Abstract
Congenital pituitary hormone deficiency is a disabling condition. It is part of a spectrum of disorders including craniofacial midline developmental defects ranging from holoprosencephaly through septo-optic dysplasia to combined and isolated pituitary hormone deficiency. The first genes discovered in the human disease were based on mouse models of dwarfism due to mutations in transcription factor genes. High-throughput DNA sequencing technologies enabled clinicians and researchers to find novel genetic causes of hypopituitarism for the more than three quarters of patients without a known genetic diagnosis to date. Transcription factor (TF) genes are at the forefront of the functional analysis of novel variants of unknown significance due to the relative ease in in vitro testing in a research lab. Genetic testing in hypopituitarism is of high importance to the individual and their family to predict phenotype composition, disease progression and to avoid life-threatening complications such as secondary adrenal insufficiency.
This chapter aims to highlight our current understanding about (1) the contribution of TF genes to pituitary development (2) the diversity of inheritance and phenotype features in combined and select isolated pituitary hormone deficiency and (3) provide an initial assessment on how to approach variants of unknown significance in human hypopituitarism. Our better understanding on how transcription factor gene variants lead to hypopituitarism is a meaningful step to plan advanced therapies to specific genetic changes in the future.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Pituitary hormone deficiency
- Transcription factor
- Inheritance
- Genetic testing
- Variants of unknown significance
1 Introduction
1.1 Incidence and Diagnosis of Human Hypopituitarism
Hypopituitarism affects around 1 in 4000 live births (Castinetti et al. 2012, 2008a; Regal et al. 2001). Combined pituitary hormone deficiency (CPHD) is defined by the deficiency of GH (growth hormone) and at least one more hormone of TSH, ACTH, LH, FSH, PRL (thyroid-stimulating hormone, adrenocorticotropic hormone, luteinizing hormone, follicle-stimulating hormone, and prolactin, respectively). The incidence of CPHD is estimated to be 1:8000 according to the Genetics Home Reference at the National Institutes of Health (ghr.nlm.nih.gov). The most common pituitary hormone deficient is GH in 1:4000–1:10,000 individuals (Alatzoglou and Dattani 2010), while other isolated pituitary hormone deficiencies are rare. Congenital hypothyroidism has an incidence of 1:3000 (Grosse and Van Vliet 2011), isolated hypogonadotropic hypogonadism (isolated HH) has an incidence under 1:10,000 and is frequently associated with anosmia/hyposmia (Hayes et al. 1998; Seminara et al. 2000). The incidence of congenital isolated ACTH (corticotrope) deficiency (IAD) is largely unknown (Patti et al. 2018). Overall, this places hypopituitarism in the upper end of rare diseases (Richter et al. 2015).
Genetic factors substantially influence height, and short stature is a common cause for referrals to endocrinologists (Pfäffle 2006). The diagnosis of pituitary hormone deficiency is based on guidelines by professional organizations and medical institutes (Ergin et al. 2015). We refer to these for specific details regarding the clinical diagnosis of growth hormone deficiency (GHD) in children (Chinoy and Murray 2016), GHD in adults (Molitch et al. 2011), congenital HH (Boehm et al. 2015) and congenital central hypothyroidism (Leger et al. 2014). Guidelines are not yet established for isolated ACTH deficiency (IAD) (Andrioli et al. 2006) or PRL deficiency in particular. The focus of this chapter is to explore the non-acquired/genetic causes with special attention to transcription factor (TF) genes.
Transcription factors are widely recognized as regulators of pituitary development. Mouse models provided the fundamental evidence for their role in pituitary development; however, not all of the orthologous human genes turned out to be involved in human pituitary disease. An extensive list of TFs involved in vertebrate pituitary development is provided in Table 13.1 [TF classification is based on http://tfclass.bioinf.med.uni-goettingen.de (Wingender et al. 2015)].
Around 2000 TFs are known today. Nearly a third of them are known to have functions during development. They are classified based on protein domains and about 80% of all TFs have C2H2-zinc-finger, homeodomain or helix-loop-helix motifs (Vaquerizas et al. 2009). Most of the genes currently known in the pathogenesis of human isolated growth hormone deficiency (IGHD) or CPHD are TFs discussed in this review. Genes predominantly involved in HH are discussed elsewhere (Maione et al. 2018). Also, those genes that are involved in signaling (BMP4, CDON, FGF8, FGFR1, GPR161, HHIP, IGSF1, PROKR2, SHH, WDR11), RNA processing (EIF2B5, HNRNPU, POLR3A, RBM28, RNPC3), and other processes (CHD7, IFT72, 52KCNQ1, PNPLA6, ZSWIM6) (Di Iorgi et al. 2016; Fang et al. 2016b; Norppa et al. 2018; Tommiska et al. 2017) are not the focus of this review.
1.2 Why Does Genetic Diagnosis Matter in Hypopituitarism?
About 15% of CPHD cases have mutations in PROP1, POU1F1, LHX3, LHX4, or HESX1 but systematic screens have not been done for all genes implicated in the disorder (De Rienzo et al. 2015; Fang et al. 2016b). Genetic diagnosis in hypopituitarism has consequences for disease progression and family screening. The international GENHYPOPIT network—with more than 1200 patients (Brue 2018)—reported that only ~25% of their GHD patients were diagnosed neonatally, 32% during puberty, and about 10% well into adulthood (Brue et al. 2017). Pituitary hormone deficiency can evolve over the course of time; therefore, intermittent screening for new hormone deficiency is warranted. For example, IGHD diagnosed in childhood can evolve to CPHD with TSH and LH deficiency in young adulthood, and with ACTH deficiency later in adulthood (>30 year) (Brue et al. 2017; Coya et al. 2007; Halasz et al. 2006). While some gene deficiencies present with a consistent phenotype (PROP1, POU1F1), incomplete penetrance and variable expressivity pose a challenge in predicting pituitary disease progression and extra-pituitary manifestations (i.e., LHX4, GLI2). The size of the pituitary is often smaller than normal in patients with hypopituitarism; however, patients with PROP1 variants may exhibit pituitary hyperplasia and apparent dynamic changes in the organ size (waxing and waning) (Obermannova et al. 2011; Turton et al. 2005a). The diagnosis of PROP1 variants in these cases can prevent invasive procedures and spontaneous regression can be anticipated (Dattani 2005). Additionally, the rationale for genetic testing of close family members is quintessential to prevent serious/life-threatening conditions such as secondary adrenal insufficiency (Pekic et al. 2011).
1.3 Genetic Diagnostics in Hypopituitarism
Endocrinologists and medical geneticists typically share the responsibility of establishing the genetic diagnosis in hypopituitarism. There is no “state of the art” hypopituitarism-specific genetic diagnostics guideline published by a medical society to date. Family history is the most essential component in the analysis. To identify the genetic origin for hypopituitarism it is important to consider several genetic models: (1) large families with multiple affected individuals suggesting a dominant inheritance; (2) consanguineous families where the odds for recessive disorders is increased; or (3) trios with an affected child with at least one unaffected parent, suggesting incompletely penetrant dominant, recessive, or de novo variants in the proband. In addition, people from the Iberian Peninsula or Lithuania have a higher probability of carrying one of the two founder mutations of PROP1 (Dusatkova et al. 2016).
The technology used to detect genetic changes includes single gene Sanger sequencing, panel sequencing of the most well-established genes, or next-generation sequencing technologies to assess coding regions genome-wide (Whole Exome Sequencing—WES). Single gene sequencing revealed that around 11% of CPHD patients had variants in PROP1, whereas POU1F1, LHX4, LHX3, and HESX1 were around 1% each, respectively (Fang et al. 2016b). In most diseases the overall genetic diagnosis “solve rate” of WES is ~30% and that would be an excellent progress from the current 15% at best with traditional methods (Trujillano et al. 2017). Papers reporting on results with whole genome sequencing are scarce in hypopituitarism. Only a few publications provide insight into the incidence of larger, chromosomal changes. Copy number variations account for ~8% of the congenital hypopituitarism cases (Correa et al. 2018; Dateki et al. 2010a; Takagi et al. 2015). Recently, a targeted version of WES using the principle of molecular inversion probes was reported to screen 51 patients for 30 known and 37 candidate genes, which has excellent perspectives in screening and identifying more novel variants (Perez Millan et al. 2018).
2 Pituitary Gland Structure, Function, and Development
2.1 The Structure of the Pituitary: “One Gland Above All”
The pituitary is the major neuroendocrine gland serving as a key hub between the central nervous system (CNS) and the majority of endocrine organs. The mammalian pituitary can be divided into three lobes: anterior (AL), intermediate (IL), and posterior (PL). The AL and IL are derived from the evaginating oral ectoderm (Rathke’s cleft) and ensphere both the stalk and the anterolateral aspect of the PL. The IL is rudimentary in humans and a common site for cystic lesions (Rathke’s cleft cysts). A fine mesh of a portal vessel system in the anterior lobe allows direct communication from the hypothalamus to the pituitary through blood flow. The axon terminals are surrounded by glial-like cell types (pituicytes) and form the posterior lobe (PL) (Goto et al. 2015).
2.2 The Basic Function of the Pituitary
Pituitary function is essential in growth, fertility, lactation, stress response, and general homeostasis. The anterior lobe has five major cell types producing six major hormones: somatotrophs (producing GH); lactotrophs (PRL); melano-corticotropes (POMC) and its cleavage products: ACTH, α-MSH; thyrotrophs (TSH); and gonadotrophs (LH, FSH). TSH, FSH, and LH are heterodimers of the choriogonadotropin alpha subunit (CGA) and specific beta subunits TSHB, FSHB, and LHB, respectively. The proportion of these cell types is unequal in the adult pituitary such as ~40% are somatotrophs, ~40% lactotrophs, ~10% gonadotrophs, 10% corticotropes, and only 5% are thyrotropes (Kulig et al. 1998). While these make up the majority of resident cells in the AL, there is a fraction that is hormone negative and includes non-differentiated stem cells, progenitor cells, folliculostellate cells, endothelial cells, pericytes, and mesenchymal cells. Defects leading to the loss of predominant cell types can frequently result in a hypoplastic AL (Gangat and Radovick 2017). The PL contains the axon terminals of hypothalamic neurons in the supraoptic and paraventricular nuclei producing arginine-vasopressin (AVP) and oxytocin (OXT). While AVP and OXT are stored in the terminals they are surrounded by a subset of glial-like cells (Goto et al. 2015). Single cell sequencing technologies did not reveal a new major physiological cell type so far but a better resolution of known cell types important in critical stages of development, adaptation to stimuli and neoplasia are highly anticipated (Cheung et al. 2018).
3 Lessons from Mouse Pituitary Development to Human Hypopituitarism
3.1 Early Patterning of the Pituitary Primordium
Spatiotemporal expression of TFs in the ventral diencephalon and the oral ectoderm results in the formation of the AL/IL/PL between mouse E9 and E12 days. In addition to a severe pituitary abnormality, a wide spectrum of features is present when specific TFs are disrupted. Defects in Pitx2, Isl1, Nkx2.1 result in complex anomalies involving the CNS, the eyes, and multiple non-ectodermal organs such as the heart and the thyroid. Hesx1, Vax1, Pax6, Otx2, Six3, Six6 deficient mice present with CNS, eye, and other malformations predominantly in the head region (McCabe and Dattani 2014). Others show CNS abnormalities and disorders affecting the ventral motor neurons [Lhx3/Lhx4, (Gergics et al. 2015)], segmental bone formation [Gli2, (Haddad-Tovolli et al. 2015)] or the gonads [Sox3, (Rizzoti et al. 2004)]. Sox2 is essential in the specification of all pituitary hormone producing and folliculostellate cells and is considered as a signature pituitary stem cell marker (Fauquier et al. 2008). Sox2/Sox9 co-expressing cells are regarded as committed progenitor cells in the pituitary (Rizzoti et al. 2013).
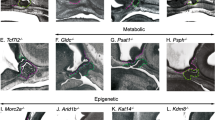
Pituitary organogenesis and hormone cell specification are outlined in Figs. 13.1 and 13.2.
Schematic development of the pituitary in the mouse and human in the midsagittal plane. By mouse embryonic day E16.5, the organ reaches its final shape. Several signaling pathways regulate pituitary development. A continuous Shh expression gets interrupted by Wnt signaling from the diencephalon at E9.5 and the Rathke’s pouch protrudes from the rooftop of the oral cavity. These events result in altered expressions of Bmps and Fgfs and define the pituitary organizer domain of the ventral diencephalon [references within Osmundsen et al. (2017)]. Fgf and Notch signaling orchestrate the evagination of the hypothalamic floor plate of the third ventricle to form the infundibulum and the subsequent PL (Goto et al. 2015)
Involvement of transcription factors in the development hormone producing cells in the pituitary anterior lobe. Multiple transcription factors (TFs) participate in the specification of pituitary hormone producing cells. Details of the three main phases of pituitary development are described in the main text. Asterisk: Supernumerary pituitary gland formation is noted in the—Bmp inhibitor—Noggin −/− (Davis and Camper 2007), Tg(Cga-Fgf8)Rsd (Treier et al. 2001), Six3 +/− Hesx1 cre/+ (Gaston-Massuet et al. 2008), and Vax1 −/− mice (Bharti et al. 2011). In the differentiation phase certain TFs are needed for multiple lineages. For example, Gata2 is a major factor in the transcriptional regulation of Cga, Tshb, Lhb (Dasen et al. 1999). An array of steroid/retinoid/thyroid hormone receptor stimulation is also needed for physiological pituitary hormone expression. Solid arrows mark upstream/downstream relation between factors but do not necessarily mark direct regulation. Dotted curve represents repressive relationship. Acronyms in bold are TFs and correspond to the Table 13.1
3.2 Progenitor Cell Determination
Prop1 (Prophet of Pit1) is a key pituitary-specific TF (Sornson et al. 1996). All pituitary hormone producing cell types go through a Prop1 expressing progenitor stage (Davis et al. 2016). Its main downstream target Pou1f1 is a lineage determining factor for somatolactotrophs and most thyrotrophs (Li et al. 1990). Insm1 is key in the differentiation of multiple neuroendocrine cell types. In the absence of Insm1, the Sox2/Sox9+ pituitary stem/progenitor cell pool is maintained, lineage-specific transcription factors (Pou1f1, Tbx19, NeuroD1, Nr5a1) are moderately expressed, but all GH, TSH, LH/FSH cells are missing, and PRL, ACTH, and αMSH cell numbers are drastically reduced (Welcker et al. 2013).
