Abstract
Blood pressure telemonitoring (BPT) allows remote transmission of patients’ BP values from their home or the community setting, to the doctor’s office or hospital. Evidence from several clinical trials has supported the efficacy of BPT in improving patients’ compliance and adherence to antihypertensive treatment and in achieving hypertension control, with the consequent possibility to improve cardiovascular protection by preventing the adverse consequences associated with elevated BP levels. Until a few years ago, computer-tailored solutions were the main approach to BPT. In recent years, however, the widespread use of smartphone technologies along with the development of related applications for BP monitoring and remote transmission, have made also possible to implement and deliver BPT via mobile phones (mHealth). This chapter will review the clinical relevance of BPT, either when using computer-based or m-health strategies, addressing important methodological aspects for its clinical application, the evidence on their effects on BP levels and achievement of hypertension control, as well as their advantages and limitations for the overall management and follow-up of hypertension and the yet pending issues to be addressed in future studies.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Digital health (e-health)
- Telemedicine
- Teletransmission
- Mobile health (m-health)
- Blood pressure telemonitoring (BPT)
11.1 Introduction
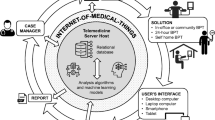
Home blood pressure monitoring (HBPM) represents a cost-effective and well-validated strategy for out-of-office BP monitoring [1]. In consideration of its well-known advantages (i.e., superior prognostic value against conventional clinic BP levels, easy availability, and good acceptance by patients) most hypertension guidelines have recommend the use of HBPM as a useful method for the evaluation of patients with suspected or diagnosed and treated hypertension [2, 3]. Despite its demonstrated benefits, a critical aspect for a proper application of HBPM in clinical practice is data reporting by patients and their interpretation by practicing physicians. In general, BP values obtained by patients at home are reported in handwritten logbooks which sometimes are inaccurate and/or illegible making interpretation of HBPM values difficult. This may discourage physicians from using HBPM data for clinical decision making. A possible solution to this problem was the introduction of HBP measuring devices equipped with memory. However, also in this case the problems of reporting may persist since data could be stored over different time periods in different devices. Alternatively, BP measurements taken from different family members could be stored in the same device memory log, with the risk of having average family BP levels rather than individual BP values. A potentially better solution has been provided more recently by progress in information and communication technologies, which in the last decades have made possible the remote transmission of BP values, measured at home or in a community setting, to the doctor’s office or hospital, by means of telehealth strategies, an approach defined as home BP telemonitoring (HBPT). The conventional approach to HBPT has been based on the use of strategies based on computer-tailored interventions through the Internet (see Fig. 11.1) and a number of observational and randomized controlled studies have shown its efficacy in improving patients’ compliance and adherence to antihypertensive treatment and in achieving more satisfactory hypertension control rates, thus improving cardiovascular protection by preventing the adverse consequences associated with elevated BP levels [4, 5]. In recent years, the widespread use of smartphone technologies, along with the development of applications for BP monitoring and remote transmission, has offered a new approach to HBPT (mHealth). Although, a number of issues, mainly related to the scientific validation of applications developed for mobile healthcare support, still need to be addressed, preliminary data from small studies have suggested the value of these technologies in improving patients’ compliance and adherence to antihypertensive treatment, and in achieving higher BP control rates [6]. This chapter will review the role of BPT in hypertension management, focusing on the reasons for its development, the methodological aspects that should be considered for its clinical implementation as well as its role in improving hypertension control and cardiovascular risk reduction. Current evidence on the use of mobile applications for the management of hypertension will also be addressed by highlighting their potential for clinical use, the current limitations and the yet pending issues to be addressed in future studies.
11.2 Definitions
Telemedicine or telehealth consists in the exchange or delivery of medical information (e.g., health parameters, biological signals, diagnostic images) from one site to another via electronic communications in order to provide diagnosis and care at distance [7].
For many years, telemedicine systems were based mainly on strategies in which teletransmission was performed by means of personal computers equipped with internet connection [8]. However, the worldwide increase in the use of smartphones observed in recent years, along with the development of applications for patients’ data monitoring, has offered new perspectives for telemedicine and the potential to improve interaction between doctors and patients, an approach defined as “ mobile health ” or m-health [9,10,11]. BPT represents a particular application of telemedicine using either computer-tailored or m-health strategies [12]. It consists of automatic data transmission of BP values and additional parameters, from the patient’s living site (home or work place HBPT) or from a professional healthcare environment (e.g., primary care clinic or community pharmacy) to the doctor’s office or to a hospital [12] (Box 11.1).
