Abstract
Vaccine approaches for cancer differ from traditional vaccine approaches for infectious disease in tending to focus on clearing active disease rather than preventing disease. In this review, we provide a brief overview of different types of vaccines and adjuvants that have been investigated for the purpose of controlling cancer burdens in patients, some of which are approved for clinical use or in late-stage clinical trials, such as the personalized dendritic cell vaccine sipuleucel-T (Provenge) and the recombinant viral prostate cancer vaccine PSA-TRICOM (Prostvac-VF). Vaccines against human viruses implicated in the development and progression of certain cancers, such as human papillomavirus in cervical cancer, are not considered here. Cancers express “altered self” antigens that tend to induce weaker responses than the “foreign” antigens expressed by infectious agents. Thus, immune stimulants and adjuvant approaches have been explored widely. Vaccine types considered include autologous patient-derived immune cell vaccines, tumor antigen-expressing recombinant virus vaccines, peptide vaccines, DNA vaccines, and heterologous whole-cell vaccines derived from established human tumor cell lines. Opportunities to develop effective cancer vaccines may benefit from seminal recent advances in understanding how immunosuppressive barricades are erected by tumors to mediate immune escape. In particular, targeted ablation of these barricades with novel agents, such as the immune checkpoint drug ipilimumab (anti-CTLA-4) approved recently for clinical use, may offer significant leverage to vaccinologists seeking to control and prevent malignancy.
Access provided by CONRICYT – Journals CONACYT. Download protocol PDF
Similar content being viewed by others
Key words
1 Introduction
Vaccines against cancer have been explored for over a century, but they have offered more hope than impact compared to the huge impact of vaccines against infectious diseases. However, unlike infectious disease vaccines, which focus mainly on disease prevention, cancer vaccines have focused mainly on disease treatment, a much higher bar to address, given the extant power of cancers on the immune system at levels little understood. Moreover, additional challenges for cancer vaccines to address are that the immune system in the patient is generally damaged, suppressed, or senescent, not only because of tumor burden but also the harmful experience of standard-of-care therapies and the advanced age of most cancer patients. On a brighter note, the rapid recent increase in knowledge of immune effector mechanisms and molecular signals responsible for immune suppression is stimulating the development of new modalities with greater promise. In particular, new genetic tools and insights into the key inflammatory and immune molecules to manipulate immunity in cancer patients are presenting themselves. Two recent outstanding reviews are recommended for more in-depth consideration of this area [1, 2]. The brief overview offered here introduces some fundamental issues of specific interest to cancer vaccine development, followed by an illustrative consideration of several types of vaccines that incorporate various cellular and molecular principles, vectors, and clinical trial designs.
2 Tumor Antigens, Adjuvants, and T Cell Help
Questions about what constitutes the best tumor antigen and how to target it have attracted long-standing and mainly unresolved study. Unlike microbial antigens, tumor antigens vary enormously in different cancers and cancer patients. Thus, significant effort has been put into searching for antigens that are widely mutated or aberrantly expressed in specific types of cancer and that are also capable of stimulating efficacious immune response s in preclinical model systems. Two general distinctions in the cancer vaccines that have been studied are those that target specific tumor antigens (more often molecular vaccines) and those that do not discriminate (more often cellular vaccines). Cell lineage-specific proteins can be useful to target, particularly in cancers where the normal tissue may be surgically resected as part of the standard of care (e.g., prostate or breast cancer). Since tumor antigens represent “altered self,” the induction of autoimmunity in preclinical and clinical studies by a cancer vaccine can be viewed in positive and negative contexts, depending on its severity and manageability. Consensus lists of tumor antigens considered attractive have been suggested although much work and debate continue [3].
Immunity to infectious disease produced by vaccination relies centrally on an effective adjuvant. Accordingly, adjuvant substances have received great attention from cancer vaccinologists but unfortunately without the breakthrough results produced as in the development of microbial vaccines. Pathogens, particulates, saponins, and emulsions such as incomplete Freund’s adjuvant (e.g., Montanides) have all been explored extensively, especially in peptide and recombinant virus vaccine preparations. An excellent recent presentation of this area in detail can be found elsewhere [4].
