Abstract
The coordinated regulatory interactions among fibroblast growth factor 23 (FGF23), klotho, parathyroid hormone (PTH), and vitamin D ensure homeostatic balance of phosphate in the human body. The endocrine actions of FGF23, in association with PTH and vitamin D, mobilize sodium/phosphate cotransporters to control intestinal and renal phosphate transport. However, the availability of adequate amount of klotho is essential for FGF23 to exert its phosphate lowering effects in the kidney. In the presence of klotho, FGF23 activates downstream signaling components to influence phosphate metabolism. Animal models have been used to convincingly demonstrate that FGF23 is unable to regulate systemic phosphate homeostasis in the absence of klotho. Several factors, including phosphate and vitamin D, can regulate FGF23 and klotho production and influence their functions. In various acquired and genetic human diseases, dysregulation of FGF23 and/or klotho is associated with vascular and skeletal anomalies due to altered phosphate turnover. In this chapter, we will summarize how the endocrine effects of bone-derived FGF23, in coordination with klotho, can regulate systemic phosphate homeostasis, and how an inadequate balance of these molecules can lead to disease conditions due to abnormal phosphate metabolism.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
FormalPara Key Points-
Fibroblast growth factor 23 (FGF23), parathyroid hormone (PTH), and vitamin D ensure homeostatic balance of phosphorus in the human body.
-
Klotho is a key cofactor that allows FGF23 to bind to its cognate receptor with high affinity and effect downstream signaling that regulates phosphorus and vitamin D metabolism.
-
Dysregulation of FGF23, PTH, and/or klotho is associated with vascular and skeletal anomalies due to altered phosphate turnover.
Introduction
The optimal balance of phosphate level is biologically important, as inorganic phosphorus performs many essential cellular functions within the body. Phosphate is a component of nucleic acids (DNA and RNA), and it is also an important component in the structure of phospholipids in cell membranes. Phosphate also plays roles in cell signaling (through phosphorylation), in energy metabolism (as ATP), and in bone mineralization (as hydroxyapatite). Recent studies have provided evidence of endocrine regulation of systemic phosphate homeostasis; such regulation of phosphate depends on a delicate balance among circulating factors like active form of vitamin D, parathyroid hormone (PTH), bone-derived fibroblast growth factor 23 (FGF23), and kidney-derived klotho. Dysregulation of these factors can induce phosphorus imbalances which can affect the functionality of almost every human system, eventually leading to an increase in morbidity and mortality.
In Vivo Phosphate Turnover
Renal function is essential to preserve physiologic water, electrolyte, and mineral ion balance. In most chronic renal diseases, impaired renal function perturbs the physiologic water, electrolyte, and mineral ion levels, including phosphate homeostasis. Phosphate is widely distributed in the body and is an important factor in bone formation. In addition, phosphate is also involved in cell signaling, energy metabolism, nucleic acid synthesis, and the maintenance of acid-base balance through affecting urinary buffering system.
The coordinated interactions of small intestine, bone, parathyroid gland, and kidney maintain physiologic phosphate balance; structural and functional impairments in any of these organs can lead to abnormal phosphate balance (Table 3.1) [3–6]. Dietary phosphate is usually absorbed from the intestine and taken up by the cells that need it, and the remaining amount is mostly excreted out of body through urine. Transepithelial phosphate transport in the intestine (by enterocytes) and in the kidney (by proximal epithelial cells) is primarily mediated by the sodium phosphate (Na/Pi) cotransporter family (Na/Pi-2a, Na/Pi-2b, and Na/Pi-2c) that are expressed in the apical membranes. More than 80 % of the filtrated phosphate in the kidney is reabsorbed in the proximal tubules, mostly with the help of Na/Pi-2a and Na/Pi-2c. Various endocrine factors, including PTH, active vitamin D metabolites, and FGF23 can directly or indirectly control Na/Pi activities to influence systemic phosphate balance (Fig. 3.1) [7–10].
FGF23 produced in the bone can suppress Na/Pi-2a and Na/Pi-2c cotransporters to increase the renal excretion of phosphate. Similarly, FGF23 can also suppress renal expression of 1α(OH)ase to reduce production of 1,25(OH)2D to decrease intestinal phosphate absorption, resulting in reduced serum levels of phosphate [1, 2]
Among these factors, PTH is one of the most potent regulators of phosphate metabolism. PTH can suppress the reabsorption of phosphate in the proximal tubules by reducing Na/Pi-2a and Na/Pi-2c activities. Such PTH-mediated suppression of Na/Pi-2a and Na/Pi-2c is achieved by internalization of Na/Pi proteins from the luminal side of the proximal tubular epithelial cells [11–13]. PTH can also mobilize phosphate from the bone into the bloodstream, possibly by enhancing osteoclastic bone resorption. Moreover, PTH can increase the production of 1,25- dihydroxyvitamin D3 [1,25(OH)2D] by inducing the renal expression of 1α-hydroxylase [1α(OH)ase] to influence intestinal phosphate absorption. In addition to PTH and vitamin D, numerous hormones can also affect renal phosphate handling. Growth hormone, insulin, and thyroid hormone can all increase phosphate reabsorption, while calcitonin, glucocorticoids, and atrial natriuretic factor can decrease phosphate reabsorption, primarily by influencing Na/Pi-2a activities [14, 15].
Cellular, intracellular, transcellular, and pericellular mineral ion transports are complex processes achieved by both active and passive translocation. Phosphate transport across renal proximal tubular epithelial cells is mostly driven by a high extracellular sodium gradient, which is thought to be maintained by the membrane-associated Na,K-ATPase. It has been claimed that the transmembrane protein klotho can influence Na,K-ATPase activity to increase the Na+ gradient and drive transepithelial calcium transport in the choroid plexus and kidney. Until very recently, changes in serum phosphate levels were thought to be a secondary process related to calcium transport and balance. A major breakthrough in understanding the active regulation of phosphate homeostasis was achieved by the identification of the novel phosphatonin FGF23 [16, 17].
