Abstract
Adoptive T cell transfer (ACT) is a new era for cancer treatment, involving infusion of autologous lymphocytes. Chimeric antigen receptors (CAR) on the surface of T cells are emerging as a novel therapeutic that is giving other direction to T-cell specificity and precision medicine. T cells are engineered modification to recognize specific target antigen and are co-stimulated with intracellular signal to increase the T cell response. CAR-T cells have impressive involvement in outcome on hematological malignancies; however severe toxicities as cytokine release syndrome or neurotoxicity are a challenge to face. Solid tumors have heterogeneous antigens and tumor microenvironment that hinder CAR-T cell efficacy and increase the risk of on-target/off-tumor. Novel strategies to increase CAR-Ts specificity, safety and efficacy are ongoing in clinical trials to improve clinical outcomes in hematological and solid malignances.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Adaptive immune system
- Chimeric antigen receptor (CAR)
- Hematological malignancies
- Solid tumors
- Target antigen
9.1 Introduction
Diverse are the efforts to find new therapeutic options to treat malignancies. For long time several immunotherapy approaches have been tested in cancer to strength the patient’s immune system against tumor. Now we have improved our understanding about tumor immunosurveillance and molecular biology tools, increasing our capacity to personalize immune therapy options with clinical efficacy and safety. An emerging immunotherapy approach is adoptive cell transfer (ACT) that consists in the collection of autologous or allogenic T cells with high affinity to tumor antigens (TA) to fight against patient’s cancer. The most common types of ACT are: tumor infiltrating lymphocytes (TILs) from the tumor microenvironment that are isolated from surgically resected patient’s tumor and are ex vivo propagated to be re-infused back into the same patient [1]. The others ACT types are genetically engineered T cells expressing high affinity receptors (TCRs) to tumour-specific antigen or chimeric antigen receptors (CAR-Ts) that consist of an extracellular antigen-recognition domain and an intracellular signaling domain [2].
9.1.1 CARs Structure Designs
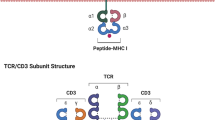
Chimeric antigen receptors are formed by an extracellular antigen-recognition domain usually an antibody single chain variable fragment (scFv) specific for a TA, or less frequently a peptide or protein and an intracellular signaling domain, which usually consists in TCR-associated CD3ζ (CD3 zeta) chain.
The external domain of CAR allows the specific antigen recognition by T cell and, posterior stimulation of intracellular domain that stimulates T cell proliferation, cytolysis and cytokine secretion to eliminate target cell. To generate this T modified cells, is necessary to isolate own patients’ T cells, to activate and genetically modify them using retroviral or lentiviral vectors or non-viral methods such as transposon, and finally to reinfuse back into the same patient. This strategy carries low risk of graft-versus host disease and enables lipid, protein and carbohydrate antigens to be targeted by T cells in a MHC non dependent fashion [3] (Fig. 9.1).
CAR T cell manufacturing and treatment process.
Patient T cells are isolated by leukapheresis, then are in vitro activated by stimulation of T cell by magnetic beads or artificial antigen presenting cells. Cells are genetically engineered CARs are delivered by lenti-viral or retroviral and transposon method. The cells are expanded in culture divices. The patient undergo to prior infusion treatment, and then CARs are re-infusion back
The antigen-recognition domain is anchored to the cell by a flexible spacer/hinge region and a transmembrane domain. The intracellular domain consists of termed signaling domains necessary for T cell activation [4]. There are three CAR-Ts generation. First generation contains CD3ζ signaling chains, as termed signal 1. This CAR-T has limited efficacy in clinical trials , one possibility could be the activation-induced cell death of the transplanted T cells or lack to maintain long-term T cell expansion [5, 6]. To avoid these difficulties second generation CAR-Ts includes in their structure a first generation backbone and two co-stimulatory signaling domains to provide a second activation signal. For example, second generation CD19-CAR-T cells include a CD3ζ chain and CD28 signaling domain, this structure enhances persistence a proliferation of CAR-Ts compared with first-generation CD19-specific CAR-T. In acute lymphoblastic leukemia B (B-ALL) second generation CAR-Ts includes CD28 or 4-1BB (CD137) co-stimulatory signaling domains to enhance the response. Third generation CAR-Ts contains a CD3ζ domain and two co-stimulatory domains that could include CD28, 4.1BB or OX40 (CD143), showing higher antitumor efficacy than second-generation CAR-T cells [7, 8] (Fig. 9.2).
Structure of CAR-T cells generation.
First generation CAR consist in extracellular scFV domain with antigen recognition region, the hinge domain and intracellular activation domain. Second and third generation CAR-Ts had one or two co-stimulatory domain including signals such as CD28, 4-1BB or 0X40. CAR chemeric antigen receptor, CD cluster of differentation, scFV single chain variable fragment
9.2 CAR-Ts and Hematological Malignancies
CAR-Ts efficacy have been proved in hematological malignancies. Clinical trials of CARs-T therapy have mostly been conducted in patients with CD19-positive hematological diseases, such as acute and chronic B leukemia (B-ALL or CLL), follicular lymphoma (FL), diffuse large B-cell lymphoma (DLBCL) and mantle-cell lymphoma. For example, CD19-targeted-CAR-Ts have achieved 70–90% response rate in B-ALL or CLL resulting in an important tool to treat these malignancies. Below the most important trials in hematological diseases are described. Table 9.1 summarizes CD19-specific published trials. Table 9.2 shows the ongoing clinical trials in hematological malignancies.
