Abstract
We describe a case of double tachycardia with a continuous fast/slow atrioventricular nodal reentrant tachycardia and a repetitive left fascicular ventricular tachycardia (VT) during which a transformation between wide QRS complex tachycardia and narrow QRS complex tachycardia was repeatedly seen. The coexistence of idiopathic left fascicular VT and supra-ventricular tachycardia is an uncommon but a possible condition since left fascicular VT can be initiated by atrial stimulus. Making an accurate diagnosis was a key to successful catheter ablation of the tachycardias.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Atrioventricular nodal reentrant tachycardia
- Catheter ablation
- Double tachycardia
- His-ventricular interval
- Left fascicular ventricular tachycardia
- Verapamil-sensitive
1 Case Summary
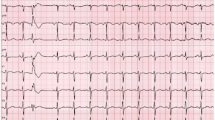
A 29-year-old male with no apparent structural heart disease was referred for catheter ablation of recurrent wide QRS complex tachycardia (W-Tach) with a right bundle branch block morphology and superior axis deviation (QRS duration 120 ms; QRS axis −142°). The tachycardia was not affected by intravenous administration of adenosine but was terminated with intravenous verapamil. The 12-lead electrocardiogram during sinus rhythm (SR) (sinus cycle length [CL], 720 ms) was unremarkable with normal atrio-His (AH) (75 ms) and His-ventricular (HV) (40 ms) intervals. An atrial extra-stimulus induced the tachycardia without an AH jump. During tachycardia, a transformation between narrow QRS and W-Tach (asterisk) with an unchanged CL of 370 ms was repeatedly seen (Fig. 101.1). The QRS morphology of the W-Tach was identical to the clinical tachycardia, whereas the QRS morphology of the narrow QRS complex tachycardia (N-Tach) was identical to that observed during SR. What are the mechanisms of the tachycardia?
2 Case Discussion
A 1:1 atrio-ventricular (AV) relationship and the same atrial activation sequence were maintained despite the change in the QRS morphology. The issue is whether these represent two tachycardias or one tachycardia with two different QRS morphologies. The HV interval is a key to differentiating supraventricular tachycardia (SVT) from ventricular tachycardia (VT) . While the HV interval during the N-Tach was the same as that during SR, the HV interval during the W-Tach was much shorter than that during SR. One possible mechanism is ventricular pre-excitation via a left-sided accessory pathway; however, this is unlikely since no ventricular pre-excitation was observed during atrial extra-stimulus or constant pacing with a different CL. Thus, W-Tach is highly likely to be VT. In addition, the His-bundle potentials were activated antegradely during W-Tach, which indicates that SVT continued even during W-Tach.
The earliest atrial activation was located in the coronary sinus ostium. We gave the overdrive pacing and scanning from the ventricle systematically in order to diagnose the SVT; however, reproducible results could not be obtained due to the frequent transformation of the tachycardias. Then, we delivered ventricular extra-stimulus during a drive train given simultaneously to the atrium and the ventricle (Fig. 101.2a–c). A decremental VA conduction was seen and the conducted atrial sequence was identical to that during SVT. The SVT was resumed with a V-A-V activation sequence. These findings suggest that the SVT was either fast-slow (F/S) AV nodal reentrant tachycardia (AVNRT) or orthodromic AV reentrant tachycardia (ORT). During this protocol, the CL of the induced SVT was 355 ms and the CL of W-Tach was 350–360 ms. At the beginning of W-Tach, the activation sequences of His-bundle potential were changed, and the H-H interval was shortened. Since the VT became sustainable with a gradual shortening of the CL of the VT, the left ventricle was mapped with an ablation catheter. The diastolic Purkinje potentials (P1) were recorded near the posterior papillary muscle (Fig. 101.3a) [1]. The VT was entrained, and the post-pacing interval (VTCL+25 ms) suggested that P1 was on the VT circuit. The diagnosis was made as the left fascicular VT. After the VT was successfully treated with P1-guided ablation, the SVT was only induced with ventricular extra-stimulus. A ventricular stimulus given on the refractory period of the His-bundle did not reset the SVT (Fig. 101.3b), neglecting the possibility of ORT. The diagnosis of F/S AVNRT was made, and slow pathway ablation was successfully performed.
