory Coast): preliminary results. Med Trop (Mars). 1992;52(3):279–83.
Wolff PT, Arison L, Rahajamiakatra A, Raserijaona F, Niggemann B. High asthma prevalence and associated factors in urban malagasy schoolchildren. J Asthma. 2012;49(6):575–80.
Bouayad Z, Aichane A, Afif A, Benouhoud N, Trombati N, Chan-Yeung M, et al. Prevalence and trend of self-reported asthma and other allergic disease symptoms in Morocco: ISAAC phase I and III. Int J Tuberc Lung Dis. 2006;10(4):371–7.
Mavale-Manuel S, Joaquim O, Nunes E, Pedro A, Bandeira S, Eduardo E, et al. Prevalence of asthma-like symptoms by ISAAC video questionnaire in Mozambican schoolchildren. Monaldi Arch Chest Dis. 2006;65(4):189–95.
Falade AG, Ige OM, Yusuf BO, Onadeko MO, Onadeko BO. Trends in the prevalence and severity of symptoms of asthma, allergic rhinoconjunctivitis, and atopic eczema. J Natl Med Assoc. 2009;101(5):414–8.
Falade AG, Olawuyi JF, Osinusi K, Onadeko BO. Prevalence and severity of symptoms of asthma, allergic rhinoconjunctivitis, and atopic eczema in 6- to 7-year-old Nigerian primary school children: the international study of asthma and allergies in childhood. Med Princ Pract. 2004;13(1):20–5.
Falade AG, Olawuyi F, Osinusi K, Onadeko BO. Prevalence and severity of symptoms of asthma, allergic rhino-conjunctivitis and atopic eczema in secondary school children in Ibadan, Nigeria. East Afr Med J. 1998;75(12):695–8.
Hooper LG, Dieye Y, Ndiaye A, Diallo A, Fan VS, Neuzil KM, et al. Estimating pediatric asthma prevalence in rural senegal: a cross-sectional survey. Pediatr Pulmonol. 2017;52(3):303–9.
Herrant M, Loucoubar C, Boufkhed S, Bassene H, Sarr FD, Baril L, et al. Risk factors associated with asthma, atopic dermatitis and rhinoconjunctivitis in a rural Senegalese cohort. Allergy Asthma Clin Immunol. 2015;11(1):24.
Olaniyan T, Dalvie MA, Roosli M, Naidoo R, Kunzli N, de Hoogh K, et al. Asthma-related outcomes associated with indoor air pollutants among schoolchildren from four informal settlements in two municipalities in the Western Cape Province of South Africa. Indoor Air. 2019;29(1):89–100.
Teclessou JN, Mouhari-Toure A, Akakpo S, Bayaki S, Boukari OB, Elegbede YM, et al. Risk factors and allergic manifestations associated with atopic dermatitis in Lome (Togo): a multicenter study of 476 children aged 0–15 years. Med Sante Trop. 2016;26(1):88–91.
Sonia T, Meriem M, Yacine O, Nozha BS, Nadia M, Bechir L, et al. Prevalence of asthma and rhinitis in a Tunisian population. Clin Respir J. 2018;12(2):608–15.
Khaldi F, Fakhfakh R, Mattoussi N, Ben Ali B, Zouari S, Khemiri M. Prevalence and severity of asthma, allergic rhinoconjunctivitis and atopic eczema in “Grand Tunis” schoolchildren: ISAAC. Tunis Med. 2005;83(5):269–73.
Nantanda R, Ostergaard MS, Ndeezi G, Tumwine JK. Factors associated with asthma among under-fives in Mulago hospital, Kampala Uganda: a cross sectional study. BMC Pediatr. 2013;13:141.
Bemanin MH, Fallahpour M, Arshi S, Nabavi M, Yousofi T, Shariatifar A. First report of asthma prevalence in Afghanistan using international standardized methods. East Mediterr Health J. 2015;21(3):194–8.
Fazlollahi MR, Najmi M, Fallahnezhad M, Sabetkish N, Kazemnejad A, Bidad K, et al. Paediatric asthma prevalence: the first national population-based survey in Iran. Clin Respir J. 2019;13(1):14–22.
Alavinezhad A, Boskabady MH. The prevalence of asthma and related symptoms in Middle East countries. Clin Respir J. 2018;12(3):865–77.
Fazlollahi MR, Souzanch G, Nourizadeh M, Sabetkish N, Tazesh B, Entezari A, et al. The prevalence of allergic rhinitis and it’s relationship with second-hand tobacco smoke among adults in Iran. Acta Med Iran. 2017;55(11):712–7.
Varmaghani M, Farzadfar F, Sharifi F, Rashidian A, Moin M, Moradi-Lakeh M, et al. Prevalence of asthma, COPD, and chronic bronchitis in Iran: a systematic review and meta-analysis. Iran J Allergy Asthma Immunol. 2016;15(2):93–104.
Mehravar F, Rafiee S, Bazrafshan B, Khodadost M. Prevalence of asthma symptoms in Golestan schoolchildren aged 6–7 and 13–14 years in Northeast Iran. Front Med. 2016;10(3):345–50.
Mohammadbeigi A, Hassanzadeh J, Mousavizadeh A. Prevalence of asthma in elementary school age children in Iran--a systematic review and meta analysis study. Pak J Biol Sci. 2011;14(19):887–93.
Golshan M, Mohamad-Zadeh Z, Zahedi-Nejad N, Rostam-Poor B. Prevalence of asthma and related symptoms in primary school children of Isfahan, Iran, in 1998. Asian Pac J Allergy Immunol. 2001;19(3):163–70.