3.3 Differentiation Phase
The POU1F1 Lineage (Somatolactotrophs and Thyrotrophs)
Pou1f1 (formerly Pit-1) is a signature pituitary transcription factor that directly regulates the transcription of Gh, Prl, Tshb, and Cga (Gordon et al. 1993; Li et al. 1990). A cluster of thyrotrophs in the rostral tip develops independently of Pou1f1 (Lin et al. 1994). Notable significant other factors for this lineage are: Neurod4 (Ando et al. 2018), Foxo1 (Kapali et al. 2016) for somatotrophs, the estrogen receptor for lactotrophs (Day et al. 1990), and thyrotroph embryonic factor (TEF) for thyrotrophs (Drolet et al. 1991).
Gonadotroph and Melanocorticotroph Lineages
Nr5a1 (previously known as Sf1) is a hallmark TF for gonadotroph commitment (Zhao et al. 2001). Egr1 is expressed predominantly in gonadotrophs (Man et al. 2014). Tbx19 (previously known as Tpit) is a signature TF of melanocorticotrope commitment and in the transcriptional regulation of POMC (Budry et al. 2011). Pax7 is a pioneer transcription factor acting as a selector to melanotrope over corticotrope faith through chromatin remodeling (Budry et al. 2012). The expression of specific proprotein convertases (PC or PCSK) is key in the differential cleavage of POMC (Marcinkiewicz et al. 1993).
4 Human Gene Variants in Pituitary Hormone Deficiency
4.1 Interpretation of Novel Genes/Variants in the Era of Whole Exome/Genome Sequencing
The discovery of specific genes in hypopituitarism started in the 1990s with Pou1f1 about 60 years after the discovery of the Snell dwarf (Pou1f1 dw/dw) (Li et al. 1990). A dozen other genes such as PROP1, HESX1, LHX3, LHX4 were described in human hypopituitarism in the next two decades. Thanks to the Human Genome Project and the availability of Sanger sequencing, genetic testing improved for patients with hypopituitarism. Single gene sequencing was amenable as long as a limited number of candidate genes needed to be screened. As the number of candidate genes increased, automated panel sequencing took over (Klee et al. 2011).
The rise of next-generation sequencing technologies from around 2007 changed the landscape dramatically and dozens of novel candidate genes and variants were identified in a decade (Warr et al. 2015). This flipped the order such that the candidate genes and variants were found in the human first and then functional studies in cell lines and vertebrate model organisms were implemented to discern the pathogenicity and disease mechanism. In this new era, the most difficult task is to evaluate the many novel genes and variants with unknown significance (VUS).
Analyzing VUS in patients with hypopituitarism is of utmost importance since less than 15% of hypopituitarism patients have a genetic diagnosis (De Rienzo et al. 2015; Fang et al. 2016b). Professional organizations such as the American College of Medical Genetics (ACMG), the Association for Molecular Pathology (AMP) (Richards et al. 2015), ClinGen Sequence Variant Interpretation (SVI) Working Group (ClinGen SVI WG) (Strande et al. 2017) in the USA, or the Association for Clinical Genomic Science in the UK developed recommendations for variant interpretation. This effort is ongoing and expanding to develop some disease-specific guidelines as well. These recommendations classify VUS based on evidence of (1) known physiological expression and function, (2) changes in these when the variant is present, as well as on (3) animal and in vitro model systems and rescue experiments corresponding to the human disease.
Initial evaluation of VUS includes the assessment of the (1) probability for loss of intolerance (pLI) of the gene; (2) frequency of the VUS in a matched population [e.g., Genome Aggregation Database (gnomAD), gnomad.broadinstitute.org (Lek et al. 2016)]; (3) protein structure and function prediction combined with evolutionary conservation [e.g. Combined Annotation Dependent Depletion (CADD), cadd.gs.washington.edu, (Rentzsch et al. 2019)].
A more detailed analysis includes investigation of (4) spatial and temporal expression of the mRNA/protein especially in the disease-affected tissues (postnatally, e.g., Genotype-Tissue Expression (GTEx) project, gtexportal.org/home/, Tabula Muris, tabula-muris.ds.czbiohub.org (Schaum et al. 2018), The Human Protein Atlas www.proteinatlas.org/humanproteome/tissue) or embryonic ages (Brinkmeier et al. 2009; Ma et al. 2009) (5) knockout vertebrate models (e.g., Mouse Genome Informatics: www.informatics.jax.org/phenotypes.shtml, The Zebrafish Information Network zfin.org).
These surveys can support the role of a VUS but further (6) in vitro and (7) in vivo vertebrate studies are necessary to elevate the level of proof for pathogenicity. The in vitro studies need to demonstrate the biological difference between the wild type and the variant protein. The more elegant approach uses cultured native cells from healthy and affected individuals, or immortalized or engineered cells such as induced pluripotent stem cells (iPS) or CRISPR-edited cells (Strande et al. 2017). Established in vitro assays are excellent to use if they are available, but many times there is no available assay and the validation of a new one can be tedious. In vivo studies still pose the greatest bottleneck in the analysis as time to generate a mouse carrying the orthologous VUS can be at least 6 months. Other model systems like the Zebrafish are excellent for knock-down and rescue experiments in a shorter time frame (Davis et al. 2014).
4.2 TF Gene Variants in Patients with Hypopituitarism
4.2.1 TF Gene Variants in Patients with Combined Pituitary Hormone Deficiency and Isolated Growth Hormone Deficiency
This chapter has two comprehensive goals for clinicians and researchers who encounter patients with hypopituitarism: (1) to describe the landscape of genetic and phenotypic heterogeneity in hypopituitarism and (2) to create a resource for the first steps of in vitro testing for VUS in select hypopituitarism genes based on published scenarios.
Phenotypic Heterogeneity in Hypopituitarism
The majority of human genes tested in patients with CPHD, IGHD, IAD to date are TFs, which are illustrated in Tables 13.2, 13.3, and 13.4. We aimed to collect information on the genetics and common phenotypic features of around 300 probands and families. Due to space limitations of this chapter not all original references could be cited.
An Approach to Perform In Vitro Testing of VUS in TF Genes
One can achieve a detailed analysis on a computer for a small set of novel genes/variants in a shorter time; however, the next step is frequently to start in vitro testing. A generalized view of active TFs is that they localize to the nucleus, bind to specific promoter/enhancer DNA sequences with partner proteins, and change the mRNA expression of target genes (Vaquerizas et al. 2009). Loss of function (nonsense and select frame shift) variants may require little to no testing if the gene is sensitive to haploinsufficiency indicated by dominant inheritance and a high pLI score (Lek et al. 2016) (Tables 13.2 and 13.4).
Depending on the affected functional domain in the TF, the assessment can include the following by overexpressing the TF from a plasmid DNA in cell culture: (1) quantitative assessment of protein expression by Western blot; (2) subcellular localization of the green fluorescence protein tagged TF, (3) protein-DNA binding assays such as electrophoretic mobility shift assay (EMSA) where the TF binds to specific DNA sequences, (4) transactivation reporter assays, and (5) protein–protein binding by co-immunoprecipitation.
4.2.1.1 PROP1
Patients with PROP1 variants present with a highly consistent phenotype: GH, TSH, and more than two-thirds of the cases have ACTH, FSH/LH, PRL deficiency. Typically, they present with AL hypoplasia, 1:10 patients have AL hyperplasia, and PL is intact. Waxing and waning of the pituitary size over time is common (Obermannova et al. 2011; Turton et al. 2005a). Patients carry homozygous or compound heterozygous variants. About three-quarters of variants are missense/nonsense while one-quarter are splicing or large deletions (Fang et al. 2016b; Madeira et al. 2017). Two founder mutations are well known: c. 301-302delAG from the Iberian Peninsula (Cogan et al. 1998; Dusatkova et al. 2016) and c. 296-297delGA from Lithuania (Navardauskaite et al. 2014). Functional testing includes binding to/transactivation on the PRDQ9 sequence (Kelberman et al. 2009). While the pituitary phenotype is extremely consistent there are two reports of stating extra-pituitary features: (1) two patients with pituitary stalk interruption syndrome (PSIS) and four with heart/kidney malformations and deafness were described from the GENHYPOPIT network in consanguineous patients with PROP1 and POU1F1 variants (Brue et al. 2017); (2) one CPHD patient was described with ectopic posterior pituitary (EPP) who carried a heterozygous c.301_302delAG, which is inconsistent with the recessive inheritance (Avbelj Stefanija et al. 2015). However, it is possible that these individuals had additional genetic or environmental causes of the atypical features.
4.2.1.2 POU1F1
Patients with POU1F1 variants show the most consistent manifestation of all CPHD patients with GH, TSH, PRL deficiency and no other hormones being affected, AL hypoplasia, and PL placed normally. Typical inheritance is recessive (homozygous and compound heterozygous), although there are some examples of dominant inheritance. There are two published families with IGHD carrying a heterozygous p.P76L (Sobrier et al. 2016) or a homozygous p.E230K (Gat-Yablonski et al. 2002). Functional testing is performed by transactivation on the Gh, Prl and Tshb promoters (Hendriks-Stegeman et al. 2001; Turton et al. 2005b), altered promoter/enhancer autoregulation (Vallette-Kasic et al. 2001), exon trapping of splice variants (Inoue et al. 2012; Takagi et al. 2017; Turton et al. 2012).
POU1F1 variants with dominant inheritance have an incomplete penetrance and reveal mechanisms other than roles as a transcriptional regulator on the known promoters. The most common dominant variant p.R271W was shown as a dominant negative transcriptional repressor as well as amino acid R271 binding to MATR3 and SATB1 in the nuclear matrix enabling features in chromatin remodeling (Cohen et al. 2006; Pellegrini et al. 2006; Skowronska-Krawczyk et al. 2014). POU1F1 p.P76L presented with IGHD, and the variant protein exhibited increased interaction with ELK1, PITX1, and LHX3a and with the enhancer region of GH1 (Sobrier et al. 2015). Splice variants revealed either complete skipping of exon 2 (c.142+3A>G and c.214+1G>T) (Inoue et al. 2012; Turton et al. 2012) or splicing into the longer beta isoform of POU1F1 possessing repressor activities in vitro (c.143-83A>G) (Takagi et al. 2017). The variant p.K216E has an increased (not decreased!) activation of Gh and Prl and drastically reduced retinoic acid dependent autoactivation of the Pou1f1 enhancer (Cohen et al. 1999).
4.2.1.3 LHX3
The typical hypopituitarism patient with homozygous LHX3 variants presents with GH and TSH deficiency, two-thirds with LH/FSH and PRL deficiency while only a third of them have ACTH deficiency (Bechtold-Dalla Pozza et al. 2012). Less than half of the patients have abnormal pituitary size, with AL hypoplasia and eutopic PL. Additional features are fairly common, such as limited neck rotation (not present in Lhx3 −/− mice), enlarged fontanels, hearing impairment, frontal bossing or more rarely thinning of the corpus callosum and dolichocephaly (Bonfig et al. 2011; Jullien et al. 2018; Kristrom et al. 2009; Rajab et al. 2008; Ramzan et al. 2017).
One family was published with a generation of two miscarriages, one child with compound heterozygous LHX3 p.C118Y & c.252-3 C>G variants with CPHD and limited neck rotation while members of this family carrying the c.252-3 C>G splice variant had a high incidence of limited neck rotation (Sobrier et al. 2012). Another heterozygous variant also showed CPHD but no other distinctive features and the phenotype was incompletely penetrant (Jullien et al. 2018).
Variants are tested by using the activator LHX3A isoform for transactivation and DNA binding on Cga, Gh, Prl, Tshb promoters (Bechtold-Dalla Pozza et al. 2012; Rajab et al. 2008). Heterozygous variants are typically tested for dominant negative effects on the same promoters together with POU1F1 interaction (Jullien et al. 2018; Sobrier et al. 2012).
4.2.1.4 LHX4
These patients typically present with dominant inheritance and incomplete penetrance. GH, TSH deficiency is high while more than half of the cases have ACTH and less than half of them have gonadotroph deficiency and PRL deficiency is rare. AP hypoplasia and EPP are typical, underdeveloped sella is common. Rare features include Chiari I malformation and thin stalk (Castinetti et al. 2008b; Cohen et al. 2017; Dateki et al. 2010a; Machinis et al. 2001; Pfaeffle et al. 2008; Rochette et al. 2015). There are two examples of IGHD described (Cohen et al. 2017; Gucev et al. 2016).
Functional testing is typically carried out on the same promoters as with LHX3 or on the Pou1f1 and Fshb promoters. Haploinsufficiency appears to be the typical mode of dominant action (same references as in previous paragraph and Fuxman Bass et al. 2015).
The only patient with a homozygous allele (p.T126 M) described so far presented with the features of a typical heterozygous LHX4 patient (CPHD, AP aplasia, EPP, sella defect) but also with midfacial hypoplasia, small upturned nose with depressed nasal bridge, low-set crumpled ears and death during the first postnatal week (Gregory et al. 2015b). Homozygosity mapping and high conservation of amino acid 126 suggested pathogenicity. Transactivation ability of p.T126 M alone on the Prl promoter was not different; however, the interaction with POU1F1 was significantly reduced on the reporter construct.