Fibroblast Growth Factor 23
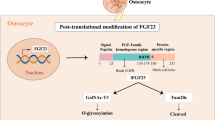
FGF23 is a ~30 kDa protein that is proteolytically processed to smaller N-terminal (~18 kDa) and C-terminal (~12 kDa) fragments. The receptor-binding domain of FGF23 is present in the N-terminus. FGF23 is able to suppress Na/Pi-2a and Na/Pi-2c cotransporters either directly or through influencing PTH activity to induce urinary phosphate excretion [18–24]. Transgenic mice overexpressing FGF23 have hypophosphatemia due to the suppression of the renal Na/Pi cotransporters, as well as reduced serum 1,25(OH)2D levels and skeletal mineral deposition defects in the form of rickets/osteomalacia [25–27]. Of relevance, FGF23 can also influence systemic vitamin D activity by suppressing the renal expression of 1-α(OH)ase to decrease the production of 1,25(OH)2D. In addition, FGF23 can reduce 1,25(OH)2D activity by increasing the synthesis of the catabolic enzyme 24-hydroxylase [28–31].
Vitamin D-resistant rickets/osteomalacia in patients with X-linked hypophosphatemia (XLH) is caused by inactivating mutations in the PHEX gene (a phosphate-regulating gene that is homologous to endopeptidases on the X-chromosome) that, in turn, increase serum levels of FGF23 [32–36]. In the case of autosomal-dominant hypophosphatemic rickets (ADHR), gain-of-function mutations of the FGF23 gene are associated with excessive urinary phosphate wasting, causing rickets in the bones [32, 37, 38]. Patients with ADHR have mutations in the FGF23 gene that are located within three nucleotides between residues 176 and 179 in the pro-protein convertase cleavage site, and thus prevent the proteolytic cleavage of the FGF23 protein. The net effect of such change is phosphate wasting in the affected patients due to enhanced FGF23 activity. In some patients with epidermal nevus syndrome (ENS), which is reported to be caused by activating mutations of FGFR3, increased serum levels of FGF23 are found to be associated with renal phosphate wasting [39, 40].
Similarly, increased production of FGF23 by tumor cells in patients with tumor-induced osteomalacia (TIO) can induce excessive renal phosphate wasting and mineralization defects in the bone [41–46]. These clinical symptoms can be reversed by surgical removal of the FGF23-producing tumor. A pathological role for FGF23 has also been suggested in McCune-Albright syndrome, in which FGF23 is believed to cause hypophosphatemia [47]. Furthermore, in some patients with osteoglophonic dysplasia (OGD), increased serum levels of FGF23 can cause hypophosphatemia; OGD is an autosomal-dominant disorder characterized by non-ossifying bone lesions with abnormal mineral ion balance, including hypophosphatemia. Heterozygous missense mutations in FGFR1 lead to constitutive receptor activation in OGD and induce disease pathology [48].
Recently, hypophosphatemia in patients with autosomal recessive hypophosphatemic rickets/osteomalacia (ARHR) has been attributed to high serum FGF23 levels [49–52]. It is worth mentioning that mutations in the dentin matrix protein-1 (DMP- 1) gene have been reported in patients with ARHR, but the mechanism by which mutation in DMP-1 can lead to increased FGF23 production is not yet clear. In a related experimental study, increased production of FGF23 was detected in Dmp-1 knockout mice; such increased levels of FGF23 is thought to induce hypophosphatemia in these mutant mice, as genetic deletion of fgf23 in Dmp-1 knockout mice resulted in hyperphosphatemia, a comparable phenotype as seen in FGF23 single knockout mice [52, 53].
In contrast to the diseases associated with increased production and bioactivity of FGF23, there are human diseases that can be caused by reduced FGF23 activity (Table 3.2). For instance, patients with familial tumoral calcinosis (FTC) usually develop hyperphosphatemia and ectopic calcification due to loss-of-function mutations in the FGF23 gene [54–59]. Similarly, mutations in the GALNT3 gene, which encodes the glycosyl transferase ppGaNTase-T3 (UDP-N-acetyl-a-D-galactosamine: polypeptide N-acetylgalactosaminyltransferase-3), have also been identified in patients with FTC. In these patients, serum levels of intact FGF23 are reduced, while levels of the processed C-terminal FGF23 fragment are increased, suggesting an accelerated proteolytic degeneration of full-length bioactive FGF23 protein. Similarly, recently developed GALNT3 knockout mice showed impaired secretion of intact FGF23, despite increased expression of FGF23 in the bone, indicating an important in vivo role of GALNT3 in the processing and secretion of FGF23 [60]. Together, these observations imply that mutations in the GALNT3 gene can impair O-glycosylation of the FGF23 protein in patients with FTC, thereby increasing the susceptibility of the FGF23 protein to proteolytic inactivation. Study of these human genetic disorders and knockout mice models that influence the functionality of FGF23 have substantially increased our understanding of how systemic phosphate homeostasis is regulated. However, the exact role and mechanisms by which FGF23 regulation is perturbed in acquired human diseases should be investigated further, particularly in patients with renal diseases.
FGF23 and Chronic Kidney Disease
Patients with advanced stages of chronic kidney diseases (CKD) have elevated serum levels of FGF23. Despite increased serum levels of FGF23, CKD patients develop hyperphosphatemia. It is not clear why the serum level of FGF23 is high in patients with CKD, but there are several possibilities, including decreased renal clearance of FGF23 and increased production of FGF23 to counteract hyperphosphatemia. This second possibility is supported by both human and experimental studies that have shown that a high dietary phosphorus load can increase serum levels of FGF23 [61]. Moreover, calcitriol therapy in patients with CKD may also contribute to increased serum levels of FGF23. Saito and colleagues have reported that both phosphorus and 1,25-dihydroxyvitamin D independently promote an increase in circulating FGF23 levels [62]. Patients with CKD tend to have a low levels of 1,25(OH)2D and secondary hyperparathyroidism. Whether increased levels of FGF23 can influence this dysregulation is a complex issue and deserves additional study. Since FGF23 can suppress vitamin D activity, the increased levels of FGF23 in patients with CKD may reduce vitamin D activity and eventually facilitate the development of compensatory secondary hyperparathyroidism.
The endocrine functions of PTH help in the maintenance of phosphate balance by promoting renal phosphate excretion. It may also reduce urinary calcium excretion and stimulate the renal production of active vitamin D metabolites. Nevertheless, even though serum PTH levels are high in patients with CKD, PTH fails to reduce serum phosphate levels in patients with this chronic illness. Increased production of PTH to counteract hyperphosphatemia could significantly contribute to the development of secondary hyperparathyroidism [63]. Of particular interest, elevated serum FGF23 levels are suggested to be an important predictor of secondary hyperparathyroidism in patients undergoing dialysis treatment [64].