Khazaei HA, Hashemi SR, Aghamohammadi A, Farhoudi F, Rezaei N. The study of type 1 allergy prevalence among people of south-east of Iran by skin prick test using common allergens. Iran J Allergy Asthma Immunol. 2003;2(3):165–8.
Khatami A, Nassiri-Kashani M, Gorouhi F, Babakoohi S, Kazerouni-Timsar A, Davari P, et al. Allergic contact dermatitis to metal allergens in Iran. Int J Dermatol. 2013;52(12):1513–8.
Ahanchian H, Jafari S, Behmanesh F, Haghi NM, Nakhaei AA, Kiani MA, et al. Epidemiological survey of pediatric food allergy in Mashhad in Northeast Iran. Electron Physician. 2016;8(1):1727–32.
Moghtaderi M, Hosseini Teshnizi S, Farjadian S. Sensitization to common allergens among patients with allergies in major Iranian cities: a systematic review and meta-analysis. Epidemiol Health. 2017;39:e2017007.
Nabavi M, Lavavpour M, Arshi S, Bemanian MH, Esmaeilzadeh H, Molatefi R, et al. Characteristics, etiology and treatment of pediatric and adult anaphylaxis in Iran. Iran J Allergy Asthma Immunol. 2017;16(6):480–7.
Pereg D, Tirosh A, Lishner M, Goldberg A, Shochat T, Confino-Cohen R. Prevalence of asthma in a large group of Israeli adolescents: influence of country of birth and age at migration. Allergy. 2008;63(8):1040–5.
Magen E, Mishal J, Schlesinger M. Sensitizations to allergens of TRUE test in 864 consecutive eczema patients in Israel. Contact Dermatitis. 2006;55(6):370–1.
Abu-Ekteish F, Otoom S, Shehabi I. Prevalence of asthma in Jordan: comparison between Bedouins and urban schoolchildren using the international study of asthma and allergies in childhood phase III protocol. Allergy Asthma Proc. 2009;30(2):181–5.
Abdualrasool M, Al-Shanfari S, Booalayan H, Boujarwa A, Al-Mukaimi A, Alkandery O, et al. Exposure to environmental tobacco smoke and prevalence of atopic dermatitis among adolescents in Kuwait. Dermatology. 2018;234(5–6):186–91.
Ali F. A survey of self-reported food allergy and food-related anaphylaxis among young adult students at Kuwait University, Kuwait. Med Princ Pract. 2017;26(3):229–34.
Owayed A, Behbehani N, Al-Momen J. Changing prevalence of asthma and allergic diseases among Kuwaiti children. An ISAAC Study (Phase III). Med Princ Pract. 2008;17(4):284–9.
Behbehani NA, Abal A, Syabbalo NC, Abd Azeem A, Shareef E, Al-Momen J. Prevalence of asthma, allergic rhinitis, and eczema in 13- to 14-year-old children in Kuwait: an ISAAC study. International Study of Asthma and Allergies in Childhood. Ann Allergy Asthma Immunol. 2000;85(1):58–63.
Ramadan FM, Khoury MN, Hajjar TA, Mroueh SM. Prevalence of allergic diseases in children in Beirut: comparison to worldwide data. J Med Liban. 1999;47(4):216–21.
Qasem JA, Nasrallah H, Al-Khalaf BN, Al-Sharifi F, Al-Sherayfee A, Almathkouri SA, et al. Meteorological factors, aeroallergens and asthma-related visits in Kuwait: a 12-month retrospective study. Ann Saudi Med. 2008;28(6):435–41.
Almutairi N, Almutawa F. Allergic contact dermatitis pattern in Kuwait: nickel leads the pack. In-depth analysis of nickel allergy based on the results from a large prospective patch test series report. Postepy Dermatol Alergol. 2017;34(3):207–15.
Alkazemi D, Albeajan M, Kubow S. Early infant feeding practices as possible risk factors for immunoglobulin E-mediated food allergies in Kuwait. Int J Pediatr. 2018;2018:1701903.
Irani C, Maalouly G. Prevalence of self-reported food allergy in Lebanon: a Middle-Eastern taste. Int Sch Res Notices. 2015;2015:639796.
Musharrafieh U, Al-Sahab B, Zaitoun F, El-Hajj MA, Ramadan F, Tamim H. Prevalence of asthma, allergic rhinitis and eczema among Lebanese adolescents. J Asthma. 2009;46(4):382–7.
Waked M, Salameh P. Risk factors for asthma and allergic diseases in school children across Lebanon. J Asthma Allergy. 2008;2:1–7.
Al-Rawas OA, Al-Maniri AA, Al-Riyami BM. Home exposure to Arabian incense (bakhour) and asthma symptoms in children: a community survey in two regions in Oman. BMC Pulm Med. 2009;9:23.
Al-Rawas OA, Al-Riyami BM, Al-Kindy H, Al-Maniri AA, Al-Riyami AA. Regional variation in the prevalence of asthma symptoms among Omani school children: comparisons from two nationwide cross-sectional surveys six years apart. Sultan Qaboos Univ Med J. 2008;8(2):157–64.
Al-Riyami BM, Al-Rawas OA, Al-Riyami AA, Jasim LG, Mohammed AJ. A relatively high prevalence and severity of asthma, allergic rhinitis and atopic eczema in schoolchildren in the Sultanate of Oman. Respirology. 2003;8(1):69–76.
Shafique RH, Akhter S, Abbas S, Ismail M. Sensitivity to house dust mite allergens and prevalence of allergy-causing house dust mite species in Pothwar, Pakistan. Exp Appl Acarol. 2018;74(4):415–26.
Hasnain SM, Khan M, Saleem A, Waqar MA. Prevalence of asthma and allergic rhinitis among school children of Karachi, Pakistan, 2007. J Asthma. 2009;46(1):86–90.