4.2.1.5 HESX1
Less than two dozen HESX1 families with hypopituitarism were described to date. Thus far, those with recessive inheritance are all CPHD (Fang et al. 2016a; Reynaud et al. 2011; Sobrier et al. 2006), while heterozygous HESX1 patients can be IGHD (Cohen et al. 2003; McNay et al. 2007; Vivenza et al. 2011) or CPHD (Corneli et al. 2008; Coya et al. 2007; Reynaud et al. 2012; Tajima et al. 2003; Takagi et al. 2016; Thomas et al. 2001). The variants identified so far are predominantly missense. The onset of hormone deficiency is typically early and frequently evolving from IGHD to CPHD (Coya et al. 2007; Reynaud et al. 2011). GH, TSH, ACTH deficiency is very high while FSH/LH and PRL deficiency is gradually fewer. AL hypoplasia and EPP are common and rare features can include variable penetrance of PSIS, thin stalk, septo-optic dysplasia (SOD), and optic nerve hypoplasia (ONH). HESX1 is a well-characterized gene in SOD (Dattani et al. 1998). Only a few SOD cases are reported to have hypopituitarism (Cohen et al. 2003; Coya et al. 2007; Thomas et al. 2001). Functional testing of variants includes testing HESX1’s ability to repress activation caused by PROP1 on a multimerized paired HD binding site (P3E4) reporter, binding to DNA (Cohen et al. 2003; Fang et al. 2016a; McNay et al. 2007; Reynaud et al. 2012; Sobrier et al. 2006; Takagi et al. 2016).
4.2.1.6 SOX2
Individuals with SOX2 variants present with anophtalmia, intellectual disability, and growth delay/short stature. Hypopituitarism is frequently not assessed (Schilter et al. 2013) and is reviewed in the works by Bakrania et al. (Bakrania et al. 2007) and Schneider et al. (Schneider et al. 2009). Information is limited to less than 20 cases that present with isolated HH (Bakrania et al. 2007; Errichiello et al. 2018; Kelberman et al. 2006; Sato et al. 2007; Takagi et al. 2014b), IGHD (Kelberman et al. 2006; Schilter et al. 2013; Schneider et al. 2009), and a few with CPHD (Blackburn et al. 2018; Kelberman et al. 2006; Macchiaroli et al. 2014; Schneider et al. 2009). They often have bilateral/unilateral anophtalmia (missing in Sox2-null mice), but other features including ONH, EPP, learning disability are occasionally present. Inheritance is dominant and in patients with hypopituitarism most variants are de novo frame shifts. Functional testing of variants involves transactivation of the Hesx1 promoter and binding to consensus SOX DNA binding sites (Kelberman et al. 2006; Takagi et al. 2014b). The role of Sox2 in pituitary tumors requires further investigation.
4.2.1.7 SOX3
The Xq26–27 chromosomal region of SOX3 was first implicated in a large family with X-linked mental retardation (XLMR) and IGHD in 1996 (Laumonnier et al. 2002). Very few families were described to date and most of them have CPHD: GH and TSH deficiencies, occasional LH/FSH deficiency and rarely ACTH or PRL (Alatzoglou et al. 2011; Bauters et al. 2014; Izumi et al. 2014; Takagi et al. 2014a; Woods et al. 2005). In these hemizygous males, most genetic changes are small, in-frame deletions and insertions affecting polyalanine tracts (Alatzoglou et al. 2011; Izumi et al. 2014; Laumonnier et al. 2002). There are two examples of CPHD with complete SOX3 duplications (Bauters et al. 2014; Woods et al. 2005). Larger chromosomal duplications can result in XX sex reversal (Sutton et al. 2011). The single missense variant example (p.R5Q) had CPHD and a central incisor (Alatzoglou et al. 2011). EPP is occasionally reported (Woods et al. 2005).
The polyalanine tract changes result in perinuclear/cytoplasmic aggregates, impair the ability to transactivate via consensus SOX DNA binding sites, and have a reduced propensity to inhibit Wnt/Ctnnb/TCF mediated transcription (Alatzoglou et al. 2011; Takagi et al. 2014a; Woods et al. 2005).
4.2.1.8 OTX2
Families with OTX2 variants present with an autosomal dominant inheritance and incomplete penetrance. Incomplete penetrance and variable expressivity are well demonstrated in Otx2 −/− mice in a genetic background specific manner (Hide et al. 2002). Patients with heterozygous OTX2 variants can present with ocular only, or ocular with hypopituitarism phenotypes, while cases of hypopituitarism-only cases are rare (Diaczok et al. 2008). The ocular phenotype is anophtalmia/microphtalmia typically involving both eyes (Gerth-Kahlert et al. 2013 from Ragge and Wyatt). In the cases with ocular and pituitary phenotypes, the same ocular phenotypes were observed as well as optic nerve hypoplasia/dysplasia/aplasia (ONH) (Dateki et al. 2008; Gorbenko Del Blanco et al. 2012; Prasov et al. 2012; Schilter et al. 2011; Tajima et al. 2009). IGHD is almost as common as CPHD (Ashkenazi-Hoffnung et al. 2010; Dateki et al. 2008; Delahaye et al. 2012; Henderson et al. 2009; Lonero et al. 2016). Less than two dozen hypopituitarism cases are described, and they typically present with CPHD (GH, TSH, and fewer ACTH and FSH/LH and rarely PRL deficiency), EPP, and five of them had PSIS (all ONH and IGHD references and Diaczok et al. 2008; Shimada et al. 2016; Takagi et al. 2015; Vincent et al. 2014). The one published recessive CPHD case with an OTX2 variant is only based on in silico prediction and segregation (Catania et al. 2019). Missense, nonsense, frame shift variants and large deletions are all common with OTX2. Although some reviews suggest that variants in the N-terminal region of the protein are associated with ocular features and in the C-terminal with pituitary involvement, we believe there are not enough cases with hypopituitarism to support this idea (Gorbenko Del Blanco et al. 2012; Schilter et al. 2011). In vitro variant testing is performed with single or multimerized consensus bicoid binding sites and transactivation is carried out on native promoters of Hesx1, Pou1f1 as well (Dateki et al. 2008, 2010b; Diaczok et al. 2008; Gorbenko Del Blanco et al. 2012; Shimada et al. 2016; Tajima et al. 2009). Knock-down of the endogenous zebrafish mRNA in combination with other genes resulted in a complex eye, head, and mandible phenotype comparable to the human otocephaly-dysgnatia complex (Chassaing et al. 2012).
4.2.1.9 GLI2 and ZIC2
Patients with GLI2 variants typically show autosomal dominant inheritance with incomplete penetrance (Babu et al. 2019; Bear et al. 2014; Flemming et al. 2013; Franca et al. 2013; Juanes et al. 2016; Roessler et al. 2005; Shirakawa et al. 2018; Simm et al. 2018; Zwaveling-Soonawala et al. 2018). CPHD (GH, TSH, ACTH most of the time, LH/FSH frequently, PRL rarely deficient) is the most common while IGHD is infrequent (Bear et al. 2014; Gregory et al. 2015a; Juanes et al. 2016; Roessler et al. 2005; Shirakawa et al. 2018). Most patients have hypoplastic AL, about half of the patients have EPP, and a few have absent PP/PSIS. About 10% of the patients have postaxial polydactyly and/or HPE-like features. While most variants are unique to the family the allele affected by both p.M1352V and p.D1520N variants was described by multiple authors in CPHD (Flemming et al. 2013; Franca et al. 2013; Zwaveling-Soonawala et al. 2018). Most variants described are missense. Functional assessment includes binding to a consensus GLI-site in the PTCH1 promoter. Transactivation studies test variants either on the octamerized GLI-binding site from the enhancer of Hnf3b (Foxa2) or on the single GLI-binding site from the promoter of keratin 17. The variant testing includes two steps on these reporter constructs: (1) Testing the mutated full-length GLI2 alone and (2) testing the mutated full-length GLI2 together with a GLI2 cDNA construct missing the N-terminal (1–328) repressor domain (ΔN-GLI2). The ΔN-GLI2 acts a potent activator on these reporter constructs and co-transfection of the mutant + ΔN-GLI2 can demonstrate a dominant negative effect. Embryonic sarcoma cell line (C3H10T1/2) was used to demonstrate osteogenic differentiation upon transfection with normal GLI2. In vivo assays were demonstrated with frog eggs where injection of normal GLI2 results in secondary tail formation (Babu et al. 2019; Flemming et al. 2013; Roessler et al. 2005).
ZIC2 is a common HPE gene and a member of the GLI TF subfamily. A heterozygous p.Gln364Leufs∗2 variant was described in a child with alobar HPE, complex facial/dental features, and the involvement of both the AL/PL with subsequent CPHD (GH, TSH) and central diabetes insipidus (Tasdemir et al. 2014).
4.2.1.10 GLI3
Heterozygous variants in GLI3 are known to cause Greig cephalopolysyndactyly and Pallister–Hall syndrome (PHS). A clear genotype–phenotype correlation exists where variants affecting the middle-third of the open reading frame (nucleotides 1998–3481) can be found in PHS only. PHS is characterized by the presence of major criteria such as hypothalamic hamartoma and mesaxial polydactyly plus several minor features (bifid epiglottis, IGHD, CPHD, genital hypoplasia, imperforate anus, and small nails) (Demurger et al. 2015; Johnston et al. 2005; Kang et al. 1997). A sub-PHS is diagnosed when one major criterion is present with at least one minor criterion. Most published cases with hypopituitarism or pituitary agenesis are in patients with PHS and to lesser extent with sub-PHS. Almost all patients have IGHD, several of the minor features and adrenal and renal agenesis (Demurger et al. 2015; Johnston et al. 2005). Very few cases were described with CPHD (Li et al. 2015; Narumi et al. 2010). Detailed imaging of the pituitary region is not available. Functional testing is similar to GLI2.
4.2.1.11 TF Genes with Limited Evidence in Hypopituitarism
4.2.1.11.1 FOXA2
A few patients with heterozygous FOXA2 variants were described so far. They share the features of CPHD (GH, TSH, ACTH), and have a high incidence of hyperinsulinemia, hypoplastic/absent AL, EPP and have a range of minor features such as single central incisor, dysmorphic facial features, biliary tract abnormalities, heart defects, and neurodevelopmental delay (Boda et al. 2018; Giri et al. 2017; Tsai et al. 2015; Vajravelu et al. 2018). These patients have either missense or large deletions affecting 20p11.21. FOXA2 is expressed in multiple tissues corresponding to the phenotype spectrum (Giri et al. 2017). Transactivation can be tested on the human GLUT2 (phGT2–294), ABCC8, KCNJ11, HADH, SHH, GLI2, and NKX2–2 promoter reporters (Giri et al. 2017; Vajravelu et al. 2018).
4.2.1.11.2 ARNT2
ARNT2 is part of the protein complex that includes the aryl hydrocarbon receptor-interacting protein (AIP), widely studied in specific groups of pituitary adenomas (Raitila et al. 2010; Rostomyan et al. 2017) and cancer (Bogeas et al. 2018). ARNT2 is highly expressed in the mouse and human CNS, retina, kidney, lung, and the pituitary (Webb et al. 2013). A recessive ARNT2 c.1373_1374dupTC variant was identified in a large family with CPHD, kidney, urogenital tract, eye, and CNS anomalies (postnatal microcephaly, frontotemporal hypoplasia, seizures) (Webb et al. 2013). This variant resulted in a frame shift and nonsense mediated decay of the transcript.
4.2.1.11.3 PAX6
PAX6 patients typically present with aniridia and microphtalmia (Lim et al. 2017). Few patients were described with borderline GHD, HH, central hypothyroidism or low cortisol levels (Hergott-Faure et al. 2012; Shimo et al. 2014; Solomon et al. 2009). PAX6 heterozygous variants were described in two cases of IGHD (Takagi et al. 2015). One of them presented with cleft palate, optic disc cupping, AL hypoplasia, and EPP and had a 310 kb deletion of the PAX6 enhancer. The other case with a missense p.N116S had AL hypoplasia. Functional analysis included showing normal protein expression, subcellular localization, binding to a consensus PAX6 binding element from the promoter of CD19 (Mishra et al. 2002) as well as transactivation on a hexamer PAX6 consensus binding element where only the latter showed significant impairment.
4.2.1.11.4 TGIF1
TGIF1 is highly expressed in the liver, kidney, gonads, forebrain, and several other tissues including the pituitary during development and postnatally (Hu et al. 2011). TGIF1 acts as a repressor in retinoid X receptor (RXR) mediated transcription in a TGFB/SMAD-dependent manner (Bartholin et al. 2006; Bertolino et al. 1995). Patients with heterozygous variants in TGIF1 typically present with variable degrees of midline defects ranging from a single central incisor to HPE (Dubourg et al. 2004; El-Jaick et al. 2007). A pool of 30 patients with CPHD were screened, and only one patient had a TGIF1 variant (p.Q267X). This individual had CPHD (GH, TSH, LH/FSH), AL hypoplasia, and a single central incisor. No functional studies were carried out (Tatsi et al. 2013). The repressor effect of TGIF1 is typically demonstrated in the context of retinoic acid activating on a promoter construct of RBP2 (DR1-TATA-luc) or TGFB activating a promoter construct of MMP1 (3-TP-lux). TGIF1 co-immunoprecipitated with RXRA and SMAD3 (El-Jaick et al. 2007). Another patient with a complex CNS phenotype with pituitary hypoplasia and single central incisor had a chromosomal rearrangement affecting TGIF1 (Kantaputra et al. 2006).
4.2.1.11.5 PITX2
Heterozygous PITX2 variants are one cause of Axenfeld-Rieger syndrome (ARS) characterized by the defects of the eye anterior segment, hypodontia (including single central incisor), maxillary hypoplasia, umbilical protrusion, and heart defects in humans (Franco et al. 2017; Seifi and Walter 2018; Semina et al. 1996). No PITX2 variants have yet been discovered in patients with hypopituitarism. A few papers studying PITX2 variants are clear on the lack of hypopituitarism and the presence of ARS with the patient variants studied (Quentien et al. 2011), while others have no more indication of pituitary involvement than a flattened sella turcica (Idrees et al. 2006) and some actually state the lack of PITX2 variants (Lowry et al. 2007). Mouse mutants heterozygous for Pitx2 loss of function alleles do not have hypopituitarism.
