Abstract
Addiction to drugs of abuse is a debilitating chronic disease, for which long-term treatment success rates are low. Because of the human and financial cost of addiction, considerable effort is dedicated toward understanding the processes that initiate and sustain substance abuse disorders. Among these processes, growing evidence indicates an integral contribution of glial cells, including astrocytes, oligodendrocytes, and microglia. For example, decreased white matter content and integrity in the prefrontal cortex is correlated with impaired prefrontal cognitive control, a cardinal feature of addiction pathology. In addition, decreased astroglial plasma membrane glutamate transport in the nucleus accumbens is a critical mediator of seeking for multiple classes of drugs of abuse. The following chapter introduces addiction neurocircuitry, and goes on to describe drug-dependent changes in glial cells that have been identified within this circuitry. Special emphasis is given to drug-induced impairments in the physiological relationships between neurons and glia. Lastly, evidence for the therapeutic potential of glial-specific targets is discussed.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
17.1 Introduction: The Neurocircuitry and Cell Biology of Addiction
Despite the fact that glial cells outnumber neurons in the brain, they have historically been largely considered as a secondary source of trophic support to neurons (Barres 2008) . Over the past several years, however, seminal roles for neuron-glial interactions in nervous system function have become increasingly clear. There is now extensive evidence for a functional relationshipbetween neurons and glia in a wide variety of nervous system processes, including development, synaptic plasticity, injury response, vascular function, sleep, and others (Chung and Barres 2012; Parpura et al. 2012) . As discussed in detail in this edition, there is also a considerable and growing body of data that indicate important roles for glial cells in pathological processes, representing a target of intervention for conditions among epilepsy , encephalopathy, cancer, neurodegenerative diseases , and psychiatric conditions (Parpura et al. 2012) .
Among the psychiatric conditions in which glial dysfunction is implicated is addiction to drugs of abuse (Haydon et al. 2009; Cooper et al. 2012) . Drug-induced changes in morphology, content, and function of glial cells have been shown at the levels of functional magnetic resonance imaging and molecular and cellular physiology in both human addicts and in preclinical animals models, and in response to drugs across chemical categories including psychostimulants, opiates, nicotine, and ethanol. In advance of an in depth discussion of the drug-induced changes in gliobiology, it is worthwhile to consider the neurocircuitry engaged by the rewarding and pathological actions of drugs abuse. This circuitry provides the framework of brain nuclei where drug-related adaptations have been observed.
Cellular effects of drugs of abuse have been thoroughly described in brain regions within reward centers of the brain, supporting the hypothesis that addiction is a disease of reward learning and associations (Hyman et al. 2006; Lalumiere and Kalivas 2007; Mameli and Luscher 2011) . Acute reinforcing effects of many drugs of abuse are mediated by robust release of dopamine (DA) from the ventral tegmental area (VTA) onto structures of the mesocorticolimbic system, including prefrontal cortex (PFC), nucleus accumbens (NAc), dorsal striatum, amygdala, and hippocampus (17.1) (Di Chiara and Imperato 1988; Koob and Nestler 1997; Martinez and Narendran 2010) . Similarly, DA release also occurs in association with natural rewards, and constitutes an important mechanism of association between salience and environment or adaptive behaviors. However, in contrast to drug-induced DA signaling, DA responsiveness declines following multiple exposures to natural rewards, and it is the repeated release of dopamine that commandeers the normally adaptive process of reward learning (Lalumiere and Kalivas 2007) .
The intensity and mechanisms of DA release varies depending on the addictive drug, but nonetheless represents a common theme of reinforcement. Following multiple exposures, changes in cellular physiology, morphology , and gene expression patterns are observed within the DA-ergic axon terminal fields. Thus, the hyperdopaminergic state induced by chronic drug exposures leads to long-term changes in the cells of the VTA and in those receiving innervation from the VTA, as well as in synaptic connections downstream, in particular in the glutamatergic projection from the PFC to the NAc (Fig. 17.1) (Kalivas et al. 2005; Mameli et al. 2009; Mameli and Luscher 2011) . Thus, it is generally believed that understanding the long term cellular changes induced within the mesocorticolimbic reward pathways depicted in Fig. 17.1 by chronic exposure to drugs of abuse will not only inform understanding of the fundamental biology of adaptive and maladaptive reward learning, but will also illuminate candidate targets for pharmacotherapies for addiction .
Reward neurocircuitry engaged by chronic drug abuse. AMY, amygdala; DS, dorsal striatum HIPP, hippocampus; NAc, nucleus accumbens; PFC, prefrontal cortex; VP, ventral pallidum; VTA, ventral tegmental area (VTA). Dopaminergic projections from the VTA are depicted by a heavy line. Glutamatergic and γ-aminobutyric acid (GABA)ergic projections, the latter from the NAc to VP, are depicted by thin lines. (For additional information, see (Feltenstein and See 2008; Koob and Volkow 2010; McGinty et al. 2011; Reissner and Kalivas 2013))
A growing appreciation of enduring changes in cellular dynamics within the reward circuitry following chronic drug exposure has fueled the belief that cellular targets of addiction may lie within deficits in executing goal-directed behaviors (Nestler and Aghajanian 1997; Chen et al. 2010; Kalivas and Volkow 2011; Van den Oever et al. 2012) . The appreciation has contributed to a growing shift in the understanding and treatment of addiction as a chronic disease based on cellular pathology following protracted drug abuse (Leshner 1997; Dackis and O’Brien 2005; Chandler et al. 2009; Courtwright 2012) . This shift has in turn fueled study of the relationship between drug-dependent cellular adaptations and addiction-related behaviors. Accordingly, within the last 10 years, changes in glial content, structure, and function have been revealed. The following sections provide an overview of studies from human and preclinical animal models and across levels of analysis from whole brain imaging to cell biology and electrophysiology.
17.2 Astroglial Expression of Receptors and Transporters
In considering the effects of drugs of abuse on glial cells, and on glial contributions to mechanisms of addiction, it is important to appreciate to what degree relevant classes of receptors and transporters are expressed on these cells within the brain reward circuitry. Because the relationship between astrocytes and neurons are the most thoroughly studied in this context, astrocytes will be the predominant glial cell type considered in this section. It has for some time been appreciated that receptors for many transmitter systems are expressed on astrocytes, including glutamate, γ-aminobutyric acid (GABA), serotonin, opioids, purines, and others (Porter and McCarthy 1997; Abbracchio et al. 2006; Shigetomi et al. 2012) . More recently, receptor expression has also been demonstrated for endocannabinoid CB1 receptors, and stimulation of astroglial CB1 receptors by neuronal endocannabinoid release leads to synaptic potentiation via astroglial-derived glutamate transmission (Navarrete and Araque 2008, 2010) . Of particular relevance to this chapter, recent evidence has accumulated showing expression of multiple types of DA receptors in a range of glial cell types in vivo, particularly astrocytes. For example, DA receptors of the subtypes D1, D3–5 (Miyazaki et al. 2004) and D2 (Khan et al. 2001; Shao et al. 2013) have been reported.