Inam M, Shafique RH, Roohi N, Irfan M, Abbas S, Ismail M. Prevalence of sensitization to food allergens and challenge proven food allergy in patients visiting allergy centers in Rawalpindi and Islamabad, Pakistan. Springerplus. 2016;5(1):1330.
El-Sharif NA, Nemery B, Barghuthy F, Mortaja S, Qasrawi R, Abdeen Z. Geographical variations of asthma and asthma symptoms among schoolchildren aged 5 to 8 years and 12 to 15 years in Palestine: the International Study of Asthma and Allergies in Childhood (ISAAC). Ann Allergy Asthma Immunol. 2003;90(1):63–71.
El-Sharif N, Abdeen Z, Qasrawi R, Moens G, Nemery B. Asthma prevalence in children living in villages, cities and refugee camps in Palestine. Eur Respir J. 2002;19(6):1026–34.
Mohamed Hussain S, Ayesha Farhana S, Mohammed AS. Time trends and regional variation in prevalence of asthma and associated factors in Saudi Arabia: a systematic review and meta-analysis. Biomed Res Int. 2018;2018:8102527.
Alruwaili MF, Elwan A. Prevalence of asthma among male 16 to 18-year-old adolescents in the Northern Borders Region of Saudi Arabia. Electron Physician. 2018;10(6):6920–6.
Al Ghobain MO, Algazlan SS, Oreibi TM. Asthma prevalence among adults in Saudi Arabia. Saudi Med J. 2018;39(2):179–84.
Moradi-Lakeh M, El Bcheraoui C, Daoud F, Tuffaha M, Kravitz H, Al Saeedi M, et al. Prevalence of asthma in Saudi adults: findings from a national household survey, 2013. BMC Pulm Med. 2015;15:77.
Nahhas M, Bhopal R, Anandan C, Elton R, Sheikh A. Prevalence of allergic disorders among primary school-aged children in Madinah, Saudi Arabia: two-stage cross-sectional survey. PLoS One. 2012;7(5):e36848.
Al Ghobain MO, Al-Hajjaj MS, Al Moamary MS. Asthma prevalence among 16- to 18-year-old adolescents in Saudi Arabia using the ISAAC questionnaire. BMC Public Health. 2012;12:239.
Sobki SH, Zakzouk SM. Point prevalence of allergic rhinitis among Saudi children. Rhinology. 2004;42(3):137–40.
Bener A, al-Jawadi TQ, Ozkaragoz F, Anderson JA. Prevalence of asthma and wheeze in two different climatic areas of Saudi Arabia. Indian J Chest Dis Allied Sci. 1993;35(1):9–15.
Alqahtani JM, Asaad AM, Awadalla NJ, Mahfouz AA. Environmental determinants of bronchial asthma among Saudi school children in Southwestern Saudi Arabia. Int J Environ Res Public Health. 2016;14(1):22.
Dogruel D, Bingol G, Yilmaz M, Altintas DU. The ADAPAR birth cohort study: food allergy results at five years and new insights. Int Arch Allergy Immunol. 2016;169(1):57–61.
Dogruel D, Bingol G, Altintas DU, Yilmaz M, Kendirli SG. Prevalence of and risk factors for atopic dermatitis: a birth cohort study of infants in Southeast Turkey. Allergol Immunopathol (Madr). 2016;44(3):214–20.
Tamay Z, Akcay A, Ergin A, Guler N. Prevalence of allergic rhinitis and risk factors in 6- to 7-yearold children in Istanbul, Turkey. Turk J Pediatr. 2014;56(1):31–40.
Talay F, Kurt B, Tug T, Kurt OK, Goksugur N, Yasar Z. The prevalence of asthma and allergic diseases among adults 30–49 years of age in Bolu, Western Black Sea Region of Turkey. Clin Ter. 2014;165(1):e59–63.
Duksal F, Becerir T, Ergin A, Akcay A, Guler N. The prevalence of asthma diagnosis and symptoms is still increasing in early adolescents in Turkey. Allergol Int. 2014;63(2):189–97.
Duksal F, Akcay A, Becerir T, Ergin A, Becerir C, Guler N. Rising trend of allergic rhinitis prevalence among Turkish schoolchildren. Int J Pediatr Otorhinolaryngol. 2013;77(9):1434–9.
Civelek E, Cakir B, Boz AB, Yuksel H, Orhan F, Uner A, et al. Extent and burden of allergic diseases in elementary schoolchildren: a national multicenter study. J Investig Allergol Clin Immunol. 2010;20(4):280–8.
Gelincik A, Buyukozturk S, Gul H, Isik E, Issever H, Ozseker F, et al. Confirmed prevalence of food allergy and non-allergic food hypersensitivity in a Mediterranean population. Clin Exp Allergy. 2008;38(8):1333–41.
Selcuk ZT, Caglar T, Enunlu T, Topal T. The prevalence of allergic diseases in primary school children in Edirne, Turkey. Clin Exp Allergy. 1997;27(3):262–9.
Orhan F, Karakas T, Cakir M, Aksoy A, Baki A, Gedik Y. Prevalence of immunoglobulin E-mediated food allergy in 6-9-year-old urban schoolchildren in the eastern Black Sea region of Turkey. Clin Exp Allergy. 2009;39(7):1027–35.
Kurt E, Demir AU, Cadirci O, Yildirim H, Ak G, Eser TP. Occupational exposures as risk factors for asthma and allergic diseases in a Turkish population. Int Arch Occup Environ Health. 2011;84(1):45–52.
Akcay A, Tamay Z, Hocaoglu AB, Ergin A, Guler N. Risk factors affecting asthma prevalence in adolescents living in Istanbul, Turkey. Allergol Immunopathol (Madr). 2014;42(5):449–58.