4.2.1.11.6 NKX2–1, TCF7L1, INSM1, SIX3, and SIX6
A large chromosomal deletion involving NKX2–1 (and MBIP, NKX2.8, PAX9, SLC25A1) was described in a patient with pituitary stalk duplication and exaggerated response to TRH stimulation (Accornero et al. 2010). So far, one nonsense variant of NKX2–1 was implicated in one family with IGHD and HH (Balicza et al. 2018). Heterozygous missense variants in the Wnt signaling repressor TCF7L1 were described in two patients with IGHD and SOD-like features (Gaston-Massuet et al. 2016). There are very few variants reported in INSM1; however, it appears to be a very specific marker for neuroendocrine differentiation in primary lung cancer (Mukhopadhyay et al. 2019). HPE and micro/anophtalmia is prevalent in patients with SIX3 or SIX6 variants but there is no clear evidence for pathogenicity in human hypopituitarism thus far (Gallardo et al. 1999; Martinez-Frias et al. 2014; Rauchman et al. 2001).
4.2.2 Select Genetic Causes of Isolated Pituitary Hormone Deficiency
4.2.2.1 Isolated ACTH Deficiency (IAD)
Genetic causes for IAD include two established genes: TBX19 and POMC. Pathogenic TBX19 TF variants result in recessive, neonatal onset ACTH deficiency, and they represent about two-thirds of the patients with IAD (Couture et al. 2012; Metherell et al. 2004; Pulichino et al. 2003). Patients present with severe hypoglycemia and high mortality unless promptly treated with hydrocortisone (Abali et al. 2019; Couture et al. 2012; Vallette-Kasic et al. 2005). Recessive mutations were described in POMC resulting in a protein translation defect with red hair pigmentation, severe, early onset obesity, and secondary adrenal insufficiency (Aslan et al. 2014; Krude et al. 1998). The mechanism of corticotrope deficiency remains elusive and likely indirect in patients with heterozygous, de novo NFKB2 TF mutations who present with IAD, hypogammaglobulinemia similar to common variable immunodeficiency (CVID), alopecia, lymphocyte and NK-cell defects, and trachyonychia (Brue et al. 2014; Chen et al. 2013; Lougaris et al. 2015).
4.2.2.2 Isolated TSH Deficiency (ITD)
While congenital hypothyroidism has an incidence 1:3000 congenital central hypothyroidism (isolated thyrotroph deficiency) is extremely rare (<1:20,000) (Grosse and Van Vliet 2011; van Tijn et al. 2005). Variants in TSHB and TRHR are the longest known causes (Collu et al. 1997; Hayashizaki et al. 1989). Variants in TSHB typically affect the “seat belt” region where TSHB binds CGA in a tightly regulated process to form biologically active TSH (Matzuk et al. 1988; Nicholas et al. 2017). The mechanism by which heterozygous TRHR variants lead to TSH deficiency is not completely understood (Collu et al. 1997). The cause of isolated TSH deficiency can be clarified with TRH stimulation testing. TSHB defects preserve the secretory response of CGA and PRL (Bonomi et al. 2001). The response is blunted if TRHR is defective (Collu et al. 1997).
Recently, an X-linked cause of TSH deficiency was described in men carrying variants in IGSF1. They present with PRL deficiency and macroorchidism, but no GHD (Asakura et al. 2015; Hughes et al. 2016; Joustra et al. 2016; Nakamura et al. 2013; Sun et al. 2012; Tajima et al. 2013; Tenenbaum-Rakover et al. 2016). TBLX1 is the newest member of genes in isolated congenital central hypothyroidism (Heinen et al. 2016).
4.2.2.3 Isolated Growth Hormone Deficiency (IGHD)
Typical genetic causes for IGHD remain to be those in GHRHR, GH1 while defects in SOX3, HESX1 GLI3, OTX2 are rare (Alatzoglou and Dattani 2010; Demurger et al. 2015). Overall, GHRH and GH1 defects are recessive (type I GHD) but a non-insignificant pool of patients shows autosomal-dominant or X-linked inheritance (Alatzoglou and Dattani 2012). SOX3, GLI3, and OTX2 were discussed previously.
4.2.2.4 Isolated LH/FSH Deficiency
Currently more than 30 genes are implicated in congenital HH with or without anosmia. This is a huge increase since 2000, when only four well-established congenital HH genes were known: KAL1, GNRHR, DAX1, and PCSK1 (Seminara et al. 2000). An extensive review was recently published (Maione et al. 2018).
5 Concluding Remarks
Current diagnostic opportunities have enabled physicians to establish the clinical diagnosis of pituitary hormone deficiency with high confidence. Advancements in DNA sequencing technology provided an incredible pool of novel candidate genes and variants to test for the clinician and the researcher. We have just begun to understand the functional consequences of changes in the coding region of the genome. According to the Genetics Home Reference at the NIH, the coding information is only 1% of our genome. Improving of the understanding of large copy number variations as well as the “meaning” of the noncoding genome will be driven by the progression of whole genome sequencing technology and bioinformatics analysis. Currently, the treatment of pituitary hormone deficiency consists of replacement of growth hormone and end organ hormones such as thyroid hormone or steroid hormones. Creating artificial endocrine organs is at its dawn. Gene therapy for specific genetic defects is at its very early stages for non-pituitary diseases. Improving our understanding on how genetic defects in the most common TF genes lead to disease such as hypopituitarism is fundamental in this progress.
Abbreviations
- ACTH:
-
Adrenocorticotropic hormone
- AL:
-
Anterior lobe of pituitary
- Bmp:
-
Bone morphogenetic protein
- CGA:
-
Choriogonadotropin alpha subunit
- CNS:
-
Central nervous system
- CPHD:
-
Combined pituitary hormone deficiency
- Fgf:
-
Fibroblast growth factor
- FSH:
-
Follicle-stimulating hormone
- GH:
-
Growth hormone
- GHD:
-
Growth hormone deficiency
- GR:
-
Glucocorticoid receptor
- HH:
-
Hypogonadotropic hypogonadism
- IAD:
-
Isolated ACTH deficiency
- IGHD:
-
Isolated growth hormone deficiency
- IL:
-
Intermediate lobe of pituitary
- LH:
-
Luteinizing hormone
- MSH-α:
-
Melanocyte-stimulating hormone, alpha
- ONH:
-
Optic nerve hypoplasia
- PC(SK):
-
Proprotein convertase (subtilisin/kexin)
- PL:
-
Posterior lobe of pituitary
- POMC:
-
Pro-opiomelanocortin
- PRL:
-
Prolactin
- RAR:
-
Retinoic acid receptor
- Shh:
-
Sonic hedgehog
- TF:
-
Transcription factor
- TR:
-
Thyroid hormone receptor
- TSH:
-
Thyroid-stimulating hormone
- VUS:
-
Variants of unknown significance
- WES:
-
Whole exome sequencing
- Wnt:
-
Wingless-type MMTV integration site family/beta-catenin
References
Abali ZY, Yesil G, Kirkgoz T et al (2019) Evaluation of growth and puberty in a child with a novel TBX19 gene mutation and review of the literature. Hormones (Athens). https://doi.org/10.1007/s42000-019-00096-7
Accornero S, Danesino C, Bastianello S, D’Errico I, Guala A, Chiovato L (2010) Duplication of the pituitary stalk in a patient with a heterozygous deletion of chromosome 14 harboring the thyroid transcription factor-1 gene. J Clin Endocrinol Metab 95:3595–3596. https://doi.org/10.1210/jc.2010-0621
Alatzoglou KS, Dattani MT (2010) Genetic causes and treatment of isolated growth hormone deficiency-an update. Nat Rev Endocrinol 6:562–576. https://doi.org/10.1038/nrendo.2010.147
Alatzoglou KS, Dattani MT (2012) Phenotype-genotype correlations in congenital isolated growth hormone deficiency (IGHD). Indian J Pediatr 79:99–106. https://doi.org/10.1007/s12098-011-0614-7
Alatzoglou KS, Kelberman D, Cowell CT et al (2011) Increased transactivation associated with SOX3 polyalanine tract deletion in a patient with hypopituitarism. J Clin Endocrinol Metab 96:E685–E690. https://doi.org/10.1210/jc.2010-1239
Ando M, Goto M, Hojo M et al (2018) The proneural bHLH genes Mash1, Math3 and NeuroD are required for pituitary development. J Mol Endocrinol 61:127–138. https://doi.org/10.1530/JME-18-0090
Andrioli M, Pecori Giraldi F, Cavagnini F (2006) Isolated corticotrophin deficiency. Pituitary 9:289–295. https://doi.org/10.1007/s11102-006-0408-5
Asakura Y, Abe K, Muroya K et al (2015) Combined growth hormone and thyroid-stimulating hormone deficiency in a Japanese patient with a novel frameshift mutation in IGSF1. Horm Res Paediatr 84:349–354. https://doi.org/10.1159/000438672
Ashkenazi-Hoffnung L, Lebenthal Y, Wyatt AW (2010) A novel loss-of-function mutation in OTX2 in a patient with anophthalmia and isolated growth hormone deficiency. Hum Genet 127:721–729. https://doi.org/10.1007/s00439-010-0820-9
Aslan IR, Ranadive SA, Valle I, Kollipara S, Noble JA, Vaisse C (2014) The melanocortin system and insulin resistance in humans: insights from a patient with complete POMC deficiency and type 1 diabetes mellitus. Int J Obes 38:148–151. https://doi.org/10.1038/ijo.2013.53
Avbelj Stefanija M, Kotnik P, Bratanič N et al (2015) Novel mutations in HESX1 and PROP1 genes in combined pituitary hormone deficiency. Horm Res Paediatr 84:153–158. https://doi.org/10.1159/000433468
Babu D, Fanelli A, Mellone S et al (2019) Novel GLI2 mutations identified in patients with Combined Pituitary Hormone Deficiency (CPHD): evidence for a pathogenic effect by functional characterization. Clin Endocrinol 90:449–456. https://doi.org/10.1111/cen.13914
Bakrania P, Robinson DO, Bunyan DJ et al (2007) SOX2 anophthalmia syndrome: 12 new cases demonstrating broader phenotype and high frequency of large gene deletions. Br J Ophthalmol 91:1471–1476. https://doi.org/10.1136/bjo.2007.117929
Balicza P, Grosz Z, Molnár V et al (2018) NKX2-1 new mutation associated with myoclonus, dystonia, and pituitary involvement. Front Genet 9:335. https://doi.org/10.3389/fgene.2018.00335
Bartholin L, Powers SE, Melhuish TA, Lasse S, Weinstein M, Wotton D (2006) TGIF inhibits retinoid signaling. Mol Cell Biol 26:990–1001. https://doi.org/10.1128/MCB.26.3.990-1001.2006
Bauters M, Frints SG, Van Esch H et al (2014) Evidence for increased SOX3 dosage as a risk factor for X-linked hypopituitarism and neural tube defects. Am J Med Genet A 164a:1947–1952. https://doi.org/10.1002/ajmg.a.36580
Bear KA, Solomon BD, Antonini S et al (2014) Pathogenic mutations in GLI2 cause a specific phenotype that is distinct from holoprosencephaly. J Med Genet 51:413–418. https://doi.org/10.1136/jmedgenet-2013-102249
Bechtold-Dalla Pozza S, Hiedl S, Roeb J et al (2012) A recessive mutation resulting in a disabling amino acid substitution (T194R) in the LHX3 homeodomain causes combined pituitary hormone deficiency. Horm Res Paediatr 77:41–51. https://doi.org/10.1159/000335929
Bertolino E, Reimund B, Wildt-Perinic D, Clerc RG (1995) A novel homeobox protein which recognizes a TGT core and functionally interferes with a retinoid-responsive motif. J Biol Chem 270:31178–31188. https://doi.org/10.1074/jbc.270.52.31178
Bharti K, Gasper M, Bertuzzi S, Arnheiter H (2011) Lack of the ventral anterior homeodomain transcription factor VAX1 leads to induction of a second pituitary. Development 138:873–878. https://doi.org/10.1242/dev.056465
Blackburn PR, Chacon-Camacho OF, Ortiz-González XR et al (2018) Extension of the mutational and clinical spectrum of SOX2 related disorders: description of six new cases and a novel association with suprasellar teratoma. Am J Med Genet A 176:2710–2719. https://doi.org/10.1002/ajmg.a.40644
Boda H, Miyata M, Inagaki H, Shinkai Y, Kato T, Yoshikawa T, Kurahashi H (2018) FOXA2 gene mutation in a patient with congenital complex pituitary hormone deficiency. Eur J Med Genet. https://doi.org/10.1016/j.ejmg.2018.11.004
Boehm U, Bouloux PM, Dattani MT et al (2015) Expert consensus document: European Consensus Statement on congenital hypogonadotropic hypogonadism—pathogenesis, diagnosis and treatment. Nat Rev Endocrinol 11:547–564. https://doi.org/10.1038/nrendo.2015.112
Bogeas A, Morvan-Dubois G, El-Habr EA et al (2018) Changes in chromatin state reveal ARNT2 at a node of a tumorigenic transcription factor signature driving glioblastoma cell aggressiveness. Acta Neuropathol 135:267–283. https://doi.org/10.1007/s00401-017-1783-x
