Abstract
The advent of nanotechnology in the medical arena has led to unique ways of biomaterials engineering and device modifications, disease detection and treatment. To this end, the two principal nanomedicine focus areas are cancer and cardiovascular pathologies. The current chapter is aimed at presenting a comprehensive review of nanotechnology-based strategies in cardiovascular diseases, with emphasis on targeted delivery of therapeutic payloads selectively at the disease site. The rationale for such strategies stem from the need of resolving the issues of (1) rapid drug clearance, (2) plasma-induced drug deactivation, (3) suboptimal drug availability at the disease site, and (4) indiscriminate biodistribution of the drugs leading to harmful systemic side effects, all of which arise when drugs are administered directly in systemic circulation. The most significant application of nanotechnology in resolving these issues is by packaging the drugs within plasma-stable nanovehicles that can preferentially accumulate at the vascular disease site via passive uptake or bind actively to the site via antigen-specific ligands decorated on the vehicle surface. During past three decades, significant advancements in understanding vascular disease-associated genomics and proteomics, cellular and molecular mechanisms as well as nanoscale and microscale strategies of biomaterials engineering have led to several exciting nanomedicine approaches in vascular disease treatment. The chapter will describe these approaches in terms of materials engineering, payload release mechanisms, biochemical and biophysical design parameters of the delivery platforms, and integration of multiple design parameters and functionalities on single vehicle platform, along with discussing the promises and limitations of such vascular nanomedicine approaches.
Access provided by CONRICYT – Journals CONACYT. Download protocol PDF
Similar content being viewed by others
Key words
1 Introduction
Vascular diseases continue to be the number one cause of tissue morbidities and mortalities in the USA and globally [1, 2]. According to the recent statistical data reported by the American Heart Association, ~40 % of adult American adults suffer from vascular diseases and the number is over 80 % in the aging (80+ years) population. Mortalities from vascular diseases in the USA were reported to be close to 800,000 (male + female) in a recent statistical report in 2010 [1]. Consequently, significant research and clinical efforts are directed in prevention and treatment of these diseases. Vascular diseases can fall into many categories, for example, coronary heart disease leading to unstable angina and myocardial infarction, cerebrovascular disease leading to ischemia and stroke, atherosclerosis and peripheral arterial diseases, deep vein thrombosis, pulmonary and distal embolisms, restenosis following catheterized interventions, and congenital or acquired heart diseases or hemostatic dysfunctions. Many of these disease conditions have common spatiotemporal cellular and molecular mechanisms, the most predominant of which is the formation of intravascular occlusive clots (thrombi) that reduce antegrade blood flow to vital tissues and organs, often leading to tissue morbidities and mortalities. Therefore, many clinical strategies are focused on prophylactic, emergent and sustained prevention of thrombo-occlusive events to maintain normal blood flow to tissues and organs. The prophylactic strategies mainly involve oral or systemic administration of anticoagulant (e.g., heparin) and antiplatelet (e.g., Aspirin and Clopidogrel) agents, the emergent strategies mainly involve mechanical (e.g., catheter-mediated or aspiration-based thrombectomy, balloon angioplasty), surgical (e.g., aortic or coronary thrombus removal, bypass grafting) and fibrinolytic pharmacotherapy (e.g., intravascular bolus administration or infusion of plasminogen activators like streptokinase (SK) and tissue plasminogen activator (tPA)) procedures, while the sustained strategies mostly involve post-procedural prolonged oral administration of anticoagulant and antiplatelet drugs as well as drug-eluting stent (DES, releasing anticoagulant or antiproliferative drugs) placement during catheter-based interventional procedures like balloon angioplasty. As evident from these descriptions, systemic (oral and intravascular) administration of drug molecules that prevent platelet activation and aggregation (antiplatelet agents), block coagulation pathways (anticoagulant agents), degrade clot proteins (fibrinolytic agents), or downregulate unwanted cellular proliferation (antiproliferative agents) remain a major component of clinical regimen in treating occlusive vascular disease conditions. Systemic administration of these drugs presents several harmful issues [3–6]:
-
(a)
Rapid drug washout and clearance from the target site due to dynamic blood flow
-
(b)
Plasma-induced inactivation of the drugs and reduced circulation half-life
-
(c)
Systemic nonspecific distribution of the drugs resulting in suboptimal availability at target
-
(d)
Systemic nonspecific action of the drugs leading to harmful side effects like coagulopathy, neurotoxicity and nephrotoxicity, and hemorrhage
These issues can be potentially resolved by localizing the delivery (and action) of the drugs at the target clot sites. One way to achieve such site-selective delivery is by implanted devices like trans-arterial infusion catheters and DES. Implantation procedures like these are expensive, require specific expertise in terms personnel and facilities, and are not accessible by or amenable to many patients within required treatment windows [7–10]. Another way is to manufacture drug molecules that possess some target-specificity of binding (and action) by virtue of bioconjugation of antibodies and other ligands directly to the drug molecules or by recombinant modifications of the drug itself to impart target-specificity [11–15]. Direct antibody conjugation to drugs may affect drug activity and recombinant technologies make the resultant products quite expensive for global use especially in developing countries. Therefore, in recent years, alternative drug delivery strategies utilizing the “nanomedicine” approach have raised significant clinical interest [16]. The ideal “nanomedicine” design for site-selective delivery of drugs in vascular diseases should consist of a “carrier vehicle” that can encapsulate the drug in its core or embed it on the vehicle surface, protect the drug from plasma-induced inactivation while increasing its circulation half-life, localize via passive uptake and/or active molecular mechanisms to the vascular disease site to ensure site-specific delivery of the drug payload, enable controlled release of the payload via diffusion, dispersion, or stimuli-triggered mechanisms to allow site-selective therapeutic action while reducing systemic harmful side-effects, and biodegrade or get cleared from the body safely within a reasonable time frame so as to not render long term effects. The “payload” in such vehicles can not only be drug molecules, but also imaging probes that can allow detection and diagnosis of disease sites, and the combination of therapeutic and diagnostic payloads can potentially lead to “theranostic” nanomedicine systems targeted to vascular disease sites. The following sections review the various “nanomedicine” technologies that have been developed and are undergoing research currently in the context of the above-described design, followed by a discussion of the pros and cons and future endeavors.
2 Nanomedicine Systems Without Ligand-Based Site-Specific Active Binding Mechanisms
Direct systemic delivery of therapeutic (and diagnostic) agents often leads to inactivation of the agents by various plasma components, rapid washout from target site, and rapid clearance from circulation via organs like liver and kidney. Resolving these issues require increasing the circulation residence time of the agents in active form. This is where “packaging” of the agents within carrier vehicles can provide a solution. The concept is derived originally from the “Ringsdorf Model” in the application of macromolecular modifications of cancer drugs (Fig. 1), where the drug molecules are conjugated to polymers that prevent rapid plasma clearance of the small drug molecules due to enhancement of overall hydrodynamic radius by virtue of the drug–polymer conjugates [17–19]. The conjugation of the drugs to the various polymers are mediated by chemical bonds like amide, orthoester, ester, anhydride, carbonate, and urethane that can be cleaved by enzymatic and/or pH-sensitive reaction mechanisms to release the active drug for subsequent action. For cardiovascular drugs, this design has been tried by polyethylene glycol (PEG )-based modification (PEG-ylation) of fibrinolytic agents like tPA, SK, urokinase (uPA), and staphylokinase (Sak) [20–24]. The antiproliferative drug Paclitaxel (clinicaly used in DES for treatment of restenosis and intimal hyperplasia) has also been conjugated to polymers like polyglutamic acid (PGA) to result in products like Xyotax that are undergoing clinical study for cancer treatment but may also find cardiovascular applications. Besides drug–polymer conjugates, the other strategy to protect the drugs and increase circulation stability and residence time, is to package them in microparticulate and nanoparticulate vehicles. To this end, extensive research has been carried out using vehicles like liposomes, polymeric particles, lipoprotein particles, micelles, engineered red blood cells (RBCs), quantum dots, gold particles, dendrimers , ultrasound-sensitive bubbles and iron oxide particles (Fig. 1).
Vesicular liposomal structures, originally reported by Sir Alec Bangham [25, 26], have a lipidic (hydrophobic) shell and an aqueous core, thereby providing potential volume fractions for encapsulating both hydrophobic and hydrophilic drugs. Liposomes are formed by thermodynamically driven self-assembly of lipid-based amphiphilic molecules when exposed to an aqueous environment. Specifically, these molecules would need to have a packing fraction (v × a −1 × l −1 where “v” is the hydrophobic volume, “a” is the hydrophilic surface area, “l” is hydrophobic length) equal to 1, such that when exposed in an aqueous environment, they would form planar lamellar bilayer structures that ultimately fold into spherical vesicles with a bilayer lipidic shell and aqueous core. This kind of self-assembled vesicular structure can be unilamellar (single lamellar shell) or multilamellar (multiple concentric bilayer shells), and their size can range from about 50 nm to a few microns in diameter. Usually by extrusion through nanoporous polycarbonate membranes or by exposing to high frequency ultrasound, larger multilamellar vesicles can be reduced to nanoscale (50–200 nm diameter) unilamellar vesicles. Furthermore, modification of the liposome lamella outer surface with hydrophilic polymers like PEG imparts a steric hindrance to opsonization (blood protein adsorption) and macrophagic uptake, and thereby renders a “stealth” property to avoid rapid clearance from circulation [27], that in effect enhances the circulation residence time of the encapsulated drug payload. The most significant clinical application of liposomes is in the formulation of cancer drugs like Doxil®, Daunosome®, and Myocet® [28], which have made this class of vehicles a popular choice in studying encapsulation and delivery of drugs to other diseases including cardiovascular diseases. To this end, various antithrombotic agents have been encapsulated in liposomes and these formulations have shown enhanced circulation half-life of the drugs and increased therapeutic efficacy in vitro as well as in vivo in small animal models [29–33]. Liposomes, especially with cationic lipid shells, have been also used to complex DNA for gene delivery in cardiovascular diseases [34–39]. Besides drugs and DNA, liposomes have also been reported to encapsulate imaging agents like the MRI contrast agent gadolinium (Gd), either by direct loading of Gd salts or by lipid conjugation of Gd chelates, for imaging of vascular diseases [40–43]. Instead of lipidic systems, amphiphilic block co-polymeric systems with packing fraction equal to 1 can also be used to assemble similar vesicular structures called polymersomes [44–46]. Potentially such structures can also be used to package and deliver a wide variety of therapeutic agents in cardiovascular pathologies. Similar to liposomes, micelles are also self-assembled colloidal nanostructures with a hydrophobic core and a hydrophilic shell formed from amphiphilic molecules with packing parameter of ~1/3 when exposed to aqueous environment, and can be formed from lipid-based or polymer -based amphiphilic systems. These vehicles also have been extensively investigated in formulation of cancer drugs, but only a limited number of reports are available regarding their drug delivery applications in the cardiovascular area. PEG-polycation micelles have been utilized for gene delivery to arterial disease lesions in rabbit models [47]. Potential micelle-based strategies that could be directed toward diseased or dysregulated endothelial components of atherosclerotic and thrombotic sites in vascular diseases have been recently reviewed [48, 49]. To this end, several micelle-based strategies have been studied by incorporating ligand-based active targeting, which will be discussed in the next section.