9.2.1 B-Cell Malignancies
Memorial Sloan Kettering Cancer Center (MSKCC) published their results of second generation CD19 specific-CAR-T (CD28/CD3ζ), called 19–28 z, in 33 relapsed-refractory adults with B-ALL. All patients received conditioning chemotherapy and then 1–3 × 106 19–28 z CAR-T cells/kg. Minimum residual disease (MRD-negative) was achieved in 81% and overall complete response rate (CRR) was 91%. The toxicities reported were cytokine-release syndrome (CRS) and neurological toxicities [9].
The University of Pennsylvania and Children’s Hospital of Philadelphia conducted a trial in 57 pediatric and adult patients with B-ALL treated with CD19 transduced second-generation CAR-Ts cells (4-1BB/ CD3ζ) or CTL019 cells. Patients receive doses of 1–10 × 106 CAR-T cells/kg. This group reported 93% of CRR, 55% had recurrence free survival (RFS) and 79% overall survival at 1 year. Twenty patients relapsed, 13 with CD19 disease. Patients CTL019 persistence had B-cell aplasia, which continued up last assessment (1–39 months) in 24/34 patients with ongoing CR. Cytokine release was seen in 88% of patients [10,11,12].
National Cancer Institute (NCI) performed an “intent-to-treat” clinical trial in 21 children and young adults with relapsed or relapsed B-ALL or NHL. They were treated with CD19-CAR-Ts (CD28/CD3ζ), CRR of 60.8% with 90% of responders negative for minimal residual disease (MDR-) was observed. The median leukemia free survival (mLFS) of MDR-CR responders was 18.7 months; the median disease survival of MDR- CR responders was 49.5%. Severe CRS occurs in 13.5% [13, 14].
The Fred Hutchinson Cancer Research Cancer (FHCRC) group used central memory-enriched CD8 cells for starting material of 29 adults to be treated with CD19-targeted CAR-Ts (CD3ζ/41BB) and defined composition of CD4:CD8 T cells. This treatment approach with a defined subset composition achieved 83% complete response rate. The peak level and duration of persistence of both CD4+ and CD8+ CAR-Ts were associated with clinical response [15, 16]. Posterior update reports 93% of bone marrow remission, these investigators identify as risk factors for severe toxicity CAR-T cell dose and tumor burden [17].
Dr. Porter et al. reported their results of CTL019 in CLL. The overall response rate in heavily pretreated patients CLL was 57% (8/14 patients). The in vivo expansion of CAR-Ts correlated with clinical response. CAR-Ts persisted and remained functional beyond 4 years in the two patients whose achieving CR. All responding patients developed B-cell aplasia and experienced cytokine release syndrome that correspond with T cell proliferation [18].
CD-19 specific CAR-Ts (CD28/CD3ζ) have been studied in DLBCL, indolent lymphoma or CLL. In a multicenter phase 2 trial that enrolled 11 previously treated patients with large B-cell lymphoma, including diffuse large B-cell lymphoma and primary mediastinal B-cell lymphoma. Those patients receiving a conditioning therapy and after CD19-specific CAR-Ts showed 82% objective response, 54% complete response and 28% partial response. With a median follow-up of 15.4 months, 42% of these patients had still response, 40% of them with complete response. The most common adverse events were pyrexia (85%), neutropenia (84%) and anemia 66% [19].
9.3 Multiple Myeloma
CD19-specific CARs-T cells were evaluated in 10 patients with multiple myeloma (MM). Patients received pre-conditioning treatment with autoHSCT and melphalan followed by an infusion of second generation CD19-targeted CARs-T cells (4-1BB/CD3ζ). One patient experienced a complete response for 12 months following treatment and six patients remained progression free [20].
9.3.1 CAR-Ts and Solid Tumors
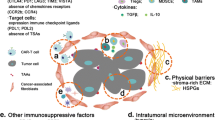
There are diverse research efforts to evaluate efficacy and safety of CAR-Ts in solid tumors, but results are less exciting than findings in hematological malignances. Prior identification of new possible target antigen and posterior preclinical models of solid tumors it is necessary to evaluate efficacy and animal safety of these therapies based on these antigens. The response to CAR-Ts depends on diverse parameters: (1) A good choice of the target epitope, (2) Specific target antigen, (3) CARs structure, CAR-T cell dose, frequency or administration way, (4) Tumor environment, (5) Patient’s lymphodepletion and pre-condition treatment previous to CARs-T administration, (6) CAR-Ts engraftment and trafficking capacity [38].
The ideal target antigen is one that could be found specifically in epithelial cancer cells; however solid tumors have over-expression of proteins that are also expressed in normal cells, making difficult the work of find a specific antigen. Despite of this, there are several efforts to test CAR-T in solid tumors.
9.3.2 EGFR and EGFRvIII
The alternately splice variant of EGFR (EGFRvIII) is commonly associated with glioma cells and is necessary for their survival. A phase 1 trial has been done in 10 recurrent glioblastoma (GBM) patients, whose has been previously treated. After EGFRvIII determination, patients were treated by an infusion of EGFRvIII-CAR-T cells. One patient showed residual stable disease for over 18 months of follow-up. All patients had demonstrable detected transient expansion of EGFRvIII-CAR-T in peripheral blood. Seven patients had posterior surgical intervention, which allowed tissue-specific analysis of EGFRvIII-CAR-T trafficking into the tumor; patients had a patchy pattern of lymphocyte infiltrate com-posed of CD8 T cells after CARs-T infusion compared with pre-infusion brain tumor specimens from the same patient [39].
