Abstract
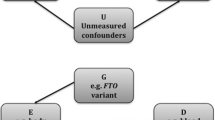
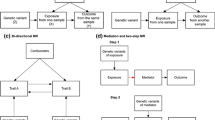
Mendelian randomization (MR) is becoming a popular approach to estimate the causal effect of an exposure on an outcome overcoming limitations of observational epidemiology. The advent of genome-wide association studies and the increasing accumulation of summarized data from large genetic consortia make MR a powerful technique. In this review, we give a primer in MR methodology, describe efficient MR designs and analytical strategies, and focus on methods and practical guidance for conducting an MR study using summary association data. We show that the analysis is straightforward utilizing either the MR-base platform or available packages in R. However, further research is required for the development of specialized methodology to assess MR assumptions.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Thomas DC, Conti DV (2004) Commentary: the concept of 'Mendelian Randomization'. Int J Epidemiol 33(1):21–25. https://doi.org/10.1093/ije/dyh048
Smith GD, Ebrahim S (2003) Mendelian randomization': can genetic epidemiology contribute to understanding environmental determinants of disease? Int J Epidemiol 32(1):1–22
Lawlor DA, Harbord RM, Sterne JA et al (2008) Mendelian randomization: using genes as instruments for making causal inferences in epidemiology. Stat Med 27(8):1133–1163. https://doi.org/10.1002/sim.3034
Bochud M, Rousson V (2010) Usefulness of Mendelian randomization in observational epidemiology. Int J Environ Res Public Health 7(3):711–728. https://doi.org/10.3390/ijerph7030711
Burgess S, Butterworth A, Malarstig A et al (2012) Use of Mendelian randomisation to assess potential benefit of clinical intervention. BMJ 345:e7325. https://doi.org/10.1136/bmj.e7325
Kivimaki M, Smith GD, Timpson NJ et al (2008) Lifetime body mass index and later atherosclerosis risk in young adults: examining causal links using Mendelian randomization in the cardiovascular risk in young finns study. Eur Heart J 29(20):2552–2560. https://doi.org/10.1093/eurheartj/ehn252
Voight BF, Peloso GM, Orho-Melander M et al (2012) Plasma HDL cholesterol and risk of myocardial infarction: a mendelian randomisation study. Lancet 380(9841):572–580. https://doi.org/10.1016/S0140-6736(12)60312-2
Carreras-Torres R, Haycock PC, Relton CL et al (2016) The causal relevance of body mass index in different histological types of lung cancer: a Mendelian randomization study. Sci Rep 6:31121. https://doi.org/10.1038/srep31121
Dixon SC, Nagle CM, Thrift AP et al (2016) Adult body mass index and risk of ovarian cancer by subtype: a Mendelian randomization study. Int J Epidemiol 45(3):884–895. https://doi.org/10.1093/ije/dyw158
Gao C, Patel CJ, Michailidou K et al (2016) Genetically predicted body mass index and breast cancer risk: mendelian randomization analyses of data from 145,000 women of European descent. PLoS Med 13(8):e1002105. https://doi.org/10.1371/journal.pmed.1002105
Guo Y, Warren Andersen S, Shu XO et al (2016) Genetically predicted body mass index and breast cancer risk: mendelian randomization analyses of data from 145,000 women of European descent. PLoS Med 13(8):e1002105. https://doi.org/10.1371/journal.pmed.1002105
Didelez V, Sheehan N (2007) Mendelian randomization as an instrumental variable approach to causal inference. Stat Methods Med Res 16(4):309–330. https://doi.org/10.1177/0962280206077743
Glymour MM, Tchetgen Tchetgen EJ, Robins JM (2012) Credible Mendelian randomization studies: approaches for evaluating the instrumental variable assumptions. Am J Epidemiol 175(4):332–339. https://doi.org/10.1093/aje/kwr323