Polymer based microparticles and nanoparticles have been of great interest in vascular drug delivery for past two decades [7, 8, 50]. Polymer-based drug-carrier particles can be formed by a wide variety of methods like oil/water or water/oil/water emulsion based solvent evaporation technique, solvent diffusion technique, solvent displacement technique, salting out technique, interfacial polymerization technique, and supercritical fluid technologies [51]. Polymeric nanoparticle carriers based on co-polymerized systems of biocompatible polymers like poly-lactic-co-glycolic acid (PLGA ), polyethylene glycol (PEG ), polyvinyl alcohol (PVA), etc. have been utilized to encapsulate and deliver anticoagulant agents like heparin [52], fibrinolytic agents like tPA and SK for clot dissolution [31, 53], and antiproliferative agents like probucol, rapamycin and paclitaxel for reducing restenosis [54–61]. Some polymer nanoparticle-based anti-restenotic formulations have also been evaluated in clinical studies [62]. Ultrasound imaging modalities are well established in diagnosis of physiological and pathological tissues , and ultrasound contrast agent bubbles like Definity (Bristol Meyers Squibb), a perfluoropropane/air filled lipid-shelled microbubble, have been approved in the clinic for cardiac imaging [63]. Consequently, such bubble systems have also been investigated for vascular therapeutic and diagnostic applications, where the bubble not only acts as a carrier for drugs but also allows focused ultrasound-mediated cavitation for site-selective release of the drugs. For example, poly(vinyl alcohol) (PVA)-based bubble structures were reported that can be loaded with the vasodilatory and antithrombotic bioactive gas nitric oxide (NO), for simultaneous imaging and NO delivery to vascular disease tissues [64]. Ultrasound-sensitive bubbles that allow cavitation-induced payload release have been reported for delivery of DNA, double stranded RNA and oligonucleotides, recombinant proteins , growth factors and thrombolytic agents (e.g., SK, tPA, etc.) [65–69]. Terminologies like “sonothrombolysis” has been coined to emphasize the combined effect of ultrasound-induced mechanical cavitation and site-specific thrombolytic drug release to enhance clot dissolution properties. Dendrimers are another important class of highly branched polymeric globular nanosystems originally developed in the 1980s by “convergent” or “divergent” chemical techniques [70, 71], that have undergone extensive studies in the delivery of genes, drugs and imaging agents utilizing the dendrimer core, the branching zone and the branch extremities [72]. Most dendrimeric applications in vascular drug delivery have involved ligand-based active targeting and will be discussed in the next section.
Among inorganic nanovehicle systems, carrier particles made from gold and iron oxide have been extensively studied in delivery of therapeutic and imaging agents in cancer [73–78]. Colloidal gold nanoparticle s can be prepared by an array of methods that are mainly based on reduction of chloroauric acid in presence of a colloidal suspension stabilizing agent, and the methods vary mostly in terms of the reducing agents and reaction conditions [79–82]. Galvanic replacement methods have also been utilized to synthesize hollow gold nanostructures from gold salts [83, 84]. Gold nanoparticles and nanostructures have been studied not only as carrier vehicles for drug delivery and imaging, but also because of their plasmonic activity and near infra-red (NIR) wavelength sensitivity, they have been used to render NIR-induced targeted photothermal phenomena and photoacoustic imaging. To this end, gold nanoparticles have been recently reported in the context of cell-specific imaging as well as image -guided targeted drug delivery in the cardiovascular disease area [85, 86]. In a recent report, novel Au-based lipoprotein-coated nanoparticles (Au core coated with Apolipoprotein A-1 and phospholipids) were shown to be taken up by atherosclerosis-relevant macrophages in ApoE−/− mice in vivo and hence provided a way for enhanced multispectral and multimodality imaging of the lesions for characterization of macrophage burden, calcification and stenosis [87]. In another report, NIR-fluorescence-quenched gold nanoparticle based imaging probes were used where the particles were surface-modified by a peptide sequence that can be specifically degraded by matrix metalloproteases (MMPs) and also surface-modified with an NIR fluorescence dye, Cy5.5 [88]. MMP activity is prevalent in matrix remodeling and lesion progression processes in atherosclerosis, and therefore such nanosystems may become useful in detection and evaluation of vascular lesion progression. In another interesting work, the photothermal ablative effects of gold nanoparticles were used to render disruption and recanalization of atherosclerotic plaques in coronary arteries in human postmortem ex vivo specimens [89]. Iron oxide particles are usually prepared by co-precipitation methods involving addition of alkali to iron salts [90]. Superparamagnetic iron oxide (SPIO) particles are categorized mostly by their hydrodynamic diameter, e.g., Oral-SPIO (300 nm–3.5 μm), Standard-SPIO (SSPIO, 60–150 nm), Ultrasmall-SPIO (USPIO, 5–40 nm), and a subset of USPIO called monocrystalline iron oxide NPs (MION). Furthermore, MIONs with a chemically cross-linked polysaccharide shell are termed Cross Linked Iron Oxide (CLIO) [91, 92]. Iron oxide nanoparticles have been extensively reported in magnetic resonance based cellular and molecular imaging of cardiovascular diseases [93–102]. Incorporating therapeutic molecules in such iron oxide systems can provide efficient theranostic systems for cardiovascular therapies, as has been recently demonstrated regarding delivery of antithrombotic and anticoagulant agents using such particles [103, 104]. In another interesting work, iron oxide nanoparticles were incorporated within PLGA particles and co-loaded with paclitaxel to form drug-loaded magnetic nanoconstructs, which were guided by an induced magnetic field to carotid artery sites in vivo in animal models for sustained-release vascular antiproliferative therapy [105]. In recent years, there has been significant interest in engineering of multicomponent nanoparticle systems for theranostic use or multimodal targeted imaging applications, by combining different types of imaging probes and therapeutic agents on an iron oxide nanoparticle platform [106–109]. Another class of inorganic nanostructures that have been extensively researched in targeted drug delivery and imaging is Quantum dots (QDs), that are semiconductor nanocrystals (e.g., QD with a cadmium selenide core with a zinc sulfide shell) with unique size - and composition-dependent fluorescent properties and are also sufficiently electron dense to facilitate electron microscopy [110]. The in vivo distribution, residence, and safety of QDs remain a matter of debate [111–114]. Nonetheless, QDs have been investigated in vascular delivery and imaging applications, for example, by incorporating them in high density lipoprotein (HDL)-based plaque-targeting for optical imaging of plaques [115]. The same HDL particles, incorporated with MRI probes, have been further investigated for targeted imaging of atherosclerotic plaques [115–117]. Several QD-based nanosystems have also been investigated in ligand-mediated active targeting to vascular lesions, which will be discussed in the next section.
3 Nanomedicine Systems with Ligand-Based Site-Specific Active Binding Mechanisms
Many of the nanovehicle systems described in the previous section have also been utilized to developed “actively targeted” delivery devices where the particles can bind to disease sites and diseased cells by virtue of specific ligand–receptor interactions. The ligands in such cases can be antibodies, antibody fragments, proteins and peptides, while, the receptors are antigens and proteins either uniquely expressed or quantitatively upregulated at the disease site cells and matrix. Such active targeting is thought to help with selectivity and specificity of targeting as well as with receptor-mediated internalization of the vehicles within diseased cells for intracellular delivery in some cases [118–120]. The ligands can be decorated on the nanoparticulate vehicles via non-covalent methods as well as a variety of covalent bioconjugation techniques.
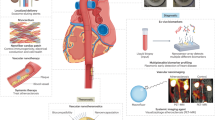
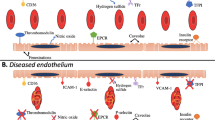
Non-covalent adsorption methods to surface-decorate nanovehicles with ligands mostly involve physical (e.g., hydrophobic, affinity-based, charge-based) interactions of ligand molecules with the surface material of the particles. For example, polystyrene particles have been reported to be coated with P-selectin and E-selectin targeting antibodies using adsorbed bacterial protein A molecules as spacers [121]. These selectins are often expressed on activated platelets, stimulated endothelial cells and monocytes at the site of vascular injuries and lesions, and therefore are relevant systems for active targeting of drug delivery system s to such vascular disease sites. Similar techniques have also been reported for coating chitosan particles with anti-amyloid monoclonal antibodies to target amyloid beta-protein deposits in cerebral vasculature of mice [122]. In other work, liposomes, latex beads and albumin particles have been non-covalently surface-modified with recombinant glycoprotein Ib-alpha (rGPIbα) and recombinant glycoprotein Ia-IIa (rGPIa-IIa) to actively bind to von Willebrand Factor (vWF) and collagen respectively [123–125]. vWF is secreted and deposited from injured endothelial cells and activated platelets, while collagen is often exposed as the major sub-endothelial matrix protein at vascular injury sites due to endothelial denudation. Therefore such vWF- and collagen-targeting systems can have potential application in targeted delivery to vascular injury sites. Another interesting non-covalent approach to decorate nanoparticles with targeting motifs is the use of avidin-biotin affinity interaction . Avidin (and analogous Streptavidin) is a highly glycosylated positively charged protein that is uniquely stable against heat, denaturants, pH and proteolytic enzymes, and has high affinity towards Biotin (Vitamin B6) with a dissociation constant (K d) of 10−15 M [126, 127]. Consequently particles can be surface-modified with avidin and incubated with biotinylated ligand motifs, or vice versa, to create ligand-decorated actively targeted delivery systems. This approach has been used extensively in decorating particle surfaces with antibodies and antibody fragments for targeting to cancer . In the area of targeting cardiovascular diseases, this technique has been employed to surface-decorate RBCs with antithrombotic molecules (e.g., tPA) as well as to decorate various nanovehicle systems with antibodies directed to a variety of vascularly relevant cell adhesion molecules (CAMs) [128–131]. Covalent bioconjugation techniques involve specific chemical reactions of reactive groups on ligand motifs to complimentary reactive groups on the nanovehicle surface. The most common chemical bioconjugation methods are amide linkages (reaction between amine and carboxyl termini), hydrazine-based linkages (reaction between hydrazide and aldehyde termini), sulfhydryl-mediated linkages (reaction between sulfhydryl group and maleimide, sulfone, acetamide or pyridyl groups) and alkyne-azide based “click” chemistry [132]. Figure 2 shows schematic of some common bioconjugation strategies for decorating nanoparticle surfaces with targeting motifs. These methods can be utilized to conjugate antibodies, antibody fragments, aptamers, proteins , and peptides to a wide variety of nanovehicle systems either by reacting to appropriate functional groups on the surface of preformed particles (solid polymer particles, QDs, dendrimers , etc.), or by reacting to the termini of constituent molecules first and then assembling the modified molecules into particles (e.g., liposomes, micelles). Figure 3 shows the commonly studied cellular and noncellular targets for vascular nanomedicine technologies.