Hyperphosphatemia is an important determinant of mortality in patients with CKD, irrespective of other associated biochemical changes. However, serum phosphate levels can be influenced by numerous factors including diet, the use of phosphate lowering drugs, or abnormal skeletal conditions. Serum phosphate levels, therefore, can at times be misleading in risk assessment, particularly when serum levels remain within the normal range. Recent studies have suggested that under normophosphatemic conditions, serum levels of FGF23 may be a better biomarker than serum phosphate levels for risk assessment in patients with CKD [19, 65].
A number of studies have pointed to an association between increased serum levels of FGF23 and increased mortality in patients with CKD, particularly in patients undergoing hemodialysis [66]. The cause of high mortality in CKD patients with higher serum levels of FGF23 is not clear, but recent studies have found a correlation between elevated serum FGF23 and an increased rate of left ventricular hypertrophy [67–70]. Although these association studies are suggestive, they do not provide enough mechanistic evidence to prove that FGF23 has a direct role in affecting cardiovascular structural components to influence cardiac functions and eventual mortality. The available (genetically altered) animal models may be able to show a direct effect of FGF23 on cardiovascular structure and function more convincingly. Klotho knockout mice have extremely high serum levels of FGF23 compared to control mice, and a shortened lifespan due to early sudden death. The sudden death in klotho knockout mice is linked to cardiac dysfunction of the sinoatrial node [71]. Determining whether high serum levels of FGF23 contribute to the cardiac dysfunction and early mortality of klotho knockout mice may help us understand the pathologic role of elevated serum levels of FGF23 in patients with CKD.
Klotho and Its Structure
Klotho is a type 1 membrane protein, with a single transmembrane domain near its C-terminus that is believed to anchor the protein to the membrane [72] (Fig. 3.2). Once the short transmembrane domain is removed, the remaining fragment (the “secreted form”) can be released into the circulatory system. The mouse klotho gene has 5 exons and 4 introns and is located on chromosome 13q12. The transcript of mouse klotho is about 5.2 kb. Interestingly, the promoter region lacks a TATA-box and contains four potential binding sites for Sp1-transcription factor. A splice site in the third exon of the klotho gene can be alternatively spliced to generate two transcripts encoding the transmembrane and secreted forms of the klotho protein. The full-length klotho (transmembrane form) transcript encodes a protein of 1014 amino acids with a molecular weight of 130 kDa. Alternative mRNA splicing generates a truncated klotho protein (the secreted form) that encodes a protein of 550 amino acids with a molecular weight of approximately 65–70 kDa [73–75]. The full-length mouse klotho cDNA and its protein have around 93 % and 80 % homology to those of rat and human, respectively. The transmembrane form of the mouse klotho protein possesses a putative signal sequence at its N-terminus, a putative transmembrane domain, and a short cytoplasmic domain at the C-terminus. The extracellular domain of the klotho protein consists of two internal repeats of about 550 amino acids (KL1 and KL2) that share sequence homology with beta-glucosidase. Between two internal repeats (KL1 and KL2), there is a short stretch of basic amino acids (Lys-Lys-Arg-Lys) that forms a possible site for proteolytic cleavage, similar to the polybasic proteolytic processing site. This short stretch of basic amino acids is present in the rat, human, and mouse klotho protein. The secreted form of mouse klotho only contains the N-terminal half of klotho, including its extracellular domain (KL1) [72].
Schematic diagram of the α-klotho protein structure, which is composed of 1014 amino acids and possesses a putative signal sequence (SS) at its N-terminus and a putative transmembrane domain (TM) with a short cytoplasmic domain (CD) at the C-terminus. The extracellular domain of the klotho protein consists of two internal repeats (KL1 and KL2) that share sequence homology with β-glucosidase (adapted from reference [1])
FGF23-Klotho Signaling Pathways
Klotho expression has been detected in the distal convoluted tubules of the kidney, the parathyroid gland, and the epithelium of the choroid plexus in the brain [72]. The klotho knockout mice exhibit increased renal expression of Na/Pi-2a and Na/Pi-2c protein with concomitant hyperphosphatemia and develop physical, biochemical, and morphological phenotypes identical to those of FGF23 knockout mice [76]. The identical phenotypes of these two separate knockout lines eventually led to the identification of klotho as an essential cofactor in FGF23 signaling pathways [76].
In general, most FGFs bind to FGF receptors on the cell surface and activate downstream signaling events to exert diverse biological functions. FGF23 is a member of the FGF19 subfamily, which also contains FGF19 and FGF21. FGF23 has been shown to bind to multiple FGF receptors, including FGFR1c, FGFR3c, and FGFR4 [77–80]. Further research has suggested that the klotho protein can bind to multiple FGF receptors, and that the klotho-FGF receptor complex binds to FGF23 with much higher affinity than either the FGF receptor or klotho alone. The binding of the klotho-FGF complex can then activate downstream signaling events, as demonstrated by the activation of early growth response element-1 (Egr-1) and the phosphorylation of FGF receptor substrate-2a, extracellular signal-regulated kinase (ERK), p38, Jun N-terminal kinase (JNK), and AKT [80, 81]. It is worth noting that these signaling phosphoproteins were detected only when cells were treated with both FGF23 and klotho together, and not in cells treated with FGF23 without klotho. These results, along with earlier observations, clearly suggest that the FGF23–FGF receptor interaction and subsequent signaling activities require klotho as a cofactor.
In response to elevated serum phosphate levels, FGF23 is produced in the bone and exerts endocrine effects on the kidney in coordination with klotho protein, which is mostly expressed in the distal tubular epithelial cells to promote renal phosphate excretion. The phosphate lowering action of FGF23 is partly mediated through the reduced expression of Na/Pi-2a and 1α(OH)ase in the proximal tubular epithelial cells. Despite the fact that klotho is mostly present in the distal tubular epithelial cells, how FGF23-mediated phosphate metabolism takes place in the proximal tubules is an intense area of research. In a recent study, presence of low level klotho has been reported in proximal tubules [82], and formed the basis for in-depth study of FGF23- klotho interactions in FGF23-mediated phosphate metabolism.