Bonfig W, Krude H, Schmidt H (2011) A novel mutation of LHX3 is associated with combined pituitary hormone deficiency including ACTH deficiency, sensorineural hearing loss, and short neck-a case report and review of the literature. Eur J Pediatr 170:1017–1021. https://doi.org/10.1007/s00431-011-1393-x
Bonomi M, Proverbio MC, Weber G, Chiumello G, Beck-Peccoz P, Persani L (2001) Hyperplastic pituitary gland, high serum glycoprotein hormone alpha-subunit, and variable circulating thyrotropin (TSH) levels as hallmark of central hypothyroidism due to mutations of the TSH beta gene. J Clin Endocrinol Metab 86:1600–1604. https://doi.org/10.1210/jcem.86.4.7411
Brinkmeier ML, Davis SW, Carninci P et al (2009) Discovery of transcriptional regulators and signaling pathways in the developing pituitary gland by bioinformatic and genomic approaches. Genomics 93:449–460. https://doi.org/10.1016/j.ygeno.2008.11.010
Brue T (2018) Lessons from screening of genetic causes of hypopituitarism in session S54—“New developments of pituitary disease”, session 54 edn. In: The Endocrine Society’s 100th Annual Meeting and Expo (ENDO 2018), Chicago, IL
Brue T, Quentien MH, Khetchoumian K et al (2014) Mutations in NFKB2 and potential genetic heterogeneity in patients with DAVID syndrome, having variable endocrine and immune deficiencies. BMC Med Genet 15:139. https://doi.org/10.1186/s12881-014-0139-9
Brue T, Saveanu A, Jullien N et al (2017) Lessons from monogenic causes of growth hormone deficiency. Ann Endocrinol (Paris) 78:77–79. https://doi.org/10.1016/j.ando.2017.04.001
Budry L, Couture C, Balsalobre A, Drouin J (2011) The Ets factor Etv1 interacts with Tpit protein for pituitary pro-opiomelanocortin (POMC) gene transcription. J Biol Chem 286:25387–25396. https://doi.org/10.1074/jbc.M110.202788
Budry L, Balsalobre A, Gauthier Y et al (2012) The selector gene Pax7 dictates alternate pituitary cell fates through its pioneer action on chromatin remodeling. Genes Dev 26:2299–2310. https://doi.org/10.1101/gad.200436.112
Castinetti F, Reynaud R, Saveanu A et al (2008a) [Clinical and genetic aspects of combined pituitary hormone deficiencies]. Ann Endocrinol (Paris) 69:7–17. https://doi.org/10.1016/j.ando.2008.01.001
Castinetti F, Saveanu A, Reynaud R et al (2008b) A novel dysfunctional LHX4 mutation with high phenotypical variability in patients with hypopituitarism. J Clin Endocrinol Metab 93:2790–2799. https://doi.org/10.1210/jc.2007-2389
Castinetti F, Reynaud R, Saveanu A, Barlier A, Brue T (2012) Genetic causes of combined pituitary hormone deficiencies in humans. Ann Endocrinol (Paris) 73:53–55. https://doi.org/10.1016/j.ando.2012.03.025
Catania A, Legati A, Peverelli L et al (2019) Homozygous variant in OTX2 and possible genetic modifiers identified in a patient with combined pituitary hormone deficiency, ocular involvement, myopathy, ataxia, and mitochondrial impairment. Am J Med Genet A 179(5):827–831. https://doi.org/10.1002/ajmg.a.61092
Chassaing N, Sorrentino S, Davis EE et al (2012) OTX2 mutations contribute to the otocephaly-dysgnathia complex. J Med Genet 49:373–379. https://doi.org/10.1136/jmedgenet-2012-100892
Chen K, Coonrod EM, Kumánovics A et al (2013) Germline mutations in NFKB2 implicate the noncanonical NF-kappaB pathway in the pathogenesis of common variable immunodeficiency. Am J Hum Genet 93:812–824. https://doi.org/10.1016/j.ajhg.2013.09.009
Cheung LYM, George AS, McGee SR, Daly AZ, Brinkmeier ML, Ellsworth BS, Camper SA (2018) Single-cell RNA sequencing reveals novel markers of male pituitary stem cells and hormone-producing cell types. Endocrinology 159:3910–3924. https://doi.org/10.1210/en.2018-00750
Chinoy A, Murray PG (2016) Diagnosis of growth hormone deficiency in the paediatric and transitional age. Best Pract Res Clin Endocrinol Metab 30:737–747. https://doi.org/10.1016/j.beem.2016.11.002
Cogan JD, Wu W, Phillips JA 3rd et al (1998) The PROP1 2-base pair deletion is a common cause of combined pituitary hormone deficiency. J Clin Endocrinol Metab 83:3346–3349. https://doi.org/10.1210/jcem.83.9.5142
Cohen LE, Zanger K, Brue T, Wondisford FE, Radovick S (1999) Defective retinoic acid regulation of the Pit-1 gene enhancer: a novel mechanism of combined pituitary hormone deficiency. Mol Endocrinol 13:476–484. https://doi.org/10.1210/mend.13.3.0251
Cohen RN, Cohen LE, Botero D, Yu C, Sagar A, Jurkiewicz M, Radovick S (2003) Enhanced repression by HESX1 as a cause of hypopituitarism and septooptic dysplasia. J Clin Endocrinol Metab 88:4832–4839. https://doi.org/10.1210/jc.2002-021868
Cohen RN, Brue T, Naik K, Houlihan CA, Wondisford FE, Radovick S (2006) The role of CBP/p300 interactions and Pit-1 dimerization in the pathophysiological mechanism of combined pituitary hormone deficiency. J Clin Endocrinol Metab 91:239–247. https://doi.org/10.1210/jc.2005-1211
Cohen E, Maghnie M, Collot N et al (2017) Contribution of LHX4 mutations to pituitary deficits in a cohort of 417 unrelated patients. J Clin Endocrinol Metab 102:290–301. https://doi.org/10.1210/jc.2016-3158
Collu R, Tang J, Castagné J et al (1997) A novel mechanism for isolated central hypothyroidism: inactivating mutations in the thyrotropin-releasing hormone receptor gene. J Clin Endocrinol Metab 82:1561–1565. https://doi.org/10.1210/jcem.82.5.3918
Corneli G, Vivenza D, Prodam F et al (2008) Heterozygous mutation of HESX1 causing hypopituitarism and multiple anatomical malformations without features of septo-optic dysplasia. J Endocrinol Investig 31:689–693. https://doi.org/10.1007/bf03346416
Correa FA, Jorge AA, Nakaguma M et al (2018) Pathogenic copy number variants in patients with congenital hypopituitarism associated with complex phenotypes. Clin Endocrinol 88:425–431. https://doi.org/10.1111/cen.13535
Couture C, Saveanu A, Barlier A et al (2012) Phenotypic homogeneity and genotypic variability in a large series of congenital isolated ACTH-deficiency patients with TPIT gene mutations. J Clin Endocrinol Metab 97:E486–E495. https://doi.org/10.1210/jc.2011-1659
Coya R, Vela A, Perez de Nanclares G, Rica I, Castano L, Busturia MA, Martul P (2007) Panhypopituitarism: genetic versus acquired etiological factors. J Pediatr Endocrinol Metab 20:27–36. https://doi.org/10.1515/JPEM.2007.20.1.27
Dasen JS, O’Connell SM, Flynn SE et al (1999) Reciprocal interactions of Pit1 and GATA2 mediate signaling gradient-induced determination of pituitary cell types. Cell 97:587–598. https://doi.org/10.1016/S0092-8674(00)80770-9
Dateki S, Fukami M, Sato N, Muroya K, Adachi M, Ogata T (2008) OTX2 mutation in a patient with anophthalmia, short stature, and partial growth hormone deficiency: functional studies using the IRBP, HESX1, and POU1F1 promoters. J Clin Endocrinol Metab 93:3697–3702. https://doi.org/10.1210/jc.2008-0720
Dateki S, Fukami M, Uematsu A et al (2010a) Mutation and gene copy number analyses of six pituitary transcription factor genes in 71 patients with combined pituitary hormone deficiency: identification of a single patient with LHX4 deletion. J Clin Endocrinol Metab 95:4043–4047. https://doi.org/10.1210/jc.2010-0150
Dateki S, Kosaka K, Hasegawa K et al (2010b) Heterozygous orthodenticle homeobox 2 mutations are associated with variable pituitary phenotype. J Clin Endocrinol Metab 95:756–764. https://doi.org/10.1210/jc.2009-1334
Dattani MT (2005) Growth hormone deficiency and combined pituitary hormone deficiency: does the genotype matter? Clin Endocrinol 63:121–130. https://doi.org/10.1111/j.1365-2265.2005.02289.x
Dattani MT, Martinez-Barbera JP, Thomas PQ et al (1998) Mutations in the homeobox gene HESX1/Hesx1 associated with septo-optic dysplasia in human and mouse. Nat Genet 19:125–133. https://doi.org/10.1038/477
Davis SW, Camper SA (2007) Noggin regulates Bmp4 activity during pituitary induction. Dev Biol 305:145–160. https://doi.org/10.1016/j.ydbio.2007.02.001
Davis EE, Frangakis S, Katsanis N (2014) Interpreting human genetic variation with in vivo zebrafish assays. Biochim Biophys Acta 1842:1960–1970. https://doi.org/10.1016/j.bbadis.2014.05.024
Davis SW, Keisler JL, Perez-Millan MI, Schade V, Camper SA (2016) All hormone-producing cell types of the pituitary intermediate and anterior lobes derive from Prop1-expressing progenitors. Endocrinology 157:1385–1396. https://doi.org/10.1210/en.2015-1862
Day RN, Koike S, Sakai M, Muramatsu M, Maurer RA (1990) Both Pit-1 and the estrogen receptor are required for estrogen responsiveness of the rat prolactin gene. Mol Endocrinol 4:1964–1971. https://doi.org/10.1210/mend-4-12-1964
De Rienzo F, Mellone S, Bellone S et al (2015) Frequency of genetic defects in combined pituitary hormone deficiency: a systematic review and analysis of a multicentre Italian cohort. Clin Endocrinol 83:849–860. https://doi.org/10.1111/cen.12849
Delahaye A, Bitoun P, Drunat S et al (2012) Genomic imbalances detected by array-CGH in patients with syndromal ocular developmental anomalies. Eur J Hum Genet 20:527–533. https://doi.org/10.1038/ejhg.2011.233
Demurger F, Ichkou A, Mougou-Zerelli S et al (2015) New insights into genotype-phenotype correlation for GLI3 mutations. Eur J Hum Genet 23:92–102. https://doi.org/10.1038/ejhg.2014.62
Di Iorgi N, Morana G, Allegri AE et al (2016) Classical and non-classical causes of GH deficiency in the paediatric age. Best Pract Res Clin Endocrinol Metab 30:705–736. https://doi.org/10.1016/j.beem.2016.11.008
Diaczok D, Romero C, Zunich J, Marshall I, Radovick S (2008) A novel dominant negative mutation of OTX2 associated with combined pituitary hormone deficiency. J Clin Endocrinol Metab 93:4351–4359. https://doi.org/10.1210/jc.2008-1189
Drolet DW, Scully KM, Simmons DM, Wegner M, Chu KT, Swanson LW, Rosenfeld MG (1991) TEF, a transcription factor expressed specifically in the anterior pituitary during embryogenesis, defines a new class of leucine zipper proteins. Genes Dev 5:1739–1753. https://doi.org/10.1101/gad.5.10.1739
Dubourg C, Lazaro L, Pasquier L et al (2004) Molecular screening of SHH, ZIC2, SIX3, and TGIF genes in patients with features of holoprosencephaly spectrum: mutation review and genotype-phenotype correlations. Hum Mutat 24:43–51. https://doi.org/10.1002/humu.20056
Dusatkova P, Pfäffle R, Brown MR et al (2016) Genesis of two most prevalent PROP1 gene variants causing combined pituitary hormone deficiency in 21 populations. Eur J Hum Genet 24:415–420. https://doi.org/10.1038/ejhg.2015.126
El-Jaick KB, Powers SE, Bartholin L et al (2007) Functional analysis of mutations in TGIF associated with holoprosencephaly. Mol Genet Metab 90:97–111. https://doi.org/10.1016/j.ymgme.2006.07.011
Ergin AB, Kennedy AL, Gupta MK, Hamrahian AH (2015) The Cleveland Clinic manual of dynamic endocrine testing. Springer International, Cham. https://doi.org/10.1007/978-3-319-13048-4
Errichiello E, Gorgone C, Giuliano L et al (2018) SOX2: not always eye malformations. Severe genital but no major ocular anomalies in a female patient with the recurrent c.70del20 variant. Eur J Med Genet 61:335–340. https://doi.org/10.1016/j.ejmg.2018.01.011
Fang Q, Benedetti AF, Ma Q et al (2016a) HESX1 mutations in patients with congenital hypopituitarism: variable phenotypes with the same genotype. Clin Endocrinol 85:408–414. https://doi.org/10.1111/cen.13067
Fang Q, George AS, Brinkmeier ML et al (2016b) Genetics of combined pituitary hormone deficiency: roadmap into the genome era. Endocr Rev 37:636–675. https://doi.org/10.1210/er.2016-1101
Fauquier T, Rizzoti K, Dattani M, Lovell-Badge R, Robinson IC (2008) SOX2-expressing progenitor cells generate all of the major cell types in the adult mouse pituitary gland. Proc Natl Acad Sci USA 105:2907–2912. https://doi.org/10.1073/pnas.0707886105
Flemming GM, Klammt J, Ambler G et al (2013) Functional characterization of a heterozygous GLI2 missense mutation in patients with multiple pituitary hormone deficiency. J Clin Endocrinol Metab 98:E567–E575. https://doi.org/10.1210/jc.2012-3224
Franca MM, Jorge AA, Carvalho LR et al (2013) Relatively high frequency of non-synonymous GLI2 variants in patients with congenital hypopituitarism without holoprosencephaly. Clin Endocrinol 78:551–557. https://doi.org/10.1111/cen.12044