Relevant cellular and noncellular targets utilized for active targeting of vascular nanomedicine systems. The targets can be cell-surface antigens as well as a variety of substrate proteins relevant to the vascular disease site. CAMs cell adhesion molecules, ADP adenosine diphosphate, PDGF platelet derived growth factor, FGF fibroblast growth factor, LDL low density lipoproteins
By utilizing the various non-covalent or covalent surface-modification techniques stated above, a large number of actively targeted nanoparticle systems have been reported for site-specific delivery of drugs and imaging probes in vascular diseases. To this end, echogenic liposomes have been reported that can target fibrinogen, fibrin or intercellular adhesion molecule-1 (ICAM-1) by virtue of anti-fibrinogen, anti-fibrin, and anti-ICAM-1 antibodies and allow ultrasound-induced cavitation mediated delivery of thrombolytic agents [133–135]. In another work, Gadolinium (Gd)-based MRI contrast agent delivery to atherosclerotic tissue was demonstrated by using liposomes modified with Gd-lipid conjugates and phosphatidylserine (PS) to enable preferential uptake by atherosclerotic site-relevant macrophages [41]. Similar strategy in macrophage-targeting of liposomes was also demonstrated with liposomes modified by the ligand decadeoxyguanine, which has high affinity to macrophagic scavenger receptor class A (SRA) [42]. Liposomes surface-decorated with antibodies directed to low density lipoprotein receptors LOX-1 have been reported to enable atherosclerotic lesion-targeted delivery of radioimaging and MR imaging agents [136]. Another liposomal formulation, named LipoCardium, was reported for targeted delivery of anti-inflammatory prostaglandins to atheroslecrotic sites using liposomes surface decorated with antibodies directed to Vascular Cell Adhesion Molecule-1 (VCAM-1) [137]. Besides surface-decoration of antibodies, liposomes have also been reported to be surface-decorated with small peptides having targeting ability to vWF, collagen, activated platelet glycoprotein IIb-IIIa (GPIIb-IIIa) and P-selectin, all of which are suitable target molecules in the context of endothelial injury, endothelial denudation, platelet activation, and thrombosis in vascular pathologies [138–145]. Therefore these liposomal systems can have potential application in targeted delivery of drugs and imaging agents to various spatiotemporal phases of vascular injury and vascular disease. Similar to liposomes, micelles (both lipidic and block co-polymeric) have been studied for actively targeted delivery to vascular disease sites. Micelles surface-decorated with antibodies specific for macrophage scavenger receptors (MSR) and loaded with Gd chelates or fluorescent probes were shown to selectively target and accumulate at atherosclerotic arterial sites in ApoE−/− mice for molecular imaging of the disease [146, 147]. Gd-loaded PEG -lipid micelles surface-modified by antibodies that bind to oxidized LDL lipoproteins in atherosclerotic plaques, have also been reported [148]. Similar Gd-loaded micelles surface-decorated with anti-CD36 antibodies were shown to target macrophages in atherosclerotic vessels [149]. Recently, lipid-polymer hybrid particles (polymer core with lipid shell) decorated with a phage library-identified peptide sequence KZWXLPX (Z: hydrophobic amino acid, X: any amino acid) were reported as “nanoburrs” that can actively target exposed collagen IV at arterial injury (i.e., endothelial denudation) sites and deliver antiproliferative agents to modulate smooth muscle cell activity [150, 151]. In another recent work, micelles were surface decorated with a 9-amino acid sequence CGNKRTRGC (also known as Lyp-1) that binds to p32 receptors in atherosclerotic plaques as well as with CREKA peptides that bind to fibrin-fibronectin clots, and these micelles showed enhanced homing to atherosclerotic plaques in vivo [152, 153].
Similar to liposomes and micelles, solid polymeric particles have also been studied for surface-modification with ligands to enable targeted binding to vascular injury or vascular disease sites. For example, PLGA nanoparticles have been loaded with thrombolytic drugs like tPA and coated with Arginine-Glycine-Aspartic Acid (RGD)-peptide modified chitosan to render targeted binding to clots for enhanced thrombolytic efficacy [53]. PLGA nanoparticles have also been reported to be surface-modified with anti-ICAM-1 antibodies for specific immunotargeting to inflamed vascular endothelium in vitro and in vivo, which has relevance to targeting atherosclerotic plaques [154]. Similarly, poly(sebacic acid)-co-PEG (PSAPEG) microparticles and nanoparticles surface-modified with anti-VCAM-1 antibodies have been reported to undergo enhanced adhesion, binding and accumulation at atherosclerotic lesion sites in ApoE−/− mice [155]. Nanoparticles made from poly-l-lysine-co-poly-lactic acid copolymer (PLL-PLA), surface-decorated with RGD peptides have been reported to be able to aggregate with active platelets at the site of traumatic vascular injury [156]. Similar designs of RGD-decorated or the fibrinogen-derived peptide sequence HHLGGAKQAGDV-decorated particles have also been reported using RBCs, latex beads or albumin particles as the carrier vehicle [157–162]. The HDL nanoparticles described in the previous section were designed to be naturally taken up into atherosclerotic lesions via lipoprotein transport mechanisms; however these same particles have also been reported to be modified with RGD peptides to enable active targeting ability to vasculature [163]. Ligand-based active targeting strategies have also been reported for ultrasound-sensitive bubbles where the bubbles were surface-decorated with antibodies directed against inflammation and atherosclerosis relevant upregulated cell-surface markers like various CAMs and integrins (e.g., αVβ3), on leukocytes and injured endothelium, in vitro and in vivo, for targeted drug delivery to and molecular imaging of vascular disease [164–166]. In similar work, ultrasound-sensitive bubbles were developed with shells bearing maleimido-4(p-phenylbutyrate)-phospholipid, which were then surface-conjugated with platelet integrin GPIIb-IIIa-specific therapeutic antibody Abciximab (ReoPro by Eli Lilly, Indianapolis, Indiana), that enabled enhanced targeting to activated platelet-rich thrombi for molecular imaging applications in vitro and in vivo [167]. Dendrimers have also been studied for active targeting to vascular pathology sites, where biodegradable dendritic structures surface-modified with endothelial αVβ3 integrin-targeting cyclic RGD peptides and loaded with radioactive Bromine (76Br) for positron emission tomography (PET), were capable of targeted molecular imaging of hindlimb ischemia in a mouse model [168]. Similar targeted molecular imaging of vascular disease-specific biomolecules and cellular phenotypes have also been demonstrated with dendrimers modified by a variety of other ligands [169–171].
The inorganic nanosystems described in the previous section have also undergone extensive investigation for actively targeted delivery to vascular disease and injury sites. Cross-linked dextran-coated iron oxide (CLIO) nanoparticles have also been surface-decorated with peptides and small molecules that can target CAMs and clot-associated fibrin to enable active targeting of the particles to inflammatory, angiogenic and thrombotic cellular phenotypes and biomarkers of atherosclerosis for contrast enhanced targeted molecular imaging [92]. Iron oxide particles have also been reported to be surface-decorated with ligands directed towards VCAM-1, P-selectin and platelet integrin GPIIb-IIIa for targeted contrast-enhanced MR imaging of atherosclerosis and thrombosis in animal models [172]. In another interesting work, SPIOs were surface-modified by Annexin V that can specifically interact with lipoproteins on the outer membrane leaflet of apoptotic cells and hence enabled interaction and selective targeting of “foam cells” in atheromatous plaque in rabbit models for T2-weighted MR imaging [173]. QDs have also been utilized to actively bind a variety of CAMs (e.g., VCAM, ICAM, PECAM) using QD surface-decoration with anti-CAM antibodies [174, 175] and these facilitated in vivo optical imaging of atherosclerotic lesions. Other approaches to ligand-directed vascular disease-specific targeting of QDs for optical imaging include targeting to oxidized LDL receptor CD36, phosphatidylserine-exposing cells, and plaque-relevant MMPs [176, 177]. Instead of directly targeting QDs to the vascular disease site, they have also been used as “payloads” in other actively targeted nanosystems to allow for concurrent optical imaging modality for vascular diseases. This strategy has been utilized by loading QDs within paramagnetic micelles immunotargeted to macrophagic scavenger receptors [178] as well as within HDL nanoparticles [115]. In an interesting work, gold nanoparticle s were conjugated to QDs via a proetolytically degradable peptide sequence such that in the “bound” state the QD luminescence was non-radiatively suppressed, and enzymatic cleavage of the conjugate links significantly restored luminescence [179]. Such unique strategies can be envisioned to be applicable in probing proteolytic activities (e.g., MMP activity) in atherosclerotic lesions.
4 Other Miscellaneous Applications of Nanomaterials in Cardiovascular Disease Treatment
As evident from the descriptions and examples provided in the previous sections, “nanotechnology” has provided an efficient way to render localized or site-selective delivery of various therapeutic agents and imaging probes in vascular diseases and injuries. Such localized delivery can potentially overcome the issues of potency and narrow therapeutic window of many drug molecules by achieving greater local concentrations with lower overall dose, to maximize the effects in target tissue while avoiding systemic indiscriminate distribution and harmful side-effects. The idea of local delivery in the cardiovascular arena emerged about two decades ago in the context of using perivascular delivery systems successfully in animal models [180, 181]. In these systems, heparin-releasing polymeric matrix devices were placed around rat carotid arteries at the time of balloon angioplasty, to allow continuous local release of the drug for predetermined periods of time. These approaches were found to reduce post-procedural arterial occlusion more effectively compared to systemic heparin infusion from pumps or from drug-releasing polymer matrices placed subcutaneously distant from the target artery site. Similar local polymeric systems bearing endothelial cells as a source of endogenous vasoregulatory agents were also shown to have enhanced efficiency in reducing neointimal hyperplasia in rat and pig models of vascular injury [182, 183]. Over the past two decades, other “local delivery” systems have been developed for cardiovascular applications, including intraluminal, intramural and stent-based systems [184], all of which have proved to be much more efficient in rendering therapeutic effect at the target tissue while avoiding poor distribution and harmful side-effect issues of systemic delivery. Nanotechnology has contributed to refinement such devices. For example, silver nanoparticles have been used to modify implantable and intravascular devices to prevent bacterial adhesion, growth and biofilm development [185]. Carbon nanotubes have been incorporated in catheters to provide mechanical versatility as well as impart antithrombotic and drug delivery functions [186]. Such carbon nanotubes have also been incorporated in stents [187]. Other application of nanotechnology in stents include refined nanofabrication and nanomorphological texturing techniques to allow for enhanced drug loading, tissue-material interactions and drug release [188], as well as incorporating drug- or gene-loaded nanoparticles within stent coatings for sustained local delivery following angiopalstic procedures and stent placement [189, 190]. Nanotechnology has also been used in fabrication of artificial arterial grafts and conduits [191], although it is too early to conclude on long-term success of these designs. In the context of artificial vascular grafts, chemical nanocomposites have also been incorporated to release nitric oxide and to impart infection resistance [192].