9.3.3 HER2
The tyrosine-protein kinase receptor erbB2 (HER2) is commonly expressed in diverse epithelial cells such as gastrointestinal, respiratory, urinary and reproductive systems. However, HER2 overexpression has been detected in tumors cells of gastric, breast, colon and ovarian cancer.
A third generation HER2-CAR-T cell (CD28/4-1BB and CD3ζ) was tested in metastatic cancer (NCT00924287 trial). This trial stopped ahead of time because one colon cancer patient with lung and liver metastases died for acute respiratory failure. Post mortem analysis exhibited signs of systemic ischemia and hemorrhagic microangiopathic injury. The lungs had a diffuse alveolar damage with an immediate accumulation of T lymphocyte demonstrated in the patient’s lung. The patient had a marked increase of IFN-ϒ, granulocyte macrophage-colony stimulating factor (GM-CSF), tumor necrosis factor-α (TNF-α), IL and IL-10 after HER-2- CAR-T cell infusion. This trial included in the CAR-T cell structure a scFV based on trastuzumab. One explanation for this severe toxicity could be the recognition and depletion of low levels of ERBB-2 in lung epithelium, triggering pulmonary failure and massive cytokine release [40].
Despite of this severe toxicity there are several ongoing trials with HER2-CAR-T in others tumors such as sarcoma where investigators are using a scFv with lower affinity than trastuzumab-based CAR, therefore with better results in safety setting. Nineteen patients with advanced-stage sarcoma have been treated with these second-generation HER2-specific CAR-T cells (CD28/CD3ζ). HER2-CAR T cells persisted for at least 6 weeks in seven out of nine evaluable patients. HER-CAR-T cells were detected at tumor site in 2 patients. Four patients had stable disease for 12–14 weeks. Three patients with surgery after HER-CAR-T cells infusion had ≥90% necrosis. Median overall survival was 10.3 months [41].
9.3.4 Mesothelin
Mesothelin (MSN) is a novel attractive target for cancer immunotherapy. This protein is low expressed in normal mesothelial cells, but has a high expression in many solid tumors. Physiologically, MSN is expressed on mesothelial cells of pericardium and peritoneal and pleural cavities.It has been found to be overexpressed in mesothelioma and ovarian cancer, and in other tumors such as lung, pancreatic, gastric, endometrial, colon and breast cancer [42, 43].
A clinical trial tested CAR-T cells with mRNA encoding for second-generation MSN-CAR-T (SS1-4-1BB) in advanced mesothelioma or pancreatic tumors by intravenous or intratumor MSN-CAR-T. Cell infusions were well-tolerated and no off-target toxicities were observed (pleuritis, pericarditis or pericarditis). A severe anaphylaxis and cardiac arrest were reported with the third infusion of MSN-CAR-T, secondary to a high production of IgE antibodies targeted against MSN-CAR-T, probably associated with the murine SS1 scFV. Despite of this severe toxic event, the treatment in general was well- tolerated. Antitumor activity was demonstrated by a decrease in tumor-cell numbers in ascitis and a decrease of peritoneal lesions [44].
9.3.5 Disialogangloside GD2
Disialongangloside GD2 is a glycosphingolipid with low-level expression in neural tissues; however tumors as neuroblastoma overexpress this protein. GD2-CAR-T had been investigated in patients with neroblastoma. They used autologous activated T cells (ATCs) and autologus Epstein barr-virus specific T cells (EV-CTLs), each modified with a distinguishable GD2-specific CAR (GD2-CAR-T). Three patients out of 11 with active disease achieved complete remission and persistence of CAR-ATCs or CAR-CTL-S beyond 6 weeks associated with superior clinical outcome [45]. Third generation GD2-CAR-T cells (OX40/CD28/CD3ζ) in patients with neuroblastoma, osteosarcoma and melanoma are under investigation. To increase the safety of this CAR-T, the investigators modified the GD2-CAR-T cells to express inducible caspase 9 (icaspas9) suicide gene [46].
9.3.6 Prostate Specific Membrane Antigen
Prostate specific membrane antigen (PSMA) is a type II membrane protein expressed in most of prostate-cancer cells and tumor –associated neovasculature of many solid tumors [47]. A second generation PMSA-CAR-T cell (CD28/CD3ζ) has been tested in prostate cancer patients. No toxicity was reported, two out of three patients included in this study had stable disease at 6 months of follow up [48]. Similar results are reported in other study that treated prostate cancer patients with second generation PMSA-CAR-T cell (CD28/CD3ζ). Patients had decreased PSA levels, and disease progression was delayed in two out of five patients [49].
9.3.7 Other Tumor Antigens
Several tumor antigens in solid tumors are investigated on clinical trial, they are summarized in Table 9.3. Those antigens include glycoproteins as carcinoembryonic antigen (CEA) expressed on many epithelial tumorsfrequently located atthe gastrointestinal tract. Other protein is the neural cell adhesion molecule L1 (CD171) that is expressed in ovarian cancer, neuroblastoma and melanoma. This protein is also expressed on normal tissues as peripheral nerve and kidney, but with a different glycosylation pattern than CD171 expressed in malignant cells, making it a suitable target for CAR T therapy. Other proteins under investigation are the glypican-3, a surface proteoglycan overexpressed on hepatocellular carcinoma, and the IL-13R, a high affinity monomer receptor overexpressed in 50% of glioblastoma, with low expression in normal brain tissues.