Franco D, Sedmera D, Lozano-Velasco E (2017) Multiple roles of Pitx2 in cardiac development and disease. J Cardiovasc Dev Dis 4. https://doi.org/10.3390/jcdd4040016
Fuxman Bass JI, Sahni N, Shrestha S et al (2015) Human gene-centered transcription factor networks for enhancers and disease variants. Cell 161:661–673. https://doi.org/10.1016/j.cell.2015.03.003
Gallardo ME, Lopez-Rios J, Fernaud-Espinosa I et al (1999) Genomic cloning and characterization of the human homeobox gene SIX6 reveals a cluster of SIX genes in chromosome 14 and associates SIX6 hemizygosity with bilateral anophthalmia and pituitary anomalies. Genomics 61:82–91. https://doi.org/10.1006/geno.1999.5916
Gangat M, Radovick S (2017) Pituitary hypoplasia. Endocrinol Metab Clin N Am 46:247–257. https://doi.org/10.1016/j.ecl.2017.01.003
Gaston-Massuet C, Andoniadou CL, Signore M, Sajedi E, Bird S, Turner JM, Martinez-Barbera JP (2008) Genetic interaction between the homeobox transcription factors HESX1 and SIX3 is required for normal pituitary development. Dev Biol 324:322–333. https://doi.org/10.1016/j.ydbio.2008.08.008
Gaston-Massuet C, McCabe MJ, Scagliotti V et al (2016) Transcription factor 7-like 1 is involved in hypothalamo-pituitary axis development in mice and humans. Proc Natl Acad Sci USA 113:E548–E557. https://doi.org/10.1073/pnas.1503346113
Gat-Yablonski G, Lazar L, Pertzelan A, Phillip M (2002) A novel mutation in PIT-1: phenotypic variability in familial combined pituitary hormone deficiencies. J Pediatr Endocrinol Metab 15:325–330. https://doi.org/10.1515/JPEM.2002.15.3.325
Gergics P, Brinkmeier ML, Camper SA (2015) Lhx4 deficiency: increased cyclin-dependent kinase inhibitor expression and pituitary hypoplasia. Mol Endocrinol 29:597–612. https://doi.org/10.1210/me.2014-1380
Gerth-Kahlert C, Williamson K, Ansari M et al (2013) Clinical and mutation analysis of 51 probands with anophthalmia and/or severe microphthalmia from a single center. Mol Genet Genomic Med 1:15–31. https://doi.org/10.1002/mgg3.2
Giri D, Vignola ML, Gualtieri A et al (2017) Novel FOXA2 mutation causes hyperinsulinism, hypopituitarism with craniofacial and endoderm-derived organ abnormalities. Hum Mol Genet 26:4315–4326. https://doi.org/10.1093/hmg/ddx318
Gorbenko Del Blanco D, Romero CJ, Diaczok D, de Graaff LC, Radovick S, Hokken-Koelega AC (2012) A novel OTX2 mutation in a patient with combined pituitary hormone deficiency, pituitary malformation, and an underdeveloped left optic nerve. Eur J Endocrinol 167:441–452. https://doi.org/10.1530/EJE-12-0333
Gordon DF, Haugen BR, Sarapura VD, Nelson AR, Wood WM, Ridgway EC (1993) Analysis of Pit-1 in regulating mouse TSH beta promoter activity in thyrotropes. Mol Cell Endocrinol 96:75–84. https://doi.org/10.1016/0303-7207(93)90097-4
Goto M, Hojo M, Ando M et al (2015) Hes1 and Hes5 are required for differentiation of pituicytes and formation of the neurohypophysis in pituitary development. Brain Res 1625:206–217. https://doi.org/10.1016/j.brainres.2015.08.045
Gregory LC, Gaston-Massuet C, Andoniadou CL et al (2015a) The role of the sonic hedgehog signalling pathway in patients with midline defects and congenital hypopituitarism. Clin Endocrinol 82:728–738. https://doi.org/10.1111/cen.12637
Gregory LC, Humayun KN, Turton JP, McCabe MJ, Rhodes SJ, Dattani MT (2015b) Novel lethal form of congenital hypopituitarism associated with the first recessive LHX4 mutation. J Clin Endocrinol Metab 100:2158–2164. https://doi.org/10.1210/jc.2014-4484
Grosse SD, Van Vliet G (2011) Prevention of intellectual disability through screening for congenital hypothyroidism: how much and at what level? Arch Dis Child 96:374–379. https://doi.org/10.1136/adc.2010.190280
Gucev Z, Tasic V, Plaseska-Karanfilska D et al (2016) LHX4 gene alterations: patient report and review of the literature. Pediatr Endocrinol Rev 13:749–755
Haddad-Tovolli R, Paul FA, Zhang Y et al (2015) Differential requirements for Gli2 and Gli3 in the regional specification of the mouse hypothalamus. Front Neuroanat 9:34. https://doi.org/10.3389/fnana.2015.00034
Halasz Z, Toke J, Patócs A et al (2006) High prevalence of PROP1 gene mutations in Hungarian patients with childhood-onset combined anterior pituitary hormone deficiency. Endocrine 30:255–260. https://doi.org/10.1007/s12020-006-0002-7
Hayashizaki Y, Hiraoka Y, Endo Y, Miyai K, Matsubara K (1989) Thyroid-stimulating hormone (TSH) deficiency caused by a single base substitution in the CAGYC region of the beta-subunit. EMBO J 8:2291–2296. https://doi.org/10.1002/j.1460-2075.1989.tb08355.x
Hayes FJ, Seminara SB, Crowley WF Jr (1998) Hypogonadotropic hypogonadism. Endocrinol Metab Clin North Am 27:739–763, vii. https://doi.org/10.1016/S0889-8529(05)70039-6
Heinen CA, Losekoot M, Sun Y et al (2016) Mutations in TBL1X are associated with central hypothyroidism. J Clin Endocrinol Metab 101:4564–4573. https://doi.org/10.1210/jc.2016-2531
Henderson RH, Williamson KA, Kennedy JS et al (2009) A rare de novo nonsense mutation in OTX2 causes early onset retinal dystrophy and pituitary dysfunction. Mol Vis 15:2442–2447
Hendriks-Stegeman BI, Augustijn KD, Bakker B, Holthuizen P, van der Vliet PC, Jansen M (2001) Combined pituitary hormone deficiency caused by compound heterozygosity for two novel mutations in the POU domain of the Pit1/POU1F1 gene. J Clin Endocrinol Metab 86:1545–1550. https://doi.org/10.1210/jcem.86.4.7371
Hergott-Faure L, Borot S, Kleinclauss C, Abitbol M, Penfornis A (2012) Pituitary function and glucose tolerance in a family with a PAX6 mutation. Ann Endocrinol (Paris) 73:510–514. https://doi.org/10.1016/j.ando.2012.10.001
Hide T, Hatakeyama J, Kimura-Yoshida C et al (2002) Genetic modifiers of otocephalic phenotypes in Otx2 heterozygous mutant mice. Development 129:4347–4357
Hu Y, Yu H, Shaw G, Renfree MB, Pask AJ (2011) Differential roles of TGIF family genes in mammalian reproduction. BMC Dev Biol 11:58. https://doi.org/10.1186/1471-213X-11-58
Hughes JN, Aubert M, Heatlie J et al (2016) Identification of an IGSF1-specific deletion in a five-generation pedigree with X-linked central hypothyroidism without macroorchidism. Clin Endocrinol 85:609–615. https://doi.org/10.1111/cen.13094
Idrees F, Bloch-Zupan A, Free SL et al (2006) A novel homeobox mutation in the PITX2 gene in a family with Axenfeld-Rieger syndrome associated with brain, ocular, and dental phenotypes. Am J Med Genet B Neuropsychiatr Genet 141B:184–191. https://doi.org/10.1002/ajmg.b.30237
Inoue H, Mukai T, Sakamoto Y et al (2012) Identification of a novel mutation in the exon 2 splice donor site of the POU1F1/PIT-1 gene in Japanese identical twins with mild combined pituitary hormone deficiency. Clin Endocrinol 76:78–87. https://doi.org/10.1111/j.1365-2265.2011.04165.x
Izumi Y, Suzuki E, Kanzaki S et al (2014) Genome-wide copy number analysis and systematic mutation screening in 58 patients with hypogonadotropic hypogonadism. Fertil Steril 102:1130–1136.e1133. https://doi.org/10.1016/j.fertnstert.2014.06.017
Johnston JJ, Olivos-Glander I, Killoran C et al (2005) Molecular and clinical analyses of Greig cephalopolysyndactyly and Pallister-Hall syndromes: robust phenotype prediction from the type and position of GLI3 mutations. Am J Hum Genet 76:609–622. https://doi.org/10.1086/429346
Joustra SD, Roelfsema F, Endert E et al (2016) Pituitary hormone secretion profiles in IGSF1 deficiency syndrome. Neuroendocrinology 103:408–416. https://doi.org/10.1159/000439433
Juanes M, Di Palma I, Ciaccio M et al (2016) Two novel heterozygous missense variations within the GLI2 gene in two unrelated Argentine patients. Medicina (B Aires) 76:213–218
Jullien N, Romanet P, Philippon M et al (2018) Heterozygous LHX3 mutations may lead to a mild phenotype of combined pituitary hormone deficiency. Eur J Hum Genet. https://doi.org/10.1038/s41431-018-0264-6
Kang S, Graham JM Jr, Olney AH, Biesecker LG (1997) GLI3 frameshift mutations cause autosomal dominant Pallister-Hall syndrome. Nat Genet 15:266–268. https://doi.org/10.1038/ng0397-266
Kantaputra PN, Limwongse C, Tochareontanaphol C, Mutirangura A, Mevatee U, Praphanphoj V (2006) Contiguous gene syndrome of holoprosencephaly and hypotrichosis simplex: association with an 18p11.3 deletion. American J Med Genet A 140:2598–2602. https://doi.org/10.1002/ajmg.a.31386
Kapali J, Kabat BE, Schmidt KL et al (2016) Foxo1 is required for normal somatotrope differentiation. Endocrinology 157:4351–4363. https://doi.org/10.1210/en.2016-1372
Kelberman D, Rizzoti K, Avilion A et al (2006) Mutations within Sox2/SOX2 are associated with abnormalities in the hypothalamo-pituitary-gonadal axis in mice and humans. J Clin Invest 116:2442–2455. https://doi.org/10.1172/JCI28658
Kelberman D, Turton JP, Woods KS et al (2009) Molecular analysis of novel PROP1 mutations associated with combined pituitary hormone deficiency (CPHD). Clin Endocrinol 70:96–103. https://doi.org/10.1111/j.1365-2265.2008.03326.x
Klee EW, Hoppman-Chaney NL, Ferber MJ (2011) Expanding DNA diagnostic panel testing: is more better? Expert Rev Mol Diagn 11:703–709. https://doi.org/10.1586/erm.11.58
Kristrom B, Zdunek AM, Rydh A, Jonsson H, Sehlin P, Escher SA (2009) A novel mutation in the LIM homeobox 3 gene is responsible for combined pituitary hormone deficiency, hearing impairment, and vertebral malformations. J Clin Endocrinol Metab 94:1154–1161. https://doi.org/10.1210/jc.2008-0325
Krude H, Biebermann H, Luck W, Horn R, Brabant G, Gruters A (1998) Severe early-onset obesity, adrenal insufficiency and red hair pigmentation caused by POMC mutations in humans. Nat Genet 19:155–157. https://doi.org/10.1038/509
Kulig E, Camper SA, Kuecker S, Jin L, Lloyd RV (1998) Remodeling of hyperplastic pituitaries in hypothyroid alpha-subunit knockout mice after thyroxine and 17beta-estradiol treatment: role of apoptosis. Endocr Pathol 9:261–274. https://doi.org/10.1007/BF02739967
Laumonnier F, Ronce N, Hamel BC et al (2002) Transcription factor SOX3 is involved in X-linked mental retardation with growth hormone deficiency. Am J Hum Genet 71:1450–1455. https://doi.org/10.1086/344661
Leger J, Olivieri A, Donaldson M et al (2014) European Society for Paediatric Endocrinology consensus guidelines on screening, diagnosis, and management of congenital hypothyroidism. J Clin Endocrinol Metab 99:363–384. https://doi.org/10.1210/jc.2013-1891
Lek M, Karczewski KJ, Minikel EV et al (2016) Analysis of protein-coding genetic variation in 60,706 humans. Nature 536:285. https://doi.org/10.1038/nature19057
Li S, Crenshaw EB 3rd, Rawson EJ, Simmons DM, Swanson LW, Rosenfeld MG (1990) Dwarf locus mutants lacking three pituitary cell types result from mutations in the POU-domain gene pit-1. Nature 347:528–533. https://doi.org/10.1038/347528a0
Li MH, Eberhard M, Mudd P et al (2015) Total colonic aganglionosis and imperforate anus in a severely affected infant with Pallister-Hall syndrome. Am J Med Genet A 167A:617–620. https://doi.org/10.1002/ajmg.a.36915
Lim HT, Kim DH, Kim H (2017) PAX6 aniridia syndrome: clinics, genetics, and therapeutics. Curr Opin Ophthalmol 28:436–447. https://doi.org/10.1097/ICU.0000000000000405
Lin SC, Li S, Drolet DW, Rosenfeld MG (1994) Pituitary ontogeny of the Snell dwarf mouse reveals Pit-1-independent and Pit-1-dependent origins of the thyrotrope. Development 120:515–522
Lonero A, Delvecchio M, Primignani P et al (2016) A novel OTX2 gene frameshift mutation in a child with microphthalmia, ectopic pituitary and growth hormone deficiency. J Pediatr Endocrinol Metab 29:603–605. https://doi.org/10.1515/jpem-2015-0425
Lougaris V, Tabellini G, Vitali M et al (2015) Defective natural killer-cell cytotoxic activity in NFKB2-mutated CVID-like disease. J Allergy Clin Immunol 135:1641–1643. https://doi.org/10.1016/j.jaci.2014.11.038
Lowry RB, Gould DB, Walter MA, Savage PR (2007) Absence of PITX2, BARX1, and FOXC1 mutations in De Hauwere syndrome (Axenfeld-Rieger anomaly, hydrocephaly, hearing loss): a 25-year follow up. Am J Med Genet A 143A:1227–1230. https://doi.org/10.1002/ajmg.a.31732