In recent years, another facet of nanotechnology that is raising significant interest, especially in the context of drug delivery vehicles in the vascular compartment, is the role of “physical” design parameters like shape, size , modulus, etc. Several recent reports have established that particles of anisotropic shapes (spheroids, rods, disks, etc.) have a higher probability of margination from flowing blood volume towards the vascular wall [193–195]. Parallel studies have also shown that size of particles play an important role in their extent of margination to the vascular wall [196–198]. In fact a natural example of this is seen in blood platelets which can marginate better to the vascular wall through the RBC volume of flowing blood owing to their biconvex discoid shape and their quiescent ~2 μm size [199–201]. Based on such studies, recent research has focused on development of particles with tailored shapes and sizes to facilitate margination to the vascular wall [202–207]. Such margination-facilitating geometric parameters can be potentially integrated with ligand-based active targeting functionalities on particle platforms to create drug delivery and nanomedicine systems with increased site-selective localization and delivery efficiency in the vascular compartment. Another important design parameter for drug delivery system s is the mechanism of drug release. Traditionally most particulate delivery systems depend upon diffusion and degradation/dissolution mediated mechanisms for payload release [208–210]. Beyond such mechanisms, certain stimuli-triggered mechanisms have been investigated for drug delivery systems, where the payload release is induced by chemical and/or physical changes in the drug delivery system in response to internal stimuli like pH, enzyme action, temperature, etc., or, external triggers like NIR irradiation (e.g., for gold nanoparticle s ), electromagnetic wave (e.g., for iron oxide particles), high frequency focused ultrasound (e.g., for ultrasound bubbles), etc. [211–216]. A few recent studies have utilized “shear forces” as a physical release trigger because of its relevance to vascular thrombo-occlusive sites. In these studies using polymeric or lipidic particles, the increased shear forces caused by thrombo-occlusion have resulted in the disintegration of the carrier particles to release drugs like thrombolytic agents, site-selectively [217, 218]. Furthermore, an interesting aspect in the context of ligand-mediated active targeting of drug delivery vehicles is the utilization of concurrent binding to multiple receptor/antigen types pertinent to the disease site (also known as heteromultivalent binding) instead of targeting to only one type of receptor. Such targeting approaches have shown enhanced efficacy of anchorage of the vehicles to the target site under hemodynamic flow environment [142, 219], and this can potentially allow for increased target specificity as well as retention for enhanced therapeutic release. These newer design parameters are continuing to add exciting properties to vascular nanomedicine systems, that can be tailored to act selectively at disease sites by virtue of enhanced margination, enhanced anchorage, and enhanced drug release.
5 Discussion
Localized delivery of therapeutic molecules and imaging probes at the sites of vascular disease results in enhanced treatment and detection efficacy. Nanotechnology provides an efficient way to achieve such localized delivery in the context of packaging therapeutic payloads within nanoparticulate vehicles that can be intravenously injected and can accumulate passively or bind actively at the target vascular sites. The success of such approaches depend upon efficient encapsulation of the payload within the nanoparticles to protect from plasma-induced deactivation, minimize pre-target leakage or release of the payload, maintain circulation for sufficient periods of time to reach the target site, render efficient passive or active binding to the target site under hemodynamic flow, and enable efficient release of the payload by internal or external triggers. Because of the need to stay retained at the target site under hemodynamic flow environment, active binding strategies may be more effective in vascular drug delivery, compared to passive accumulation mechanisms. The delivery systems must be biocompatible, in terms of minimal immunogenicity, minimal complement activation, minimal toxicity, and minimal carcinogenicity. The drug delivery system s must also be either easily cleared from the body within a reasonable period of time, or easily biodegradable to resorbable or metabolizable products in the body. Additional design parameters to consider for the particulate vehicles are their margination-influencing shape, size , and morphology, their active targeting and anchorage-influencing ligand decoration chemistry and density, and their response to internal and external triggers. For efficient clinical translation, research should also be focused on cost and convenience of manufacture and quality control of vascular nanomedicine technologies.
References
Go AS, Mozaffarian D, Roger VL, Benjamin EJ, Berry JD, Blaha MJ et al. (2014) On behalf of the American Heart Association Statistics Committee and Stroke Statistics Subcommitte. Heart disease and stroke statistics – 2014 update: a report from the American Heart Association. Circulation 129: e28
WHO (2011) Global atlas on cardiovascular disease prevention and control. World Health Organization, Geneva
Phillips DR, Conley PB, Sinha U, Andre P (2005) Therapeutic approaches in arterial thrombosis. J Thromb Haemost 3:1577–1589
Gurbel PA, Serebruany VL (2000) Oral Platelet IIb/IIIa inhibitors: from attractive theory to clinical failures. J Thromb Thrombolysis 10:217–220
Marzilli M (1995) From the experimental myocardial infarction to the clinical acute myocardial infarction: limitations of thrombolytic therapy. Int J Cardiol 49:S71–S75
Rebeiz AG, Granger CB, Simoons ML (2005) Incidence and management of complications of fibrinolytic, antiplatelet, and anticoagulant therapy. Fundam Clin Cardiol 52:375–395
Brieger D, Topol E (1997) Local drug delivery systems and prevention of restenosis. Cardiovasc Res 35:405–413
Eccleston DS, Lincoff AM (1997) Catheter-based drug delivery for restenosis. Adv Drug Deliv Rev 24:31–43
Fattori R, Piva T (2003) Drug-eluting stents in vascular intervention. Lancet 361:247–249
Torchilin VP (1995) Targeting of drugs and drug carriers within the cardiovascular system. Adv Drug Deliv Rev 17:75–101
Zolot RS, Basu S, Million RP (2013) Antibody–drug conjugates. Nat Rev Drug Discov 12:259–260
Wang X, Palasubramaniam J, Gkanatsas Y, Hohmann JD, Westein E, Kanojia R, Alt K, Huang D, Jia F, Ahrens I, Medcalf RL, Peter K, Hagemeyer CE (2014) Towards effective and safe thrombolysis and thromboprophylaxis: preclinical testing of a novel antibody-targeted recombinant plasminogen activator directed against activated platelets. Circ Res 114:1083–1093
Dong N, Da Cunha V, Citkowicz A, Wu F, Vincelette J, Larsen B, Wang YX, Ruan C, Dole WP, Morser J, Wu Q, Pan J (2004) P-selectin-targeting of the fibrin selective thrombolytic Desmodus rotundus salivary plasminogen activator alpha1. Thromb Haemost 92:956–965
Diamond SL (1999) Engineering design of optimal strategies for blood clot dissolution. Annu Rev Biomed Eng 1:427–461
Thomas AC, Campbell JH (2004) Targeted delivery of heparin and LMWH using a fibrin antibody prevents restenosis. Atherosclerosis 176:73–81
Sen Gupta A (2011) Nanomedicine approaches in vascular disease: a review. Nanomedicine 7:763–779
Ringsdorf H (1975) Structure and properties of pharmacologically active polymers. J Poly Sci Symp 51:135–153
Elvira C, Gallardo A, Roman JS, Cifuentes A (2005) Covalent polymer-drug conjugates. Molecules 10:114–125
Duncan R (2006) Polymer conjugates as anticancer nanomedicines. Nat Rev Cancer 6:688–701
Berger HJ Jr, Pizzo SV (1988) Preparation of polyethylene glycol-tissue plasminogen activator adducts that retain functional activity: characteristics and behavior in three animal species. Blood 71:1641–1647
Rajagopalan S, Gonias SL, Pizzo SV (1985) A nonantigenic covalent streptokinasepolyethylene glycol complex with plasminogen activator function. J Clin Invest 75:413–419
Sakuragawa N, Shimizu K, Kondo K, Kondo S, Niwa M (1986) Studies on the effect of PEG-modified urokinase on coagulation-fibrinolysis using beagles. Thromb Res 41:627–635
Moreadith RW, Collen D (2003) Clinical development of PEGylated recombinant staphylokinase (PEGSak) for bolus thrombolytic treatment of patients with acute myocardial infarction. Adv Drug Deliv Rev 55:1337–1345
Collen D, Sinnaeve P, Demarsin E, Moreau H, De Maeyer M, Jespers L, Laroche Y, Van de Werf F (2000) Polyethylene glycol-derivatized cysteine substitution variants of recombinant staphylokinase for single-bolus treatment of acute myocardial infarction. Circulation 102:1766–1772
Lasic DD, Papahadjopaulos D (eds) (1998) Medical applications of liposomes. Elsevier, Amsterdam
Torchilin VP (2005) Recent advances with liposomes as pharmaceutical carriers. Nat Rev Drug Discov 4:145–160
Cˇeh B, Winterhalter M, Frederik PM, Vallner JJ, Lasic DD (1997) Stealth® liposomes: from theory to product. Adv Drug Deliv Rev 24:165–177
Wang AZ, Langer R, Farokhzad OC (2012) Nanoparticle delivery of cancer drugs. Annu Rev Med 63:185–198