Klotho and Systemic FGF23 Function
Transgenic mice overexpressing human or mouse FGF23 develop hypophosphatemia due to severe urinary phosphate wasting, while FGF23 knockout mice develop hyperphosphatemia due to increased renal uptake of filtrated phosphate. A genetic restoration of the systemic actions of human FGF23 in FGF23 knockout mice reversed this hyperphosphatemia to hypophosphatemia and prevented associated complications, including ectopic calcification [83]. Recent studies have clearly demonstrated the in vivo importance of klotho in FGF23-mediated regulation of phosphate homeostasis. For instance, serum phosphate levels were significantly reduced following an injection of bioactive FGF23 in wild-type or FGF23−/− mice; since wild-type and FGF23−/− mice both have endogenous klotho, the exogenous FGF23 is able to influence systemic phosphate homeostasis. In contrast, the injection of bioactive FGF23 protein into either klotho−/− mice or FGF23−/− /klotho−/− double knockout mice does not produce any obvious changes in the serum levels of phosphate [76], implying that klotho is essential for the FGF23-mediated regulation of phosphate homeostasis. This essential in vivo role of klotho has recently been demonstrated further in a genetically engineered hypophosphatemic (Hyp) mouse model [84].
Hyp mice possess a mutation that inactivates PHEX, a phosphate-regulating gene that is homologous to the endopeptidases of the X-chromosome. This mutation is associated with severe hypophosphatemia due to excessive urinary phosphate wasting caused by increased serum accumulation of FGF23. In vivo genetic manipulation studies have shown that the inactivation of klotho in Hyp mice resulted in hyperphosphatemia, not hypophosphatemia, even though Hyp/klotho−/− double mutant mice have significantly elevated serum levels of FGF23 [84]. The opposing phenotypes of Hyp and Hyp/klotho−/− mice suggest that the disruption of klotho-mediated pathways abrogates the hypophosphatemic phenotype normally caused by the increased serum levels of FGF23. Furthermore, genetic inactivation of klotho in FGF23 transgenic mice resulted in a phenotype consistent with klotho deficiency, again emphasizing the in vivo importance of klotho in FGF23 function. Similarly, a homozygous loss-of-function mutation in the Klotho gene causes tumoral calcinosis, severe hyperphosphatemia, and ectopic calcification despite high serum levels of FGF23 in the affected patient [85]. Together, these human and mouse genetic studies provide compelling evidence that klotho is essential in the FGF23-mediated regulation of systemic phosphate homeostasis in vivo.
Nevertheless, under pathological conditions where the concentration of FGF23 is extremely high, FGF23 may exert nonspecific effects without klotho, as FGF23 can bind to FGF receptors with low affinity in the absence of klotho [80]. Several in vitro studies also support the possibility of such off-target responses. Additional studies will explain whether effects of FGF23 on klotho nonexpressing or low expressing tissues, including bone, blood vessels are off-target responses or not. For example, FGF23 was shown to exhibit weak proliferative effects on a murine bone marrow-derived pro-B cell line that overexpresses FGFRs but does not express klotho. Experimental explanation is needed to know if extremely high serum levels of FGF23 can lead to ectopic activation of FGF receptors and thus induce cardiac morbidity in patients with CKD. In this scenario, patients with CKD might benefit from therapy to lower FGF23. However, a better understanding of the exact role of elevated serum levels of FGF23 in CKD patients is needed before any therapeutic strategy can be proposed. For example, it is not clear whether increased FGF23 levels are a protective response (in early stages) or a detrimental side effect (in later stages) in CKD patients. Thus, any therapeutic designs will need to be assessed carefully. Moreover, vitamin D deficiency has been linked to increased mortality in advanced CKD patients; since FGF23 can suppress the production of active vitamin D metabolites, it is possible that any detrimental effect of FGF23 on the mortality of CKD patients may be influenced by reduced vitamin D activity.
As discussed above, the generation of Hyp/klotho−/− double mutant mice has clearly demonstrated that the FGF23-mediated hypophosphatemia in Hyp mice is klotho dependent. These genetic studies have provided in vivo evidence suggesting that klotho may be a potential therapeutic tool to manipulate FGF23 function, and that direct manipulation of klotho may prove a novel therapeutic strategy for FGF23-related hypophosphatemic diseases. The clinical application of a controlled reduction of FGF23 might be of therapeutic benefit for patients with excessive urinary phosphate wasting diseases, including ADHR, ARHR, and XLH. The current treatments for these genetic hypophosphatemic diseases are mostly palliative, such as oral phosphate replacement. Also, the prolonged use of these therapies can cause complications, notably secondary hyperparathyroidism. Finally, in contrast to anti-FGF23 therapy, providing exogenous bioactive FGF23 protein might help restore phosphate balance and delay associated complications, such as the ectopic calcifications in patients with FTC that are usually caused by reduced FGF23 activity. In a recent study, exogenous FGF23 treatment was shown to delay the progression of experimental nephritis-induced renal failure. However, this treatment also aggravated renal osteodystrophy due to reduced levels of 1,25(OH)2D, demonstrating one potential limitation of FGF23 therapy [86]. Renal osteodystrophy is often described as a CKD-mineral and bone disorder (CKD-MBD). Of particular interest, 1,25(OH)2D can exert opposing effects on serum phosphate levels: 1,25(OH)2D can induce both FGF23 and klotho to increase urinary excretion of phosphate and lower serum phosphate levels, but can also facilitate increased intestinal absorption of phosphate to increase serum phosphate levels.
Concluding Remarks
The regulation of systemic phosphate homeostasis appears to be strictly controlled by a limited number of factors, as demonstrated by the opposing phenotypes of FGF23 transgenic and knockout mice, their similarities with klotho-mutant mice, and—more importantly, the corresponding clinical phenotype in hereditary diseases caused by FGF23 or klotho mutations in humans (Table 3.1) [1, 2, 21, 27, 32, 76, 87–92]. The overlapping phenotypes and lack of redundancy suggest that a limited number of essential factors form the biological network that actively regulates phosphate homeostasis. Our understanding of the essential in vivo endocrine role of FGF23 in maintaining systemic phosphate homeostasis has laid the foundation for future work to determine the therapeutic benefit of manipulating the FGF23-klotho network in patients with excessive urinary phosphate wasting diseases. In addition, serum FGF23 measurements may have both diagnostic and prognostic significance in these patients, and may be used to determine the underlying causes of diseases associated with abnormal mineral ion metabolism; for instance, serum FGF23 levels can aid in the diagnosis of tumor-induced osteomalacia (TIO). Studies suggest that the pretreatment serum level of FGF23 can be a good predictor of vitamin D therapy efficacy in dialysis patients, and is also believed to be a useful predictor for the development of refractory hyperparathyroidism [63].