Ma Y, Qi X, Du J et al (2009) Identification of candidate genes for human pituitary development by EST analysis. BMC Genomics 10:109. https://doi.org/10.1186/1471-2164-10-109
Macchiaroli A, Kelberman D, Auriemma RS et al (2014) A novel heterozygous SOX2 mutation causing congenital bilateral anophthalmia, hypogonadotropic hypogonadism and growth hormone deficiency. Gene 534:282–285. https://doi.org/10.1016/j.gene.2013.10.043
Machinis K, Pantel J, Netchine I et al (2001) Syndromic short stature in patients with a germline mutation in the LIM homeobox LHX4. Am J Hum Genet 69:961–968. https://doi.org/10.1086/323764
Madeira JL, Nishi MY, Nakaguma M et al (2017) Molecular analysis of brazilian patients with combined pituitary hormone deficiency and orthotopic posterior pituitary lobe reveals eight different PROP1 alterations with three novel mutations. Clin Endocrinol 87:725–732. https://doi.org/10.1111/cen.13430
Maione L, Dwyer AA, Francou B, Guiochon-Mantel A, Binart N, Bouligand J, Young J (2018) GENETICS IN ENDOCRINOLOGY: genetic counseling for congenital hypogonadotropic hypogonadism and Kallmann syndrome: new challenges in the era of oligogenism and next-generation sequencing. Eur J Endocrinol 178:R55–R80. https://doi.org/10.1530/EJE-17-0749
Man PS, Wells T, Carter DA (2014) Cellular distribution of Egr1 transcription in the male rat pituitary gland. J Mol Endocrinol 53:271–280. https://doi.org/10.1530/JME-14-0158
Marcinkiewicz M, Day R, Seidah NG, Chretien M (1993) Ontogeny of the prohormone convertases PC1 and PC2 in the mouse hypophysis and their colocalization with corticotropin and alpha-melanotropin. Proc Natl Acad Sci USA 90:4922–4926. https://doi.org/10.1073/pnas.90.11.4922
Martinez-Frias ML, Ocejo-Vinyals JG, Arteaga R et al (2014) Interstitial deletion 14q22.3-q23.2: genotype-phenotype correlation. Am J Med Genet A 164A:639–647. https://doi.org/10.1002/ajmg.a.36330
Matzuk MM, Kornmeier CM, Whitfield GK, Kourides IA, Boime I (1988) The glycoprotein alpha-subunit is critical for secretion and stability of the human thyrotropin beta-subunit. Mol Endocrinol 2:95–100. https://doi.org/10.1210/mend-2-2-95
McCabe MJ, Dattani MT (2014) Genetic aspects of hypothalamic and pituitary gland development. Handb Clin Neurol 124:3–15. https://doi.org/10.1016/b978-0-444-59602-4.00001-0
McNay DE, Turton JP, Kelberman D et al (2007) HESX1 mutations are an uncommon cause of septooptic dysplasia and hypopituitarism. J Clin Endocrinol Metab 92:691–697. https://doi.org/10.1210/jc.2006-1609
Metherell LA, Savage MO, Dattani M, Walker J, Clayton PE, Farooqi IS, Clark AJ (2004) TPIT mutations are associated with early-onset, but not late-onset isolated ACTH deficiency. Eur J Endocrinol 151:463–465
Mishra R, Gorlov IP, Chao LY, Singh S, Saunders GF (2002) PAX6, paired domain influences sequence recognition by the homeodomain. J Biol Chem 277:49488–49494. https://doi.org/10.1074/jbc.M206478200
Molitch ME, Clemmons DR, Malozowski S, Merriam GR, Vance ML, Endocrine Society (2011) Evaluation and treatment of adult growth hormone deficiency: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab 96:1587–1609. https://doi.org/10.1210/jc.2011-0179
Mukhopadhyay S, Dermawan JK, Lanigan CP, Farver CF (2019) Insulinoma-associated protein 1 (INSM1) is a sensitive and highly specific marker of neuroendocrine differentiation in primary lung neoplasms: an immunohistochemical study of 345 cases, including 292 whole-tissue sections. Mod Pathol 32:100–109. https://doi.org/10.1038/s41379-018-0122-7
Nakamura A, Bak B, Silander TL et al (2013) Three novel IGSF1 mutations in four Japanese patients with X-linked congenital central hypothyroidism. J Clin Endocrinol Metab 98:E1682–E1691. https://doi.org/10.1210/jc.2013-1224
Narumi Y, Kosho T, Tsuruta G et al (2010) Genital abnormalities in Pallister-Hall syndrome: report of two patients and review of the literature. Am J Med Genet A 152A:3143–3147. https://doi.org/10.1002/ajmg.a.33720
Navardauskaite R, Dusatkova P, Obermannova B et al (2014) High prevalence of PROP1 defects in Lithuania: phenotypic findings in an ethnically homogenous cohort of patients with multiple pituitary hormone deficiency. J Clin Endocrinol Metab 99:299–306. https://doi.org/10.1210/jc.2013-3090
Nicholas AK, Jaleel S, Lyons G et al (2017) Molecular spectrum of TSHbeta subunit gene defects in central hypothyroidism in the UK and Ireland. Clin Endocrinol 86:410–418. https://doi.org/10.1111/cen.13149
Norppa AJ, Kauppala TM, Heikkinen HA, Verma B, Iwai H, Frilander MJ (2018) Mutations in the U11/U12-65K protein associated with isolated growth hormone deficiency lead to structural destabilization and impaired binding of U12 snRNA. RNA 24:396–409. https://doi.org/10.1261/rna.062844.117
Obermannova B, Pfaeffle R, Zygmunt-Gorska A et al (2011) Mutations and pituitary morphology in a series of 82 patients with PROP1 gene defects. Horm Res Paediatr 76:348–354. https://doi.org/10.1159/000332693
Osmundsen AM, Keisler JL, Taketo MM, Davis SW (2017) Canonical WNT signaling regulates the pituitary organizer and pituitary gland formation. Endocrinology 158:3339–3353. https://doi.org/10.1210/en.2017-00581
Patti G, Guzzeti C, Di Iorgi N, Maria Allegri AE, Napoli F, Loche S, Maghnie M (2018) Central adrenal insufficiency in children and adolescents. Best Pract Res Clin Endocrinol Metab 32:425–444. https://doi.org/10.1016/j.beem.2018.03.012
Pekic S, Doknic M, Miljic D et al (2011) Case seminar: a young female with acute hyponatremia and a sellar mass. Endocrine 40:325–331. https://doi.org/10.1007/s12020-011-9516-8
Pellegrini I, Roche C, Quentien MH et al (2006) Involvement of the pituitary-specific transcription factor pit-1 in somatolactotrope cell growth and death: an approach using dominant-negative pit-1 mutants. Mol Endocrinol 20:3212–3227. https://doi.org/10.1210/me.2006-0122
Perez Millan MI, Vishnopolska SA, Daly AZ et al (2018) Next generation sequencing panel based on single molecule molecular inversion probes for detecting genetic variants in children with hypopituitarism. Mol Genet Genomic Med. https://doi.org/10.1002/mgg3.395
Pfaeffle RW, Hunter CS, Savage JJ et al (2008) Three novel missense mutations within the LHX4 gene are associated with variable pituitary hormone deficiencies. J Clin Endocrinol Metab 93:1062–1071. https://doi.org/10.1210/jc.2007-1525
Pfäffle R (2006) Genetics of growth in the normal child. Eur J Endocrinol 155:S27–S33. https://doi.org/10.1530/eje.1.02234
Prasov L, Masud T, Khaliq S et al (2012) ATOH7 mutations cause autosomal recessive persistent hyperplasia of the primary vitreous. Hum Mol Genet 21:3681–3694. https://doi.org/10.1093/hmg/dds197
Pulichino AM, Vallette-Kasic S, Couture C et al (2003) Human and mouse TPIT gene mutations cause early onset pituitary ACTH deficiency. Genes Dev 17:711–716. https://doi.org/10.1101/gad.1065603
Quentien MH, Vieira V, Menasche M et al (2011) Truncation of PITX2 differentially affects its activity on physiological targets. J Mol Endocrinol 46:9–19. https://doi.org/10.1677/JME-10-0063
Raitila A, Lehtonen HJ, Arola J et al (2010) Mice with inactivation of aryl hydrocarbon receptor-interacting protein (Aip) display complete penetrance of pituitary adenomas with aberrant ARNT expression. Am J Pathol 177:1969–1976. https://doi.org/10.2353/ajpath.2010.100138
Rajab A, Kelberman D, de Castro SC et al (2008) Novel mutations in LHX3 are associated with hypopituitarism and sensorineural hearing loss. Hum Mol Genet 17:2150–2159. https://doi.org/10.1093/hmg/ddn114
Ramzan K, Bin-Abbas B, Al-Jomaa L, Allam R, Al-Owain M, Imtiaz F (2017) Two novel LHX3 mutations in patients with combined pituitary hormone deficiency including cervical rigidity and sensorineural hearing loss. BMC Endocr Disord 17:17. https://doi.org/10.1186/s12902-017-0164-8
Rauchman M, Hoffman WH, Hanna JD, Kulharya AS, Figueroa RE, Yang J, Tuck-Miller CM (2001) Exclusion of SIX6 hemizygosity in a child with anophthalmia, panhypopituitarism and renal failure. Am J Med Genet 104:31–36. https://doi.org/10.1002/ajmg.10016
Regal M, Paramo C, Sierra SM, Garcia-Mayor RV (2001) Prevalence and incidence of hypopituitarism in an adult Caucasian population in northwestern Spain. Clin Endocrinol 55:735–740. https://doi.org/10.1046/j.1365-2265.2001.01406.x
Rentzsch P, Witten D, Cooper GM, Shendure J, Kircher M (2019) CADD: predicting the deleteriousness of variants throughout the human genome. Nucleic Acids Res 47:D886–D894. https://doi.org/10.1093/nar/gky1016
Reynaud R, Albarel F, Saveanu A et al (2011) Pituitary stalk interruption syndrome in 83 patients: novel HESX1 mutation and severe hormonal prognosis in malformative forms. Eur J Endocrinol 164:457–465. https://doi.org/10.1530/eje-10-0892
Reynaud R, Jayakody SA, Monnier C et al (2012) PROKR2 variants in multiple hypopituitarism with pituitary stalk interruption. J Clin Endocrinol Metab 97:E1068–E1073. https://doi.org/10.1210/jc.2011-3056
Richards S, Aziz N, Bale S et al (2015) Standards and guidelines for the interpretation of sequence variants: a joint consensus recommendation of the American College of Medical Genetics and Genomics and the Association for Molecular Pathology. Genet Med 17:405–424. https://doi.org/10.1038/gim.2015.30
Richter T, Nestler-Parr S, Babela R et al (2015) Rare disease terminology and definitions-a systematic global review: report of the ISPOR rare disease special interest group. Value Health 18:906–914. https://doi.org/10.1016/j.jval.2015.05.008
Rizzoti K, Brunelli S, Carmignac D, Thomas PQ, Robinson IC, Lovell-Badge R (2004) SOX3 is required during the formation of the hypothalamo-pituitary axis. Nat Genet 36:247–255. https://doi.org/10.1038/ng1309
Rizzoti K, Akiyama H, Lovell-Badge R (2013) Mobilized adult pituitary stem cells contribute to endocrine regeneration in response to physiological demand. Cell Stem Cell 13:419–432. https://doi.org/10.1016/j.stem.2013.07.006
Rochette C, Jullien N, Saveanu A et al (2015) Identifying the deleterious effect of rare LHX4 allelic variants, a challenging issue. PLoS One 10:e0126648. https://doi.org/10.1371/journal.pone.0126648
Roessler E, Ermilov AN, Grange DK, Wang A, Grachtchouk M, Dlugosz AA, Muenke M (2005) A previously unidentified amino-terminal domain regulates transcriptional activity of wild-type and disease-associated human GLI2. Hum Mol Genet 14:2181–2188. https://doi.org/10.1093/hmg/ddi222
Rostomyan L, Potorac I, Beckers P, Daly AF, Beckers A (2017) AIP mutations and gigantism. Ann Endocrinol (Paris) 78:123–130. https://doi.org/10.1016/j.ando.2017.04.012
Sato N, Kamachi Y, Kondoh H, Shima Y, Morohashi K, Horikawa R, Ogata T (2007) Hypogonadotropic hypogonadism in an adult female with a heterozygous hypomorphic mutation of SOX2. Eur J Endocrinol 156:167–171. https://doi.org/10.1530/EJE-06-0606
Schaum N, Karkanias J, Neff NF et al (2018) Single-cell transcriptomics of 20 mouse organs creates a Tabula Muris. Nature 562:367–372. https://doi.org/10.1038/s41586-018-0590-4
Schilter KF, Schneider A, Bardakjian T, Soucy JF, Tyler RC, Reis LM, Semina EV (2011) OTX2 microphthalmia syndrome: four novel mutations and delineation of a phenotype. Clin Genet 79:158–168. https://doi.org/10.1111/j.1399-0004.2010.01450.x
Schilter KF, Reis LM, Schneider A et al (2013) Whole-genome copy number variation analysis in anophthalmia and microphthalmia. Clin Genet 84:473–481. https://doi.org/10.1111/cge.12202
Schneider A, Bardakjian T, Reis LM, Tyler RC, Semina EV (2009) Novel SOX2 mutations and genotype-phenotype correlation in anophthalmia and microphthalmia. Am J Med Genet A 149A:2706–2715. https://doi.org/10.1002/ajmg.a.33098
Seifi M, Walter MA (2018) Axenfeld-Rieger syndrome. Clin Genet 93:1123–1130. https://doi.org/10.1111/cge.13148
Semina EV, Reiter R, Leysens NJ et al (1996) Cloning and characterization of a novel bicoid-related homeobox transcription factor gene, RIEG, involved in Rieger syndrome. Nat Genet 14:392–399. https://doi.org/10.1038/ng1296-392
Seminara SB, Oliveira LM, Beranova M, Hayes FJ, Crowley WF Jr (2000) Genetics of hypogonadotropic hypogonadism. J Endocrinol Investig 23:560–565. https://doi.org/10.1007/BF03343776