Astrocytes also express a wide range of plasma membrane transporters for amino acids, nucleosides, glucose, monocarboxylates, GABA, monoamines, and more (Morgello et al. 1995; Inazu et al. 2003; Pierre and Pellerin 2005; Nagasawa et al. 2007; Fuente-Martin et al. 2012; Kittel-Schneider et al. 2012) . Although astroglial expression of DA transporters has been found in some cases (Takeda et al. 2002; Karakaya et al. 2007), but not others (Dahlin et al. 2007; Kittel-Schneider et al. 2012) , functional uptake of both DA and serotonin in astrocytes has been reported (Kimelberg and Katz 1985; Hirst et al. 1998; Inazu et al. 1999) . Of relevance to this chapter, expression of glutamate transporters on astrocytes has been demonstrated to be of particular importance for protection against excitotoxicity and in maintaining fidelity in synaptic communication. Greater than 90 % of glutamate uptake occurs via high affinity glutamate transporters expressed on astrocytes (Anderson and Swanson 2000; Danbolt 2001) . A deficit in astroglial glutamate uptake has been widely reported following exposure to multiple drugs of abuse, and is discussed in greater detail below.
Functionality of astroglial G protein-linked receptors has also been well described (Bradley and Challiss 2012) . Considerable evidence both in vitro and in vivo indicates that neurotransmitters released from neurons (as well as neuromodulators and hormones) can stimulate astroglial receptors, leading to a Ca2+ signal which triggers release of gliotransmitters and in turn evoked Ca2+ signals in neurons (Bezzi and Volterra 2001; Agulhon et al. 2008; Lu et al. 2009; Zorec et al. 2012) , as well as local and long-distance Ca2+ waves that are propagated through networks of astrocytes via gap junctions (Goldberg et al. 2010) . In vivo, sensory stimulation to a mouse whisker leads to an astroglial Ca2+ response that is dependent upon metabotropic glutamate receptors (mGluRs) (Wang et al. 2006; Halassa and Haydon 2010) .
Signaling from neurons to astrocytes also leads to reciprocal modulation of synaptic and neuronal function by astrocytes themselves (Lu et al. 2009) . This bidirectional nature of communication between neurons and astrocytes and its role in shaping synaptic function has led to the concept of the tripartite synapse (Araque et al. 1999) , which is further supported by electron microscopy and reconstruction studies illustrating the intimate and intricate physical relationship between neurons and astrocytes (Genoud et al. 2006; Witcher et al. 2007; Belanger et al. 2011) .
Because changes in synaptic strength and signaling within the reward neurocircuitry have been heavily implicated in the cellular pathophysiology of addiction , in particular to cocaine (Stuber et al. 2010; Luscher and Malenka 2011) , the morphological and functional relationships between neurons and astrocytes indicate the potential for involvement of astrocytes in mechanisms of drug dependence. Accordingly, the following sections will in more detail discuss evidence for drug-dependent changes in glial cell biology in both human addicts and animal models of addiction, with consideration for how these changes relate to changes in synaptic function.
17.3 Effects of Drug Administration on White Matter Volume and Glial Content
Human brain imaging studies have revealed a great deal of information about neural differences between drug-dependent individuals and healthy, abstinent controls, particularly within regions of the PFC (Goldstein and Volkow 2011) . Brain matter is largely characterized as white and gray matter; white matter is primarily comprised of glial cells and myelinated axons, in contrast to neuronal cell bodies, which are the major constituent of gray matter (Fowler et al. 2007) . Many studies have documented deficits in both volume of both white and gray matter, as well as in metabolic activity in the PFC, of human drug abusers (for review see (Fowler et al. 2007)) .
For example, a number of studies have revealed significant differences in white matter content between drug addicts and healthy controls (Schlaepfer et al. 2006) . Further, while frontal and temporal white matter volume in humans continues to increase until the mid-40s, compared to normal control subjects, cocaine dependent subjects do not exhibit an age-dependent increase in white matter volume (Bartzokis et al. 2002) . Relatedly, deficits in frontal white matter integrity also appear with chronic drug abuse (Lim et al. 2002, 2008) . Integrity is a measure revealed by techniques including diffusion tensor imaging, which quantifies directional diffusion of molecules along a fiber tract, providing an indicator of fiber structure and connectivity (Le Bihan et al. 2001) . White matter integrity across the brain is significantly correlated with treatment outcome for cocaine dependence (Xu et al. 2010) ; relatedly, frontal lobe white matter integrity at the start of treatment is a predictor of alcohol relapse 6 months later (Sorg et al. 2012) . Collectively, these studies indicate that structural deficits in white matter, composed largely of glia , correlate with cortical structural deficits in addicted individuals.
Other studies have reported decreased gray matter measured in a variety of brain regions within cocaine-dependent subjects (Bartzokis et al. 2000; Franklin et al. 2002; Sim et al. 2007) . Prolonged cocaine abuse has been postulated to represent an accelerated aging process with respect to reduction in gray matter volume (Bartzokis et al. 2000; Ersche et al. 2013) . Indeed, the rate of loss of cortical and subcortical gray matter volume in cocaine-dependent subjects is almost twice that of healthy age-matched subjects (Ersche et al. 2013) and accelerated age-dependent loss of gray and white matter has also been reported in chronic alcoholics (Pfefferbaum et al. 1992) .
What is the implication of a prefrontal white matter deficit? Deficient prefrontal cognitive control is a hallmark feature of addiction (Goldstein and Volkow 2002; Kalivas and Volkow 2005; George and Koob 2010) . Impairments of this nature are correlated with increased measures of impulsivity and loss of executive control; for example, decreased frontal and parietal cortex white matter integrity of cocaine-dependent subjects correlates with impaired performs on the Iowa Gambling Task, suggesting that white matter integrity may well be functionally related to functional impairments in decision making (Lane et al. 2010) . However, it is difficult using human studies to dissociate correlation with causation in the relationship between white matter content and integrity with impaired executive function. Furthermore, in all human imaging studies, changes identified between drug-dependent and healthy controls cannot be differentiated between drug-related changes and pre-existing difference which might serve a correlative or causative relationship. As such, preclinical animal models serve a valuable function to allow comparison between naïve baseline and changes which develop with drug experience. Moreover, human studies are confounded by complexity of single drug versus polydrug abusers, length and severity of drug abuse, and other environmental factors and individual differences. These confounds underscore the importance of animal models in understanding the cellular mechanisms responsible for addiction-related behaviors.