Since most cancer vaccines have sought to recruit T cell immunity, there also has been much effort dedicated to defining mechanisms of T cell help most relevant to antitumor immune response s. CD4+ T cell help is critical to generate CD8+ T effector cells and CD8+ T memory cells that are closely associated with antitumor immunity in many cancers (e.g., [5, 6]). However, as mentioned above, because of their similarity to normal cell proteins which are tolerated by the host, tumor antigens tend to trigger weak CD4+ T cell help responses. Thus, cancer vaccines that have been explored may integrate efforts to engage more florid CD4+ T cell help either directly or indirectly. For vaccines that target specific molecules, a complex phenomenon of “epitope spreading” involving drift of immune reactions to other nontargeted antigens is clearly associated with antitumor efficacy. However, limited mechanistic insights into this phenomenon remain scant, and strategies to leverage it in vaccines in any ritualized manner have yet to be done.
3 Patient-Derived Immune Cell Vaccines: Sipuleucel-T (Provenge)
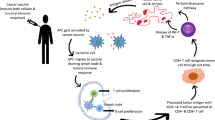
Sipuleucel-T is an autologous dendritic cell (DC) vaccine used to treat prostate cancer that is generated by modifying patient-derived DC to express a fusion protein comprised of prostatic acid phosphatase (PAP) and granulocyte-macrophage colony-stimulating factor (GM-CSF). The treatment has three parts. Patient cells are collected and a leukapheresis method is used to extract the antigen -presenting DC. The cell preparation is then sent to a corporate production facility where they are co-incubated with the fusion protein, which is taken up, processed, and presented on the cell surface. The PAP antigen is nearly universally expressed in prostate cancer cells, and the GM-CSF provides a maturation factor for the DC. In this activated antigen-presenting state, the DCs are then returned to the infusion center where they are readministered to the patient. Three courses of treatment are administered over a period of 6 weeks to trigger an immune response against PAP-positive prostate cancer cells.
In three clinical trials in advanced prostate cancer patients, sipuleucel-T treatment did not significantly extend time to progression, but it did safely lengthen overall survival of patients for an average of 4 months [7]. The vaccine was approved by the US FDA in 2010 as the first immunotherapeutic product to treat cancer, in this case asymptomatic or minimally symptomatic metastatic hormone-refractory prostate cancer. While it was assigned “category 1” status (highly recommended treatment), there has been controversy about its use due to high cost and limited benefits to patients. However, there are now 20 active trials (about half of which have completed recruitment) to test whether sipuleucel-T efficacy can be extended when combined with other standard, approved, and experimental therapies (clinicaltrials.gov). Although the impact of this vaccine has been limited in practical terms to date, its development and continued investigation have offered a clinical proof of concept for the safe and at least partially effective application of immunological principles in managing an advanced cancer that is generally intractable.
4 Recombinant Viral Vaccines Expressing Tumor Antigens: PSA-TRICOM (Prostvac-VF)
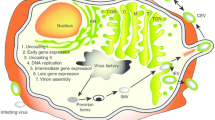
PSA-TRICOM is a recombinant viral vaccine that has been developed to treat advanced prostate cancer. The viral backbone is based on poxvirus sequences (derived from vaccinia or fowl pox) which enable expression of prostate-specific antigen (PSA) along with three immune-stimulatory T cell receptor co-regulatory molecules (LFA-3, ICAM-1, and B7.1 comprising the TRICOM element). These co-regulatory molecules were chosen to activate host DC and cytotoxic T effector cells that recognize and kill PSA-expressing prostate cancer cells. As a recombinant poxvirus, PSA-TRICOM is an off-the-shelf vaccine that is directly administered as an injection to patients. As employed clinically, the vaccinia-based vaccine is used to prime patients followed by six booster injections with the fowl pox-based vaccine.
In a Phase II clinical trial of 125 patients with minimally symptomatic metastatic prostate cancer, PSA-TRICOM was administered with GM-CSF (to promote DC activation) and compared to a control arm administered with saline. Similar to the sipuleucel-T findings, PSA-TRICOM vaccination did not affect progression-free survival (PFS), but it did extend overall survival by approximately 8 months [8]. Toxicity was low with fever, nausea, fatigue, and injection site reactions, the most common adverse events. Given this encouraging result, several trials of PSA-TRICOM in combinatorial regimens are now under way, including a highly anticipated study with the immune checkpoint inhibitor ipilimumab [9, 10], along with a global Phase III trial (PROSPECT) orchestrated by the US National Cancer Institute to validate the Phase II results.