Box 11.1: Definitions
e-health of Digital health
The use of electronic processes and information and communication technologies to provide healthcare services
Telemedicine (also referred to as telehealth )
Teletransmission of health-related data from one site to another via electronic communications
M-health or “ mobile health ”
Teletransmission of health-related data by means of mobile communication devices (i.e., smartphones)
Blood Pressure Telemonitoring (BPT)
Teletransmission of BP values by means of traditional computer-based or m-health strategies
11.3 Methodological Aspects for Application of BPT
11.3.1 Conventional (eHealth Based) BPT Systems
The wide availability and low cost of automated BP measuring devices, the current advances in communication and information technologies, and the emphasis put by healthcare systems on delivering patient-centered care have stimulated development of home BPT, i.e., a particular application of telemedicine based on either personal computer or m-health strategies (see Fig. 11.1 and Box 11.1).
Devices for home BPT are usually based on automated upper-arm BP monitors which may collect multiple readings either over the 24-h, when applying 24 h ambulatory BP monitoring, or during several days, when repeated self BP measurements are performed by patients at home. Given the large number of monitors commercially available, significant differences among them may be observed in terms of data collection, transmission, reporting and reminders (for BP measurement to be performed and/or for medication intake). A list of available technologies for BP measurement, collection, and teletransmission is presented in Table 11.1.
Overall, home BPT systems require active involvement of patients who should self-monitor their BP levels and other related clinical variables and send these values to a healthcare provider. Current HBPT solutions allow self-BP measurements performed by patients at home to be in the device memory and the forwarded, immediately or periodically, to a remote computer host through a landline broadband or mobile network, and through the web by applying encryption transmission protocols which ensure data integrity and security [13]. Once data are received at the central telemedicine server they are stored and analyzed. Reports are automatically generated and then reviewed by a healthcare professional (usually a technician, a nurse, or a pharmacist), before they are submitted to the reporting physician, although in some instances reports are directly sent to the family doctor in charge. At the end of this process a medical report is forwarded to the patient and referring primary physician through a website, via e-mail or through dedicated smartphone apps (see Fig. 11.1). During all these processes the healthcare professional may also interact with the patient in order to obtain feedbacks on his/her health status and adjust treatment according to the indications of the managing physician (co-intervention or additional support) [14].
11.3.2 mHealth-Based BPT Strategies
As shown in Table 11.2, mHealth-based HBPT strategies can be implemented using different types of smartphone applications (Apps) currently available. Apps that record and store BP values manually inserted by users are the simplest ones, as they only require the user to manually enter the BP values he or she has detected with a measurement device. The main advantages of these apps are flexibility and availability, as they do not require the measurements to be performed at the same time of data entry, and they are not tied to a single device type. Thus, measurements can be performed at any time and with any device of choice. The consequent critical (and obvious) drawback is the consistent risk of errors during transcription of measured BP values into the app.
Apps associated to automated transmission of BP values from the BP measurement devices to the phone have the advantage to be associated to either conventional or automated oscillometric BP measurement devices able to send data to smartphones, or equipped with specifically designed cuffs with an inflating system that works only when paired to a phone. Although wireless cuffs that work with a paired phone have been developed and seem appealing for the user due to their extreme portability, their accuracy has been questioned due to the high variability of BP measures compared to standard BP measurement techniques [15].
Apps that turn the smartphone into a BP measurement device (cuffless measurement) without the need for ad hoc external devices have also been developed based on measurement principles such as pulse transit time assessment or even without the need for any other device than the smartphone, by applying the subject’s finger to the phone camera. Although their extreme ease of use in any circumstance and free availability make them particularly attractive to smartphone users, a major limitation of these apps is the limited evidence from validation studies supporting their accuracy. A recent study evaluating one of these apps indeed indicated that this approach may be highly inaccurate, underestimating higher BP and overestimating lower BP values (mean, SD of the absolute values of the difference between the app and standard were 12.4, 10.5 mmHg for SBP and 10.1, 8.1 mmHg for DBP), thus strongly supporting the need of proper validation of the BP data provided by apps of this kind [16]. The low sensitivity for hypertensive measurements means that approximately four-fifths (77.5%) of individuals with hypertensive BP levels will be falsely reassured that their BP is in the non-hypertensive range. These results have raised awareness on the need to reinforce partnership of app developers, distributors, and regulatory bodies to set and follow standards for safe, validated mHealth technologies.