Haktanir Abul M, Dereci S, Hacisalihoglu S, Orhan F. Is kiwifruit allergy a matter in kiwifruit-cultivating regions? A population-based study. Pediatr Allergy Immunol. 2017;28(1):38–43.
Ozdemir SK, Ozguvarsigmalu S. Pollen food allergy syndrome in Turkey: clinical characteristics and evaluation of its association with skin test reactivity to pollens. Asian Pac J Allergy Immunol. 2018;36(2):77–81.
Zhang Y, Chen Y, Zhao A, Li H, Mu Z, Zhang Y, et al. Prevalence of self-reported food allergy and food intolerance and their associated factors in 3–12 year-old children in 9 areas in China. Wei Sheng Yan Jiu. 2015;44(2):226–31.
Du EC, Li ZM, Sui C, Wang W, Zhang QX. Relationship between asthma and allergic antigens in rural houses. Biomed Environ Sci. 1993;6(1):27–30.
Norback D, Lu C, Wang J, Zhang Y, Li B, Zhao Z, et al. Asthma and rhinitis among Chinese children – indoor and outdoor air pollution and indicators of socioeconomic status (SES). Environ Int. 2018;115:1–8.
Guo X, Li Z, Ling W, Long J, Su C, Li J, et al. Epidemiology of childhood asthma in mainland China (1988–2014): a meta-analysis. Allergy Asthma Proc. 2018;39(3):15–29.
Guo Y, Li P, Tang J, Han X, Zou X, Xu G, et al. Prevalence of atopic dermatitis in Chinese children aged 1–7 ys. Sci Rep. 2016;6:29751.
Huang C, Liu W, Hu Y, Zou Z, Zhao Z, Shen L, et al. Updated prevalences of asthma, allergy, and airway symptoms, and a systematic review of trends over time for childhood asthma in Shanghai, China. PLoS One. 2015;10(4):e0121577.
Sha L, Shao M, Liu C, Li S, Li Z, Luo Y, et al. The prevalence of asthma in children: a comparison between the year of 2010 and 2000 in urban China. Zhonghua Jie He He Hu Xi Za Zhi. 2015;38(9):664–8.
Zeng GQ, Luo JY, Huang HM, Zheng PY, Luo WT, Wei NL, et al. Food allergy and related risk factors in 2540 preschool children: an epidemiological survey in Guangdong Province, southern China. World J Pediatr. 2015;11(3):219–25.
Yang Z, Zheng W, Yung E, Zhong N, Wong GW, Li J. Frequency of food group consumption and risk of allergic disease and sensitization in school children in urban and rural China. Clin Exp Allergy. 2015;45(12):1823–32.
Wang Y, Sai X, Sun Y, Zheng Y. A cross sectional survey on the prevalence of food intolerance and its determinants through physical checkup programs in the elderly. Zhonghua Liu Xing Bing Xue Za Zhi. 2014;35(11):1249–51.
Xiong M, Ni C, Pan JH, Wang Q, Zheng LL. Epidemiological survey of childhood asthma in Hefei City, China. Zhongguo Dang Dai Er Ke Za Zhi. 2013;15(2):109–11.
Chang ML, Shao B, Liu YH, Li LL, Pei LC, Wang BY. Analysis of allergens in 5 473 patients with allergic diseases in Harbin, China. Biomed Environ Sci. 2013;26(11):886–93.
Hao GD, Zheng YW, Gjesing B, Kong XA, Wang JY, Song ZJ, et al. Prevalence of sensitization to weed pollens of Humulus scandens, Artemisia vulgaris, and Ambrosia artemisiifolia in northern China. J Zhejiang Univ Sci B. 2013;14(3):240–6.
Chen J, Liao Y, Zhang HZ, Zhao H, Chen J, Li HQ. Prevalence of food allergy in children under 2 years of age in three cities in China. Zhonghua Er Ke Za Zhi. 2012;50(1):5–9.
Gu JL, Ma HL, Zheng YJ. Epidemiological survey of asthma in children aged 0–14 years in the Futian District of Shenzhen, China between 2010 and 2011. Zhongguo Dang Dai Er Ke Za Zhi. 2012;14(12):918–23.
Li F, Zhou Y, Li S, Jiang F, Jin X, Yan C, et al. Prevalence and risk factors of childhood allergic diseases in eight metropolitan cities in China: a multicenter study. BMC Public Health. 2011;11:437.
Sai XY, Zheng YS, Zhao JM, Hao W. A cross sectional survey on the prevalence of food intolerance and its determinants in Beijing, China. Zhonghua Liu Xing Bing Xue Za Zhi. 2011;32(3):302–5.
Zhao J, Bai J, Shen KL, Xiang L, Huang Y, Huang S, et al. Questionnaire-based survey of allergic diseases among children aged 0–14 years in the downtown of Beijing, Chongqing and Guangzhou. Zhonghua Er Ke Za Zhi. 2011;49(10):740–4.
Hu Y, Chen J, Li H. Comparison of food allergy prevalence among Chinese infants in Chongqing, 2009 versus 1999. Pediatr Int. 2010;52(5):820–4.
Zhao J, Bai J, Shen K, Xiang L, Huang S, Chen A, et al. Self-reported prevalence of childhood allergic diseases in three cities of China: a multicenter study. BMC Public Health. 2010;10:551.
Chen J, Hu Y, Allen KJ, Ho MH, Li H. The prevalence of food allergy in infants in Chongqing, China. Pediatr Allergy Immunol. 2011;22(4):356–60.