Nguyen PD, O’Rear EA, Johnson AE, Patterson E, Whitsett TL, Bhakta R (1990) Accelerated thrombolysis and reperfusion in a canine model of myocardial infarction by liposomal encapsulation of streptokinase. Circ Res 66:875–878
Heeremans JLM, Prevost R, Bekkers MEA, Los P, Emeis JJ, Kluft C, Crommelin DJ (1995) Thrombolytic treatment with tissue-type plasminogen activators (t-PA) containing liposomes in rabbit: a comparison with free t-PA. Thromb Haemost 73:488–494
Leach JK, O’Rear EA, Patterson E, Miao Y, Johnson AE (2003) Accelerated thrombolysis in a rabbit model of carotid artery thrombosis with liposome-encapsulated and microencapsulated streptokinase. Thromb Haemost 90:64–70
Perkins WR, Vaughan DE, Plavin SR, Daley WL, Rauch J, Lee L, Janoff AS (1997) Streptokinase entrapment in interdigitation-fusion liposomes improves thrombolysis in an experimental rabbit model. Thromb Haemost 77:1174–1178
Kim I-S, Choi H-G, Choi H-S, Kim B-K, Kim C-K (1998) Prolonged systemic delivery of streptokinase using liposome. Arch Pharm Res 21:248–252
Dzau VJ, Mann MJ, Morishita R, Kaneda Y (1996) Fusigenic viral liposome for gene therapy in cardiovascular diseases. Proc Natl Acad Sci U S A 93:11421–11425
Nabel EG (1995) Gene therapy for cardiovascular disease. Circulation 91:541–548
Morishita R, Gibbons GH, Kaneda Y, Ogihara T, Dzau VJ (1993) Novel and effective gene transfer technique for study of vascular renin angiotensin system. J Clin Invest 91:2580–2585
Leclerc G, Gal D, Takeshita S, Nikol S, Weir L, Isner JM (1992) Percutaneous arterial gene transfer in a rabbit model: efficiency in normal and balloon-dilated atherosclerotic arteries. J Clin Invest 90:936–944
Lim CS, Chapman GD, Gammon RS, Muhlestein JB, Bauman RP, Stack RS, Swain JL (1991) Direct in vivo gene transfer into the coronary and peripheral vasculatures of the intact dog. Circulation 83:2007–2011
Chapman GD, Lim CS, Gammon RS, Culp SC, Desper S, Bauman RP, Swain JL, Stack RS (1992) Gene transfer into coronary arteries of intact animals with a percutaneous balloon catheter. Circ Res 71:27–33
Zheng J, Liu J, Dunne M, Jaffray DA, Allen C (2007) In vivo performance of a liposomal vascular contrast agent for CT and MR-based image guidance applications. Pharm Res 24:1193–1201
Maiseyeu A, Mihai G, Kampfrath T, Simonetti OP, Sen CK, Roy S, Rajagopalan S, Parthasarathy S (2009) Gadolinium-containing phosphatidylserine liposomes for molecular imaging of atherosclerosis. J Lipid Res 50:2157–2163
Rensen PC, Gras JC, Lindfors EK, van Dijk KW, Jukema JW, van Berkel TJ, Biessen EA (2006) Selective targeting of liposomes to macrophages using a ligand with high affinity for the macrophage scavenger receptor class A. Curr Drug Discov Technol 3:135–144
Mulder WJM, Douma K, Koning GA, van Zandvoort MA, Lutgens E, Daemen MJ, Nikolay K, Strijkers GJ (2006) Liposome-enhanced MRI of neointimal lesions in the ApoE-KO mouse. Magn Reson Med 55:1170–1174
Discher DE, Ahmed F (2006) Polymersomes. Annu Rev Biomed Eng 8:323–341
Lee JS, Feijen J (2012) Polymersomes for drug delivery: design, formation and characterization. J Control Release 161:473–483
Massignani M, Lomas H, Battaglia G (2010) Polymersomes: a synthetic biological approach to encapsulation and delivery. Adv Polym Sci 229:115–154
Akagi D, Oba M, Koyama H, Nishiyama N, Fukushima S, Miyata T, Nagawa H, Kataoka K (2007) Biocompatible micellar nanovectors achieve efficient gene transfer to vascular lesions without cytotoxicity and thrombus formation. Gene Ther 14:1029–1038
Ding B-S, Dziubla T, Shuvaev VV, Muro S, Muzykantov VR (2006) Advanced drug delivery systems that target the vascular endothelium. Mol Interv 6:98–112
Torchilin VP (2007) Micellar nanocarriers: pharmaceutical perspectives. Pharm Res 24:1–16
Lincoff MA, Topol EJ, Ellis SG (1994) Local drug delivery for the prevention of restenosis: facts, fancy and future. Circulation 90:2070–2084
Soppimath KS, Aminabhavi TM, Kulkarni AR, Rudzinski WE (2001) Biodegradable polymeric nanoparticles as drug delivery devices. J Control Release 70:1–20
Yang Z, Birkenhauer P, Julmy F, Chickering D, Ranieri JP, Merkle HP, Lüscher TF, Gander B (1999) Sustained release of heparin from polymeric particles for inhibition of human vascular smooth muscle cell proliferation. J Control Release 60:269–277
Chung T-W, Wang SS, Tsai W-J (2008) Accelerating thrombolysis with chitosan-coated plasminogen activators encapsulated in poly-(lactide-co-glycolide) (PLGA) nanoparticles. Biomaterials 29:228–237
Klugherz BD, Meneveau N, Chen W, Wade-Whittaker F, Papandreou G, Levy R, Wilensky RL (1999) Sustained intramural retention and regional redistribution following local vascular delivery of Polylactic-co-glycolic acid and liposomal nanoparticulate formulations containing probucol. J Cardiovasc Pharmacol Ther 4:167–174
Kolodgie FD, John M, Khurana C, Farb A, Wilson PS, Acampado E, Desai N, Soon-Shiong P, Virmani R (2002) Sustained reduction of in-stent neointimal growth with the use of a novel systemic nanoparticle paclitaxel. Circulation 106:1195–1198
Westedt U, Kalinowski M, Wittmer M, Merdan T, Unger F, Fuchs J, Schaller S, Bakowsky U, Kissel T (2007) Poly (vinyl alcohol)-graft-poly (lactide-co-glycolide) nanoparticles for local delivery of paclitaxel for restenosis treatment. J Control Release 119:41–51
Deshpande D, Devalapally H, Amiji M (2008) Enhancement in anti-proliferative effects of paclitaxel in aortic smooth muscle cells upon coadministration with ceramide using biodegradable polymeric nanoparticles. Pharm Res 25:1936–1947
Zou W, Cao G, Xi Y, Zhang N (2009) New approach for local delivery of rapamycin by bioadhesive PLGA-carbopol nanoparticles. Drug Deliv 16:15–23
Zweers ML, Engbers GH, Grijpma DW, Feijen J (2006) Release of anti-restenosis drugs from poly (ethylene oxide)-poly(DL-lactic-co-glycolic acid) nanoparticles. J Control Release 114:317–324
Luderer F, Lobler M, Rohm HW, Gocke C, Kunna K, Kock K, Kroemer HK, Westschies W, Shmitz KP, Sternberg K (2011) Biodegradable sirolimus loaded poly(lactide) nanoparticles as drug delivery systems for the prevention of in-stent restenosis in coronary stent application. J Biomater Appl 25:851–875
Nakano K, Egashira K, Masuda S, Funakoshi K, Zhao G, Kimura S, Matoba T, Sueishi K, Endo Y, Kawashima Y, Hara K, Tsujimoto H, Tominagu R, Sunagawa K (2009) Formulation of nanoparticle eluting stents by a cationic electrodesposition coating technology: efficient nano-drug delivery via bioabsorbable polymeric nanoparticle eluting stents in porcine coronary arteries. JACC Cardiovasc Interv 2:277–283
Margolis J, McDonald J, Heuser R, Klkinke P, Waksman R, Virmani R, Desai N, Hilton D (2007) Systemic nanoparticle paclitaxel (nab-paclitaxel) for in-stent restenosis-I (SNAPIST-I): a first in human safety and dose finding study. Clin Cardiol 30:165–170
Unger E, Matsunaga TO, Schumann PA, Zutshi R (2003) Microbubbles in molecular imaging and therapy. Medicamundi 47:58–65
Cavalieri F, Finelli I, Tortora M, Mozetic P, Chiessi E, Polizio F, Brismar TB, Paradossi G (2008) Polymer microbubbles as diagnostic and therapeutic gas delivery device. Chem Mater 20:3254–3258
Tsivgoulis G, Culp WC, Alexandrov AV (2008) Ultrasound enhanced thrombolysis in acute arterial ischemia. Ultrasonics 48:303–311
Marta R, Alexandrov AV (2010) Sonothrombolysis in the management of acute ischemic stroke. Am J Cardiovasc Drugs 10:5–10
Mayer CR, Bekeredjian R (2008) Ultrasonic gene and drug delivery to cardiovascular system. Adv Drug Deliv Rev 60:1177–1192
Shaw GJ, Meunier JM, Huang SL, Lindsell CJ, McPherson DD, Holland CK (2009) Ultrasound-enhanced thrombolysis with tPA-loaded echogenic liposomes. Thromb Res 124:306–310
Tiukinhoy-Laing SD, Buchanan K, Parikh D, Huang S, MacDonald RC, McPherson DD, Klegerman ME (2007) Fibrin targeting of tissue plasminogen activator-loaded echogenic liposomes. J Drug Target 15:109–114
Tomalia DA (1996) Starburst dendrimers—nanoscopic supermolecules according to dendritic rules and principles. Macromol Symp 101:243–255
Hawker CJ, Fréchet JMJ (1990) Preparation of polymers with controlled molecular architecture. A new convergent approach to dendritic macromolecules. J Am Chem Soc 112:7638–7647
Svenson S, Tomalia DA (2005) Dendrimers in biomedical applications - reflections on the field. Adv Drug Deliv Rev 57:2106–2129
Chen PC, Mwakwari SC, Oyelere AK (2008) Gold nanoparticles: from nanomedicine to nanosensing. Nanotechnol Sci Appl 1:45–66
Sperling RA, Gil PR, Zhang F, Zanella M, Parak WJ (2008) Biological applications of gold nanoparticles. Chem Soc Rev 37:1896–1908
Huang X, Jain PK, El-Sayed IH, El-Sayed MA (2008) Lasers Med Sci 23:217–228
Rosen JE, Chan L, Shieh DB, Gu FX (2012) Iron oxide nanoparticles for targeted cancer imaging and diagnostics. Nanomedicine 8:275–290
Tassa C, Shaw SY, Weissleder R (2011) Dextran-coated iron oxide nanoparticles: a versatile platform for targeted molecular imaging, molecular diagnostics, and therapy. Acc Chem Res 44:842–852
Yen SK, Padmanabhan P, Selvan ST (2013) Multifunctional iron oxide nanoparticles for diagnostics, therapy and macromolecule delivery. Theranostics 3:986–1003
Turkevitch J, Stevenson PC, Hillier J (1951) A study of the nucleation and growth process in the synthesis of colloidal gold. Discuss Faraday Soc 11:55–75