(a–c) Premature ventricular stimulation (V2) during a drive train (V1, 300 ms) given simultaneously to the atrium and the ventricle with V1–V2 260 ms (a), 240 ms (b), and 220 ms (c). A decremental VA conduction was seen, and the conducted atrial sequence was identical to that during tachycardia. The narrow QRS complex tachycardia (N-Tach) was resumed with a V-A-V activation sequence. The findings suggest that the N-Tach was either fast-slow AV nodal reentrant tachycardia or orthodromic AV reentrant tachycardia. At the beginning of the wide QRS complex tachycardia (W-Tach), the activation sequences of the His-bundle potential were changed, and the H-H interval was shortened. Thus, the W-Tach was highly likely to be ventricular tachycardia. CS coronary sinus, HRA high right atrium, HIS His bundle, RVA right ventricular apex, d distal, p proximal
(a, b) Left fascicular ventricular tachycardia (a) and fast-slow atrioventricular nodal reentrant tachycardia (b). A ventricular stimulus given on the refractory period of the His bundle did not reset the long RP’ tachycardia. CS coronary sinus, HRA high right atrium, H His bundle potential, HIS His bundle, LV left ventricle, P1 diastolic Purkinje potential, RVA right ventricular apex, S stimulus, d distal, m mid, p proximal
In summary, the case represents double tachycardia with a continuous F/S AVNRT and a repetitive left fascicular VT. Diagnosing double tachycardia may be challenging, especially when it is combined with a transformation between W-Tach and N-Tach. Since left fascicular VT can be initiated by atrial stimulus [2], the coexistence of idiopathic left fascicular VT and SVT is a possible condition [3,4,5]. Keeping this in mind may help in performing an accurate diagnosis.
References
Komatsu Y, Nogami A, Kurosaki K, Morishima I, Masuda K, Ozawa T, et al. Fascicular ventricular tachycardia originating from papillary muscles: Purkinje network involvement in the reentrant circuit. Circ Arrhythm Electrophysiol. 2017;10(3):e004549.
Zipes DP, Foster PR, Troup PJ, Pedersen DH. Atrial induction of ventricular tachycardia: reentry versus triggered automaticity. Am J Cardiol. 1979;44:1–8.
Wagshal AB, Mittleman RS, Schuger CD, Huang SK. Coincident idiopathic left ventricular tachycardia and atrioventricular nodal reentrant tachycardia: control by radiofrequency catheter ablation of the slow atrioventricular nodal pathway. Pacing Clin Electrophysiol. 1994;17(3 Pt 1):386–96.
Watanabe I, Kunimoto S, Kondo K, Kojima T, Nakai T, Shindo A, et al. Radiofrequency catheter ablation of coexistent atrioventricular reciprocating tachycardia and left ventricular tachycardia originating in the left anterior fascicle. Jpn Circ J. 1999;63:223–7.
Weng KP, Chiou CW, Kung MH, Lin CC, Hsieh KS. Radiofrequency catheter ablation of coexistent idiopathic left ventricular tachycardia and atrioventricular nodal reentrant tachycardia. J Chin Med Assoc. 2005;68:479–83.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2020 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Morishima, I., Nogami, A. (2020). A Case of Tachycardia Transformation Between Narrow and Wide QRS Complex. In: Natale, A., Wang, P., Al-Ahmad, A., Estes, N. (eds) Cardiac Electrophysiology. Springer, Cham. https://doi.org/10.1007/978-3-030-28533-3_101
Download citation
DOI: https://doi.org/10.1007/978-3-030-28533-3_101
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-28531-9
Online ISBN: 978-3-030-28533-3
eBook Packages: MedicineMedicine (R0)