Conclusions
Recent studies have provided compelling evidence of the in vivo importance of klotho in FGF23-mediated regulation of systemic phosphate homeostasis. Translating this research to new therapies for patients suffering from the complications of abnormal mineral ion metabolism will be a challenging, and yet clinically rewarding effort.
References
Razzaque MS. The FGF23-Klotho axis: endocrine regulation of phosphate homeostasis. Nat Rev Endocrinol. 2009;5:611–9.
Brown RB, Razzaque MS. Phosphate toxicity: a stealth biochemical stress factor? Med Mol Morphol. 2016;49:1–4.
Ohnishi M, Razzaque MS. Osteo-renal cross-talk and phosphate metabolism by the FGF23-Klotho system. Contrib Nephrol. 2013;180:1–13.
Sabbagh Y, Giral H, Caldas Y, Levi M, Schiavi SC. Intestinal phosphate transport. Adv Chronic Kidney Dis. 2011;18:85–90.
Razzaque MS. FGF23-mediated regulation of systemic phosphate homeostasis: is Klotho an essential player? Am J Physiol Renal Physiol. 2009;296:F470–6.
Tenenhouse HS. Phosphate transport: molecular basis, regulation and pathophysiology. J Steroid Biochem Mol Biol. 2007;103:572–7.
Kaneko I, Segawa H, Furutani J, Kuwahara S, Aranami F, Hanabusa E, Tominaga R, Giral H, Caldas Y, Levi M, Kato S, Miyamoto K. Hypophosphatemia in vitamin D receptor null mice: effect of rescue diet on the developmental changes in renal Na+−dependent phosphate cotransporters. Pflugers Arch. 2011;461:77–90.
Tomoe Y, Segawa H, Shiozawa K, Kaneko I, Tominaga R, Hanabusa E, Aranami F, Furutani J, Kuwahara S, Tatsumi S, Matsumoto M, Ito M, Miyamoto K. Phosphaturic action of fibroblast growth factor 23 in Npt2 null mice. Am J Physiol Renal Physiol. 2010;298:F1341–50.
Cheng CY, Kuro-o M, Razzaque MS. Molecular regulation of phosphate metabolism by fibroblast growth factor-23-klotho system. Adv Chronic Kidney Dis. 2011;18:91–7.
Ito M, Sakai Y, Furumoto M, Segawa H, Haito S, Yamanaka S, Nakamura R, Kuwahata M, Miyamoto K. Vitamin D and phosphate regulate fibroblast growth factor-23 in K-562 cells. Am J Physiol Endocrinol Metab. 2005;288:E1101–9.
Elhalel MD, Wald H, Rubinger D, Gal-Moscovici A, Inoue M, Levi M, Popovtzer MM. Regulation of NaPi-IIa mRNA and transporter protein in chronic renal failure: role of parathyroid hormone (PTH) and dietary phosphate (Pi). Pflugers Arch. 2004;449:265–70.
Biber J, Hernando N, Forster I, Murer H. Regulation of phosphate transport in proximal tubules. Pflugers Arch. 2009;458:39–52.
Pfister MF, Lederer E, Forgo J, Ziegler U, Lotscher M, Quabius ES, Biber J, Murer H. Parathyroid hormone-dependent degradation of type II Na+/Pi cotransporters. J Biol Chem. 1997;272:20125–30.
Gupta N, Tarif SR, Seikaly M, Baum M. Role of glucocorticoids in the maturation of the rat renal Na+/H+ antiporter (NHE3). Kidney Int. 2001;60:173–81.
Berner YN, Shike M. Consequences of phosphate imbalance. Annu Rev Nutr. 1988;8:121–48.
Imura A, Tsuji Y, Murata M, Maeda R, Kubota K, Iwano A, Obuse C, Togashi K, Tominaga M, Kita N, Tomiyama K, Iijima J, Nabeshima Y, Fujioka M, Asato R, Tanaka S, Kojima K, Ito J, Nozaki K, Hashimoto N, Ito T, Nishio T, Uchiyama T, Fujimori T. alpha-Klotho as a regulator of calcium homeostasis. Science. 2007;316:1615–8.
Razzaque MS. Klotho and Na+, K+−ATPase activity: solving the calcium metabolism dilemma? Nephrol Dial Transplant. 2008;23:459–61.
Olauson H, Larsson TE. FGF23 and Klotho in chronic kidney disease. Curr Opin Nephrol Hypertens. 2013;22:397–404.
Gutierrez OM. Fibroblast growth factor 23, Klotho, and disordered mineral metabolism in chronic kidney disease: unraveling the intricate tapestry of events and implications for therapy. J Ren Nutr. 2013;23:250–4.
Stubbs J, Liu S, Quarles LD. Role of fibroblast growth factor 23 in phosphate homeostasis and pathogenesis of disordered mineral metabolism in chronic kidney disease. Semin Dial. 2007;20:302–8.
Lanske B, Razzaque MS. Mineral metabolism and aging: the FGF-23 enigma. Curr Opin Nephrol Hypertens. 2007;16(4):311–8.
Larsson T, Yu X, Davis SI, Draman MS, Mooney SD, Cullen MJ, White KE. A novel recessive mutation in fibroblast growth factor-23 causes familial tumoral calcinosis. J Clin Endocrinol Metab. 2005;90:2424–7.
Razzaque MS. Osteo-renal regulation of systemic phosphate metabolism. IUBMB Life. 2011;63:240–7.
Razzaque MS. Therapeutic potential of klotho-FGF23 fusion polypeptides: WO2009095372. Expert Opin Ther Pat. 2010;20:981–5.
Larsson T, Marsell R, Schipani E, Ohlsson C, Ljunggren O, Tenenhouse HS, Juppner H, Jonsson KB. Transgenic mice expressing fibroblast growth factor 23 under the control of the alpha1(I) collagen promoter exhibit growth retardation, osteomalacia, and disturbed phosphate homeostasis. Endocrinology. 2004;145:3087–94.