Brust M, Walker M, Bethell D, Schiffrin DJ, Whyman RJ (1994) Synthesis of thiol derivatized gold nanoparticles in a two phase liquid-liquid system. J Chem Soc Chem Commun 7:801–802
Sun Y, Xia Y (2002) Shape-controlled synthesis of gold and silver nanoparticles. Science 298:2176–2179
Vekilov PG (2011) Gold nanoparticles: grown in a crystal. Nat Nanotechnol 6:82–83
Au L, Lu X, Xia Y (2008) A comparative study of galvanic replacement reactions involving Ag nanocubes and AuCl2− or AuCl4−. Adv Mater 20:2517–2522
Choi Y, Hong S, Liu L, Kim SK, Park S (2012) Galvanically replaced hollow Au-Ag nanospheres: study of their surface plasmon resonance. Langmuir 28:6670–6676
Spivak MY, Bubnov RV, Yemets IM, Lazarenko LM, Tymoshok NO, Ulberg ZR (2013) Gold nanoparticles - the theranostic challenge for PPPM: nanocardiology application. EPMA J 4:18. doi:10.1186/1878-5085-4-18
Wang B, Yantsen E, Larson T, Karpiouk AB, Sethuraman S, Su JL, Sokolov K, Emelianov SY (2009) Plasmonic intravascular photoacoustic imaging for detection of macrophages in atherosclerotic plaques. Nano Lett 9:2212–2217
Cormode DP, Roessl E, Thran A, Skajaa T, Gordon RE, Schlomka JP, Fuster V, Fisher EA, Mulder WJ, Proksa R, Fayad ZA (2010) Atherosclerotic plaque composition: analysis with multicolor CT and targeted gold nanoparticles. Radiology 256:774–782
Lee S, Cha EJ, Park K, Lee SY, Hong JK, Sun IC, Kim SY, Choi K, Kwon IC, Kim K, Ahn CH (2008) A near-infrared fluorescence- quenched gold-nanoparticle imaging probe for in vivo drug screening and protease activity determination. Angew Chem Int Ed 47:2804–2807
Lukianova-Hleb EY, Mrochek AG, Lapotko DO (2009) Method for disruption and re-canalization of atherosclerotic plaques in coronary vessels with photothermal bubbles generated around gold nanoparticles. Lasers Surg Med 41:240–247
Karaagac O, Kockar H, Beyaz S, Tanrisever T (2010) A simple way to synthesize superparamagnetic Iron Oxide nanoparticles in air atmosphere: iron ion concentration effect. IEEE Trans Magn 46:3978–3983
Weissleder R, Elizondo G, Wittenberg J, Rabito CA, Bengele HH, Josephson L (1990) Ultrasmall superparamagnetic iron oxide: characterization of a new class of contrast agents for MR imaging. Radiology 175:489–493
McCarthy JR, Weissleder R (2008) Multifunctional magnetic nanoparticles for targeted imaging and therapy. Adv Drug Deliv Rev 60:1241–1251
Sosnovik DE, Nahrendorf M, Weissleder R (2008) Magnetic nanoparticles for MR imaging: agents, techniques and cardiovascular applications. Basic Res Cardiol 103:122–130
Bjørnerud A, Johansson L (2004) The utility of superparamagnetic contrast agents in MRI: theoretical consideration and applications in the cardiovascular system. NMR Biomed 17:465–477
Yilmaz A, Dengler MA, van der Kuip H, Yildiz H, Rösch S, Klumpp S, Klingel K, Kandolf R, Helluy X, Hiller KH, Jakob PM, Sechtem U (2013) Imaging of myocardial infarction using ultrasmall superparamagnetic iron oxide nanoparticles: a human study using a multi-parametric cardiovascular magnetic resonance imaging approach. Eur Heart J 34:462–475
Jaffer FA, Nahrendorf M, Sosnovik D, Kelly KA, Aikawa E, Weissleder R (2006) Cellular imaging of inflammation in atherosclerosis using magnetofluorescent nanomaterials. Mol Imaging 5:85–92
Trivedi RA, U-King-Im JM, Graves MJ, Cross JJ, Horsley J, Goddard MJ, Skepper JN, Quartey G, Warburton E, Joubert I, Wang L, Kirkpatrick PJ, Brown J, Gillard JH (2004) In vivo detection of macrophages in human carotid atheroma: temporal dependence of ultrasmall superparamagnetic particles of iron oxide-enhanced MRI. Stroke 35:1631–1635
Tang TY, Muller KH, Graves MJ, Li ZY, Walsh SR, Young V, Sadat U, Howarth SP, Gillard JH (2009) Iron oxide particles for atheroma imaging. Arterioscler Thromb Vasc Biol 29:1001–1008
Schmitz SA, Taupitz M, Wagner S, Wol KJ, Beyersdorff D, Hamm B (2001) Magnetic resonance imaging of atherosclerotic plaques using superparamagenetic iron oxide particles. J Magn Reson Imaging 14:355–361
Morishige K, Kacher DF, Libby P, Josephson L, Ganz P, Weissleder R, Aikawa M (2010) High- resolution magnetic resonance imaging enhanced with superparamagnetic nanoparticles measures macrophage burden in atherosclerosis. Circulation 122:1707–1715
Sigovan M, Boussel L, Sulaiman A, Sappet-Marinier D, Alsaid H, Desbled-Mansard C, Ibarrola D, Gamondès D, Corot C, Lancelot E, Raynaud JS, Vives V, Laclédère C, Violas X, Douek PC, Canet-Soulas E (2009) Rapid clearance iron nanoparticles for inflammation imaging of atherosclerotic plaque: initial experience in animal model. Radiology 252:401–409
Kawahara I, Nakamoto M, Kitagawa N, Tsutsumi K, Nagata I, Morikawa M, Hayashi T (2008) Potential of magnetic resonance plaque imaging using superparamagnetic particles of iron oxide for the detection of carotid plaque. Neurol Med Chir 48:157–162
Erdem SS, Sazonova IY, Hara T, Jaffer FA, McCarthy JR (2012) Detection and treatment of intravascular thrombi with magnetofluorescent nanoparticles. Methods Enzymol 508:191–209
Wuang SC, Neoh KG, Kang E-T, Pack DW, Leckband DE (2006) Heparinized magnertic nanoparticles: in vitro assessment for biomedical applications. Adv Funct Mater 16:1723–1730
Chorny M, Fishbein I, Yellen BB, Alferiev IS, Bakay M, Ganta S, Adamo R, Amiji M, Friedman G, Levy RJ (2010) Targeting stents with local delivery of paclitaxel-loaded magnetic nanoparticles using uniform fields. Proc Natl Acad Sci U S A 107:8346–8651
Sharma R, Kwon S (2007) New applications of nanoparticles in cardiovascular imaging. J Exp Nanosci 2:115–126
Cormode DP, Skajaa T, Fayad ZA, Mulder WJM (2009) Nanotechnology in medical imaging. Probe design and applications. Arterioscler Thromb Vasc Biol 29:992–1000
Sinusas AJ, Bengel F, Nahrendorf M, Epstein FH, Wu JC, Villanueva FS, Fayad ZA, Gropler RJ (2008) Multimodality cardiovascular molecular imaging, Part I. Circ Cardiovasc Imaging 1:244–256
Nahrendorf M, Sosnovik DE, French BA, Swirski FK, Bengel F, Sadeghi MM, Lindner JR, Wu JC, Kraitchman DL, Fayad ZA, Sinusas AJ (2009) Multimodality cardiovascular molecular imaging, Part II. Circ Cardiovasc Imaging 2:56–70
Smith AM, Gao X, Nie S (2004) Quantum dot nanocrystals for in vivo molecular and cellular imaging. Photochem Photobiol 80:377–385
Douma K, Prinzen L, Slaaf DW, Reutelingsperger CPM, Biessen EA, Hackeng TM, Post MJ, van Zandvoort MA (2009) Nanoparticles for optical molecular imaging of atherosclerosis. Small 5:544–557
Choi HS, Ipe BI, Misra P, Lee JH, Bawendi MG, Frangioni JV (2009) Tissue and organ-selective biodistribution of NIR-fluorescent quantum dots. Nano Lett 9:2354–2359
Tang Y, Han S, Liu H, Chen X, Huang L, Li X, Zhang J (2013) The role of surface chemistry in determining in vivo biodistribution and toxicity of CdSe/ZnS core-shell quantum dots. Biomaterials 34:8741–8755
Hauck TS, Anderson RE, Fischer HC, Newbigging S, Chan WC (2010) In vivo quantum-dot toxicity assessment. Small 6:138–144
Skajaa T, Cormode DP, Falk E, Mulder WJM, Fisher EA, Fayad ZA (2010) High-density lipoprotein based contrast agents for multimodal imaging of atherosclerosis. Arterioscler Thromb Vasc Biol 30:169–176
Frias JC, Williams KJ, Fisher EA, Fayad ZA (2004) Recombinant HDL-like nanoparticles: a specific contrast agent for MRI of atherosclerotic plaques. J Am Chem Soc 126:16316–16317
Frias JC, Ma Y, Williams KJ, Fayad ZA, Fisher EA (2006) Properties of a versatile nanoparticle platform contrast agent to image and characterize atherosclerotic plaques by magnetic resonance imaging. Nano Lett 6:2220–2224
Danhier F, Feron O, Préat V (2010) To exploit the tumor microenvironment: passive and active tumor targeting of nanocarriers for anti-cancer drug delivery. J Control Release 148:135–146
Hirsjärvi S, Passirani C, Benoit JP (2011) Passive and active tumour targeting with nanocarriers. Curr Drug Discov Technol 8:188–196
Huynh NT, Roger E, Lautram N, Benoît JP, Passirani C (2010) The rise and rise of stealth nanocarriers for cancer therapy: passive versus active targeting. Nanomedicine (Lond) 5:1415–1433
Blackwell JE, Dagia NM, Dickerson JB, Berg EL, Goetz DJ (2001) Ligand coated nanosphere adhesion to E- and P-selectin under static and flow conditions. Ann Biomed Eng 29:523–533
Jancsó G, Domoki F, Sántha P, Varga J, Fischer J, Orosz K, Penke B, Becskei A, Dux M, Tóth L (1998) Beta-amyloid (1-42) peptide impairs blood-brain barrier function after intracarotid infusion in rats. Neurosci Lett 253:139–141
Nishiya T, Kainoh M, Murata M, Handa M, Ikeda Y (2002) Reconstitution of adhesive properties of human platelets in liposomes carrying both recombinant glycoproteins Ia/IIa and Ib alpha under flow conditions: specific synergy of receptor-ligand interactions. Blood 100:136–142
Wada T, Okamura Y, Takeoka S, Sudo R, Ikeda Y, Tanishita K (2009) Deformability and adhesive force of artificial platelets measured by atomic force microscopy. J Biorheol 23:35–40
Nishiya T, Kainoh M, Murata M, Handa M, Ikeda Y (2001) Platelet interactions with liposomes carrying recombinant platelet membrane glycoproteins or fibrinogen: approach to platelet substitutes. Artif Cells Blood Substit Immobil Biotechnol 29:453–464
Wilchek M, Bayer EA, Livnah O (2006) Essentials of biorecognition: the (strept)avidin-biotin system as a model for protein-protein and protein-ligand interaction. Immunol Lett 103:27–32
Lesch HP, Kaikkonen MU, Pikkarainen JT, Ylä-Herttuala S (2010) Avidin-biotin technology in targeted therapy. Expert Opin Drug Deliv 7:551–564