In a more limited scope of studies, these principles have been recapitulated in preclinical animal models. For example, diffusion tensor imaging of chronic cocaine treated rats has revealed a significant decrease in white matter integrity of the corpus callosum compared to saline controls; a decrease in myelin-associated protein in the same region was also observed (Narayana et al. 2009) . In a separate study, rats trained to self-administer cocaine demonstrated impairment in a working memory task, which was correlated with decreased counts of both neurons and oligodendrocytes in the PFC (George et al. 2008) . Moreover, drug seeking by rats trained to self-administer cocaine who choose drug seeking despite an adverse consequence (foot shock) was reversed by stimulation of prefrontal cortical activity (Chen et al. 2013) , providing an analog of the hypofrontality observed in human addicts. Future studies will be necessary to further ascertain the relationship between drug abuse, white matter content, and compulsive drug seeking. If then, chronic drug use leads to deficiencies in white and/or gray matter, it becomes important to understand the cellular mechanism(s) by which this may occur, and whether targeting these mechanisms may represent a means of treatment intervention for addiction.
17.4 Effects of Drug Administration on Properties of Astrocytes
17.4.1 Astroglial Inflammation
While functional imaging studies provide important insight into changes at the level of circuitry and anatomy, changes in expression and function of specific proteins provides additional information on glial consequences of drug exposure . A number of studies in preclinical animal models of drug abuse and addiction have demonstrated increased measures for astrocyte activation. For example, increased glial fibrillary acidic protein (GFAP) expression within the reward neurocircuitry has been observed following exposure to cocaine (Fattore et al. 2002; Bowers and Kalivas 2003) , methamphetamine (Guilarte et al. 2003; Friend and Keefe 2013) , morphine (Beitner-Johnson et al. 1993; Song and Zhao 2001) , and alcohol (Fletcher and Shain 1993; Goodlett et al. 1993; Franke 1995; Tagliaferro et al. 2002; Vongvatcharanon et al. 2010) . Increased GFAP expression is a hallmark feature of inflammation (or activation) of astrocytes (Pekny and Nilsson 2005; Sofroniew 2009; Sofroniew and Vinters 2010) and hence may reflect enduring cellular inflammation initiated by drug exposure. In some cases, however, long-term alcohol exposure has also been associated with a decline in GFAP expression and astrocyte complexity (Franke 1995; Rintala et al. 2001) . Detailed histological analysis on postmortem alcoholic human brains have revealed enlarged cell bodies but also patch-like losses in GFAP-positive cells (Cullen and Halliday 1994; Miguel-Hidalgo 2005) , indicating a complexity of cellular effects. Nonetheless, many studies have revealed that exposure to drugs of abuse leads to glial inflammation and activation of innate immune response (for reviews see (Watkins et al. 2005, 2009; Crews et al. 2011)) .
17.4.2 Blood-Brain Barrier Integrity
Psychostimulant abuse has also been well documented to lead to breakdown of the blood brain barrier (BBB) (Kousik et al. 2012) . The BBB is a physical barrier to the central nervous system (CNS) formed by brain endothelial cells interacting with pericytes, basement membrane of the vasculature, and astrocytes (Banerjee and Bhat 2007; Abbott et al. 2010; Krueger and Bechmann 2010; Kousik et al. 2012) . The tight association of astrocyte end-feet with vasculature is a critical component, and astroglial inflammation can lead to perturbation of BBB integrity. Permeability of the BBB for any reason leads to vulnerability to CNS exposure to a variety of chemical and biological insults, from which it is normally protected. A good example is the fact that mounting evidence indicates increased vulnerability of the nervous system to HIV infection in psychostimulant abusers (Rippeth et al. 2004; Buch et al. 2012) . HIV infection within the brain in turn leads to an increased incidence of neuro-AIDS, a condition characterized by generalized neurologic deficits secondary to HIV infection (Buch et al. 2012; Hauser et al. 2012) . The abuse of psychstimulants such as cocaine and methamphetamine leads to glial inflammation and permeability of the BBB, enhanced vulnerability to HIV infection and other opportunistic viruses and pathogens.
17.4.3 Astroglial Glutamate Transport: A Critical Mediator of Drug Seeking
Among the most widely reported astroglial changes following self-administration of drugs of abuse is downregulation of the high affinity glutamate transporter EAAT2/GLT-1 (Reissner and Kalivas 2010) . Downregulation of GLT-1 is frequently associated with activated astrocytes, particularly following injury (Binns et al. 2005; Pekny and Nilsson 2005; Cata et al. 2006; Tawfik et al. 2008) . GLT-1 is downregulated in the NAc following self-administration and withdrawal from cocaine (Knackstedt et al. 2010; Fischer-Smith et al. 2012) , nicotine (Gipson et al. 2013) , and heroin (Shen et al. personal communication). Results following alcohol exposure are more complex; however, in one study 24 h after 7 days alcohol exposure, higher basal extracellular glutamate levels and corresponding decrease in glutamate uptake was reported in the NAc (Melendez et al. 2005) , which is consistent with other studies reporting chronic increases in basal extracellular glutamate levels (Mann et al. 2008) . Moreover, chronic self-administration in alcohol-preferring rats results in decreased GLT-1 protein levels in the NAc; treatment with ceftriaxone reversed this decreased, as well as measures of alcohol seeking in alcohol-preferring rats (Qrunfleh et al. 2013; Sari et al. 2013) .
GLT-1/EAAT2 is a member of the EAAT family of high affinity glutamate transporters (Danbolt 2001), and rapid glutamate uptake is important for the tight regulation of synaptic glutamate concentrations and the prevention of synaptic excitotoxicity (Danbolt 2001; Jiang and Amara 2011) . In addition, impaired clearance of glutamate from the synaptic cleft can impact decay currents of ionotropic glutamate receptors, indicating that at sub-excitotoxic levels, changes in glutamate concentrations resulting from altered transporter function can shape neuronal currents (Tzingounis and Wadiche 2007) . Importantly, restored expression of GLT-1 is associated with decreased measures of cocaine seeking (Baker et al. 2003; Knackstedt et al. 2010; Reissner et al. 2013) .
Interestingly, besides following drug abuse, EAAT2/GLT-1 levels and transporter-dependent glutamate uptake are also decreased in aged rodent brains (Wheeler and Ondo 1986; Najlerahim et al. 1990; Saransaari and Oja 1995; Vatassery et al. 1998; Potier et al. 2010) as well as in aged brains in a transgenic mouse model of Huntington’s Disease (Behrens et al. 2002) and in postmortem brains from Alzheimer’s Disease (AD) patients (Masliah et al. 1996; Jacob et al. 2007; Simpson et al. 2010; Woltjer et al. 2010) . Moreover, heterozygous-deficient GLT-1 (+/−) mice crossed with a double transgenic AD model mouse demonstrated an earlier onset of memory deficits compared with the AD model mouse with a wild-type GLT-1 genotype (Mookherjee et al. 2011) . These findings collectively indicate that impaired GLT-1 expression and function may contribute to age-dependent synaptic and cognitive impairment, and is supportive of the idea that cocaine-dependent changes may accelerate the aging process (Ersche et al. 2013) .