Han DM, Zhang L, Huang D, Wu YF, Dong Z, Xu G, et al. Self-reported prevalence of allergic rhinitis in eleven cities in China. Zhonghua Er Bi Yan Hou Tou Jing Wai Ke Za Zhi. 2007;42(5):378–84.
Wong GW, Leung TF, Ma Y, Liu EK, Yung E, Lai CK. Symptoms of asthma and atopic disorders in preschool children: prevalence and risk factors. Clin Exp Allergy. 2007;37(2):174–9.
Chen YZ. A nationwide survey in China on prevalence of asthma in urban children. Zhonghua Er Ke Za Zhi. 2003;41(2):123–7.
Wang W, Huang X, Chen Z, Zheng R, Chen Y, Zhang G, et al. Prevalence and trends of sensitisation to aeroallergens in patients with allergic rhinitis in Guangzhou, China: a 10-year retrospective study. BMJ Open. 2016;6(5):e011085.
Li J, Huang Y, Lin X, Zhao D, Tan G, Wu J, et al. Factors associated with allergen sensitizations in patients with asthma and/or rhinitis in China. Am J Rhinol Allergy. 2012;26(2):85–91.
Saha GK. House dust mite allergy in Calcutta, India: evaluation by RAST. Ann Allergy. 1993;70(4):305–9.
Chhabra SK, Gupta CK, Chhabra P, Rajpal S. Prevalence of bronchial asthma in schoolchildren in Delhi. J Asthma. 1998;35(3):291–6.
Awasthi S, Kalra E, Roy S, Awasthi S. Prevalence and risk factors of asthma and wheeze in school-going children in Lucknow, North India. Indian Pediatr. 2004;41(12):1205–10.
Kasera R, Singh BP, Lavasa S, Prasad KN, Sahoo RC, Singh AB. Kidney bean: a major sensitizer among legumes in asthma and rhinitis patients from India. PLoS One. 2011;6(11):e27193.
Dey D, Ghosh N, Pandey N, Gupta BS. A hospital-based survey on food allergy in the population of Kolkata, India. Int Arch Allergy Immunol. 2014;164(3):218–21.
Singh S, Sharma BB, Sharma SK, Sabir M, Singh V. Prevalence and severity of asthma among Indian school children aged between 6 and 14 years: associations with parental smoking and traffic pollution. J Asthma. 2016;53(3):238–44.
Shaikh WA, Shaikh SW. Allergies in India: an analysis of 3389 patients attending an allergy clinic in Mumbai, India. J Indian Med Assoc. 2008;106(4):220, 2, 4 passim.
Kumar GS, Roy G, Subitha L, Sahu SK. Prevalence of bronchial asthma and its associated factors among school children in urban Puducherry, India. J Nat Sci Biol Med. 2014;5(1):59–62.
Nitin J, Palagani R, Shradha NH, Vaibhav J, Kowshik K, Manoharan R, et al. Prevalence, severity and risk factors of allergic disorders among people in south India. Afr Health Sci. 2016;16(1):201–9.
Phathammavong O, Ali M, Phengsavanh A, Xaysomphou D, Odajima H, Nishima S, et al. Prevalence and potential risk factors of rhinitis and atopic eczema among schoolchildren in Vientiane capital, Lao PDR: ISAAC questionnaire. Biosci Trends. 2008;2(5):193–9.
Quah BS, Razak AR, Hassan MH. Prevalence of asthma, rhinitis and eczema among schoolchildren in Kelantan, Malaysia. Acta Paediatr Jpn. 1997;39(3):329–35.
Sam CK, Kesavan P, Liam CK, Soon SC, Lim AL, Ong EK. A study of pollen prevalence in relation to pollen allergy in Malaysian asthmatics. Asian Pac J Allergy Immunol. 1998;16(1):1–4.
Quah BS, Mazidah AR, Hamzah AM, Simpson H. Prevalence of wheeze, night cough and doctor-diagnosed asthma in pre-school children in Kota Bharu. Asian Pac J Allergy Immunol. 2000;18(1):15–21.
Sonomjamts M, Dashdemberel S, Logii N, Nakae K, Chigusa Y, Ohhira S, et al. Prevalence of asthma and allergic rhinitis among adult population in Ulaanbaatar, Mongolia. Asia Pac Allergy. 2014;4(1):25–31.
Shek LP, Cabrera-Morales EA, Soh SE, Gerez I, Ng PZ, Yi FC, et al. A population-based questionnaire survey on the prevalence of peanut, tree nut, and shellfish allergy in 2 Asian populations. J Allergy Clin Immunol. 2010;126(2):324–31, 31.e1–7.
Connett GJ, Gerez I, Cabrera-Morales EA, Yuenyongviwat A, Ngamphaiboon J, Chatchatee P, et al. A population-based study of fish allergy in the Philippines, Singapore and Thailand. Int Arch Allergy Immunol. 2012;159(4):384–90.
Amarasekera ND, Gunawardena NK, de Silva NR, Weerasinghe A. Prevalence of childhood atopic diseases in the Western Province of Sri Lanka. Ceylon Med J. 2010;55(1):5–8.
de Silva NR, Dasanayake WM, Karunatilleke C, Malavige GN. Food dependant exercise induced anaphylaxis a retrospective study from 2 allergy clinics in Colombo, Sri Lanka. Allergy Asthma Clin Immunol. 2015;11(1):22.
Seneviratne R, Gunawardena NS. Prevalence and associated factors of wheezing illnesses of children aged three to five years living in under-served settlements of the Colombo Municipal Council in Sri Lanka: a cross-sectional study. BMC Public Health. 2018;18(1):127.