11.4 BPT: Effects on BP Levels and on Achievement of BP Control
11.4.1 Conventional BPT Systems
Over the last decade, a number of randomized controlled trials as well as their meta-analysis have provided evidence that addition of home BPT is effective in improving adherence and compliance to antihypertensive treatment, achievement of hypertension control, and related medical and economic outcomes in hypertensive patients [4, 12,13,14, 17,18,19,20], especially in those with treatment-resistant hypertension due to poor compliance with multiple drug prescriptions [21] (Fig. 11.2).
Percentage of patients with daytime ambulatory BP normalization (systolic BP <130 mmHg and diastolic BP <80 mmHg). In this study, hypertensive patients were randomized to be conventionally managed based on office BP measurement (withe bars, n = 111) or to be managed based on teletransmission of home BP values (gray bars: n = 187). Modified from Parati, et al. [4] by permission
In one of the largest meta-analysis of randomized controlled studies including a total of 23 studies (n = 7,037 hypertensive patients) regular implementation of BPT at home during a 6-month follow-up period, was associated with significantly greater reductions in both office [average and 95% confidence interval: 4.7 (6.2, 3.2) mmHg for SBP and 2.5 (3.3, 1.6) mmHg for DBP; p<0.001 for both] and 24-hour ambulatory BP [3.5 (5.3, 1.6 mmHg for SBP with p<0.001 and 1.4 (2.9, 0.0) mmHg for DBP with p = 0.051], and with a significantly higher chance of achieving office BP normalization [relative risk and 95% confidence interval: 1.16 (1.04, 1.29), p = 0.007] as compared to usual care (based on periodic BP measurements and visits at the doctor’s office, with no remote BP monitoring) [18]. The improvements in achievement of BP control rates obtained with the BPT intervention resulted in a significantly larger prescription of antihypertensive medications [0.40 (0.17, 0.62), p<0.001], but a similar rate of office consultations. Healthcare costs were significantly (p<0.0001) larger in the BPT group [+662.92 (+540.81, +785.04) euros per patient], but were similar to those sustained by the patients in the usual care group when costs of the technology were removed and only medical costs were considered [–12.4 (–930.52, +906.23) euros, p = 0.767]. More recently, a larger meta-analysis of 46 randomized controlled trials including 13,875 hypertensive patients, further provided evidence on the superiority of BPT in improving achievement of BP control versus usual care [22]. Further relevant evidence on the usefulness of home BPT was recently provided by the TASMINH4 study [5]. This large randomized controlled trial (n = 1182) comparatively evaluated the efficacy of self BP monitoring (self-monitoring group, n = 395), to self-monitoring blood pressure with telemonitoring (telemonitoring group, n = 393), or to usual care (clinic blood pressure; usual care group, n=394) in patients with poorly controlled blood pressure levels. After a 12-month follow-up period, SBP was lower in both intervention groups compared with usual care (self-monitoring, 137·0 [SD 16·7] mm Hg and telemonitoring, 136·0 [16·1] mmHg vs. usual care, 140·4 [16·5]; adjusted mean differences vs. usual care: self-monitoring alone, –3·5 mmHg [95% CI –5·8 to –1·2]; telemonitoring, –4·7 mm Hg [–7·0 to –2·4]). No difference between the self-monitoring and telemonitoring groups was recorded (adjusted mean difference –1·2 mm Hg [95% CI –3·5 to 1·2]), although BP reductions seemed to be quicker in the telemonitoring group.. This study thus showed evidence that self-monitoring, with or without telemonitoring, when used by general practitioners to titrate antihypertensive medication in individuals with poorly controlled blood pressure, leads to significantly lower BP than titration guided by clinic readings [5].
Of note, in most studies a high degree of acceptance of technologies by patients and physicians and a high degree of adherence to telemonitoring programs have been documented [12, 14].