Ganguly K, Krasik T, Medinilla S, Bdeir K, Cines DB, Muzykantov VR, Murciano JC (2005) Blood clearance and activity of erythrocyte-coupled fibrinolytics. J Pharmacol Exp Ther 312:1106–1113
Gersh KC, Zaitsev S, Cines DB, Muzykantov V, Weisel JW (2011) Flow-dependent channel formation in clots by an erythrocyte-bound fibrinolytic agent. Blood 117:4964–4967
Murciano JC, Medinilla S, Eslin D, Atochina E, Cines DB, Muzykantov VR (2003) Prophylactic fibrinolysis through selective dissolution of nascent clots by tPA-carrying erythrocytes. Nat Biotechnol 21:891–896
Muzykantov V (2013) Targeted drug delivery to endothelial adhesion molecules. ISRN Vasc Med 2013, 916254, http://dx.doi.org/10.1155/2013/916254
Sen Gupta A, von Recum HA (2014) Bioconjugation strategies: lipids, liposomes, polymersomes, and microbubbles. Chapter 6. In: Narain R (ed) Chemistry of bioconjugates: synthesis, characterization, and biomedical applications. Wiley, New York, NY
Demos MS, Alkan-Onyuksel H, Kane BJ, Ramani K, Nagaraj A, Greene R, Klegerman M, McPherson DD (1999) In vivo targeting of acoustically reflective liposomes for intravascular and transvascular ultrasonic enhancement. J Am Coll Cardiol 33:867–875
Klegerman ME, Zou Y, McPherson DD (2008) Fibrin targeting of echogenic liposomes with inactivated tissue plasminogen activator. J Liposome Res 18:95–112
Huang S-L (2008) Liposomes in ultrasonic drug and gene delivery. Adv Drug Deliv Rev 60:1167–1176
Li D, Patel AR, Klibanov AL, Kramer CM, Ruiz M, Kang BY, Mehta JL, Beller GA, Glover DK, Meyer CH (2010) Molecular imaging of atherosclerotic plaques targeted to oxidized LDL receptor LOX-1by SPECT/CT and Magnetic Resonance. Circ Cardiovasc Imaging 3:464–472
De Bittencourt PIH Jr, Lagranha DJ, Maslinkiewicz A, Senna SM, Tavares AMV, Baldissera LP, Janner DR, Peralta JS, Bock PM, Gutierrez LL, Scola G, Heck TG, Krause MS, Cruz LA, Abdalla DS, Lagranha CJ, Lima T, Curi R (2007) LipoCardium: endotheliumdirected cyclopentanone prostaglandin-based liposome formulation that completely reverses atherosclerotic lesions. Atherosclerosis 193:245–258
Haji-Valizadeh H, Modery-Pawlowski CL, Sen Gupta A (2014) An FVIII-derived peptide enables VWF-binding of a synthetic platelet surrogate without interfering with natural platelet adhesion to VWF. Nanoscale 6:4765–4773
Modery-Pawlowski CL, Tian LL, Ravikumar M, Wong TL, Sen Gupta A (2013) In vitro and in vivo hemostatic capabilities of a functionally integrated platelet-mimetic liposomal nanoconstruct. Biomaterials 34:3031–3041
Ravikumar M, Modery CL, Wong TL, Dzuricky M, Sen Gupta A (2012) Mimicking adhesive functionalities of blood platelets using ligand-decorated liposomes. Bioconjug Chem 23:1266–1275
Ravikumar M, Modery CL, Wong TL, Sen Gupta A (2012) Peptide-decorated liposomes promote arrest and aggregation of activated platelets under flow on vascular injury relevant protein surfaces in vitro. Biomacromolecules 13:1495–1502
Modery CL, Ravikumar M, Wong T, Dzuricky M, Durongkaveroj N, Sen Gupta A (2011) Heteromultivalent liposomal nanoconstructs for enhanced targeting and shear-stable binding to active platelets for site-selective vascular drug delivery. Biomaterials 32:9504–9514
Srinivasan R, Marchant RE, Sen Gupta A (2010) In vitro and in vivo platelet targeting by cyclic RGD-modified liposomes. J Biomed Mater Res A 93:1004–1015
Huang G, Zhou Z, Srinivasan R, Penn MS, Kottke-Marchant K, Marchant RE, Sen Gupta A (2008) Affinity manipulation of surface-conjugated RGD peptide to modulate binding of liposomes to activated platelets. Biomaterials 29:1676–1685
Sen Gupta A, Huang G, Lestini BJ, Sagnella S, Kottke-Marchant K, Marchant RE (2005) RGD-modified liposomes targeted to activated platelets as a potential vascular drug delivery system. Thromb Haemost 93:106–114
Mulder WJM, Strijkers GJ, Briley-Saboe KC, Frias JC, Aguinaldo JGS, Vucic E, Amirbekian V, Tang C, Chin PT, Nicolay K, Fayad ZA (2007) Molecular imaging of macrophages in atherosclerotic plaques using biomodal PEG-micelles. Magn Reson Med 58:1164–1170
Lipinski MJ, Amirbekian V, Frias JC, Aguinaldo JGS, Mani V, Briley-Saebo KC, Fuster V, Fallon JT, Fisher EA, Fayad ZA (2006) MRI to detect atherosclerosis with Gadoliniumcontaining immunomicelles targeting the macrophage scavenger receptor. Magn Reson Med 56:601–610
Briley-Saebo KC, Shaw PX, Mulder WJM, Choi SH, Vucic E, Aguinaldo JGS, Witztum JL, Fuster V, Tsimikas S, Fayad ZA (2008) Targeted molecular probes for imaging atherosclerotic lesions with magnetic resonance using antibodies that recognize oxidation-specific epitopes. Circulation 117:3206–3215
Amirbekian V, Lipinski MJ, Frias JC, Amirbekian S, Briley-Saebo KC, Mani V, Samber D, Abbate A, Aguinaldo JGS, Masey D, Fuster V, Vetrovec G, Fayad ZA (2009) MR imaging of human atherosclerosis using immunomicelles molecularly targeted to macrophages. J Cardiovasc Magn Reson 11(Suppl 1):83
Chan JM, Zhang L, Tong R, Ghosh D, Gao W, Liao G, Yuet KP, Gray D, Rhee JW, Cheng J, Golomb G, Libby P, Langer R, Farokhzad OC (2010) Spatiotemporal controlled delivery of nanoparticles to injured vasculature. Proc Natl Acad Sci U S A 107:2213–2218
Chan JM, Rhee JW, Drum CL, Bronson RT, Golomb G, Langer R, Farokhzad OC (2011) In vivo prevention of arterial restenosis with paclitaxel-encapsulated targeted lipid-polymeric nanoparticles. Proc Natl Acad Sci U S A 108:19347–19352
Peters D, Kastantin M, Kotamraju VR, Karmali PP, Gujraty K, Tirrell M, Ruoslahti E (2009) Targeting atherosclerosis by using modular, multifunctional micelles. Proc Natl Acad Sci U S A 106:9815–9819
Hamzah J, Kotamraju VR, Seo JW, Agemy L, Fogal V, Mahakian LM, Peters D, Roth L, Gagnon MK, Ferrara KW, Ruoslahti E (2011) Specific penetration and accumulation of a homing peptide within atherosclerotic plaques of apolipoprotein E-deficient mice. Proc Natl Acad Sci U S A 108:7154–7159
Muro S, Dziubla T, Qiu W, Leferovich J, Cui X, Berk E, Muzykantov VR (2006) Endothelial targeting of high-affinity multivalent polymer nanocarriers directed to intracellular adhesion molecule. J Pharmacol Exp Ther 317:1161–1169
Deosarkar SP, Malgor R, Fu J, Kohn LD, Hanes J, Goetz DJ (2008) Polymeric particles conjugated with a ligandto VCAM-1 exhibit selective avid and focal adhesion to sites of atherosclerosis. Biotechnol Bioeng 101:400–407
Bertram JP, Williams CA, Robinson R, Segal SS, Flynn NT, Lavik EB (2009) Intravenous hemostat: nanotechnology to halt bleeding. Sci Transl Med 1:11–22
Coller BS, Springer KT, Beer JH, Mohandas N, Scudder LE, Norton KJ, West SM (1992) Thromboerythrocytes. In vitro studies of a potential autologous, semiartificial alternative to platelet transfusions. J Clin Invest 89:546–555
Levi M, Friederich PW, Middleton S, de Groot PG, Wu YP, Harris R, Biemond BJ, Heijnen HF, Levin J, ten Cate JW (1999) Fibrinogen-coated albumin microcapsules reduce bleeding in severely thrombocytopenic rabbits. Nat Med 5:107–111
Okamura Y, Takeoka S, Teramura Y, Maruyama H, Tsuchida E, Handa M, Ikeda Y (2005) Hemostatic effects of fibrinogen gamma-chain dodecapeptide-conjugated polymerized albumin particles in vitro and in vivo. Transfusion 45:1221–1228
Okamura Y, Fujie T, Nogawa M, Maruyama H, Handa M, Ikeda Y, Takeoka S (2008) Haemostatic effects of polymerized albumin particles carrying fibrinogen gamma-chain dodecapeptide as platelet substitutes in severely thrombocytopenic rabbits. Transfus Med 18:158–166
Takeoka S, Okamura Y, Teramura Y, Watanabe N, Suzuki H, Tsuchida E, Handa M, Ikeda Y (2003) Function of fibrinogen gamma-chain dodecapeptide-conjugated latex beads under flow. Biochem Biophys Res Commun 312:773–779
Okamura Y, Handa M, Suzuki H, Ikeda Y, Takeoka S (2006) New strategy of platelet substitutes for enhancing platelet aggregation at high shear rates: cooperative effects of a mixed system of fibrinogen gamma-chain dodecapeptide- or glycoprotein Ibalpha-conjugated latex beads under flow conditions. J Artif Organs 9:251–258
Chen W, Jarzyna PA, van Tilborg GA, Nguyen VA, Cormode DP, Klink A, Griffioen AW, Randolph GJ, Fisher EA, Mulder WJ, Fayad ZA (2010) RGD peptide functionalized and reconstituted high-density lipoprotein nanoparticles as a versatile and multimodal tumor targeting molecular imaging probe. FASEB J 24:1689–9169
Kaufmann BA, Sanders JM, Davis C, Xie A, Aldred P, Sarembock IJ, Lindner JR (2007) Molecular imaging of inflammation in atherosclerosis with targeted ultrasound detection of vascular cell adhesion molecule-1. Circulation 116:276–284
Lindner JR (2009) Molecular imaging of cardiovascular disease with contrastenhanced ultrasonography. Nat Rev Cardiol 6:475–481
Villanueva FS, Wagner W (2006) Ultrasound molecular imaging of cardiovascular disease. Nat Clin Pract Cardiovasc Med 5:S26–S32
Alonso A, Della Martina A, Stroick M, Fatar M, Griebe M, Pochon S, Schneider M, Hennerici M, Allémann E, Meairs S (2007) Molecular imaging of human thrombus with novel abciximab immunobubbles and ultrasound. Stroke 38:1508–1514
Hagooly A, Almutairi A, Rossin R, Shokeen M, Ananth A, Anderson C, Abendschein D, Fréchet J, Welch M (2008) Evaluation of a RGD-dendrimer labeled with 76Br in hindlimb ischemia mouse model. J Nucl Med 49(Suppl 1):184
Taite LJ, West JL (2006) Poly(ethylene glycol)-lysine dendrimers for targeted delivery of nitric oxide. J Biomat Sci Polym Ed 17:1159–1172
Makowski M, Jansen C, Botnar R, Kim WY, Maintz D, Spuentrup E (2010) Molecular MRI of atherosclerosis: from mouse to man. Medicamundi 54:14