Shimada A, Takagi M, Nagashima Y, Miyai K, Hasegawa Y (2016) A novel mutation in OTX2 causes combined pituitary hormone deficiency, bilateral microphthalmia, and agenesis of the left internal carotid artery. Horm Res Paediatr 86:62–69. https://doi.org/10.1159/000446280
Shimo N, Yasuda T, Kitamura T et al (2014) Aniridia with a heterozygous PAX6 mutation in which the pituitary function was partially impaired. Intern Med 53:39–42. https://doi.org/10.2169/internalmedicine.53.1184
Shirakawa T, Nakashima Y, Watanabe S et al (2018) A novel heterozygous GLI2 mutation in a patient with congenital urethral stricture and renal hypoplasia/dysplasia leading to end-stage renal failure. CEN Case Rep 7:94–97. https://doi.org/10.1007/s13730-018-0302-9
Simm F, Griesbeck A, Choukair D et al (2018) Identification of SLC20A1 and SLC15A4 among other genes as potential risk factors for combined pituitary hormone deficiency. Genet Med 20:728–736. https://doi.org/10.1038/gim.2017.165
Skowronska-Krawczyk D, Ma Q, Schwartz M et al (2014) Required enhancer-matrin-3 network interactions for a homeodomain transcription program. Nature 514:257–261. https://doi.org/10.1038/nature13573
Sobrier ML, Maghnie M, Vie-Luton MP, Secco A, di Iorgi N, Lorini R, Amselem S (2006) Novel HESX1 mutations associated with a life-threatening neonatal phenotype, pituitary aplasia, but normally located posterior pituitary and no optic nerve abnormalities. J Clin Endocrinol Metab 91:4528–4536. https://doi.org/10.1210/jc.2006-0426
Sobrier ML, Brachet C, Vié-Luton MP et al (2012) Symptomatic heterozygotes and prenatal diagnoses in a nonconsanguineous family with syndromic combined pituitary hormone deficiency resulting from two novel LHX3 mutations. J Clin Endocrinol Metab 97:E503–E509. https://doi.org/10.1210/jc.2011-2095
Sobrier ML, Tsai YC, Pérez C et al (2015) Functional characterization of a human POU1F1 mutation associated with isolated growth hormone deficiency (IGHD): a novel etiology for IGHD. Hum Mol Genet. https://doi.org/10.1093/hmg/ddv486
Sobrier ML, Tsai YC, Pérez C et al (2016) Functional characterization of a human POU1F1 mutation associated with isolated growth hormone deficiency: a novel etiology for IGHD. Hum Mol Genet 25:472–483. https://doi.org/10.1093/hmg/ddv486
Solomon BD et al (2009) Compound heterozygosity for mutations in PAX6 in a patient with complex brain anomaly, neonatal diabetes mellitus, and microophthalmia. Am J Med Genet A 149A:2543–2546. https://doi.org/10.1002/ajmg.a.33081
Sornson MW, Pineda-Alvarez DE, Balog JZ et al (1996) Pituitary lineage determination by the Prophet of Pit-1 homeodomain factor defective in Ames dwarfism. Nature 384:327–333. https://doi.org/10.1038/384327a0
Strande NT, Riggs ER, Buchanan AH et al (2017) Evaluating the clinical validity of gene-disease associations: an evidence-based framework developed by the clinical genome resource. Am J Hum Genet 100:895–906. https://doi.org/10.1016/j.ajhg.2017.04.015
Sun Y, Bak B, Schoenmakers N et al (2012) Loss-of-function mutations in IGSF1 cause an X-linked syndrome of central hypothyroidism and testicular enlargement. Nat Genet 44:1375–1381. https://doi.org/10.1038/ng.2453
Sutton E, Hughes J, White S et al (2011) Identification of SOX3 as an XX male sex reversal gene in mice and humans. J Clin Invest 121:328–341. https://doi.org/10.1172/JCI42580
Tajima T, Hattorri T, Nakajima T et al (2003) Sporadic heterozygous frameshift mutation of HESX1 causing pituitary and optic nerve hypoplasia and combined pituitary hormone deficiency in a Japanese patient. J Clin Endocrinol Metab 88:45–50. https://doi.org/10.1210/jc.2002-020818
Tajima T, Ohtake A, Hoshino M, Amemiya S, Sasaki N, Ishizu K, Fujieda K (2009) OTX2 loss of function mutation causes anophthalmia and combined pituitary hormone deficiency with a small anterior and ectopic posterior pituitary. J Clin Endocrinol Metab 94:314–319. https://doi.org/10.1210/jc.2008-1219
Tajima T, Nakamura A, Ishizu K (2013) A novel mutation of IGSF1 in a Japanese patient of congenital central hypothyroidism without macroorchidism. Endocr J 60:245–249. https://doi.org/10.1507/endocrj.EJ13-0009
Takagi M, Ishii T, Torii C, Kosaki K, Hasegawa T (2014a) A novel mutation in SOX3 polyalanine tract: a case of Kabuki syndrome with combined pituitary hormone deficiency harboring double mutations in MLL2 and SOX3. Pituitary 17:569–574. https://doi.org/10.1007/s11102-013-0546-5
Takagi M, Narumi S, Asakura Y, Muroya K, Hasegawa Y, Adachi M, Hasegawa T (2014b) A novel mutation in SOX2 causes hypogonadotropic hypogonadism with mild ocular malformation. Horm Res Paediatr 81:133–138. https://doi.org/10.1159/000355279
Takagi M, Nagasaki K, Fujiwara I et al (2015) Heterozygous defects in PAX6 gene and congenital hypopituitarism. Eur J Endocrinol 172:37–45. https://doi.org/10.1530/eje-14-0255
Takagi M, Takahashi M, Ohtsu Y, Sato T, Narumi S, Arakawa H, Hasegawa T (2016) A novel mutation in HESX1 causes combined pituitary hormone deficiency without septo optic dysplasia phenotypes. Endocr J 63:405–410. https://doi.org/10.1507/endocrj.EJ15-0409
Takagi M, Kamasaki H, Yagi H, Fukuzawa R, Narumi S, Hasegawa T (2017) A novel heterozygous intronic mutation in POU1F1 is associated with combined pituitary hormone deficiency. Endocr J 64:229–234. https://doi.org/10.1507/endocrj.EJ16-0361
Tasdemir S, Sahin I, Cayır A et al (2014) Holoprosencephaly: ZIC2 mutation in a case with panhypopituitarism. J Pediatr Endocrinol Metab 27:777–781. https://doi.org/10.1515/jpem-2013-0449
Tatsi C, Sertedaki A, Voutetakis A et al (2013) Pituitary stalk interruption syndrome and isolated pituitary hypoplasia may be caused by mutations in holoprosencephaly-related genes. J Clin Endocrinol Metab 98:E779–E784. https://doi.org/10.1210/jc.2012-3982
Tenenbaum-Rakover Y, Turgeon MO, London S, Hermanns P, Pohlenz J, Bernard DJ, Bercovich D (2016) Familial central hypothyroidism caused by a novel IGSF1 gene mutation. Thyroid 26:1693–1700. https://doi.org/10.1089/thy.2015.0672
Thomas PQ, Dattani MT, Brickman JM et al (2001) Heterozygous HESX1 mutations associated with isolated congenital pituitary hypoplasia and septo-optic dysplasia. Hum Mol Genet 10:39–45. https://doi.org/10.1093/hmg/10.1.39
Tommiska J, Känsäkoski J, Skibsbye L et al (2017) Two missense mutations in KCNQ1 cause pituitary hormone deficiency and maternally inherited gingival fibromatosis. Nat Commun 8:1289. https://doi.org/10.1038/s41467-017-01429-z
Treier M, O’Connell S, Gleiberman A et al (2001) Hedgehog signaling is required for pituitary gland development. Development 128:377–386
Trujillano D, Bertoli-Avella AM, Kumar Kandaswamy K et al (2017) Clinical exome sequencing: results from 2819 samples reflecting 1000 families. Eur J Hum Genet 25:176–182. https://doi.org/10.1038/ejhg.2016.146
Tsai EA, Grochowski CM, Falsey AM et al (2015) Heterozygous deletion of FOXA2 segregates with disease in a family with heterotaxy, panhypopituitarism, and biliary atresia. Hum Mutat 36:631–637. https://doi.org/10.1002/humu.22786
Turton JP, Mehta A, Raza J et al (2005a) Mutations within the transcription factor PROP1 are rare in a cohort of patients with sporadic combined pituitary hormone deficiency (CPHD). Clin Endocrinol 63:10–18. https://doi.org/10.1111/j.1365-2265.2005.02291.x
Turton JP, Reynaud R, Mehta A et al (2005b) Novel mutations within the POU1F1 gene associated with variable combined pituitary hormone deficiency. J Clin Endocrinol Metab 90:4762–4770. https://doi.org/10.1210/jc.2005-0570
Turton JP, Strom M, Langham S, Dattani MT, Le Tissier P (2012) Two novel mutations in the POU1F1 gene generate null alleles through different mechanisms leading to combined pituitary hormone deficiency. Clin Endocrinol 76:387–393. https://doi.org/10.1111/j.1365-2265.2011.04236.x
Vajravelu ME, Chai J, Krock B, Baker S, Langdon D, Alter C, De Leon DD (2018) Congenital hyperinsulinism and hypopituitarism attributable to a mutation in FOXA2. J Clin Endocrinol Metab 103:1042–1047. https://doi.org/10.1210/jc.2017-02157
Vallette-Kasic S, Pellegrini-Bouiller I, Sampieri F et al (2001) Combined pituitary hormone deficiency due to the F135C human Pit-1 (pituitary-specific factor 1) gene mutation: functional and structural correlates. Mol Endocrinol 15:411–420. https://doi.org/10.1210/mend.15.3.0601
Vallette-Kasic S, Brue T, Pulichino AM et al (2005) Congenital isolated adrenocorticotropin deficiency: an underestimated cause of neonatal death, explained by TPIT gene mutations. J Clin Endocrinol Metab 90:1323–1331. https://doi.org/10.1210/jc.2004-1300
van Tijn DA, de Vijlder JJ, Verbeeten B Jr, Verkerk PH, Vulsma T (2005) Neonatal detection of congenital hypothyroidism of central origin. J Clin Endocrinol Metab 90:3350–3359. https://doi.org/10.1210/jc.2004-2444
Vaquerizas JM, Kummerfeld SK, Teichmann SA, Luscombe NM (2009) A census of human transcription factors: function, expression and evolution. Nat Rev Genet 10:252–263. https://doi.org/10.1038/nrg2538
Vincent A, Forster N, Maynes JT et al (2014) OTX2 mutations cause autosomal dominant pattern dystrophy of the retinal pigment epithelium. J Med Genet 51:797–805. https://doi.org/10.1136/jmedgenet-2014-102620
Vivenza D, Godi M, Faienza MF et al (2011) A novel HESX1 splice mutation causes isolated GH deficiency by interfering with mRNA processing. Eur J Endocrinol 164:705–713. https://doi.org/10.1530/EJE-11-0047
Warr A, Robert C, Hume D, Archibald A, Deeb N, Watson M (2015) Exome sequencing: current and future perspectives. G3 (Bethesda) 5:1543–1550. https://doi.org/10.1534/g3.115.018564
Webb EA, AlMutair A, Kelberman D et al (2013) ARNT2 mutation causes hypopituitarism, post-natal microcephaly, visual and renal anomalies. Brain 136:3096–3105. https://doi.org/10.1093/brain/awt218
Welcker JE, Hernandez-Miranda LR, Paul FE, Jia S, Ivanov A, Selbach M, Birchmeier C (2013) Insm1 controls development of pituitary endocrine cells and requires a SNAG domain for function and for recruitment of histone-modifying factors. Development 140:4947–4958. https://doi.org/10.1242/dev.097642
Wingender E, Schoeps T, Haubrock M, Donitz J (2015) TFClass: a classification of human transcription factors and their rodent orthologs. Nucleic Acids Res 43:D97–102 https://doi.org/10.1093/nar/gku1064
Woods KS, Cundall M, Turton J et al (2005) Over- and underdosage of SOX3 is associated with infundibular hypoplasia and hypopituitarism. Am J Hum Genet 76:833–849. https://doi.org/10.1086/430134
Zhao L, Bakke M, Krimkevich Y, Cushman LJ, Parlow AF, Camper SA, Parker KL (2001) Steroidogenic factor 1 (SF1) is essential for pituitary gonadotrope function. Development 128:147–154
Zwaveling-Soonawala N, Alders M, Jongejan A et al (2018) Clues for polygenic inheritance of pituitary stalk interruption syndrome from exome sequencing in 20 patients. J Clin Endocrinol Metab 103:415–428. https://doi.org/10.1210/jc.2017-01660
Acknowledgments
This work was supported by the grant entitled “Cell specific expression in the pituitary gland” awarded to Sally A Camper (PI) by the National Institutes of Health (R01 HD034283) with Peter Gergics as co-investigator on this grant. The author apologizes to other colleagues whose work was not cited due to space limitations. The author would like to thank Sally A. Camper for her careful review and feedback on the manuscript, to the members of her lab collecting information on specific genes/variants, and to his family for their continued support toward his research productivity.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2019 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Gergics, P. (2019). Pituitary Transcription Factor Mutations Leading to Hypopituitarism. In: Igaz, P., Patócs, A. (eds) Genetics of Endocrine Diseases and Syndromes. Experientia Supplementum, vol 111. Springer, Cham. https://doi.org/10.1007/978-3-030-25905-1_13
Download citation
DOI: https://doi.org/10.1007/978-3-030-25905-1_13
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-25904-4
Online ISBN: 978-3-030-25905-1
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)