An important aspect of any BPT strategy, is the active participation of health personnel in order to guide patients during BP measurement at home as well as to take decisions regarding therapy [1, 23]. Evidence in this regard was provided by a recent meta-analysis of randomized trials comparing self-monitoring to no-self-monitoring in hypertensive patients by showing that home BPT in conjunction with co-interventions (i.e., medication titration by a case manager, education or lifestyle counselling) may induce significant larger and persistent (up to 12 months) BP reductions than compared to self BP monitoring alone [1] (see Fig. 11.2). Overall, self-monitoring was associated with reduced clinic SBP compared to usual care at 12 months (–3.2 mmHg, [95% CI –4.9, –1.6 mmHg]). However, this effect was strongly influenced by the intensity of co-intervention ranging from no effect with self-monitoring alone (–1.0 mmHg [–3.3, 1.2]), to a 6.1 mmHg (–9.0, –3.2) reduction when monitoring was combined with intensive support [1]. The effectiveness of self-monitoring of BP levels to improve achievement of BP control was shown to be largely dependent on the degree of involvement and participation of health personnel [1] (see Fig. 11.3).
Impact of self-monitoring of BP on the RR of uncontrolled BP at 12 months according to level of co-intervention support (15 studies). Best results were obtained when self-BP monitoring was coupled with web/phone feedback and education or with counselling/telecounselling. Adapted from Tucker et al. [1] by permission. RR of uncontrolled BP adjusted for age, sex, baseline clinic BP, and history of diabetes. The trials are grouped into the four levels of intervention, and I2 and P values are shown for each level of intervention and for the overall analysis. BP blood pressure, RR relative risk
11.4.2 m-Health BPT Systems
The benefits of BPT based on m-health interventions have also been tested by some clinical trials showing them useful for the management of BP levels and other cardiovascular risk factors (i.e., smoking, blood glucose, lipids, control of body weight) [24,25,26] being particularly promising for the management of chronic diseases [27] and in conditions characterized by an elevated cardiovascular risk (i.e., for the management of diabetes mellitus patients). In the particular case of hypertension management, preliminary evidence, mostly from small studies, has indicated m-health technologies to be of value to improve achievement of BP control rates and other BP-related outcomes while reducing healthcare costs [6, 20, 28]. In a recent scientific statement of the American Heart Association about the use of mHealth apps for cardiovascular prevention [29] a specific section was dedicated to address the effectiveness of strategies based on mobile apps in achievement of BP control. In the most representative trials that compared mHealth-based BPT strategies versus usual care (consisting of standard visits in the office of a physician), a net reduction in systolic BP of 2.1–8.3 mmHg was detected in favor of the former approach. It should be mentioned, however, that in the vast majority of studies considered for this report, the follow-up was short (less than 12 months, with most of the studies lasting less than 6 months), with no data on mid- to long-term outcomes, which prevented investigators from reliably evaluating adherence to management strategies. Additionally, only three studies used an intention-to-treat approach for data analysis which might have lead to overestimation of the effectiveness of the investigated tools, limiting the applicability of results to real life. Overall, this report highlighted the need for blinded, prospective randomized clinical trials addressing the role of mHealth strategies for BPT, focusing on hard outcomes over longer follow-up times. Evidence in this regard will be provided by the ongoing ESH CARE App project, a joint initiative between the Italian Society of Hypertension and the ESH/ESC aimed at developing and evaluating a new app for BP management. The ESH CARE app allows the user to collect his/her BP values, along with information on ongoing drug therapy (with the possibility to set reminders for pill intake on the phone). It also allows to send the stored BP and heart rate values into a dedicated website, where they are saved in an encrypted end-to-end form. These data may then be managed, organized, and analyzed by a dedicated patient’s management system (“Misuriamo” platform), allowing physicians in charge to schematically evaluate BP control, cardiovascular risk level, and drug intake and to more precisely titrate drug prescription, with the consequent possibility to implement an accurate and continuous supervision of patients progress and achieved cardiovascular protection. Preliminary data on the effects of the combined use of the mobile app and the online platform “Misuriamo” (the so-called POST, “Patient Optimal Strategy of Treatment”) was tested in a pilot study in Northern Italy [6]. Overall, nine general practitioners randomized 690 consecutive uncontrolled hypertensive patients to either usual care or to the POST strategy. After 6 months of follow-up, achievement of office BP control (i.e., <140/90 mmHg) was significantly higher in the POST group (72.3%) compared to the control group (40.0%). Remarkably, achievement of Home BP control (i.e., daytime home BP <135/85 mmHg, average of 6 days) in the in the POST group was significantly more frequent than that in office BP levels (87.5% versus 72.3%, respectively), thus strongly supporting the favorable impact of home BPT based on a mHealth strategy for hypertension management (see Fig. 11.4).