Vichyanond P, Jirapongsananuruk O, Visitsuntorn N, Tuchinda M. Prevalence of asthma, rhinitis and eczema in children from the Bangkok area using the ISAAC (International Study for Asthma and Allergy in Children) questionnaires. J Med Assoc Thail. 1998;81(3):175–84.
Teeratakulpisarn J, Wiangnon S, Kosalaraksa P, Heng S. Surveying the prevalence of asthma, allergic rhinitis and eczema in school-children in Khon Kaen, Northeastern Thailand using the ISAAC questionnaire: phase III. Asian Pac J Allergy Immunol. 2004;22(4):175–81.
Uthaisangsook S. Prevalence of asthma, rhinitis, and eczema in the university population of Phitsanulok, Thailand. Asian Pac J Allergy Immunol. 2007;25(2–3):127–32.
Boonchai W, Iamtharachai P, Sunthonpalin P. Prevalence of allergic contact dermatitis in Thailand. Dermatitis. 2008;19(3):142–5.
Lam HT, Ronmark E, Tu’o’ng NV, Ekerljung L, Chuc NT, Lundback B. Increase in asthma and a high prevalence of bronchitis: results from a population study among adults in urban and rural Vietnam. Respir Med. 2011;105(2):177–85.
Lam HT, Ekerljung L, Bjerg A, Van TTN, Lundback B, Ronmark E. Sensitization to airborne allergens among adults and its impact on allergic symptoms: a population survey in northern Vietnam. Clin Transl Allergy. 2014;4(1):6.
Toizumi M, Hashizume M, Nguyen HAT, Yasunami M, Kitamura N, Iwasaki C, et al. Asthma, rhinoconjunctivitis, eczema, and the association with perinatal anthropometric factors in Vietnamese children. Sci Rep. 2019;9(1):2655.
Le TTK, Nguyen DH, Vu ATL, Ruethers T, Taki AC, Lopata AL. A cross-sectional, population-based study on the prevalence of food allergies among children in two different socio-economic regions of Vietnam. Pediatr Allergy Immunol. 2019;30(3):348–55.
Sole D, Yamada E, Vana AT, Costa-Carvalho BT, Naspitz CK. Prevalence of asthma and related symptoms in school-age children in Sao Paulo, Brazil–International Study of Asthma and Allergies in Children (ISAAC). J Asthma. 1999;36(2):205–12.
De Britto MC, Bezerra PG, Ferreira OS, Maranhao IC, Trigueiro GA. Asthma prevalence in schoolchildren in a city in north-east Brazil. Ann Trop Paediatr. 2000;20(2):95–100.
Vanna AT, Yamada E, Arruda LK, Naspitz CK, Sole D. International Study of Asthma and Allergies in Childhood: validation of the rhinitis symptom questionnaire and prevalence of rhinitis in schoolchildren in Sao Paulo, Brazil. Pediatr Allergy Immunol. 2001;12(2):95–101.
Maia JG, Marcopito LF, Amaral AN, Tavares Bde F, Santos FA. Prevalence of asthma and asthma symptoms among 13 and 14-year-old schoolchildren, Brazil. Rev Saude Publica. 2004;38(2):292–9.
Rios JL, Boechat JL, Sant’Anna CC, Franca AT. Atmospheric pollution and the prevalence of asthma: study among schoolchildren of 2 areas in Rio de Janeiro, Brazil. Ann Allergy Asthma Immunol. 2004;92(6):629–34.
Sole D, Camelo-Nunes IC, Vana AT, Yamada E, Werneck F, de Freitas LS, et al. Prevalence of rhinitis and related-symptoms in schoolchildren from different cities in Brazil. Allergol Immunopathol (Madr). 2004;32(1):7–12.
Neto AC, Annes RD, Wolff NM, Klein AP, Dos Santos FC, Dullius JL, et al. Prevalence and severity of asthma, rhinitis, and atopic eczema in 13- to 14-year-old schoolchildren from southern Brazil. Allergy Asthma Clin Immunol. 2006;2(1):3–10.
Sole D, Wandalsen GF, Camelo-Nunes IC, Naspitz CK. Prevalence of symptoms of asthma, rhinitis, and atopic eczema among Brazilian children and adolescents identified by the International Study of Asthma and Allergies in Childhood (ISAAC) – Phase 3. J Pediatr. 2006;82(5):341–6.
Kuschnir FC, Cunha AJ, Braga Dde A, Silveira HH, Barroso MH, Aires ST. Asthma in 13-14-year-old schoolchildren in the city of Nova Iguacu, Rio de Janeiro State, Brazil: prevalence, severity, and gender differences. Cad Saude Publica. 2007;23(4):919–26.
Sole D, Camelo-Nunes IC, Wandalsen GF, Rosario Filho NA, Naspitz CK. Prevalence of rhinitis among Brazilian schoolchildren: ISAAC phase 3 results. Rhinology. 2007;45(2):122–8.
Sole D, Camelo-Nunes IC, Wandalsen GF, Mallozi MC, Naspitz CK. Is the prevalence of asthma and related symptoms among Brazilian children related to socioeconomic status? J Asthma. 2008;45(1):19–25.
Castro LK, Cerci Neto A, Ferreira Filho OF. Prevalence of symptoms of asthma, rhinitis and atopic eczema among students between 6 and 7 years of age in the city of Londrina, Brazil. J Bras Pneumol. 2010;36(3):286–92.
Wehrmeister FC, Peres KG. Regional inequalities in the prevalence of asthma diagnosis in children: an analysis of the Brazilian National Household Sample Survey, 2003. Cad Saude Publica. 2010;26(9):1839–52.
Toledo MF, Rozov T, Leone C. Prevalence of asthma and allergies in 13- to 14-year-old adolescents and the frequency of risk factors in carriers of current asthma in Taubate, Sao Paulo, Brazil. Allergol Immunopathol (Madr). 2011;39(5):284–90.