Hernan MA, Robins JM (2006) Instruments for causal inference: an epidemiologist's dream? Epidemiology 17(4):360–372. https://doi.org/10.1097/01.ede.0000222409.00878.37
Lawlor DA (2016) Commentary: two-sample Mendelian randomization: opportunities and challenges. Int J Epidemiol 45(3):908–915. https://doi.org/10.1093/ije/dyw127
Burgess S, Scott RA, Timpson NJ et al (2015) Using published data in Mendelian randomization: a blueprint for efficient identification of causal risk factors. Eur J Epidemiol 30(7):543–552. https://doi.org/10.1007/s10654-015-0011-z
Burgess S, Small DS, Thompson SG (2015) A review of instrumental variable estimators for Mendelian randomization. Stat Methods Med Res. https://doi.org/10.1177/0962280215597579
Boef AG, Dekkers OM, le Cessie S (2015) Mendelian randomization studies: a review of the approaches used and the quality of reporting. Int J Epidemiol 44(2):496–511. https://doi.org/10.1093/ije/dyv071
Davies NM, Smith GD, Windmeijer F et al (2013) Issues in the reporting and conduct of instrumental variable studies: a systematic review. Epidemiology 24(3):363–369. https://doi.org/10.1097/EDE.0b013e31828abafb
Haycock PC, Burgess S, Wade KH et al (2016) Best (but oft-forgotten) practices: the design, analysis, and interpretation of Mendelian randomization studies. Am J Clin Nutr 103(4):965–978. https://doi.org/10.3945/ajcn.115.118216
Hemani G, Zheng J, Wade KH et al (2016) MR-base: a platform for systematic causal inference across the phenome using billions of genetic associations. bioRxivr. https://doi.org/10.1101/078972
Greenland S (2000) An introduction to instrumental variables for epidemiologists. Int J Epidemiol 29(4):722–729
Martens EP, Pestman WR, de Boer A et al (2006) Instrumental variables: application and limitations. Epidemiology 17(3):260–267. https://doi.org/10.1097/01.ede.0000215160.88317.cb
Wald A (1940) The fitting of straight lines if both variables are subject to error. Ann Math Stat 11(3):284–300
Fieller E (1954) Some problems in interval estimation. J R Stat Soc Series B Stat Methodology 16(2):175–185
Efron B, Tibshirani R (1993) An introduction to the bootstrap. Chapman & Hall/CRC Press, Boca Raton, Florida
Anderson T, Rubin H (1949) Estimators of the parameters of a single equation in a complete set of stochastic equations. Ann Mathe Stat 21(1):570–582
Moreira M (2003) A conditional likelihood ratio test for structural models. Econometrica 71(4):1027–1048
Ebrahim S, Davey Smith G (2008) Mendelian randomization: can genetic epidemiology help redress the failures of observational epidemiology? Hum Genet 123(1):15–33. https://doi.org/10.1007/s00439-007-0448-6
Angrist J, Pischke J (2009) Mostly harmless econometrics: an empiricist’s companion. Chapter 4: instrumental variables in action: sometimes you get what you need. Princeton University Press, Princeton, New Jersey
Nagelkerke N, Fidler V, Bernsen R et al (2000) Estimating treatment effects in randomized clinical trials in the presence of non-compliance. Stat Med 19(14):1849–1864
Davidson R, MacKinnon J (1993) Estimation and inference in econometrics. Chapter 18: simultaneous equation models. Oxford University Press, Oxford
Kleibergen F, Zivot E (2003) Bayesian and classical approaches to instrumental variable regression. J Econom 114:29–72
Foster E (1997) Instrumental variables for logistic regression: an illustration. Soc Sci Res 26(4):487–504
Johnston KM, Gustafson P, Levy AR et al (2008) Use of instrumental variables in the analysis of generalized linear models in the presence of unmeasured confounding with applications to epidemiological research. Stat Med 27(9):1539–1556. https://doi.org/10.1002/sim.3036