While synaptic glutamate levels are predominantly controlled by GLT-1, basal extracellular glutamate levels are correspondingly largely controlled by the action of the cystine-glutamate exchanger, system xc− (Baker et al. 2002a, 2002b) . System xc− is composed of a small, catalytic subunit, xCT, and a large subunit, NF2 (Lim and Donaldson 2011; Lewerenz et al. 2013) . While some neuronal expression of system xc− has been reported, it is predominantly astroglial. Hence, extracellular glutamate levels are controlled by release of glutamate via system xc− , and uptake by EAATs (largely GLT-1 in adult rodents). Interestingly, while expression of both xCT and GLT-1 are decreased following cocaine self-administration and extinction training (Knackstedt et al. 2010) , net basal extracellular glutamate levels are decreased, indicating that expression of xc− may be the more dominant toward controlling basal extracellular levels measured via microdialysis (Baker et al. 2003) . This has led to a model in which basal levels are decreased by suppressed xCT, but synaptic levels are increased following glutamate release, due to the compromised synaptic uptake cause by impaired GLT-1 function and expression (Fig. 17.2) (McFarland et al. 2003) .
Cystine/glutamate exchange and glutamate uptake regulate synaptic and extrasynaptic glutamate levels. Both the glutamate transporter GLT-1 and glutamate exchanger catalytic subunit xCT are reduced following chronic self-administration and extinction from cocaine. Ca2+-dependent glutamate release from astrocytes is also documented, although cystine/glutamate (Cys/Glu)exchange is the primary source (Baker et al. 2002a; Haydon et al. 2009). Synaptic glutamate levels (1) are tightly controlled within the sub-micromolar range at rest (during synaptic transmission glutamate can raise to ~ 1.1 mM), whereas extrasynaptic levels (2) can approach the 20 µM range. Reduced expression of xCT will lead to decreased basal extrasynaptic levels, and hence reduced tone of presynaptic inhibitory mGluR2/3 receptors. This leads to increased glutamate release (and hence, synaptic levels) within the NAc during cocaine seeking, which is exacerbated by reduced GLT-1 expression. Inotropic glutamate, AMPA (α-amino-3-hydroxy-5-methyl-isoxazole propionate) and NMDA, receptors are shown. (Figure reproduced with permission from (Moussawi et al. 2011))
A consequent dysregulation of synaptic and extrasynaptic glutamate levels following suppression of xCT and GLT-1 has considerable consequences on cellular function (Kalivas 2009) . Decreased basal levels of extracellular glutamate (due to decreased xCT) lead to decreased tone on presynaptic inhibitory mGluR2/3 receptors, which results in increased glutamatergic transmission. Activity of glutamatergic PFC innervation of medium spiny neurons of the NAc is a driving force of reinstatement to numerous drugs of abuse, and pharmacological agonism of these presynaptic mGluR2/3 receptors (or antagonism of postsynaptic excitatory glutamate receptors) can block reinstatement (Moussawi and Kalivas 2010; Reissner and Kalivas 2010) . Hence, the decreased expression of xCT and GLT-1 leads to a combinatorial effect on the cellular controls designed to regulate synaptic input to the NAc.
Extracellular glutamate levels appear not only to mediate tone on neuronal receptors, but can also stimulate Ca2+ oscillations in astrocytes via stimulation of mGluR receptors, as discussed in the preceding section. This Ca2+-dependent glutamate transmission from astrocytes leads to N-methyl D-aspartate receptors (NMDARs)-mediated slow inward currents (SICs) on medium spiny neurons in the NAc (D’Ascenzo et al. 2007) . What is the behavioral consequence of changes in glutamate transmission from astrocytes? One clue comes from transgenic mice engineered to express a dominant negative vesicle protein in astrocytes; these mice demonstrate impaired cocaine-induced reinstatement of conditioned place preference, as well as cue-induced reinstatement in a self-administration paradigm (Turner et al. 2013) . These findings are consistent with a model in which glutamatergic gliotransmission may mediate the cellular pathology of addiction. However, more studies will be required to fully understand the consequences of impairments of gliotransmission following drug abuse.
17.5 Beyond Astrocytes: Effects of Drug Administration on Oligodendrocytes and Microglia
In addition to cellular adaptations within astrocytes, drug-dependent changes in oligodendrocytes and microglia have been reported. Withdrawal from chronic cocaine administration is associated with decreased expression of white matter proteins in the NAc including myelin basic protein, proteolipid protein (PLP), myelin oligodendrocyte glycoprotein, and myelin associated glycoprotein, which is prevented by treatment with the β-lactam antibiotic ceftriaxone (Kovalevich et al. 2012) . As mentioned above, ceftriaxone is a known inducer of GLT-1 expression (Rothstein et al. 2005) , and is effective at preventing reinstatement of cocaine (Sari et al. 2009; Knackstedt et al. 2010; Fischer et al. 2013) . Interestingly, postmortem gene expression profiling in NAc tissue from human addicts has revealed a decrease in mRNA coding for myelin-associated proteins, including myelin basic protein and PLP1 (Albertson et al. 2004; Bannon et al. 2005) . In a separate study, a decrease in PLP1 was confirmed by in situ hybridization in the ventral caudate, putamen, and internal capsule of postmortem tissue from human cocaine abusers (Kristiansen et al. 2009) .
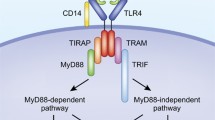
As stated in the preceding section, it is well documented that activation of glial cells occurs in response to opioid exposure. However, in contrast to the analgesic effects of opioids that are mediated through opioid receptors, activation of glial cells appears to occur via toll-like receptors (TLRs) and mediate nonanalgesic effects of opioids (Hutchinson et al. 2011) . TLRs are microbe receptors expressed on immune cells, named for homology to the Drosophila Toll protein (Anderson et al. 1985; Lemaitre et al. 1996) . The signaling of TLRs is a critical component in activating an immune response (Hanke and Kielian 2011) . Within the CNS, TLRs are expressed predominantly on microglia, but are found on activated astrocytes as well, and on oligodendrocytes and neurons to a lesser degree (Hanke and Kielian 2011) . TLR4 serves as the receptor for lipopolysaccharide, which has allowed for elucidation of a complex downstream signaling cascade leading to increased transcriptional regulation by nuclear factor kappa-light-chain-enhancer of activated B cells (Kawai and Akira 2006) . Activation of the TLR4 receptor in response to opioid exposure in vivo opposes the analgesic effects and is responsible for opioid-induced hyperalgesia, or hypersensitivity to pain that often occurs after long term opioid use and abuse and in fact oppose the analgesic effects mediated through opioid receptor (Ossipov et al. 2005; Buchanan et al. 2010) . Effects of opioid versus TLR actions can be dissociated using (−) and (+) stereoisomers of opioid agonists and antagonists; while TLRs are nonstereoselective, opioid receptors only bind to (−)-isomers. Genetic deletion or pharmacological inhibition of TLR4 receptors with (+)-naloxone impair opioid-induced CPP and reduce opioid self-administration (Hutchinson et al. 2012) .