Achievement of office and home BP control in the “Patient Optimal Strategy of Treatment” (POST group) versus control group after 6 months of follow-up in the ESH CARE App project. Data from Albini et al. [6]
Upcoming studies in different countries are being planned to further evaluate the impact on hypertension control by a management strategy based on the ESH CARE app associated to the online platform (the so-called POST strategy), by focusing not only on the possibility of a better control of BP levels over 24 h, but also on the reduction/prevention of organ damage in high-risk hypertensive patients uncontrolled by drug therapy administered according to usual care, and to evaluate whether the POST strategy grants a reduction in cardiovascular mortality and morbidity in hypertensive uncontrolled patients, thus addressing the need of large randomized controlled trials with a long follow-up time.
11.5 Advantages and Limitations of BPT
11.5.1 Conventional BPT
As mentioned above, a major advantage of conventional BPT solutions based on eHealth strategies is the possibility to empower hypertensive patients (patient-centered care) by building feelings of control and support for chronic disease self-management [30]. BPT facilitates patients to communicate with their doctors, without the need to travel long distances, which translates into a decreased transportation burden and time savings [31]. In due course, physicians and healthcare professionals may reach patients beyond their office, track their health status, and quickly and easily communicate with them. This represents an important advantage for the management of a chronic disease such as hypertension by allowing a closer long-term follow-up of treated hypertensive patients. In case of poor BP control or in the presence of acute symptoms or sudden BP rises, physicians may indeed easily indicate patients to alter their health behaviors or modify antihypertensive medication between visits, avoiding the need to wait months between visits for adjustments. In addition, several BPT systems allow sending automatic reminders to patients indicating the time of BP measurement and/or of medication intake, and may also alert the health provider about new changes in a patient’s health that may manifest with uncontrolled BP. Because of these unique characteristics, BPT systems have the potential to overcome not only physicians’ inertia but also patients’ low compliance/adherence to treatment, which ultimately translates into improvements in hypertension control rates and BP-related cardiovascular complications.
Despite all these important benefits, implementation of BPT solutions in the daily practice may be difficult due to cultural, structural, or financial barriers (Table 11.3) [32].
Poor informatics skill levels of healthcare professionals and patients, lack of adequate knowledge of BP measurement and hypertension guidelines by doctors, all represent major cultural barriers to the routine use of BPT. The incomplete evidence on the clinical efficacy and economic benefit of BPT provided so far by randomized studies, technological barriers, high costs of devices, heterogeneity of solutions and technologies, lack of infrastructures and standards, all hinder the dissemination of telehealth strategies. Regarding the duration of the studies, most current evidence on BPT is based on studies of relatively short duration (<12 months) and in the few studies looking at longer-term outcomes, no evidence of better or sustained effect could be provided. Additionally, no definition of the optimal BPT-based healthcare delivery model could be derived from the studies performed so far, due to the heterogeneity of interventions, technologies and study designs.
11.5.2 mHealth-Based BPT Systems
Mobile phones, which had been traditionally used for communications between patients and doctors only (i.e., through phone calls or SMS) [33], have not only presented a widespread use in recent years but have also expanded their applications giving new possibilities for improving BPT systems [34]. Mobile phones may indeed provide wireless diagnostic and clinical decision support tools to healthcare providers for monitoring health status or improving health outcomes, overcoming many of the technical and financial difficulties (installation and maintenance costs) of conventional BPT systems. Smartphone apps can empower patients with accurate medical information (i.e., educational sections), provide tools to promote self-monitoring and self-management, tracking services (body weight, physical activity), and encourage greater participation in medical decision making by tools that improve adherence to treatment (through reminders and tracking of drug intake) [35]. Mobile phones may thus represent an excellent tool to improve hypertension management in a population basis, i.e., by allowing billions of people to regularly check their BP status and to turn a mobile appliance into an important tool for improving BP control and cardiovascular risk prevention.