Hansen LP, Heaton J, Yaron A (1996) Finite-sample properties of some alternative GMM estimators. J Bus Econ Stat 14(3):262–280
Bowden J, Vansteelandt S (2011) Mendelian randomization analysis of case-control data using structural mean models. Stat Med 30(6):678–694. https://doi.org/10.1002/sim.4138
Greenland S, Lanes S, Jara M (2008) Estimating effects from randomized trials with discontinuations: the need for intent-to-treat design and G-estimation. Clin Trials 5(1):5–13. https://doi.org/10.1177/1740774507087703
Robins J (1986) A new approach to causal inference in mortality studies with a sustained exposure period–application to control of the healthy worker survivor effect. Math Model 7(9–12):1393–1512
Pierce BL, Burgess S (2013) Efficient design for Mendelian randomization studies: subsample and 2-sample instrumental variable estimators. Am J Epidemiol 178(7):1177–1184. https://doi.org/10.1093/aje/kwt084
Pierce BL, Ahsan H, Vanderweele TJ (2011) Power and instrument strength requirements for Mendelian randomization studies using multiple genetic variants. Int J Epidemiol 40(3):740–752. https://doi.org/10.1093/ije/dyq151
Welter D, MacArthur J, Morales J et al (2014) The NHGRI GWAS catalog, a curated resource of SNP-trait associations. Nucleic Acids Res 42(Database issue):D1001–D1006. https://doi.org/10.1093/nar/gkt1229
Burgess S, Butterworth A, Thompson SG (2013) Mendelian randomization analysis with multiple genetic variants using summarized data. Genet Epidemiol 37(7):658–665. https://doi.org/10.1002/gepi.21758
Johnson T (2011) Conditional and joint multiple-SNP analysis of GWAS summary statistics identifies additional variants influencing complex traits. Technical report, Queen Mary University of London
Thomas DC, Lawlor DA, Thompson JR (2007) Re: estimation of bias in nongenetic observational studies using "Mendelian triangulation" by Bautista et al. Ann Epidemiol 17(7):511–513. https://doi.org/10.1016/j.annepidem.2006.12.005
Burgess S, Thompson SG (2013) Use of allele scores as instrumental variables for Mendelian randomization. Int J Epidemiol 42(4):1134–1144. https://doi.org/10.1093/ije/dyt093
Burgess S, Dudbridge F, Thompson SG (2016) Combining information on multiple instrumental variables in Mendelian randomization: comparison of allele score and summarized data methods. Stat Med 35(11):1880–1906. https://doi.org/10.1002/sim.6835
Stock J, Wright J, Yogo M (2002) A survey of weak instruments and weak identification in generalized method of moments. J Bus Econ Stat 20(4):518–529
Staiger D, Stock J (1997) Instrumental variables regression with weak instruments. Econometrica 65(3):557–586
Burgess S, Granell R, Palmer TM et al (2014) Lack of identification in semiparametric instrumental variable models with binary outcomes. Am J Epidemiol 180(1):111–119. https://doi.org/10.1093/aje/kwu107
Burgess S, Thompson SG, CRP CHD Genetics Collaboration (2011) Avoiding bias from weak instruments in Mendelian randomization studies. Int J Epidemiol 40(3):755–764. https://doi.org/10.1093/ije/dyr036
Higgins JP, Thompson SG, Deeks JJ et al (2003) Measuring inconsistency in meta-analyses. BMJ 327(7414):557–560. https://doi.org/10.1136/bmj.327.7414.557
Bowden J, Del Greco MF, Minelli C et al (2016) Assessing the suitability of summary data for two-sample Mendelian randomization analyses using MR-egger regression: the role of the I2 statistic. Int J Epidemiol 45(6):1961–1974. https://doi.org/10.1093/ije/dyw220