9.3.8 Future: Strategies to Improve the Safety and Efficacy of CARs-T
CAR-Ts have impressive results in clinical trials for B-cells malignancies, however, there are still concerns about inability to control CAR-Ts after patient’s re-infusion back. CAR-Ts have the capacity to attack normal tissue (off-tumor-cross reaction), being the major limiting factor in the clinical setting.
Future challenges to improve CAR-T cells therapy [67].
-
1.
Antigen loss
-
2.
On-Target/off tumor toxicity (CAR-T cell recognize normal tissues and can cause severe and life-threatening toxicities, especially in solid tumors).
-
3.
Tumor Microenvironment (Function as a barrier to CAR-T cells penetration).
-
4.
Production difficulties (Autologous T cells manufacturing)
There are several approaches to improve safety and efficacy of CAR-Ts (Fig. 9.3). New strategy to face antigen loss relapse is for example the modification of CAR-Ts with two distinct CAR molecules with two different binding domains called dual-signaling CAR. Tandem CARs (TanCAR) is other approach, with one CAR molecule containing two different binding domains in tandem that simultaneously targets different antigens, for example HER2 and IL13Rα2 to mitigate tumor antigen escape, showing superior antitumor activity compared with pooled CAR-Ts or co-transduced T cells in mouse glioblastoma model [68].
CAR-T: Novel approaches to improve safety and efficacy.(a) Tandem CAR-T cell had two different tumoral antigen (TA) specific scFvs domains to have a synergic activation of both scFV simultaneously. (b) iCAR- is a combination of inhibitory receptor specific for the antigen present on normal cell but not on tumor cells, to protect normal cells from a CAR-T cell mediated attract. (c) 4th Generation CAR-T cell are associated to a transgene and have the capacity to produce cytokine as IL-12 to increase immune response, (d) Switch Suicide CAR-T structure, (e) target tumor stroma like VEGFR CAR-T, (f) Natural Killer Recognition domain to recognize own antigens and foreign
The inhibitory CAR (iCAR) is a fusion of an antigen recognition domain, usually an antigen expressed on normal tissue, with an inhibitory intracellular domain, which could be a programmed cell death protein 1 (PD-1) or a cytotoxic T-lymphocyte-associated protein 4 (CTLA-4). This fusion leads the inhibition of CARs activation and limits its undesired activation [69]. To improve CARs safety there are also another approach such as suicide genes as inducible caspase-9 (iCaspase-9) switch, included in 19-CAR-T cell encoding vector to remove inappropriately active CARs. This “safety switch” approach modulates the effects of CARTs-19 cells and could reduce severe toxicities related to this therapy [70, 71]. Switchable CARs (sCAR-T) are based on engineering bi-functional switched that consists of a tumor antigen-specific Fab molecule engrafted with a peptide neo-epitope, which is bound exclusively by a peptide-specific switchable CAR-T cell. This switch redirects sCAR-T cells activity through the formation of selective immunological synapses. On this way sCAR-T cell switches and targets cells in a structurally defined and temporally control manner [72].
Natural Killer (NK) cells have receptors capable to discriminate between normal and tumor cells. Recently, NK receptors are being used as antigen recognition domains in CAR-T, to improve tumor recognition by T cells. The receptor NKG2-D links to intracellular T-cell signaling domains and enables this receptor to activate T cells. It is under investigation in diseases like AML, MM and myelodysplastic syndrome [73, 74].
The phenotypic heterogeneity of solid tumors hinders CAR-T cell efficacy in these tumors. After initial tumor reduction by CAR-T cell, the antigen-negative tumor cells that are still alive, not recognized by CAR-T, are probably implicated in tumor relapse. TRUCK T cells or fourth Generation CAR-T cells are modified CAR- T cells to secrete pro-inflammatory cytokines (usually cytokine like IL-12). This TRUCK T cell can release this transgenic protein to regulate T-cell response and active innate immune response cells that can kill negative-antigen cancer cells. The transgenic IL-12 is stored into the CAR-T and only is released when is induced [75].
Tumor microenvironment like tumor-vasculature is important for tumor cell survival. VEGF ligand and their receptors are implicated in cancer. VEGFR-2 is overexpressed on tumor stroma cells and some tumor cells. VEGFR-2-specific-CAR-T cells target tumor stroma cells, without harm normal tissue. This is another possible application of CAR-T cells in solid tumors [76].
Genome editing tools as zinc finger nucleases, meganucleases, transcription activator-like effectors nuclease (TALEN), homing endonuceases, and clustered regularly interspaced short palindromic repeats (CRISPR-Cas) system are successfully applied to engineer T cells. Human genome editing led the opportunity generate “universal” CAR-T cells without a functional endogenous TCR or eliminate immunosuppressive signals such as PDL-1 and CTL-4, improving T cells function [77] (Fig. 9.4).