Although it is unquestionable that the increasing use of m-health technologies due to the large availability of user-friendly smartphones will circumvent the technical challenge of BPT and provide more flexible and cheap platforms to enhance patient care, it should be mentioned, however that the development and diffusion of these solutions in most cases, has not been accompanied by validation studies (i.e., in order to evaluate their accuracy in measuring biological variables) and standardization of protocols for data transmission and use. Indeed, while a large number of apps dedicated to hypertension management and, in general, related to health issues can be found on web stores, only very few of them can be considered accurate and safe for clinical use.
A critical meta-analysis of 107 mobile health applications designed for the management of hypertension found that only 2.8% of the apps were developed by healthcare professional agencies, none provided any documentation of validation against a gold standard in patients with hypertension, and none formally obtained approval for use as a measuring device by the US Food and Drug Administration or EC [35]. The same meta-analysis also showed that while many apps are positioned in the market and in the online stores based on their popularity rankings (i.e., number of downloads by users) there are still no guidelines nor critical and standardized methods for validating their quality, accuracy, efficacy and safety based on scientific criteria, in order to recommend their use for clinical purposes [35]. Because of all these critical issues, the great opportunity for the improvement of individual and public health carried by mHealth solutions might paradoxically turn into a possible risk for users. Assessing mobile apps is a challenge, we need adapted guidelines and expert and end user evaluation [36].
Another important limitation of studies addressing the value of mhealth systems for BPT is the extremely high level of heterogeneity among them, i.e., almost every smartphone producer has already developed its own healthcare-related app, along with accessories like smartbands and smartwatches, for detection of BP levels and related hemodynamic variables (i.e., heart rate, heart rate variability, physical activity, sleep quality). Lack of standardization in this field does indeed represent a factor that could hamper the possibility of summarizing data on impact on outcome and of drawing general assumptions and reducing the strength of the evidence provided. Future research needs to explore the specific outcomes of BPT interventions to determine their relative value. It should also determine which BPT provision model best applies to daily clinical practice and gives the maximum benefit. Such studies should particularly be focused on high-risk hypertensive patients, for whom an optimal BP control is particularly difficult to attain, also evaluating whether the benefit of BPT intervention is sustained in the long term.
Although there is still limited evidence on the use of mHealth technologies in hypertension management, a list of potential benefits and drawbacks in hypertension management is reported in Table 11.4.
11.6 Conclusions
Increasing evidence has indicated a substantial contribution of telemedicine and Information Technology to Hypertension management. When properly implemented on a regular basis, the combined use of devices that allow patients to self-measure BP at home, transmit the reading to their doctors, and get a feedback could induce an increased compliance through education and involvement of the patients in the management of their own health, plus improving doctor-patients relationship. Current evidence suggests that conventional BPT systems based on eHealth technologies not only have the potential to improve achievement of hypertension control rates, but also to enhance cardiovascular protection by preventing the cardiovascular consequences associated with elevated BP levels. This is of particular value in patients needing a tighter BP control (e.g., at high cardiovascular risk or with comorbidities) or requiring monitoring of multiple vital signs. BPT is in general well accepted by patients and may help to reduce the frequency of face-to-face consultations, and to avoid unnecessary clinic access. In the last instance, such an approach would translate in increased health and reduced restrain healthcare expenditure (i.e., human and technical costs). The increasing number of available mobile apps related to hypertension management and their usage by smartphone owners has led to the recent introduction of BPT solutions based on m-health technology. Although preliminary data from small studies have suggested the efficacy of these technologies to increase patients’ compliance and adherence to antihypertensive treatment, thus improving rates of BP control, evidence is still needed from validation studies evaluating their accuracy as well as from population-based outcome studies showing whether implementing these technologies may result in benefits for the long-term management of hypertension and to improve cardiovascular protection.
References
Tucker KL, Sheppard JP, Stevens R, Bosworth HB, Bove A, Bray EP, et al. Self-monitoring of blood pressure in hypertension: a systematic review and individual patient data meta-analysis. PLoS Med. 2017;14(9):e1002389.