Greco MF, Minelli C, Sheehan NA et al (2015) Detecting pleiotropy in Mendelian randomisation studies with summary data and a continuous outcome. Stat Med 34(21):2926–2940. https://doi.org/10.1002/sim.6522
Bowden J, Davey Smith G, Burgess S (2015) Mendelian randomization with invalid instruments: effect estimation and bias detection through egger regression. Int J Epidemiol 44(2):512–525. https://doi.org/10.1093/ije/dyv080
Brion MJ, Shakhbazov K, Visscher PM (2013) Calculating statistical power in Mendelian randomization studies. Int J Epidemiol 42(5):1497–1501. https://doi.org/10.1093/ije/dyt179
Cook JR, Stefanski LA (1994) Simulation-extrapolation estimation in parametric measurement error models. J Am Stat Assoc 89(428):1314–1328. https://doi.org/10.2307/2290994
Han C (2008) Detecting invalid instruments using L1-GMM. Econ Lett 101(3):285–287
Bowden J, Davey Smith G, Haycock PC et al (2016) Consistent estimation in mendelian randomization with some invalid instruments using a weighted median estimator. Genet Epidemiol 40(4):304–314. https://doi.org/10.1002/gepi.21965
Bowden J, Del Greco MF, Minelli C et al (2017) A framework for the investigation of pleiotropy in two-sample summary data Mendelian randomization. Stat Med. https://doi.org/10.1002/sim.7221
GTEx Consortium (2015) Human genomics. The genotype-tissue expression (GTEx) pilot analysis: multitissue gene regulation in humans. Science 348(6235):648–660. https://doi.org/10.1126/science.1262110
Gaunt TR, Shihab HA, Hemani G et al (2016) Systematic identification of genetic influences on methylation across the human life course. Genome Biol 17:61. https://doi.org/10.1186/s13059-016-0926-z
Kettunen J, Demirkan A, Wurtz P et al (2016) Genome-wide study for circulating metabolites identifies 62 loci and reveals novel systemic effects of LPA. Nat Commun 7:11122. https://doi.org/10.1038/ncomms11122
Deming Y, Xia J, Cai Y et al (2016) Genetic studies of plasma analytes identify novel potential biomarkers for several complex traits. Sci Rep 6:18092. https://doi.org/10.1038/srep18092
Locke AE, Kahali B, Berndt SI et al (2015) Genetic studies of body mass index yield new insights for obesity biology. Nature 518(7538):197–206. https://doi.org/10.1038/nature14177
Wang Y, McKay JD, Rafnar T et al (2014) Rare variants of large effect in BRCA2 and CHEK2 affect risk of lung cancer. Nat Genet 46(7):736–741. https://doi.org/10.1038/ng.3002
Acknowledgements
NLD was supported by the IKY scholarship programme, which is co-financed by the European Union (European Social Fund - ESF) and Greek national funds through the action entitled “Reinforcement of Postdoctoral Researchers” in the framework of the Operational Programme “Human Resources Development Program, Education and Lifelong Learning” of the National Strategic Reference Framework (NSRF) 2014 – 2020. KKT was supported by the World Cancer Research Fund International Regular Grant Programme (WCRF 2014/1180).
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2018 Springer Science+Business Media, LLC, part of Springer Nature
About this protocol
Cite this protocol
Dimou, N.L., Tsilidis, K.K. (2018). A Primer in Mendelian Randomization Methodology with a Focus on Utilizing Published Summary Association Data. In: Evangelou, E. (eds) Genetic Epidemiology. Methods in Molecular Biology, vol 1793. Humana Press, New York, NY. https://doi.org/10.1007/978-1-4939-7868-7_13
Download citation
DOI: https://doi.org/10.1007/978-1-4939-7868-7_13
Published:
Publisher Name: Humana Press, New York, NY
Print ISBN: 978-1-4939-7867-0
Online ISBN: 978-1-4939-7868-7
eBook Packages: Springer Protocols