Abstract
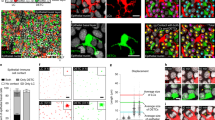
Langerhans cells (LCs) are intraepidermal dendritic cells that extend their dendrites between keratinocytes to form a dense network that covers the entire body. The mammalian epidermis has two diffusion barriers, the stratum corneum and tight junctions (TJs). In their resting state, LCs sit underneath these two barriers. Once activated, LCs elongate their dendrites to dock with, or penetrate through, TJs, which allows them to survey the environment between the two barriers. Here, we describe a method to visualize this dynamic interaction of TJs and LCs in 3D by using mouse ear epidermal sheets.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Langerhans P (1868) Ueber die Nerven der menschlichen Haut. Virchows Arch 44:325–338
Bergstresser PR, Toews GB, Streilein JW (1980) Natural and perturbed distributions of Langerhans cells: responses to ultraviolet light, heterotopic skin grafting, and dinitrofluorobenzene sensitization. J Invest Dermatol 75:73–77
Zimmerli S, Hauser C (2007) Langerhans cells and lymph node dendritic cells express the tight junction component claudin-1. J Invest Dermatol 127:2381–2390
Merad M, Ginhoux F, Collin M (2008) Origin, homeostasis and function of Langerhans cells and other langerin-expressing dendritic cells. Nat Rev Immunol 8:935–947
Kubo A, Nagao K, Yokouchi M, Sasaki H, Amagai M (2009) External antigen uptake by Langerhans cells with reorganization of epidermal tight junction barriers. J Exp Med 206:2937–2946
Kaplan DH (2010) In vivo function of Langerhans cells and dermal dendritic cells. Trends Immunol 31:446–451
Nagao K, Ginhoux F, Leitner WW, Motegi S, Bennett CL, Clausen BE, Merad M, Udey MC (2009) Murine epidermal Langerhans cells and langerin-expressing dermal dendritic cells are unrelated and exhibit distinct functions. Proc Natl Acad Sci U S A 106:3312–3317
Thomas WR, Edwards AJ, Watkins MC, Asherson GL (1980) Distribution of immunogenic cells after painting with the contact sensitizers fluorescein isothiocyanate and oxazolone. Different sensitizers form immunogenic complexes with different cell populations. Immunology 39:21–27
Larsen CP, Steinman RM, Witmer-Pack M, Hankins DF, Morris PJ, Austyn JM (1990) Migration and maturation of Langerhans cells in skin transplants and explants. J Exp Med 172:1483–1493
Nishibu A, Ward BR, Jester JV, Ploegh HL, Boes M, Takashima A (2006) Behavioral responses of epidermal Langerhans cells in situ to local pathological stimuli. J Invest Dermatol 126:787–796
Kubo A, Nagao K, Amagai M (2011) Epidermal barrier dysfunction and cutaneous sensitization in atopic diseases. J Clin Invest 122:440–447
McGrath JA, Uitto J (2008) The filaggrin story: novel insights into skin-barrier function and disease. Trends Mol Med 14:20–27
Oyoshi MK, He R, Kumar L, Yoon J, Geha RS (2009) Cellular and molecular mechanisms in atopic dermatitis. Adv Immunol 102:135–226
Medawar P (1941) Sheets of pure epidermal epithelium from human skin. Nature 148:783
Felsher Z (1947) Studies on the adherence of the epidermis to the corium. J Invest Dermatol 8:35–47
Diaz LA, Heaphy MR, Calvanico NJ, Tomasi TB, Jordon RE (1977) Separation of epidermis from dermis with sodium thiocyanate. J Invest Dermatol 68:36–38
Blank IH, Miller OG (1950) A method for the separation of the epidermis from the dermis. J Invest Dermatol 15:9–10
Van Scott EJ (1952) Mechanical separation of the epidermis from the corium. J Invest Dermatol 18:377–379
Mackenzie IC, Squier CA (1975) Cytochemical identification of ATPase-positive langerhans cells in EDTA-separated sheets of mouse epidermis. Br J Dermatol 92:523–533
Juhlin L, Shelley WB (1977) New staining techniques for the Langerhans cell. Acta Derm Venereol 57:289–296
Nordlund JJ, Ackles A (1981) A method for quantifying Langerhans cells in epidermal sheets of human and murine skin. Tissue Antigens 17:217–225
Caughman SW, Sharrow SO, Shimada S, Stephany D, Mizuochi T, Rosenberg AS, Katz SI, Singer A (1986) Ia+ murine epidermal Langerhans cells are deficient in surface expression of the class I major histocompatibility complex. Proc Natl Acad Sci U S A 83:7438–7442
Itoh M, Yonemura S, Nagafuchi A, Tsukita SA, Tsukita SH (1991) A 220-kD undercoat-constitutive protein: its specific localization at cadherin-based cell-cell adhesion sites. J Cell Biol 115:1449–1462
Itoh M, Nagafuchi A, Yonemura S, Kitani-Yasuda T, Tsukita SA, Tsukita SH (1993) The 220-kD protein colocalizing with cadherins in non-epithelial cells is identical to ZO-1, a tight junction-associated protein in epithelial cells: cDNA cloning and immunoelectron microscopy.J Cell Biol 121:491–502
Acknowledgments
This work was supported by Grants-in-Aid for Scientific Research and the “Promotion of Environmental Improvement for Independence of Young Researchers” program with funding from the Ministry of Education, Culture, Sports, Science and Technology of Japan, and Health Labour Sciences Research Grants for Research on Allergic Diseases and Immunology from the Ministry of Health, Labour and Welfare of Japan.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2013 Springer Science+Business Media, LLC
About this protocol
Cite this protocol
Kubo, A., Nagao, K., Amagai, M. (2013). 3D Visualization of Epidermal Langerhans Cells. In: Has, C., Sitaru, C. (eds) Molecular Dermatology. Methods in Molecular Biology, vol 961. Humana Press, Totowa, NJ. https://doi.org/10.1007/978-1-62703-227-8_5
Download citation
DOI: https://doi.org/10.1007/978-1-62703-227-8_5
Published:
Publisher Name: Humana Press, Totowa, NJ
Print ISBN: 978-1-62703-226-1
Online ISBN: 978-1-62703-227-8
eBook Packages: Springer Protocols