17.6 Modulation of Neuronal Cell Biology by Glial-derived Factors
17.6.1 GDNF, A Negative Regulator of Drug Reward
In the preceding section, we introduced the concept of glutamatergic gliotransmission, and how the regulation of glutamate release and uptake by astrocytes may contribute to disruptions in glutamate homeostasis and drug-induced cellular pathologies (Cali et al. 2009) . Importantly, glial cells and in particular astrocytes secrete many proteins and molecules in addition to glutamate which may also be adaptive or inflammatory in response to a protracted drug history. For example, glial cell line-derived neurotrophic factor (GDNF) is a member of the transforming growth factor-βfamily of growth factors that, despite its glio-centric name, is expressed in a variety of cell types including astrocytes, microglia , and neurons (Schaar et al. 1993; Pochon et al. 1997) . GDNF is predominantly expressed within the basal forebrain, substantia nigra, and striatum, and was initially isolated on the basis of its ability as a component of astrocytes to selectively protect DA neurons of the substantia nigra in culture (O’Malley et al. 1992; Schaar et al. 1993; Duarte et al. 2012) . A number of studies collectively indicate that GDNF action opposes drug taking, as well as the effects of chronic exposure on seeking of multiple drugs of abuse (Pierce and Bari 2001; Carnicella and Ron 2009; Ghitza et al. 2010) . However, manipulation of GDNF expression and activity in the VTA promotes the incubation of cocaine craving (Lu et al. 2009) but not heroin craving (Airavaara et al. 2011) , indicating the different roles may exist in difference brain regions and at different times following drug exposure.
17.6.2 Gliotransmitters: Beyond Glutamate
D-serine is a naturally occurring amino acid transmitter mainly released by astrocytes (and neurons in some brain regions), and is a co-agonist for NMDA receptors (Ben Achour and Pascual 2012; Radzishevsky et al. 2013) . Stimulation of NMDARs by D-serine is necessary for hippocampal NMDA-dependent long-term potentiation. Relatedly, D-cycloserine (DCS) is a broad spectrum antibiotic and partial agonist at the glycine site of NMDA receptors, with functions as a cognitive enhancer and anticonvulsant (Ohno and Watanabe 1996; Wlaz et al. 1996; Myers and Carlezon 2012) , and is under investigation as a treatment for substance use disorder (Olive et al. 2012) .
A growing body of evidence suggests that administration of either D-serine or DCS may reduce drug seeking. Reduced D-Serine levels are observed in the NAc following cocaine administration (Curcio et al. 2013) . Further, perfusion of D-Serine in the bath of NAc core slice electrophysiology restored the ability to induce long-term potentiation and depression. Relatedly, microinjection of D-Serine in the NAc blocked behavioral sensitization to cocaine . D-Serine administered systemically prior to or immediately after extinction training sessions significantly reduces the reinstatement of cocaine seeking (Kelamangalath and Wagner 2010) . Similarly, systemic administration of D-serine or DCS blocks expression of cocaine conditioned place preference (CPP) (Yang et al. 2013). DCS facilitates extinction of cocaine CPP (Botreau et al. 2006) . Moreover, the effect of DCS can be long-lasting and reduce reinstatement of the CPP behavior (Paolone et al. 2009; Thanos et al. 2009) . A Phase 2, “D-Serine for Cocaine Dependence Pilot” clinical study is currently underway (http://www.clinical trials.gov NCT01715051).
Besides glutamate and D-Serine, ATP is an additional gliotransmitter released by astrocytes. Extracellular adenosine is largely derived from astroglial ATP, acting on neuronal adenosine receptors. Evidence exists for a role of adenosine receptors, in particular A2A receptors, in the rewarding effects of drugs of abuse, and in reinstatement to drug seeking (Soria et al. 2006; Brown et al. 2009; O’Neill et al. 2012) .
17.7 Glial Cells: An Emerging Pharmacotherapeutic Target for Addiction
The study described above illustrates the potential for astrocyte-derived D-serine as pharmacotherapy for substance abuse disorder. D-serine is one of a number of examples of therapies based in glial cell biology, and adaptions in neuron-glial signaling (Cooper et al. 2012) . For example, as stated previously, at least three compounds known to induce expression of GLT-1 are also under investigation as addiction therapies. N-acetylcysteine, ceftriaxone, and propentofylline are all compounds of separate classes which upregulate GLT-1, and suppress reinstatement to cocaine (Baker et al. 2003; Sari et al. 2009; Knackstedt et al. 2010; Reissner et al. 2014) . Human clinical trials indicate safety and efficacy of N-acetylcysteine against drug use for nicotine, cocaine, and cannabis (LaRowe et al. 2007, 2013; Knackstedt et al. 2009; Gray et al. 2012; Berk et al. 2013) . Further, the restored expression of GLT-1 is necessary in order for propentofylline to effectively block reinstatement to cocaine (Reissner et al. 2014) . Thus, while the field of gliobiology in drug abuse is in a relatively early stage, credible evidence already exists to support the hypothesis that targeting glial physiology affects neuronal cell biology and drug craving.
17.8 Conclusions and Perspectives
There is no question that both acute and chronic exposure to drugs of abuse leads to changes in astrocytes, oligodendrocytes , and microglia, within regions heavily implicated in reward neurocircuitry. However, our understanding of the effects of drug-dependent changes in glial structure and activity is at an early stage. Important questions remain to be addressed, such as: what are the relationships between changes in expression of myelin-related genes, deficits in white matter volume and integrity, and compulsive drug seeking? What are the relationships between glial inflammation and changes in white matter content, or between drug-dependent changes in astrocyte physiology and neuronal synaptic communication? These questions will be central toward future progress in understanding and treating addiction as a brain disease.