Whelton PK, Carey RM, Aronow WS, Casey DE Jr, Collins KJ, Dennison Himmelfarb C, et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA guideline for the prevention, detection, evaluation, and management of high blood pressure in adults: a report of the American College of Cardiology/American Heart Association task force on clinical practice guidelines. Hypertension. 2018;71(6):e13–e115.
Williams B, Mancia G, Spiering W, Agabiti Rosei E, Azizi M, Burnier M, et al. 2018 Practice Guidelines for the management of arterial hypertension of the European Society of Hypertension and the European Society of Cardiology: ESH/ESC Task Force for the Management of Arterial Hypertension. J Hypertens. 2018;36(12):2284–309.
Parati G, Omboni S, Albini F, Piantoni L, Giuliano A, Revera M, et al. Home blood pressure telemonitoring improves hypertension control in general practice. The TeleBPCare study. J Hypertens. 2009;27(1):198–203.
McManus RJ, Mant J, Franssen M, Nickless A, Schwartz C, Hodgkinson J, et al. Efficacy of self-monitored blood pressure, with or without telemonitoring, for titration of antihypertensive medication (TASMINH4): an unmasked randomised controlled trial. Lancet. 2018;391(10124):949–59.
Albini F, Xiaoqiu L, Torlasco C, Soranna D, Faini A, Ciminaghi R, et al. An ICT and mobile health integrated approach to optimize patients’ education on hypertension and its management by physicians: the patients optimal strategy of treatment(POST) pilot study. Conf Proc IEEE Eng Med Biol Soc. 2016;2016:517–20.
Sood S, Mbarika V, Jugoo S, Dookhy R, Doarn CR, Prakash N, et al. What is telemedicine? A collection of 104 peer-reviewed perspectives and theoretical underpinnings. Telemed J E Health. 2007;13(5):573–90.
TR. E. The eHealth Landscape: A Terrain Map of Emerging Information and Communication Technologies in Health and Health Care;2001.
Silva BM, Rodrigues JJ, de la Torre Diez I, Lopez-Coronado M, Saleem K. Mobile-health: a review of current state in 2015. J Biomed Inform. 2015;56:265–72.
Akter S, D’Ambra J. P. R. Trustworthiness in mHealth information services: an assessment of a hierarchical model with mediating and moderating effects using partial least squares (PLS). J Am Soc Inf Sci Technol. 2011;62:100–16.
Baig MM, GholamHosseini H, Connolly MJ. Mobile healthcare applications: system design review, critical issues and challenges. Australas Phys Eng Sci Med. 2015;38(1):23–38.
Omboni S, Ferrari R. The role of telemedicine in hypertension management: focus on blood pressure telemonitoring. Curr Hypertens Rep. 2015;17(4):535.
Parati G, Omboni S. Role of home blood pressure telemonitoring in hypertension management: an update. Blood Press Monit. 2010;15(6):285–95.
Parati G, Dolan E, McManus RJ, Omboni S. Home blood pressure telemonitoring in the 21st century. J Clin Hypertens (Greenwich). 2018;20(7):1128–32.
Grim CE. Home blood pressure devices for the iPhone do not get the same readings on the same person. J Am Soc Hypertens. 2014;8:e54–5.
Plante TB, Urrea B, MacFarlane ZT, Blumenthal RS, Miller ER 3rd, Appel LJ, et al. Validation of the instant blood pressure smartphone app. JAMA Intern Med. 2016;176(5):700–2.
Collaborators GBDRF, Forouzanfar MH, Alexander L, Anderson HR, Bachman VF, Biryukov S, et al. Global, regional, and national comparative risk assessment of 79 behavioural, environmental and occupational, and metabolic risks or clusters of risks in 188 countries, 1990–2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet. 2015;386(10010):2287–323.
Omboni S, Gazzola T, Carabelli G, Parati G. Clinical usefulness and cost effectiveness of home blood pressure telemonitoring: meta-analysis of randomized controlled studies. J Hypertens. 2013;31(3):455–67;discussion 467-8.
Omboni S, Guarda A. Impact of home blood pressure telemonitoring and blood pressure control: a meta-analysis of randomized controlled studies. Am J Hypertens. 2011;24(9):989–98.
Omboni S, Caserini M, Coronetti C. Telemedicine and M-health in hypertension management: technologies, applications and clinical evidence. High Blood Press Cardiovasc Prev. 2016;23(3):187–96.