9.4 Toxicities
The most important toxicities related with CAR-T cell therapies are cytokine release syndrome and neurotoxicity and both have very interesting physiopathology. Similar than happens with other immune treatment such as monoclonal antibodies (MoAB), CAR-T cells administration are associated with an immune response mediated by cytokines. Cytokine release syndrome (CRS) has been observed with CD19-specific, CD22-specific and BCMA-specific CAR-T cells therapy, rates of severe CRS are around 25% among various trials. Symptoms occur any time in the first 2 weeks after CAR-T cell infusion and are related with increase cytokine levels. Tumor necrosis factor (TNF) α increases first and is followed by IFNϒ, IL-1ß, IL-1, IL-6; 1L-8 and IL-10 [78]. Others biochemical abnormalities include elevated C-reactive protein and ferritin levels. The CRS severity is related with tumor burden and the anti-tumor responses. The clinical symptoms include fever, hypotension and less common respiratory failure. Consumptive coagulopathy has been also described and is related with severe CRS in children [79]. Lee et al. suggested a CRS grading scale that it is beginning to be used in clinical trials trying to unify outcomes reports (Table 9.4). Most of the CRS related symptoms are manageable with antipyretic, steroid and intravenous fluids. Despite of, some patients will require supportive care as high doses of vasopressors and ventilatory support. Interleukine- 6 (IL-6) is predominantly elevated in these patients and is related with severe CSR. The monoclonal antibody anti-IL6R, tocilizumab, has been used in B-ALL leukemia treated with CD19-CAR-T with good outcomes. Based on these results, tocilizumab is indicated to treat severe CRS [80, 81]. Investigators are working on developing strategies for mitigate CRS occurrence. The group of Seattle Children’s Hospital (SCRI) has proposed a strategy which aimed to decrease the rates of severe CRS based on tocilizumab or dexamethasone administration, when patients demonstrate persistent symptoms of mild CRS (Table 9.5). This strategy reduces severe CRS rate in approximately 50%, without impact on efficacy or long-term persistence of the CAR-T cells therapy [49]. When the prevention fails or CRS symptoms remain, MKSCC group have proposed a CRS management algorithm (Fig. 9.5) [82].
Neurotoxicity has been observed associated with CAR-T cell therapy, with a wide spectrum of symptoms since mild confusion and aphasia to life-threatening encephalopathy and intractable seizures. Apparently these symptoms are related with cerebral edema secondary to immune activation. It is not known if cerebral edema is a consequence of CAR-T cell therapy as an extreme manifestation of CRS or it is an independent symptom. The major explanation for this pathology is endothelial injury related to cytokine release, contributing to the onset of neurotoxicity, but the exact mechanism of action is still poorly understood [83]. The Fig. 9.4 summarizes the physiopathology of CRS and Neurotoxicity.
Grades 2–4 refer to CTCAE v.4.0 grading.
9.5 Take Home Messages
-
1.
CAR-Ts are a novel precision immunotherapy strategy specifically designed to attack a tumor antigen, using patient’s T cells engineered modification.
-
2.
It is important to select the best target antigen to generate CAR-T cell effective against a specific tumor.
-
3.
Next generation CAR-T cells will be available to improve immune response, decrease off target/on tumor risk, to be more capable to penetrate tumor microenvironment, and to program death or apoptosis.
-
4.
Cytokine release syndrome management is a new challenge in the clinical oncology practice.
References
Topalian SL, Muul LM, Solomon D, Rosenberg SA (1987) Expansion of human tumor infiltrating lymphocytes for use in immunotherapy trials. J Immunol Methods 102(1):127–141
Restifo NP, Dudley ME, Rosenberg SA (2012) Adoptive immunotherapy for cancer: harnessing the T cell response. Nat Rev Immunol 12:269–281
Jackson HJ, Rafiq S, Brentjens RJ (2016) Driving CAR T – cells forward. Nat Rev Clin Oncol 13(6):370–383
Sadelain M, Brentjens R, Rivière I (2013) The basic principles of chimeric antigen receptor design. Cancer Discov 3:388–398
Jensen MC, Popplewell L, Cooper LJ, DiGiusto D, Kalos M, Ostberg JR et al (2010) Antitransgene rejection responses contribute to attenuated persistence of adoptively transferred CD20/CD19-specific chimeric antigen receptor redirected T cells in humans. Biol Blood Marrow Transplant 16(9):1245–1256
Thistlethwaite FC, Gilham DE, Guest RD, Rothwell DG, Pillai M, Burt DJ et al (2017) The clinical efficacy of first-generation carcinoembryonic antigen (CEACAM5)-specific CAR T cells is limited by poor persistence and transient pre-conditioning-dependent respiratory toxicity. Cancer Immunol Immunother 66(11):1425–1436