References
Abbott NJ, Patabendige AA, Dolman DE, Yusof SR, Begley DJ (2010) Structure and function of the blood-brain barrier. Neurobiol Dis 37:13–25
Abbracchio MP, Burnstock G, Boeynaems JM, Barnard EA, Boyer JL, Kennedy C, Knight GE, Fumagalli M, Gachet C, Jacobson KA, Weisman GA (2006) International union of pharmacology LVIII: update on the P2Y G protein-coupled nucleotide receptors: from molecular mechanisms and pathophysiology to therapy. Pharmacol Rev 58:281–341
Agulhon C, Petravicz J, McMullen AB, Sweger EJ, Minton SK, Taves SR, Casper KB, Fiacco TA, McCarthy KD (2008) What is the role of astrocyte calcium in neurophysiology? Neuron 59:932–946
Airavaara M, Pickens CL, Stern AL, Wihbey KA, Harvey BK, Bossert JM, Liu QR, Hoffer BJ, Shaham Y (2011) Endogenous GDNF in ventral tegmental area and nucleus accumbens does not play a role in the incubation of heroin craving. Addict Biol 16:261–272
Albertson DN, Pruetz B, Schmidt CJ, Kuhn DM, Kapatos G, Bannon MJ (2004) Gene expression profile of the nucleus accumbens of human cocaine abusers: evidence for dysregulation of myelin. J Neurochem 88:1211–1219
Anderson CM, Swanson RA (2000) Astrocyte glutamate transport: review of properties, regulation, and physiological functions. Glia 32:1–14
Anderson KV, Bokla L, Nusslein-Volhard C (1985) Establishment of dorsal-ventral polarity in the drosophila embryo: the induction of polarity by the toll gene product. Cell 42:791–798
Araque A, Parpura V, Sanzgiri RP, Haydon PG (1999) Tripartite synapses: glia, the unacknowledged partner. Trends Neurosci 22:208–215
Baker DA, Shen H, Kalivas PW (2002a) Cystine/glutamate exchange serves as the source for extracellular glutamate: modifications by repeated cocaine administration. Amino acids 23:161–162
Baker DA, Xi ZX, Shen H, Swanson CJ, Kalivas PW (2002b) The origin and neuronal function of in vivo nonsynaptic glutamate. J Neurosci 22:9134–9141
Baker DA, McFarland K, Lake RW, Shen H, Tang XC, Toda S, Kalivas PW (2003) Neuroadaptations in cystine-glutamate exchange underlie cocaine relapse. Nat Neurosci 6:743–749
Banerjee S, Bhat MA (2007) Neuron-glial interactions in blood-brain barrier formation. Ann Rev Neurosci 30:235–258
Bannon M, Kapatos G, Albertson D (2005) Gene expression profiling in the brains of human cocaine abusers. Addict Biol 10:119–126
Barres BA (2008) The mystery and magic of glia: a perspective on their roles in health and disease. Neuron 60:430–440
Bartzokis G, Beckson M, Lu PH, Edwards N, Rapoport R, Wiseman E, Bridge P (2000) Age-related brain volume reductions in amphetamine and cocaine addicts and normal controls: implications for addiction research. Psychiatry Res 98:93–102
Bartzokis G, Beckson M, Lu PH, Edwards N, Bridge P, Mintz J (2002) Brain maturation may be arrested in chronic cocaine addicts. Biol Psychiatry 51:605–611
Behrens PF, Franz P, Woodman B, Lindenberg KS, Landwehrmeyer GB (2002) Impaired glutamate transport and glutamate-glutamine cycling: downstream effects of the Huntington mutation. Brain 125:1908–1922
Beitner-Johnson D, Guitart X, Nestler EJ (1993) Glial fibrillary acidic protein and the mesolimbic dopamine system: regulation by chronic morphine and Lewis-Fischer strain differences in the rat ventral tegmental area. J Neurochem 61:1766–1773
Belanger M, Allaman I, Magistretti PJ (2011) Brain energy metabolism: focus on astrocyte-neuron metabolic cooperation. Cell Metab 14:724–738
Ben Achour S, Pascual O (2012) Astrocyte-neuron communication: functional consequences. Neurochem Res 37:2464–2473
Berk M, Malhi GS, Gray LJ, Dean OM (2013) The promise of N-acetylcysteine in neuropsychiatry. Trends Pharmacol Sci 34:167–177
Bezzi P, Volterra A (2001) A neuron-glia signalling network in the active brain. Curr Opin Neurobiol 11:387–394
Binns BC, Huang Y, Goettl VM, Hackshaw KV, Stephens RL Jr (2005) Glutamate uptake is attenuated in spinal deep dorsal and ventral horn in the rat spinal nerve ligation model. Brain Res 1041:38–47
Botreau F, Paolone G, Stewart J (2006) d-Cycloserine facilitates extinction of a cocaine-induced conditioned place preference. Behav Brain Res 172:173–178
Bowers MS, Kalivas PW (2003) Forebrain astroglial plasticity is induced following withdrawal from repeated cocaine administration. Eur J Neurosci 17:1273–1278
Bradley SJ, Challiss RA (2012) G protein-coupled receptor signalling in astrocytes in health and disease: a focus on metabotropic glutamate receptors. Biochem Pharmacol 84:249–259
Brown RM, Short JL, Cowen MS, Ledent C, Lawrence AJ (2009) A differential role for the adenosine A2A receptor in opiate reinforcement vs opiate-seeking behavior. Neuropsychopharmacology 34:844–856
Buch S, Yao H, Guo M, Mori T, Mathias-Costa B, Singh V, Seth P, Wang J, Su TP (2012) Cocaine and HIV-1 interplay in CNS: cellular and molecular mechanisms. Curr HIV Res 10:425–428
Buchanan MM, Hutchinson M, Watkins LR, Yin H (2010) Toll-like receptor 4 in CNS pathologies. J Neurochem 114:13–27
Cali C, Marchaland J, Spagnuolo P, Gremion J, Bezzi P (2009) Regulated exocytosis from astrocytes physiological and pathological related aspects. Int Rev Neurobiol 85:261–293
Carnicella S, Ron D (2009) GDNF-a potential target to treat addiction. Pharmacol Therap 122:9–18
Cata JP, Weng HR, Chen JH, Dougherty PM (2006) Altered discharges of spinal wide dynamic range neurons and down-regulation of glutamate transporter expression in rats with paclitaxel-induced hyperalgesia. Neuroscience 138:329–338
Chandler RK, Fletcher BW, Volkow ND (2009) Treating drug abuse and addiction in the criminal justice system: improving public health and safety. JAMA 301:183–190
Chen BT, Hopf FW, Bonci A (2010) Synaptic plasticity in the mesolimbic system: therapeutic implications for substance abuse. Ann N Y Acad Sci 1187:129–139