Shimada T, Urakawa I, Yamazaki Y, Hasegawa H, Hino R, Yoneya T, Takeuchi Y, Fujita T, Fukumoto S, Yamashita T. FGF-23 transgenic mice demonstrate hypophosphatemic rickets with reduced expression of sodium phosphate cotransporter type IIa. Biochem Biophys Res Commun. 2004;314:409–14.
Bai X, Miao D, Li J, Goltzman D, Karaplis AC. Transgenic mice overexpressing human fibroblast growth factor 23 (R176Q) delineate a putative role for parathyroid hormone in renal phosphate wasting disorders. Endocrinology. 2004;145:5269–79.
Fish RS, Cunningham J. FGF-23 and vitamin D: don’t shoot the messenger? Nephrol Dial Transplant. 2012;27:2137–9.
Ohnishi M, Nakatani T, Lanske B, Razzaque MS. Reversal of mineral ion homeostasis and soft-tissue calcification of klotho knockout mice by deletion of vitamin D 1alpha-hydroxylase. Kidney Int. 2009;75:1166–72.
Razzaque MS. The dualistic role of vitamin D in vascular calcifications. Kidney Int. 2011;79:708–14.
Shimada T, Kakitani M, Yamazaki Y, Hasegawa H, Takeuchi Y, Fujita T, Fukumoto S, Tomizuka K, Yamashita T. Targeted ablation of Fgf23 demonstrates an essential physiological role of FGF23 in phosphate and vitamin D metabolism. J Clin Invest. 2004;113:561–8.
ADHR_Consortium. Autosomal dominant hypophosphataemic rickets is associated with mutations in FGF23. The ADHR Consortium. Nat Genet. 2000;26:345–8.
Drezner MK. PHEX gene and hypophosphatemia. Kidney Int. 2000;57:9–18.
Quarles LD. FGF23, PHEX, and MEPE regulation of phosphate homeostasis and skeletal mineralization. Am J Physiol Endocrinol Metab. 2003;285:E1–9.
Roetzer KM, Varga F, Zwettler E, Nawrot-Wawrzyniak K, Haller J, Forster E, Klaushofer K. Novel PHEX mutation associated with hypophosphatemic rickets. Nephron Physiol. 2007;106:p8–12.
Kinoshita Y, Saito T, Shimizu Y, Hori M, Taguchi M, Igarashi T, Fukumoto S, Fujita T. Mutational analysis of patients with FGF23-related hypophosphatemic rickets. Eur J Endocrinol. 2012;167:165–72.
White KE, Carn G, Lorenz-Depiereux B, Benet-Pages A, Strom TM, Econs MJ. Autosomal-dominant hypophosphatemic rickets (ADHR) mutations stabilize FGF-23. Kidney Int. 2001;60:2079–86.
Imel EA, Hui SL, Econs MJ. FGF23 concentrations vary with disease status in autosomal dominant hypophosphatemic rickets. J Bone Miner Res. 2007;22:520–6.
Heike CL, Cunningham ML, Steiner RD, Wenkert D, Hornung RL, Gruss JS, Gannon FH, McAlister WH, Mumm S, Whyte MP. Skeletal changes in epidermal nevus syndrome: does focal bone disease harbor clues concerning pathogenesis? Am J Med Genet A. 2005;139:67–77.
Moreira AI, Ferreira G, Santos M, Baptista A, Ferreira EO. Epidermal nevus syndrome associated with hypophosphatemic rickets. Dermatol Online J. 2010;16:14.
Kumar R. Tumor-induced osteomalacia and the regulation of phosphate homeostasis. Bone. 2000;27:333–8.
Zimering MB, Caldarella FA, White KE, Econs MJ. Persistent tumor-induced osteomalacia confirmed by elevated postoperative levels of serum fibroblast growth factor-23 and 5-year follow-up of bone density changes. Endocr Pract. 2005;11:108–14.
Robertson A, Mansberg R, Mansberg V, Van der Wall H, Hooper M. Tumor-induced osteomalacia: a case of diagnostic dilemma. Clin Nucl Med. 2007;32:631–4.
van Boekel G, Ruinemans-Koerts J, Joosten F, Dijkhuizen P, van Sorge A, de Boer H. Tumor producing fibroblast growth factor 23 localized by two-staged venous sampling. Eur J Endocrinol. 2008;158:431–7.
Farrow EG, White KE. Tumor-induced osteomalacia. Expert Rev Endocrinol Metab. 2009;4:435–42.
Kobayashi K, Nakao K, Kawai K, Ito K, Hukumoto S, Asakage T, Oota S, Motoi R. Tumor-induced osteomalacia originating from the temporal bone: a case report. Head Neck. 2011;33:1072–5.
Yamamoto T, Imanishi Y, Kinoshita E, Nakagomi Y, Shimizu N, Miyauchi A, Satomura K, Koshiyama H, Inaba M, Nishizawa Y, Juppner H, Ozono K. The role of fibroblast growth factor 23 for hypophosphatemia and abnormal regulation of vitamin D metabolism in patients with McCune-Albright syndrome. J Bone Miner Metab. 2005;23:231–7.
White KE, Cabral JM, Davis SI, Fishburn T, Evans WE, Ichikawa S, Fields J, Yu X, Shaw NJ, McLellan NJ, McKeown C, Fitzpatrick D, Yu K, Ornitz DM, Econs MJ. Mutations that cause osteoglophonic dysplasia define novel roles for FGFR1 in bone elongation. Am J Hum Genet. 2005;76:361–7.
Levy-Litan V, Hershkovitz E, Avizov L, Leventhal N, Bercovich D, Chalifa-Caspi V, Manor E, Buriakovsky S, Hadad Y, Goding J, Parvari R. Autosomal-recessive hypophosphatemic rickets is associated with an inactivation mutation in the ENPP1 gene. Am J Hum Genet. 2010;86:273–8.
Grondel IM, van der Deure J, Zanen AL, Dogger M, van den Heuvel LP. A familial disorder with low bone density and renal phosphate wasting. Eur J Intern Med. 2009;20:503–8.
Saito T, Nishii Y, Yasuda T, Ito N, Suzuki H, Igarashi T, Fukumoto S, Fujita T. Familial hypophosphatemic rickets caused by a large deletion in PHEX gene. Eur J Endocrinol. 2009;161:647–51.