Ogedegbe G, Schoenthaler A. A systematic review of the effects of home blood pressure monitoring on medication adherence. J Clin Hypertens (Greenwich). 2006;8(3):174–80.
Duan Y, Xie Z, Dong F, Wu Z, Lin Z, Sun N, et al. Effectiveness of home blood pressure telemonitoring: a systematic review and meta-analysis of randomised controlled studies. J Hum Hypertens. 2017;31(7):427–37.
Uhlig K, Patel K, Ip S, Kitsios GD, Balk EM. Self-measured blood pressure monitoring in the management of hypertension: a systematic review and meta-analysis. Ann Intern Med. 2013;159(3):185–94.
Quinn CC, Clough SS, Minor JM, Lender D, Okafor MC, Gruber-Baldini A. WellDoc mobile diabetes management randomized controlled trial: change in clinical and behavioral outcomes and patient and physician satisfaction. Diabetes Technol Ther. 2008;10(3):160–8.
Quinn CC, Shardell MD, Terrin ML, Barr EA, Ballew SH, Gruber-Baldini AL. Cluster-randomized trial of a mobile phone personalized behavioral intervention for blood glucose control. Diabetes Care. 2011;34(9):1934–42.
Liang X, Wang Q, Yang X, Cao J, Chen J, Mo X, et al. Effect of mobile phone intervention for diabetes on glycaemic control: a meta-analysis. Diabet Med. 2011;28(4):455–63.
Goldberg EM, Levy PD. New approaches to evaluating and monitoring blood pressure. Curr Hypertens Rep. 2016;18(6):49.
Purcell R, McInnes S, Halcomb EJ. Telemonitoring can assist in managing cardiovascular disease in primary care: a systematic review of systematic reviews. BMC Fam Pract. 2014;15:43.
Burke LE, Ma J, Azar KM, Bennett GG, Peterson ED, Zheng Y, et al. Current science on consumer use of mobile health for cardiovascular disease prevention: a scientific statement from the American Heart Association. Circulation. 2015;132(12):1157–213.
Cottrell E, McMillan K, Chambers R. A cross-sectional survey and service evaluation of simple telehealth in primary care: what do patients think? BMJ Open. 2012;2(6)
Friedman RH. Automated telephone conversations to assess health behavior and deliver behavioral interventions. J Med Syst. 1998;22(2):95–102.
Wood PW, Boulanger P, Padwal RS. Home blood pressure telemonitoring: rationale for use, required elements, and barriers to implementation in Canada. Can J Cardiol. 2017;33(5):619–25.
de Jongh T, Gurol-Urganci I, Vodopivec-Jamsek V, Car J, Atun R. Mobile phone messaging for facilitating self-management of long-term illnesses. Cochrane Database Syst Rev. 2012;12:CD007459.
Parati G, Torlasco C, Omboni S, Pellegrini D. Smartphone applications for hypertension management: a potential game-changer that needs more control. Curr Hypertens Rep. 2017;19(6):48.
Kumar N, Khunger M, Gupta A, Garg N. A content analysis of smartphone-based applications for hypertension management. J Am Soc Hypertens. 2015;9(2):130–6.
Ranasinghe M, Cabrera A, Postel-Vinay N, Boyer C. Transparency and quality of health apps: the HON approach. Stud Health Technol Inform. 2018;247:656–60.
Acknowledgment
Disclosure: SO is scientific consultant of Biotechmed Ltd. provider of telemedicine services.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2020 The Editor(s) (if applicable) and The Author(s), under exclusive license to Springer Nature Switzerland AG, part of Springer Nature
About this chapter
Cite this chapter
Parati, G. et al. (2020). Home Blood Pressure Telemonitoring: Conventional Approach and Perspectives from Mobile Health Technology. In: Stergiou, G., Parati, G., Mancia, G. (eds) Home Blood Pressure Monitoring. Updates in Hypertension and Cardiovascular Protection. Springer, Cham. https://doi.org/10.1007/978-3-030-23065-4_11
Download citation
DOI: https://doi.org/10.1007/978-3-030-23065-4_11
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-23064-7
Online ISBN: 978-3-030-23065-4
eBook Packages: MedicineMedicine (R0)