Chen BT, Yau HJ, Hatch C, Kusumoto-Yoshida I, Cho SL, Hopf FW, Bonci A (2013) Rescuing cocaine-induced prefrontal cortex hypoactivity prevents compulsive cocaine seeking. Nature 496:359–362
Chung WS, Barres BA (2012) The role of glial cells in synapse elimination. Curr Opin Neurobiol 22:438–445
Cooper ZD, Jones JD, Comer SD (2012) Glial modulators: a novel pharmacological approach to altering the behavioral effects of abused substances. Expert Opin Investig Drugs 21:169–178
Courtwright DT (2012) Addiction and the science of history. Addiction 107:486–492
Crews FT, Zou J, Qin L (2011) Induction of innate immune genes in brain create the neurobiology of addiction. Brain Behav Immun 25(Suppl 1):S4–S12
Cullen KM, Halliday GM (1994) Chronic alcoholics have substantial glial pathology in the forebrain and diencephalon. Alcohol Alcohol Suppl 2:253–257
Curcio L, Podda MV, Leone L, Piacentini R, Mastrodonato A, Cappelletti P, Sacchi S, Pollegioni L, Grassi C, D’Ascenzo M (2013) Reduced D-serine levels in the nucleus accumbens of cocaine-treated rats hinder the induction of NMDA receptor-dependent synaptic plasticity. Brain 136:1216–1230
D’Ascenzo M, Fellin T, Terunuma M, Revilla-Sanchez R, Meaney DF, Auberson YP, Moss SJ, Haydon PG (2007) mGluR5 stimulates gliotransmission in the nucleus accumbens. Proc Natl Acad Sci U S A 104:1995–2000
Dackis C, O’Brien C (2005) Neurobiology of addiction: treatment and public policy ramifications. Nat Neurosci 8:1431–1436
Dahlin A, Xia L, Kong W, Hevner R, Wang J (2007) Expression and immunolocalization of the plasma membrane monoamine transporter in the brain. Neuroscience 146:1193–1211
Danbolt NC (2001) Glutamate uptake. Prog Neurobiol 65:1–105
Di Chiara G, Imperato A (1988) Drugs abused by humans preferentially increase synaptic dopamine concentrations in the mesolimbic system of freely moving rats. Proc Natl Acad Sci U S A 85:5274–5278
Duarte EP, Curcio M, Canzoniero LM, Duarte CB (2012) Neuroprotection by GDNF in the ischemic brain. Growth Factors 30:242–257
Ersche KD, Jones PS, Williams GB, Robbins TW, Bullmore ET (2013) Cocaine dependence: a fast-track for brain ageing? Mol Psychiatry 18:134–135
Fattore L, Puddu MC, Picciau S, Cappai A, Fratta W, Serra GP, Spiga S (2002) Astroglial in vivo response to cocaine in mouse dentate gyrus: a quantitative and qualitative analysis by confocal microscopy. Neuroscience 110:1–6
Feltenstein MW, See RE (2008) The neurocircuitry of addiction: an overview. Br J Pharmacol 154:261–274
Fischer KD, Houston AC, Rebec GV (2013) Role of the major glutamate transporter GLT1 in nucleus accumbens core versus shell in cue-induced cocaine-seeking behavior. J Neurosci 33:9319–9327
Fischer-Smith KD, Houston AC, Rebec GV (2012) Differential effects of cocaine access and withdrawal on glutamate type 1 transporter expression in rat nucleus accumbens core and shell. Neuroscience 210:333–339
Fletcher TL, Shain W (1993) Ethanol-induced changes in astrocyte gene expression during rat central nervous system development. Alcohol Clin Exp Res 17:993–1001
Fowler JS, Volkow ND, Kassed CA, Chang L (2007) Imaging the addicted human brain. Sci Pract Perspect 3:4–16
Franke H (1995) Influence of chronic alcohol treatment on the GFAP-immunoreactivity in astrocytes of the hippocampus in rats. Acta Histochem 97:263–271
Franklin TR, Acton PD, Maldjian JA, Gray JD, Croft JR, Dackis CA, O’Brien CP, Childress AR (2002) Decreased gray matter concentration in the insular, orbitofrontal, cingulate, and temporal cortices of cocaine patients. Biol Psychiatry 51:134–142
Friend DM, Keefe KA (2013) Glial reactivity in resistance to methamphetamine-induced neurotoxicity. J Neurochem 125:566–574
Fuente-Martin E, Garcia-Caceres C, Granado M, de Ceballos ML, Sanchez-Garrido MA, Sarman B, Liu ZW, Dietrich MO, Tena-Sempere M, Argente-Arizon P, Diaz F, Argente J, Horvath TL, Chowen JA (2012) Leptin regulates glutamate and glucose transporters in hypothalamic astrocytes. J Clinical Investig 122:3900–3913
Genoud C, Quairiaux C, Steiner P, Hirling H, Welker E, Knott GW (2006) Plasticity of astrocytic coverage and glutamate transporter expression in adult mouse cortex. PLoS Biol 4:e343
George O, Koob GF (2010) Individual differences in prefrontal cortex function and the transition from drug use to drug dependence. Neurosci Biobehav Rev 35:232–247
George O, Mandyam CD, Wee S, Koob GF (2008) Extended access to cocaine self-administration produces long-lasting prefrontal cortex-dependent working memory impairments. Neuropsychopharmacology 33:2474–2482
Ghitza UE, Zhai H, Wu P, Airavaara M, Shaham Y, Lu L (2010) Role of BDNF and GDNF in drug reward and relapse: a review. Neurosci Biobehav Rev 35:157–171
Gipson CD, Reissner KJ, Kupchik YM, Smith AC, Stankeviciute N, Hensley-Simon ME, Kalivas PW (2013) Reinstatement of nicotine seeking is mediated by glutamatergic plasticity. Proc Natl Acad Sci U S A 110:9124–9129
Goldberg M, De Pitta M, Volman V, Berry H, Ben-Jacob E (2010) Nonlinear gap junctions enable long-distance propagation of pulsating calcium waves in astrocyte networks. PLoS Comp Biol 6:e1000909
Goldstein RZ, Volkow ND (2002) Drug addiction and its underlying neurobiological basis: neuroimaging evidence for the involvement of the frontal cortex. Am J Psychiatry 159:1642–1652
Goldstein RZ, Volkow ND (2011) Dysfunction of the prefrontal cortex in addiction: neuroimaging findings and clinical implications. Nat Rev Neurosci 12:652–669
Goodlett CR, Leo JT, O’Callaghan JP, Mahoney JC, West JR (1993) Transient cortical astrogliosis induced by alcohol exposure during the neonatal brain growth spurt in rats. Brain Res Dev Brain Res 72:85–97
Gray KM, Carpenter MJ, Baker NL, DeSantis SM, Kryway E, Hartwell KJ, McRae-Clark AL, Brady KT (2012) A double-blind randomized controlled trial of N-acetylcysteine in cannabis-dependent adolescents. Am J Psychiatry 169:805–812