Savoldo B, Ramos CA, Liu E, Mims MP, Keating MJ, Carrum G et al (2011) CD28 costimulation improves expansion and persistence of chimeric antigen receptor-modified T cells in lymphoma patients. J Clin Invest 121(5):1822–1826
Zhong XS, Matsushita M, Plotkin J, Riviere I, Sadelain M (2010) Chimeric antigen receptors combining 4-1BB and CD28 signaling domains augment PI 3 kinase/AKT/Bcl-X L activation and CD8 T cell-mediated tumor eradication. Mol Ther 18(2):413–420
Park JH, Riviere I, Wang X, Bernal Y, Purdon T, Halton E, Curran KJ, Craig Steven Sauter MS (2015) Efficacy and safety of CD19-targeted 19-28z CAR modified T cells in adult patients with relapsed or refractory B-ALL. J Clin Oncol 33:7010–7010
Grupp SA, Kalos M, Barrett D, Aplenc R, Porter DL, Rheingold SR et al (2013) Chimeric antigen receptor–modified T cells for acute lymphoid leukemia. N Engl J Med 368(16):1509–1518
Maude SL, Frey N, Shaw PA, Aplenc R, Barrett DM, Bunin NJ et al (2014) Chimeric antigen receptor T cells for sustained remissions in leukemia. N Engl J Med 371(16):1507–1517
Maude SL, Teachey DT, Rheingold SR, Shaw PA, Aplenc R, Barrett DM, Barker CS, Callahan C, Frey NV, Nazimuddin F, Lacey SF, Zheng Z, Levine B, Melenhorst JJ, SAG L (2016) Sustained remissions with CD19-specific chimeric antigen receptor (CAR)-modified T cells in children with relapsed/refractory ALL. J Clin Oncol 34:3011–3011
Lee DW, Kochenderfer JN, Stetler-Stevenson M, Cui YK, Delbrook C, Feldman SA et al (2015) T cells expressing CD19 chimeric antigen receptors for acute lymphoblastic leukaemia in children and young adults: a phase 1 dose-escalation trial. Lancet 385(9967):517–528
Lee DW III, Stetler-Stevenson M, Yuan CM et al (2016) Long-term outcomes following CD19 CAR T cell therapy for B-ALL are superior in patients receiving a fludarabine/cyclophosphamide preparative regimen and post-CAR hematopoietic stem cell transplantation. Blood 128(22):218
Turtle CJ, Berger C, Sommermeyer D, Budiarto T, Hanafi L-A, Melville K, Pender B, Steevens N, Chaney C, Heimfeld S, Cherian S, Wood BL, Soma L, Chen X, Jensen M, Sta DGM (2015) Immunotherapy with CD19-specific chimeric antigen receptor (CAR)-modified T cells of defined subset composition. J Clin Oncol 33(15_suppl):3006):3006–3006):3006
Sommermeyer D, Hudecek M, Kosasih PL, Gogishvili T, Maloney DG, Turtle CJ et al (2016) Chimeric antigen receptor-modified T cells derived from defined CD8+ and CD4+ subsets confer superior antitumor reactivity in vivo. Leukemia 30(2):492–500
Turtle CJ, Hanafi L, Berger C, Gooley TA, Cherian S, Hudecek M et al (2016) CD19 CAR – T cells of defined CD4 + : CD8 + composition in adult B cell ALL patients. J Clin Invest 1(6):1–16
Porter DL, Hwang W, Frey NV, Lacey SF, P a S, Loren AW et al (2015) Chimeric antigen receptor T cells persist and induce sustained remissions in relapsed refractory chronic lymphocytic leukemia. Sci Transl Med 7(303):303ra139
Neelapu SS, Locke FL, Bartlett NL, Lekakis LJ, Miklos DB, Jacobson CA et al (2017) Axicabtagene ciloleucel CAR T-cell therapy in refractory large B-cell lymphoma. N Engl J Med. https://doi.org/10.1056/NEJMoa1707447
Garfall AL, Maus MV, Hwang W-T, Lacey SF, Mahnke YD, Melenhorst JJ et al (2015) Chimeric antigen receptor T cells against CD19 for multiple myeloma. N Engl J Med 373(11):1040–1047
Fitzgerald JC, Weiss SL, Maude SL, Barrett DM, Lacey SF, Melenhorst JJ et al (2017) Cytokine release syndrome after chimeric antigen receptor T cell therapy for acute lymphoblastic leukemia. Crit Care Med 45(2):e124–e131
Davila ML, Riviere I, Wang X, Bartido S, Park J, Curran K et al (2014) Efficacy and toxicity management of 19-28z CAR T cell therapy in B cell acute lymphoblastic leukemia. Sci Transl Med 6(224):224ra25
Gardner RA, Finney O, Annesley C, Brakke H, Summers C, Leger K et al (2017) Intent-to-treat leukemia remission by CD19 CAR T cells of defined formulation and dose in children and young adults. Blood 129(25):3322–3331
Maude SL, Barrett DM, Rheingold SR, Aplenc R, Teachey DT, Callahan C et al (2016) Efficacy of humanized CD19-targeted chimeric antigen receptor (CAR)-modified T cells in children and young adults with relapsed/refractory acute lymphoblastic leukemia. Blood 128(22):217 LP–217217
Rossig C, Pule M, Altvater B, Saiagh S, Wright G, Ghorashian S et al (2017) Vaccination to improve the persistence of CD19CAR gene-modified T cells in relapsed pediatric acute lymphoblastic leukemia. Leukemia 31(5):1087–1095
Competitive transfer of αCD19-TCRz-CD28 and αCD19-TCRz-CD137 CAR-T cells for B-cell leukemia/lymphoma – full text view – ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT02685670