Sousa CA, Cesar CL, Barros MB, Carandina L, Goldbaum M, Pereira JC. Prevalence of asthma and risk factors associated: population based study in Sao Paulo, Southeastern Brazil, 2008–2009. Rev Saude Publica. 2012;46(5):825–33.
Oliveira-Santos S, Motta-Franco J, Barreto I, Sole D, Gurgel R. Asthma in adolescents--prevalence trends and associated factors in Northeast Brazil. Allergol Immunopathol (Madr). 2015;43(5):429–35.
Goncalves LC, Guimaraes TC, Silva RM, Cheik MF, de Ramos Napolis AC, Barbosa ESG, et al. Prevalence of food allergy in infants and pre-schoolers in Brazil. Allergol Immunopathol (Madr). 2016;44(6):497–503.
Toledo MF, Saraiva-Romanholo BM, Oliveira RC, Saldiva PH, Silva LF, Nascimento LF, et al. Changes over time in the prevalence of asthma, rhinitis and atopic eczema in adolescents from Taubate, Sao Paulo, Brazil (2005–2012): relationship with living near a heavily travelled highway. Allergol Immunopathol (Madr). 2016;44(5):439–44.
Kuschnir FC, Alves da Cunha AJ. Environmental and socio-demographic factors associated to asthma in adolescents in Rio de Janeiro, Brazil. Pediatr Allergy Immunol. 2007;18(2):142–8.
de Magalhaes Simoes S, da Cunha SS, Cruz AA, Dias KC, Alcantara-Neves NM, Amorim LD, et al. A community study of factors related to poorly controlled asthma among Brazilian urban children. PLoS One. 2012;7(5):e37050.
Barreto BA, Sole D. Prevalence of asthma and associated factors in adolescents living in Belem (Amazon region), Para, Brazil. Allergol Immunopathol (Madr). 2014;42(5):427–32.
Mallol J, Cortez E, Amarales L, Sanchez I, Calvo M, Soto S, et al. Prevalence of asthma in Chilean students. Descriptive study of 24,470 children. ISAAC-Chile. Rev Med Chil. 2000;128(3):279–85.
Hoyos-Bachiloglu R, Ivanovic-Zuvic D, Alvarez J, Linn K, Thone N, de los Angeles Paul M, et al. Prevalence of parent-reported immediate hypersensitivity food allergy in Chilean school-aged children. Allergol Immunopathol (Madr). 2014;42(6):527–32.
Caraballo L, Cadavid A, Mendoza J. Prevalence of asthma in a tropical city of Colombia. Ann Allergy. 1992;68(6):525–9.
Marrugo J, Hernandez L, Villalba V. Prevalence of self-reported food allergy in Cartagena (Colombia) population. Allergol Immunopathol (Madr). 2008;36(6):320–4.
Penaranda A, Aristizabal G, Garcia E, Vasquez C, Rodriguez-Martinez CE. Rhinoconjunctivitis prevalence and associated factors in school children aged 6-7 and 13-14 years old in Bogota, Colombia. Int J Pediatr Otorhinolaryngol. 2012;76(4):530–5.
Garcia E, Aristizabal G, Vasquez C, Rodriguez-Martinez CE, Sarmiento OL, Satizabal CL. Prevalence of and factors associated with current asthma symptoms in school children aged 6-7 and 13-14 yr old in Bogota, Colombia. Pediatr Allergy Immunol. 2008;19(4):307–14.
Soto-Quiros ME, Soto-Martinez M, Hanson LA. Epidemiological studies of the very high prevalence of asthma and related symptoms among school children in Costa Rica from 1989 to 1998. Pediatr Allergy Immunol. 2002;13(5):342–9.
Tatto-Cano MI, Sanin-Aguirre LH, Gonzalez V, Ruiz-Velasco S, Romieu I. Prevalence of asthma, rhinitis and eczema in school children in the city of Cuernavaca, Mexico. Salud Publica Mex. 1997;39(6):497–506.
Rodriguez A, Vaca M, Oviedo G, Erazo S, Chico ME, Teles C, et al. Urbanisation is associated with prevalence of childhood asthma in diverse, small rural communities in Ecuador. Thorax. 2011;66(12):1043–50.
Rodriguez A, Vaca MG, Chico ME, Rodrigues LC, Barreto ML, Cooper PJ. Lifestyle domains as determinants of wheeze prevalence in urban and rural schoolchildren in Ecuador: cross sectional analysis. Environ Health. 2015;14:15.
Thongkham D, Tran J, Clunes MT, Brahim F. Prevalence and severity of asthmatic symptoms in Grenadian school children: the Grenada National Asthma Survey. BMJ Open. 2015;5(10):e008557.
Draaisma E, Garcia-Marcos L, Mallol J, Sole D, Perez-Fernandez V, Brand PL. A multinational study to compare prevalence of atopic dermatitis in the first year of life. Pediatr Allergy Immunol. 2015;26(4):359–66.
Kahwa EK, Waldron NK, Younger NO, Edwards NC, Knight-Madden JM, Bailey KA, et al. Asthma and allergies in Jamaican children aged 2-17 years: a cross-sectional prevalence survey. BMJ Open. 2012;2(4):e001132.
Garcia CR. Air-borne allergens and respiratory allergy in the state of Oaxaca, Mexico. Rev Alerg. 1991;38(3):85–7.
Baeza Bacab MA, Grahma Zapata LF. Prevalence of asthma. Survey of a school population in Villahermosa, Tabasco, Mexico. Rev Alerg. 1992;39(2):32–6.