Thukkani AK, Glaus C, Welch MJ (2010) Molecular imaging of vascular inflammation with nanoparticles. Curr Cardiovasc Imaging Rep 3:151–161
McAteer MA, Akhtar AM, von Zuhr Muhlen C, Choudhury RP (2010) An approach to molecular imaging of atherosclerosis, thrombosis, and vascular inflammation using microparticles of iron oxide. Atherosclerosis 209:18–27
Smith BR, Heverhagen J, Knopp M, Schmalbrock P, Shapiro J, Shiomi M, Moldovan NI, Ferrari M, Lee SC (2007) Localization to atherosclerotic plaque and biodistribution of biochemically derivatized superparamagnetic iron oxide nanoparticles (SPIONs) contrast particles for magnetic resonance imaging (MRI). Biomed Microdevices 9:719–727
Ferrara DE, Glaus C, Taylor WR (2008) Targeting vascular epitopes using quantum dots. Nanoparticles in biomedical imaging. Fundam Biomed Tech 102:443–461
Jayagopal A, Russ PK, Haselton FR (2007) Surface engineering of quantum dots for in vivo vascular imaging. Bioconjug Chem 18:1424–1433
Kahn E, Vejux A, Menetrier F, Maiza C, Hammann A, Sequeira-Le GA, Frouin F, Tourneur Y, Brau F, Riedinger JM, Steinmetz E, Todd-Pokropek A, Lizard G (2006) Analysis of CD36 expression on human monocytic cells and atherosclerotic tissue sections with quantum dots: investigation by flow cytometry and spectral imaging microscopy. Anal Quant Cytol Histol 28:14–26
Prinzen L, Miserus RJHM, Dirksen A, Hackend TM, Deckers N, Bitsch NJ, Megens RT, Douma K, Heemskerk JW, Kooi ME, Frederik PM, Slaaf DW, van Zandvoort MA, Reutelingsperger CP (2007) Optical and magnetic resonance imaging of cell death and platelet activation using Annexin A5-functionalized quantum dot. Nano Lett 7:93–100
Mulder WJM, Koole R, Brandwijk RJ, Storm G, Chin PTK, Strijkers GJ (2006) Quantum dots with a paramagnetic coating as a bimodal molecular imaging probe. Nano Lett 6:1–6
Chang E, Miller JS, Sun J, Yu WW, Colvin VL, Drezek R, West JL (2005) Protease-activated quantum dot probes. Biochem Biophys Res Commun 334:1317–1321
Edelman ER, Adams DA, Karnovsky MJ (1990) Effect of controlled adventitial heparin delivery on smooth muscle cell proliferation following endothelial injury. Proc Natl Acad Sci U S A 87:3773–3777
Villa AE, Guzman LA, Chen W, Golomb G, Levy RJ, Topol EJ (1994) Local delivery of dexamethasone for prevention of neointimal proliferation in a rat model of balloon angioplasty. J Clin Invest 93:1243–1249
Nathan A, Nugent MA, Edelman ER (1995) Tissue engineered perivascular endothelial cell implants regulate vascular injury. Proc Natl Acad Sci U S A 92:8130–8134
Nugent HM, Rogers C, Edelman ER (1999) Endothelial implants inhibit intimal hyperplasia after porcine angioplasty. Circ Res 84:384–391
Wilensky RL, March KL, Gradus-Pizlo I et al (1995) Regional and arterial localization of radioactive microparticles after local delivery by unsupported or supported porous balloon catheters. Am Heart J 129:852–859
Zhang L, Keogh S, Rickard CM (2013) Reducing the risk of infection associated with vascular access devices through nanotechnology: a perspective. Int J Nanomed 8:4453–4466
Harris DL, Graffagnini MJ (2007) Nanomaterials in medical devices: a snapshot of markets, technologies and companies. Nanotechnol Law Business 4:415–422
Martinez AW, Chaikof EL (2011) Microfabrication and nanotechnology in stent design. Wiley Interdiscip Rev Nanomed Nanobiotechnol 3:256–268
McDowell G, Slevin M, Krupinski J (2011) Nanotechnology for the treatment of coronary in stent restenosis: a clinical perspective. Vasc Cell 3:8, http://www.vascularcell.com
Yin R-X, Yang D-Z, Wu J-Z (2014) Nanoparticle drug- and gene-eluting stents for the prevention and treatment of coronary restenosis. Theranostics 4:175–200
Goh D, Tan A, Farhatnia Y, Rajadas J, Alavijeh MS, Seifalian AM (2013) Nanotechnology-based gene-eluting stents. Mol Pharm 10:1279–1298
Sarkar S, Schmitz-Rixen T, Hamilton G, Seifalian AM (2007) Achieving the ideal properties for vascular bypass grafts using a tissue engineered approach: a review. Med Biol Eng Comput 45:327–336
de Mel A, Naghavi N, Cousins BG, Clatworthy I, Hamilton G, Darbyshire A, Seifalian AM (2014) Nitric oxide-eluting nanocomposite for cardiovascular implants. J Mater Sci Mater Med 25:917–929
Tao L, Hu W, Liu Y, Huang G, Sumer BD, Gao J (2011) Shape-specific polymeric nanomedicine: emerging opportunities and challenges. Exp Biol Med 236:20–29
Champion JA, Katare YK, Mitragotri S (2007) Particle shape: a new design parameter for micro- and nanoscale drug delivery carriers. J Control Release 121:3–9
Shah S, Liu Y, Hu W, Gao J (2011) Modeling particle shape-dependent dynamics in nanomedicine. J Nanosci Nanotechnol 11:919–928
Charoenphol P, Huang RB, Eniola-Adefeso O (2010) Potential role of size and hemodynamics in the efficacy of vascular-targeted spherical drug carriers. Biomaterials 31:1392–1402
Toy R, Hayden E, Shoup C, Baskaran H, Karathanasis E (2011) The effects of particle size, density and shape on margination of nanoparticles in microcirculation. Nanotechnology 22:1–9
Decuzzi P, Lee S, Bhushan B, Ferrari M (2005) A theoretical model for the margination of particles within blood vessels. Ann Biomed Eng 33:179–190
Skorczewski T, Erickson LC, Fogelson AL (2013) Platelet motion near a vessel wall or thrombus surface in two-dimensional whole blood simulations. Biophys J 104:1764–1772
Tokarev AA, Butylin AA, Ermakova EA, Shnol EE, Panasenko GP, Ataullakhanov FI (2011) Finite platelet size could be responsible for platelet margination effect. Biophys J 101:1835–1843
Aarts PA, van den Broek SA, Prins GW, Kuiken GD, Sixma JJ, Heethaar RM (1988) Blood platelets are concentrated near the wall and red blood cells, in the center in flowing blood. Arterioscler Thromb Vasc Biol 8:819–824
Perry JL, Herlihy KP, Napier ME, Desimone JM (2011) PRINT: a novel platform toward shape and size specific nanoparticle theranostics. Acc Chem Res 44:990–998
Daum N, Tscheka C, Neumeyer A, Schneider M (2012) Novel approaches for drug delivery systems in nanomedicine: effects of particle design and shape. Wiley Interdiscip Rev Nanomed Nanobiotechnol 4:52–65
Caldorera-Moore M, Guimard N, Shi L, Roy K (2010) Designer nanoparticles: incorporating size, shape, and triggered release into nanoscale drug carriers. Expert Opin Drug Deliv 7:479–495
Mitragotri S, Lahann J (2009) Physical approaches to biomaterial design. Nat Mater 8:15–23
Champion JA, Katare YK, Mitragotri S (2007) Making polymeric micro- and nanoparticles of complex shapes. Proc Natl Acad Sci U S A 104:11901–11904
Doshi N, Orje JN, Molins B, Smith JW, Mitragorti S, Ruggeri ZM (2012) Platelet mimetic particles for targeting thrombi inflowing blood. Adv Mater 24:3864–3869
Siepmann J, Siepmann F (2012) Modeling of diffusion controlled drug delivery. J Control Release 161:351–362
Siepmann J, Siepmann F (2013) Mathematical model of drug dissolution. Int J Pharm 453:12–24
Peppas NA, Narasimhan B (2014) Mathematical models in drug delivery: how modeling has shaped the way we design new drug delivery systems. J Control Release 190:75
Schmaljohann D (2006) Thermo- and pH-responsive polymers in drug delivery. Adv Drug Deliv Rev 58:1655–1670
Meng F, Zhong Z, Feijen J (2009) Stimuli-responsive polymersomes for programmed drug delivery. Biomacromolecules 10:197–209
Shum P, Kim JM, Thompson DH (2001) Phototriggering of liposomal drug delivery systems. Adv Drug Deliv Rev 53:273–284
Paasonen L, Sipilä T, Subrizi A, Laurinmäki P, Butcher SJ, Rappolt M, Yaghmur A, Urtti A, Yliperttula M (2010) Gold-embedded photosensitive liposomes for drug delivery: triggering mechanism and intracellular release. J Control Release 147:136–143
Peiris PM, Toy R, Abramowski A, Vicente P, Tucci S, Bauer L, Mayer A, Tam M, Doolittle E, Pansky J, Tran E, Lin D, Schiemann WP, Ghaghada KB, Griswold MA, Karathanasis E (2014) Treatment of cancer micrometastasis using a multicomponent chain-like nanoparticle. J Control Release 173:51–58
Marsh JN, Senpan A, Hu G, Scott MJ, Gaffney PJ, Wickline SA, Lanza GM (2007) Fibrin-targeted perfluorocarbon nanoparticles for targeted thrombolysis. Nanomedicine (Lond) 2:533–543
Korin N, Kanapathipillai M, Matthews BD, Crescente M, Brill A, Mammoto T, Ghosh K, Jurek S, Bencherif SA, Bhatta D, Coskun AU, Feldman CL, Wagner DD, Ingber DE (2012) Shear-activated nanotherapeutics for drug targeting to obstructed blood vessels. Science 337:738–742
Holme MN, Fedotenko IA, Abegg D, Althaus J, Babel L, Favarger F, Reiter R, Tanasescu R, Zaffalon PL, Ziegler A, Müller B, Saxer T, Zumbuehl A (2012) Shear-stress sensitive lenticular vesicles for targeted drug delivery. Nat Nanotechnol 7:536–543
Modery-Pawlowski CL, Sen Gupta A (2014) Heteromultivalent ligand-decoration for actively targeted nanomedicine. Biomaterials 35:2568–2579
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer Science+Business Media New York
About this protocol
Cite this protocol
Sen Gupta, A. (2016). Cardiovascular Nanomedicine: Materials and Technologies. In: Lu, ZR., Sakuma, S. (eds) Nanomaterials in Pharmacology. Methods in Pharmacology and Toxicology. Humana Press, New York, NY. https://doi.org/10.1007/978-1-4939-3121-7_13
Download citation
DOI: https://doi.org/10.1007/978-1-4939-3121-7_13
Publisher Name: Humana Press, New York, NY
Print ISBN: 978-1-4939-3120-0
Online ISBN: 978-1-4939-3121-7
eBook Packages: Springer Protocols