5 Peptide Vaccines: MAGE-A3 and NY-ESO1
Among a large number of explorations of peptide antigen -based vaccines, the investigation of the widely expressed tumor antigens MAGE-A3 and NY-ESO1 stands out as paradigms. These antigens are both members of a class of “cancer-testis” antigens of obscure function that are normally expressed in testes but also overexpressed in a large number of diverse human cancers, including in lung cancers and melanomas where they have been explored deeply. Numerous preclinical and clinical studies have indicated that MAGE-A3 and MAGE-A3 fusion protein s formulated with classical immune adjuvants can trigger humoral and cellular immune response s in cancer subjects. However, a large Phase III trial of a MAGE-A3 fusion protein with H. influenzae protein D formulated with a proprietary adjuvant (MAGRIT) was stopped in 2014 due to a lack of benefit to lung cancer patients who received it. While this was a disappointing result, there remain over a dozen other clinical trials of MAGE-A3 in this and other disease settings to explore therapeutic combinations, adjuvant selection, and patient selection criteria, among other factors. One shortcoming of short peptide vaccine s can be a failure to induce memory CD8+ T cell responses [11], although it is not at all clear this factor can explain the outcome of MAGRIT. On the other hand, smaller trials of virally expressed NY-ESO1 have been encouraging and many studies of this peptide-based vaccine continue, with particular interest in combination studies such as with ipilimumab, like PSA-TRICOM .
6 DNA Vaccines
DNA vaccine s offer the opportunity to engineer protein and peptide antigen expression with more detailed design and delivery parameters, for example, to selectively express or assure suitable posttranslational modification of an antigen in the desired target cell and to enhance antigenicity and responsiveness. A vast number of preclinical studies involving numerous “gene vaccines” have established the capability to engender efficacious T cell-mediated tumor attacks against any number of target antigens [12]. These vectors may also often incorporate T cell help-inducing genes, including cytokines, chemokines, co-stimulatory molecules, or DC-targeting antibodies [13]. A similarly vast number of adjuvant and carrier formulations have been explored in both preclinical and clinical trials, with variable success. More recently, skin electroporation methods have been developed that can readily administer DNA vaccines in clinical settings. Briefly, an electric current is delivered across the tissue site at the time of vaccine injection, increasing dose levels and creating a local inflammation that helps recruit antigen-presenting cells and amplify immune response s. In general, DNA vaccination is very well tolerated with little or no side effects beyond the vaccination site. Early concerns about genomic integration or anti-DNA responses that might promote autoimmunity in patients have not proven to be issues [13].
7 Whole-Cell Vaccines Derived from Established Human Tumor Cell Lines: Algenpantucel-L (HyperAcute Pancreas)
A variety of whole-cell vaccines have been explored in human studies historically but with generally limited efficacy. One recent variation that has generated interest has incorporated the human hyperacute immune response into an “off-the-shelf” whole-cell vaccine composed of genetically modified human tumor cell lines [14, 15]. The hyperacute response is a robust mechanism of xenograft transplant rejection mediated by complement-fixing natural antibodies that recognize alpha-1,3-galactosyl (α-Gal) epitopes, a common cell surface structure found throughout evolution except in certain primate species including humans. Notably, α-Gal antibodies represent 1–2 % of all antibodies in the human peripheral blood, such that a powerful pro-inflammatory stimulus is triggered upon ligand recognition on any foreign species or tissue. In essence, the vaccine strategy coats human tumor cell lines that are lethally irradiated before subdermal injection on a traditional prime and boost schedule [16].
Whole-cell vaccines that exploit this unique pro-inflammatory mechanism have been established to be efficacious in promoting long-lasting antitumor immunity and overall survival in preclinical studies and ongoing clinical studies of resected pancreatic cancer [16]. Roving host DC readily opsonize and phagocytose the α-Gal-coated tumor cells, delivering a large number of tumor cell antigens for processing and presentation to T cells in local lymph nodes. In a Phase II study of 70 resected pancreatic cancer patients, algenpantucel-L was administered in the adjuvant setting and compared to a control arm receiving chemoradiation according to the RTOG-9704 standard of care. Disease-free survival was nearly twice the control arm at the primary endpoint despite a larger proportion of patients with node-positive disease in the experimental arm [16]. Prompted by this result, a randomized Phase III trial started in 2010 to enroll a total of 722 patients, representing the largest clinical trial of resected pancreatic cancer patients performed to date. A second Phase III study has also been initiated more recently to explore combination with standard chemotherapy and chemoradiation in 280 patients with borderline resectable or locally advanced PDA (NCT01836432).