Jiang B, Cao Z, Lu Y, Janik C, Lauziere S, Xie Y, Poliard A, Qin C, Ward LM, Feng JQ. DMP1 C-terminal mutant mice recapture the human ARHR tooth phenotype. J Bone Miner Res. 2010;25:2155–64.
Liu S, Zhou J, Tang W, Menard R, Feng JQ, Quarles LD. Pathogenic role of Fgf23 in Dmp1-null mice. Am J Physiol Endocrinol Metab. 2008;295:E254–61.
Topaz O, Shurman DL, Bergman R, Indelman M, Ratajczak P, Mizrachi M, Khamaysi Z, Behar D, Petronius D, Friedman V, Zelikovic I, Raimer S, Metzker A, Richard G, Sprecher E. Mutations in GALNT3, encoding a protein involved in O-linked glycosylation, cause familial tumoral calcinosis. Nat Genet. 2004;36:579–81.
Benet-Pages A, Orlik P, Strom TM, Lorenz-Depiereux B. An FGF23 missense mutation causes familial tumoral calcinosis with hyperphosphatemia. Hum Mol Genet. 2005;14:385–90.
Barbieri AM, Filopanti M, Bua G, Beck-Peccoz P. Two novel nonsense mutations in GALNT3 gene are responsible for familial tumoral calcinosis. J Hum Genet. 2007;52:464–8.
Chefetz I, Sprecher E. Familial tumoral calcinosis and the role of O-glycosylation in the maintenance of phosphate homeostasis. Biochim Biophys Acta. 2008;1792(9):847–52.
Bergwitz C, Banerjee S, Abu-Zahra H, Kaji H, Miyauchi A, Sugimoto T, Juppner H. Defective O-glycosylation due to a novel homozygous S129P mutation is associated with lack of fibroblast growth factor 23 secretion and tumoral calcinosis. J Clin Endocrinol Metab. 2009;94:4267–74.
Yancovitch A, Hershkovitz D, Indelman M, Galloway P, Whiteford M, Sprecher E, Kilic E. Novel mutations in GALNT3 causing hyperphosphatemic familial tumoral calcinosis. J Bone Miner Metab. 2011;29(5):621–5.
Ichikawa S, Sorenson AH, Austin AM, Mackenzie DS, Fritz TA, Moh A, Hui SL, Econs MJ. Ablation of the Galnt3 gene leads to low-circulating intact fibroblast growth factor 23 (Fgf23) concentrations and hyperphosphatemia despite increased Fgf23 expression. Endocrinology. 2009;150:2543–50.
Nishida Y, Taketani Y, Yamanaka-Okumura H, Imamura F, Taniguchi A, Sato T, Shuto E, Nashiki K, Arai H, Yamamoto H, Takeda E. Acute effect of oral phosphate loading on serum fibroblast growth factor 23 levels in healthy men. Kidney Int. 2006;70:2141–7.
Saito H, Kusano K, Kinosaki M, Ito H, Hirata M, Segawa H, Miyamoto K, Fukushima N. Human fibroblast growth factor-23 mutants suppress Na+−dependent phosphate co-transport activity and 1alpha,25-dihydroxyvitamin D3 production. J Biol Chem. 2003;278:2206–11.
Koizumi M, Komaba H, Fukagawa M. Parathyroid function in chronic kidney disease: role of FGF23-Klotho axis. Contrib Nephrol. 2013;180:110–23.
Komaba H, Fukagawa M. FGF23-parathyroid interaction: implications in chronic kidney disease. Kidney Int. 2010;77:292–8.
Gutierrez OM. Increased serum phosphate and adverse clinical outcomes: unraveling mechanisms of disease. Curr Opin Nephrol Hypertens. 2011;20(3):224–8.
Gutierrez OM, Mannstadt M, Isakova T, Rauh-Hain JA, Tamez H, Shah A, Smith K, Lee H, Thadhani R, Juppner H, Wolf M. Fibroblast growth factor 23 and mortality among patients undergoing hemodialysis. N Engl J Med. 2008;359:584–92.
Gutierrez OM, Januzzi JL, Isakova T, Laliberte K, Smith K, Collerone G, Sarwar A, Hoffmann U, Coglianese E, Christenson R, Wang TJ, deFilippi C, Wolf M. Fibroblast growth factor 23 and left ventricular hypertrophy in chronic kidney disease. Circulation. 2009;119:2545–52.
Touchberry CD, Green TM, Tchikrizov V, Mannix JE, Mao TF, Carney BW, Girgis M, Vincent RJ, Wetmore LA, Dawn B, Bonewald LF, Stubbs JR, Wacker MJ. FGF23 is a novel regulator of intracellular calcium and cardiac contractility in addition to cardiac hypertrophy. Am J Physiol Endocrinol Metab. 2013;304:E863–73.
Razzaque MS. Does FGF23 toxicity influence the outcome of chronic kidney disease? Nephrol Dial Transplant. 2009;24:4–7.
Arnlov J, Carlsson AC, Sundstrom J, Ingelsson E, Larsson A, Lind L, Larsson TE. Serum FGF23 and risk of cardiovascular events in relation to mineral metabolism and cardiovascular pathology. Clin J Am Soc Nephrol. 2013;8:781–6.
Takeshita K, Fujimori T, Kurotaki Y, Honjo H, Tsujikawa H, Yasui K, Lee JK, Kamiya K, Kitaichi K, Yamamoto K, Ito M, Kondo T, Iino S, Inden Y, Hirai M, Murohara T, Kodama I, Nabeshima Y. Sinoatrial node dysfunction and early unexpected death of mice with a defect of klotho gene expression. Circulation. 2004;109:1776–82.
Maeda R, Imura A, Nabeshima Y. Complex regulation and diverse functions of alpha-klotho. Contrib Nephrol. 2013;180:25–46.
Matsumura Y, Aizawa H, Shiraki-Iida T, Nagai R, Kuro-o M, Nabeshima Y. Identification of the human klotho gene and its two transcripts encoding membrane and secreted klotho protein. Biochem Biophys Res Commun. 1998;242:626–30.