Avila Castanon L, Perez Lopez J, del Rio Navarro BE, Rosas Vargas MA, Lerma Ortiz L, Sienra Monge JJ. Hypersensitivity detected by skin tests to food in allergic patients in the Hospital Infantil de Mexico Federico Gomez. Rev Alerg Mex. 2002;49(3):74–9.
Cisneros Perez V, Alvarado EC. Prevalence of allergic rhinitis in Durango, Mexico. Rev Alerg Mex. 2004;51(2):49–53.
Baeza Bacab MA, Davila Velazquez JR, Loeza Medina SR. Prevalence of positive skin tests to indoor allergens in preschooler children with respiratory allergy in Merida, Yucatan, Mexico. Rev Alerg Mex. 2005;52(6):237–42.
Del-Rio-Navarro B, Del Rio-Chivardi JM, Berber A, Sienra-Monge JJ, Rosas-Vargas MA, Baeza-Bacab M. Asthma prevalence in children living in north Mexico City and a comparison with other Latin American cities and world regions. Allergy Asthma Proc. 2006;27(4):334–40.
Barraza-Villarreal A, Hernandez-Cadena L, Moreno-Macias H, Ramirez-Aguilar M, Romieu I. Trends in the prevalence of asthma and other allergic diseases in schoolchildren from Cuernavaca, Mexico. Allergy Asthma Proc. 2007;28(3):368–74.
Rodriguez Orozco AR, Nunez Tapia RM. Prevalence of atopic dermatitis in 6–14 year old children in Morelia, Michoacan, Mexico. Rev Alerg Mex. 2007;54(1):20–3.
Esquivel CA, Perez VC, Arredondo DM, Iturbide MS, Hernandez Ade L, Arellano AG. Prevalence of asthma in Tepehuano and Mestizo school children from Durango, Mexico. Rev Alerg Mex. 2008;55(5):189–95.
Lopez Campos C, Carrillo Lucero JM, Lopez Campos JE, Rincon Castaneda C, Velasco Gutierrez JM, Cairo Cueto SM, et al. Prevalence and severity of asthma in 6 and 7 year-old children from Torreon, Coahuila, Mexico. Rev Alerg Mex. 2008;55(4):148–52.
Bedolla Barajas M, Barrera Zepeda AT, Morales RJ. Atopic dermatitis in scholar children from Ciudad Guzman, Mexico. Prevalence and related factors. Rev Alerg Mex. 2010;57(3):71–8.
Bedolla-Barajas M, Cuevas-Rios G, Garcia-Barboza E, Barrera-Zepeda AT, Morales-Romero J. Prevalence and associated factors to allergic rhinitis in school children of ciudad Guzman, Mexico. Rev Investig Clin. 2010;62(3):244–51.
Bedolla-Barajas M, Morales-Romero J, Hernandez-Colin DD, Arevalo-Cruz D. Prevalence of sensitization to the most common allergens in elderly patients from the Western of Mexico. Rev Alerg Mex. 2012;59(3):131–8.
Bedolla-Barajas M, Morales-Romero J, Robles-Figueroa M, Fregoso-Fregoso M. Asthma in late adolescents of Western Mexico: prevalence and associated factors. Arch Bronconeumol. 2013;49(2):47–53.
Bedolla-Barajas M, Bedolla-Pulido TR, Macriz-Romero N, Morales-Romero J, Robles-Figueroa M. Prevalence of peanut, tree nut, sesame, and seafood allergy in Mexican adults. Rev Investig Clin. 2015;67(6):379–86.
Medina-Hernandez A, Huerta-Hernandez RE, Gongora-Melendez MA, Dominguez-Silva MG, Mendoza-Hernandez DA, Romero-Tapia SJ, et al. Clinical-epidemiological profile of patients with suspicion of alimentary allergy in Mexico. Mexipreval study. Rev Alerg Mex. 2015;62(1):28–40.
Ontiveros N, Valdez-Meza EE, Vergara-Jimenez MJ, Canizalez-Roman A, Borzutzky A, Cabrera-Chavez F. Parent-reported prevalence of food allergy in Mexican schoolchildren: a population-based study. Allergol Immunopathol (Madr). 2016;44(6):563–70.
Mancilla-Hernandez E, Gonzalez-Solorzano EVM, Medina-Avalos MA, Barnica-Alvarado RH. Prevalence of allergic rhinitis and its symptoms in the school children population of Cuernavaca, Morelos, Mexico. Rev Alerg Mex. 2017;64(3):243–9.
Martin M, Sauer T, Alarcon JA, Vinoles J, Walter EC, Ton TG, et al. Prevalence and impact of asthma among school-aged students in Lima, Peru. Int J Tuberc Lung Dis. 2017;21(11):1201–5.
Bordel-Gomez MT, Miranda-Romero A, Castrodeza-Sanz J. Epidemiology of contact dermatitis: prevalence of sensitization to different allergens and associated factors. Actas Dermosifiliogr. 2010;101(1):59–75.
Monteil MA, Joseph G, Changkit C, Wheeler G, Antoine RM. Comparison of prevalence and severity of asthma among adolescents in the Caribbean islands of Trinidad and Tobago: results of a nationwide cross-sectional survey. BMC Public Health. 2005;5:96.
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2020 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Eghtesad, S. (2020). Allergic Diseases in the Developing World: An Emerging Problem or an Overseen Issue?. In: Mahdavinia, M. (eds) Health Disparities in Allergic Diseases. Springer, Cham. https://doi.org/10.1007/978-3-030-31222-0_2
Download citation
DOI: https://doi.org/10.1007/978-3-030-31222-0_2
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-31221-3
Online ISBN: 978-3-030-31222-0
eBook Packages: MedicineMedicine (R0)