References
Butterfield LH (2015) Cancer vaccines. BMJ 350:h988
Schlom J, Hodge JW, Palena C, Tsang KY et al (2014) Therapeutic cancer vaccines. Adv Cancer Res 121:67–124
Cheever MA, Allison JP, Ferris AS, Finn OJ et al (2009) The prioritization of cancer antigens: a national cancer institute pilot project for the acceleration of translational research. Clin Cancer Res 15:5323–5337
Hearnden C, Lavelle EC (2013) Adjuvant strategies for vaccines: the use of adjuvants within the cancer vaccine setting. In: Prendergast GC, Jaffee EM (eds) Cancer immunotherapy: immune suppression and tumor growth, 2nd edn. Elsevier, New York, p 655
Galon J, Costes A, Sanchez-Cabo F, Kirilovsky A et al (2006) Type, density, and location of immune cells within human colorectal tumors predict clinical outcome. Science 313:1960–1964
Angell H, Galon J (2013) From the immune contexture to the Immunoscore: the role of prognostic and predictive immune markers in cancer. Curr Opin Immunol 25:261–267
Sobol I, Thompson RH, Dong H, Krco C, Kwon ED (2015) Immunotherapy in prostate cancer. Curr Urol Rep 16:34
Kantoff PW, Schuetz TJ, Blumenstein BA, Glode LM et al (2010) Overall survival analysis of a phase II randomized controlled trial of a Poxviral-based PSA-targeted immunotherapy in metastatic castration-resistant prostate cancer. J Clin Oncol 28:1099–1105
Jochems C, Tucker JA, Tsang KY, Madan RA et al (2014) A combination trial of vaccine plus ipilimumab in metastatic castration-resistant prostate cancer patients: immune correlates. Cancer Immunol Immunother 63:407–418
Madan RA, Mohebtash M, Arlen PM, Vergati M et al (2012) Ipilimumab and a poxviral vaccine targeting prostate-specific antigen in metastatic castration-resistant prostate cancer: a phase 1 dose-escalation trial. Lancet Oncol 13:501–508
Rezvani K, Yong AS, Mielke S, Jafarpour B et al (2011) Repeated PR1 and WT1 peptide vaccination in Montanide-adjuvant fails to induce sustained high-avidity, epitope-specific CD8+ T cells in myeloid malignancies. Haematologica 96:432–440
Rice J, Ottensmeier CH, Stevenson FK (2008) DNA vaccines: precision tools for activating effective immunity against cancer. Nat Rev Cancer 8:108–120
Stevenson FK, di Genova G, Ottensmeier CH, Savelyeva N (2013) Genetic vaccines against cancer: design, testing and clinical performance. In: Prendergast GC, Jaffee EM (eds) Cancer immunotherapy: immune suppression and tumor growth, 2nd edn. Elsevier, New York, p 655
Rossi GR, Mautino MR, Unfer RC, Seregina TM, Vahanian N, Link CJ (2005) Effective treatment of preexisting melanoma with whole cell vaccines expressing alpha(1,3)-galactosyl epitopes. Cancer Res 65:10555–10561
Rossi GR, Unfer RC, Seregina T, Link CJ (2005) Complete protection against melanoma in absence of autoimmune depigmentation after rejection of melanoma cells expressing alpha(1,3)galactosyl epitopes. Cancer Immunol Immunother 54:999–1009
Springett GM (2014) Novel pancreatic cancer vaccines could unleash the army within. Cancer Control 21:242–246
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer Science+Business Media New York
About this protocol
Cite this protocol
Thomas, S., Prendergast, G.C. (2016). Cancer Vaccines: A Brief Overview. In: Thomas, S. (eds) Vaccine Design. Methods in Molecular Biology, vol 1403. Humana Press, New York, NY. https://doi.org/10.1007/978-1-4939-3387-7_43
Download citation
DOI: https://doi.org/10.1007/978-1-4939-3387-7_43
Published:
Publisher Name: Humana Press, New York, NY
Print ISBN: 978-1-4939-3385-3
Online ISBN: 978-1-4939-3387-7
eBook Packages: Springer Protocols