Genetically engineered lymphocyte therapy in treating patients with lymphoma that is resistant or refractory to chemotherapy – full text view – ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT01735604
Treatment of relapsed and/or chemotherapy refractory B-cell malignancy by tandem CAR T cells targeting CD19 and CD20 – full text view – ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT03097770
Anti-CD22 chimeric receptor T cells in pediatric and young adults with recurrent or refractory CD22-expressing B cell malignancies – full text view – ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT02315612
Administration of T lymphocytes for Hodgkin’s lymphoma and non-Hodgkin’s lymphoma (CART CD30) – full text view – ClinicalTrials.gov [Internet]. [citado 20 de abril de 2018]. https://clinicaltrials.gov/ct2/show/NCT01316146
Treatment of relapsed and/or chemotherapy refractory CD33 positive acute myeloid leukemia by CART-33 – full text view – ClinicalTrials.gov [Internet]. [citado 20 de abril de 2018]. https://clinicaltrials.gov/ct2/show/NCT01864902
Genetically modified T-cell immunotherapy in treating patients with relapsed/refractory acute myeloid leukemia and persistent/recurrent Blastic Plasmacytoid dendritic cell neoplasm – full text view – ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT02159495
Treatment of chemotherapy refractory multiple myeloma by CART-138 – full text view – ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT01886976
Autologous ROR1R-CAR-T cells for chronic lymphocytic leukemia (CLL) – full text view – ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT02194374
Kappa-CD28 T lymphocytes, chronic lymphocytic leukemia, B-cell lymphoma or multiple myeloma, CHARKALL – full text view – ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT00881920
Safety study of anti LewisY chimeric antigen receptor in myeloma, acute myeloid leukemia or myelodysplastic syndrome – full text view – ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT01716364
Study of T cells targeting B-cell maturation antigen for previously treated multiple myeloma – full text view – ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT02215967
D’Aloia MM, Zizzari IG, Sacchetti B, Pierelli L, Alimandi M (2018) CAR-T cells: the long and winding road to solid tumors review-article. Cell Death Dis 9:282
Fiorentino A, De BP, Chiesa S, Balducci M, Fusco V (2013) Elderly patients with glioblastoma: the treatment challenge. Expert Rev Neurother 13:1099–1105
Morgan RA, Yang JC, Kitano M, Dudley ME, Laurencot CM, Rosenberg SA (2010) Case report of a serious adverse event following the administration of t cells transduced with a chimeric antigen receptor recognizing ERBB2. Mol Ther 18(4):843–851
Ahmed N, Brawley VS, Hegde M, Robertson C, Ghazi A, Gerken C et al (2015) Human epidermal growth factor receptor 2 (HER2) –specific chimeric antigen receptor–modified T cells for the immunotherapy of HER2-positive sarcoma. J Clin Oncol 33(15):1688–1696
Hassan R, Bera T, Mesothelin PI (2004) A new target for immunotherapy. Clin Cancer Res 10:3937–3942
Morello A, Sadelain M, Adusumilli PS (2016) Mesothelin-targeted CARs: driving T cells to solid tumors. Cancer Discov 6:133–146
Maus MV, Haas AR, Beatty GL, Albelda SM, Levine BL, Liu X et al (2013) T cells expressing chimeric antigen receptors can cause anaphylaxis in humans. Cancer Immunol Res 1(1):26–31
Louis CU, Savoldo B, Dotti G, Pule M, Yvon E, Myers GD et al (2011) Antitumor activity and long-term fate of chimeric antigen receptor-positive T cells in patients with neuroblastoma. Blood 118(23):6050–6056
A phase I trial of t cells expressing an anti-GD2 chimeric antigen receptor in children and young adults with GD2+ solid tumors – full text view – ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT02107963
Haffner MC, Kronberger IE, Ross JS, Sheehan CE, Zitt M, Mühlmann G et al (2009) Prostate-specific membrane antigen expression in the neovasculature of gastric and colorectal cancers. Hum Pathol 40(12):1754–1761
Slovin SF, Wang X, Borquez-Ojeda O, Stefanski J, Olszewska M, Taylor C et al (2012) Targeting castration resistant prostate Cancer (CRPC) with autologous PSMA-directed chimeric antigen receptor T cells. Mol Ther 20:S33
Junghans RP, Ma Q, Rathore R, Gomes EM, Bais AJ, Lo ASY et al (2016) Phase I trial of anti-PSMA designer CAR-T cells in prostate Cancer: possible role for interacting interleukin 2-T cell pharmacodynamics as a determinant of clinical response. Prostate 76(14):1257–1270
Autologous T cells redirected to EGFRVIII-with a chimeric antigen receptor in patients with EGFRVIII+ glioblastoma – full text view – ClinicalTrials.gov.