Shiraki-Iida T, Aizawa H, Matsumura Y, Sekine S, Iida A, Anazawa H, Nagai R, Kuro-o M, Nabeshima Y. Structure of the mouse klotho gene and its two transcripts encoding membrane and secreted protein. FEBS Lett. 1998;424:6–10.
Ohyama Y, Kurabayashi M, Masuda H, Nakamura T, Aihara Y, Kaname T, Suga T, Arai M, Aizawa H, Matsumura Y, Kuro-o M, Nabeshima Y, Nagail R. Molecular cloning of rat klotho cDNA: markedly decreased expression of klotho by acute inflammatory stress. Biochem Biophys Res Commun. 1998;251:920–5.
Nakatani T, Sarraj B, Ohnishi M, Densmore MJ, Taguchi T, Goetz R, Mohammadi M, Lanske B, Razzaque MS. In vivo genetic evidence for klotho-dependent, fibroblast growth factor 23 (Fgf23) -mediated regulation of systemic phosphate homeostasis. FASEB J. 2009;23:433–41.
Eswarakumar VP, Lax I, Schlessinger J. Cellular signaling by fibroblast growth factor receptors. Cytokine Growth Factor Rev. 2005;16:139–49.
Mohammadi M, Olsen SK, Ibrahimi OA. Structural basis for fibroblast growth factor receptor activation. Cytokine Growth Factor Rev. 2005;16:107–37.
Goetz R, Nakada Y, Hu MC, Kurosu H, Wang L, Nakatani T, Shi M, Eliseenkova AV, Razzaque MS, Moe OW, Kuro-o M, Mohammadi M. Isolated C-terminal tail of FGF23 alleviates hypophosphatemia by inhibiting FGF23-FGFR-Klotho complex formation. Proc Natl Acad Sci U S A. 2010;107:407–12.
Urakawa I, Yamazaki Y, Shimada T, Iijima K, Hasegawa H, Okawa K, Fujita T, Fukumoto S, Yamashita T. Klotho converts canonical FGF receptor into a specific receptor for FGF23. Nature. 2006;444:770–4.
Kurosu H, Ogawa Y, Miyoshi M, Yamamoto M, Nandi A, Rosenblatt KP, Baum MG, Schiavi S, Hu MC, Moe OW, Kuro-o M. Regulation of fibroblast growth factor-23 signaling by klotho. J Biol Chem. 2006;281:6120–3.
Hu MC, Shi M, Zhang J, Pastor J, Nakatani T, Lanske B, Razzaque MS, Rosenblatt KP, Baum MG, Kuro-o M, Moe OW. Klotho: a novel phosphaturic substance acting as an autocrine enzyme in the renal proximal tubule. FASEB J. 2010;24:3438–50.
DeLuca S, Sitara D, Kang K, Marsell R, Jonsson K, Taguchi T, Erben RG, Razzaque MS, Lanske B. Amelioration of the premature ageing-like features of Fgf-23 knockout mice by genetically restoring the systemic actions of FGF-23. J Pathol. 2008;216:345–55.
Nakatani T, Ohnishi M, Razzaque MS. Inactivation of klotho function induces hyperphosphatemia even in presence of high serum fibroblast growth factor 23 levels in a genetically engineered hypophosphatemic (Hyp) mouse model. FASEB J. 2009;23:3702–11.
Ichikawa S, Imel EA, Kreiter ML, Yu X, Mackenzie DS, Sorenson AH, Goetz R, Mohammadi M, White KE, Econs MJ. A homozygous missense mutation in human KLOTHO causes severe tumoral calcinosis. J Clin Invest. 2007;117:2684–91.
Kusano K, Saito H, Segawa H, Fukushima N, Miyamoto K. Mutant FGF23 prevents the progression of chronic kidney disease but aggravates renal osteodystrophy in uremic rats. J Nutr Sci Vitaminol (Tokyo). 2009;55:99–105.
Razzaque MS, Lanske B. Hypervitaminosis D and premature aging: lessons learned from Fgf23 and Klotho mutant mice. Trends Mol Med. 2006;12:298–305.
Ohnishi M, Nakatani T, Lanske B, Razzaque MS. In vivo genetic evidence for suppressing vascular and soft-tissue calcification through the reduction of serum phosphate levels, even in the presence of high serum calcium and 1,25-dihydroxyvitamin d levels. Circ Cardiovasc Genet. 2009;2:583–90.
Masi L, Gozzini A, Franchi A, Campanacci D, Amedei A, Falchetti A, Franceschelli F, Marcucci G, Tanini A, Capanna R, Brandi ML. A novel recessive mutation of fibroblast growth factor-23 in tumoral calcinosis. J Bone Joint Surg Am. 2009;91:1190–8.
Osuka S, Razzaque MS. Can features of phosphate toxicity appear in normophosphatemia? J Bone Miner Metab. 2012;30:10–8.
Razzaque MS. Phosphate toxicity: new insights into an old problem. Clin Sci (Lond). 2011;120:91–7.
Lammoglia JJ, Mericq V. Familial tumoral calcinosis caused by a novel FGF23 mutation: response to induction of tubular renal acidosis with acetazolamide and the non-calcium phosphate binder sevelamer. Horm Res. 2009;71:178–84.
Acknowledgments
The author thanks Razzaque lab members at Harvard School of Dental Medicine, Boston, including Drs. M. Ohnishi, J. Akiyoshi, S. Osuka, S. Kato, Y. Hong, and K. Turkistani for their scientific contributions through different completed projects. Part of this book chapter is based on earlier published review articles from the same group [1–3, 90, 91].
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2017 Springer Science+Business Media New York
About this chapter
Cite this chapter
Rafi, S.K., Razzaque, M.S. (2017). Hormonal Regulation of Phosphorus Homeostasis: Parathyroid Hormone, Fibroblast Growth Factor 23, and Klotho. In: Gutiérrez, O., Kalantar-Zadeh, K., Mehrotra, R. (eds) Clinical Aspects of Natural and Added Phosphorus in Foods. Nutrition and Health. Springer, New York, NY. https://doi.org/10.1007/978-1-4939-6566-3_3
Download citation
DOI: https://doi.org/10.1007/978-1-4939-6566-3_3
Published:
Publisher Name: Springer, New York, NY
Print ISBN: 978-1-4939-6564-9
Online ISBN: 978-1-4939-6566-3
eBook Packages: MedicineMedicine (R0)