CAR T cell receptor immunotherapy targeting EGFRvIII for patients with malignant gliomas expressing EGFRvIII – full text view – ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT01454596
Her2 chimeric antigen receptor expressing T cells in advanced sarcoma – full text view – ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT00902044
T Cells expressing HER2-specific chimeric antigen receptors (CAR) For patients with glioblastoma – full text view – ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT02442297
CMV-specific cytotoxic T lymphocytes expressing CAR targeting HER2 in patients with GBM – full text view – ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT01109095
Autologous redirected RNA Meso-CIR T cells – full text view – ClinicalTrials.gov [Internet].https://clinicaltrials.gov/ct2/show/NCT01355965
Pilot study of autologous T-cells in patients with metastatic pancreatic cancer – full text view – ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT02465983
CAR T Cell receptor immunotherapy targeting mesothelin for patients with metastatic cancer – full text view – ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT01583686
3rd generation GD-2 chimeric antigen receptor and iCaspase suicide safety switch, neuroblastoma, grain – full text view – ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT01822652
Adoptive transfer of autologous T cells targeted to prostate specific membrane antigen (PSMA) for the treatment of castrate metastatic prostate Cancer (CMPC) – full text view – ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT01140373
Trial of anti-PSMA designer T cells in advanced prostate cancer after non-myeloablative conditioning – full text view – ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT00664196
CAR T cells in treating patients with malignant gliomas overexpressing EGFR – full text view – ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT02331693
Re-directed T cells for the treatment (FAP)-positive malignant pleural mesothelioma – full text view – ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT01722149
Phase I/II study of anti-Mucin1 (MUC1) CAR T cells for patients with MUC1+ advanced refractory solid tumor – full text view – ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT02587689
Engineered neuroblastoma cellular immunotherapy (EnciT)-01 – full text view – ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT02311621
Anti-GPC3 CAR T for treating patients with advanced HCC – full text view – ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT02395250
Genetically modified T-cells in treating patients with recurrent or refractory malignant glioma – full text view – ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT02208362
Wang Z, Wu Z, Liu Y, Han W (2017) New development in CAR-T cell therapy. J Hematol Oncol 10:53
Hegde M, Mukherjee M, Grada Z, Pignata A, Landi D, Navai SA et al (2016) Tandem CAR T cells targeting HER2 and IL13Rα2 mitigate tumor antigen escape. J Clin Invest 126(8):3036–3052
Fedorov VD, Themeli M, Sadelain M (2013) PD-1- and CTLA-4-based inhibitory chimeric antigen receptors (iCARs) divert off-target immunotherapy responses. Sci Transl Med 5(215):215ra172
Diaconu I, Ballard B, Zhang M, Chen Y, West J, Dotti G et al (2017) Inducible caspase-9 selectively modulates the toxicities of CD19-specific chimeric antigen receptor-modified T cells. Mol Ther 25(3):580–592
Gargett T, Brown MP (2014) The inducible caspase-9 suicide gene system as a “safety switch” to limit on-target, off-tumor toxicities of chimeric antigen receptor T-cells. Front Pharmacol 5:235
Rodgers DT, Mazagova M, Hampton EN, Cao Y, Ramadoss NS, Hardy IR et al (2016) Switch-mediated activation and retargeting of CAR-T cells for B-cell malignancies. Proc Natl Acad Sci 113(4):E459–E468
Sentman CL, Meehan KR (2014) NKG2D CARs as cell therapy for Cancer. Cancer J 20(2):156–159
Zhang T, Barber A, Sentman CL (2007) Chimeric NKG2D modified T cells inhibit systemic T-cell lymphoma growth in a manner involving multiple cytokines and cytotoxic pathways. Cancer Res 67(22):11029–11036
Chmielewski M, Abken H (2015) TRUCKs: the fourth generation of CARs. Expert Opin Biol Ther 15(8):1145–1154
Chinnasamy D, Yu Z, Theoret MR, Zhao Y, Shrimali RK, Morgan RA et al (2010) Gene therapy using genetically modified lymphocytes targeting VEGFR-2 inhibits the growth of vascularized syngenic tumors in mice. J Clin Invest 120(11):3953–3968
June CH, O’Connor RS, Kawalekar OU, Ghassemi S, Milone MC (2018) CAR T cell immunotherapy for human cancer. Science 359(6382):1361–1365
Suntharalingam G, Perry MR, Ward S, Brett SJ, Castello-Cortes A, Brunner MD et al (2006) Cytokine storm in a phase 1 trial of the anti-CD28 monoclonal antibody TGN1412. N Engl J Med 355(10):1018–1028
Teachey DT, Lacey SF, Shaw PA, Melenhorst JJ, Maude SL, Frey N et al (2016) Identification of predictive biomarkers for cytokine release syndrome after chimeric antigen receptor T cell therapy for acute lymphoblastic leukemia. Cancer Discov. CD-16-0040
Milone MC (2018) BVG. The pharmacology of T cell therapies. Mol Ther Methods Clin Dev 8:210–221
Lee DW, Gardner R, Porter DL, Louis CU, Ahmed N, Jensen M et al (2014) Current concepts in the diagnosis and management of cytokine release syndrome. Blood 124(2):188–195
Park JH, Rivière I, Gonen M, Wang X, Sénéchal B, Curran KJ et al (2018) Long-term follow-up of CD19 CAR therapy in acute lymphoblastic leukemia. N Engl J Med 378(5):449–459
Gust J, Hay KA, Hanafi L-A, Li D, Myerson D, Gonzalez-Cuyar LF et al (2017) Endothelial activation and blood-brain barrier disruption in neurotoxicity after adoptive immunotherapy with CD19 CAR-T cells. Cancer Discov 7(12):1404–1419
Annesley CE, Summers C, Ceppi F, Gardner RA (2018) The evolution and future of CAR T cells for B-cell acute lymphoblastic leukemia. Clin Pharmacol Ther 103(4):591–598
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2019 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Cruz-Ramos, M., García-Foncillas, J. (2019). CAR-T cell and Personalized Medicine. In: Ruiz-Garcia, E., Astudillo-de la Vega, H. (eds) Translational Research and Onco-Omics Applications in the Era of Cancer Personal Genomics. Advances in Experimental Medicine and Biology, vol 1168. Springer, Cham. https://doi.org/10.1007/978-3-030-24100-1_9
Download citation
DOI: https://doi.org/10.1007/978-3-030-24100-1_9
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-24099-8
Online ISBN: 978-3-030-24100-1
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)