Guilarte TR, Nihei MK, McGlothan JL, Howard AS (2003) Methamphetamine-induced deficits of brain monoaminergic neuronal markers: distal axotomy or neuronal plasticity. Neuroscience 122:499–513
Halassa MM, Haydon PG (2010) Integrated brain circuits: astrocytic networks modulate neuronal activity and behavior. Ann Rev Physiol 72:335–355
Hanke ML, Kielian T (2011) Toll-like receptors in health and disease in the brain: mechanisms and therapeutic potential. Clin Sci 121:367–387
Hauser KF, Fitting S, Dever SM, Podhaizer EM, Knapp PE (2012) Opiate drug use and the pathophysiology of neuroAIDS. Curr HIV Res 10:435–452
Haydon PG, Blendy J, Moss SJ, Rob Jackson F (2009) Astrocytic control of synaptic transmission and plasticity: a target for drugs of abuse? Neuropharmacology 56(Suppl 1):83–90
Hirst WD, Price GW, Rattray M, Wilkin GP (1998) Serotonin transporters in adult rat brain astrocytes revealed by [3H]5-HT uptake into glial plasmalemmal vesicles. Neurochem Int 33:11–22
Hutchinson MR, Shavit Y, Grace PM, Rice KC, Maier SF, Watkins LR (2011) Exploring the neuroimmunopharmacology of opioids: an integrative review of mechanisms of central immune signaling and their implications for opioid analgesia. Pharmacol Rev 63:772–810
Hutchinson MR et al (2012) Opioid activation of toll-like receptor 4 contributes to drug reinforcement. J Neurosci 32:11187–11200
Hyman SE, Malenka RC, Nestler EJ (2006) Neural mechanisms of addiction: the role of reward-related learning and memory. Ann Rev Neurosci 29:565–598
Inazu M, Kubota N, Takeda H, Zhang J, Kiuchi Y, Oguchi K, Matsumiya T (1999) Pharmacological characterization of dopamine transport in cultured rat astrocytes. Life Sci 64:2239–2245
Inazu M, Takeda H, Matsumiya T (2003) Expression and functional characterization of the extraneuronal monoamine transporter in normal human astrocytes. J Neurochem 84:43–52
Jacob CP, Koutsilieri E, Bartl J, Neuen-Jacob E, Arzberger T, Zander N, Ravid R, Roggendorf W, Riederer P, Grunblatt E (2007) Alterations in expression of glutamatergic transporters and receptors in sporadic Alzheimer’s disease. J Alzheimers Dis 11:97–116
Jiang J, Amara SG (2011) New views of glutamate transporter structure and function: advances and challenges. Neuropharmacology 60:172–181
Kalivas PW (2009) The glutamate homeostasis hypothesis of addiction. Nat Rev Neurosci 10:561–572
Kalivas PW, Volkow ND (2005) The neural basis of addiction: a pathology of motivation and choice. Am J Psychiatry 162:1403–1413
Kalivas PW, Volkow ND (2011) New medications for drug addiction hiding in glutamatergic neuroplasticity. Mol Psychiatry 16:974–986
Kalivas PW, Volkow N, Seamans J (2005) Unmanageable motivation in addiction: a pathology in prefrontal-accumbens glutamate transmission. Neuron 45:647–650
Karakaya S, Kipp M, Beyer C (2007) Oestrogen regulates the expression and function of dopamine transporters in astrocytes of the nigrostriatal system. J Neuroendocrinol 19:682–690
Kawai T, Akira S (2006) TLR signaling. Cell Death Differ 13:816–825
Kelamangalath L, Wagner JJ (2010) D-serine treatment reduces cocaine-primed reinstatement in rats following extended access to cocaine self-administration. Neuroscience 169:1127–1135
Khan ZU, Koulen P, Rubinstein M, Grandy DK, Goldman-Rakic PS (2001) An astroglia-linked dopamine D2-receptor action in prefrontal cortex. Proc Natl Acad Sci U S A 98:1964–1969
Kimelberg HK, Katz DM (1985) High-affinity uptake of serotonin into immunocytochemically identified astrocytes. Science 228:889–891
Kittel-Schneider S, Kenis G, Schek J, van den Hove D, Prickaerts J, Lesch KP, Steinbusch H, Reif A (2012) Expression of monoamine transporters, nitric oxide synthase 3, and neurotrophin genes in antidepressant-stimulated astrocytes. Front Psychiatry 3:33
Knackstedt LA, LaRowe S, Mardikian P, Malcolm R, Upadhyaya H, Hedden S, Markou A, Kalivas PW (2009) The role of cystine-glutamate exchange in nicotine dependence in rats and humans. Biol Psychiatry 65:841–845
Knackstedt LA, Melendez RI, Kalivas PW (2010) Ceftriaxone restores glutamate homeostasis and prevents relapse to cocaine seeking. Biol Psychiatry 67:81–84
Koob GF, Nestler EJ (1997) The neurobiology of drug addiction. J Neuropsychiatry Clin Neurosci 9:482–497
Koob GF, Volkow ND (2010) Neurocircuitry of addiction. Neuropsychopharmacology 35:217–238
Kousik SM, Napier TC, Carvey PM (2012) The effects of psychostimulant drugs on blood brain barrier function and neuroinflammation. Front Pharmacol 3:121
Kovalevich J, Corley G, Yen W, Rawls SM, Langford D (2012) Cocaine-induced loss of white matter proteins in the adult mouse nucleus accumbens is attenuated by administration of a beta-lactam antibiotic during cocaine withdrawal. Am J Pathol 181:1921–1927
Kristiansen LV, Bannon MJ, Meador-Woodruff JH (2009) Expression of transcripts for myelin related genes in postmortem brain from cocaine abusers. Neurochem Res 34:46–54
Krueger M, Bechmann I (2010) CNS pericytes: concepts, misconceptions, and a way out. Glia 58:1–10
Lalumiere RT, Kalivas PW (2007) Reward and drugs of abuse. In: Kesner RP, Martinez JL (eds) Neurobiology of learning and memory. Academic, New York, pp 459–482
Lane SD, Steinberg JL, Ma L, Hasan KM, Kramer LA, Zuniga EA, Narayana PA, Moeller FG (2010) Diffusion tensor imaging and decision making in cocaine dependence. PLoS ONE 5:e11591
LaRowe SD, Myrick H, Hedden S, Mardikian P, Saladin M, McRae A, Brady K, Kalivas PW, Malcolm R (2007) Is cocaine desire reduced by N-acetylcysteine? Am J Psychiatry 164:1115–1117
LaRowe SD, Kalivas PW, Nicholas JS, Randall PK, Mardikian PN, Malcolm RJ (2013) A double-blind placebo-controlled trial of N-acetylcysteine in the treatment of cocaine dependence. Am J Addict 22:443–452
Le Bihan D, Mangin JF, Poupon C, Clark CA, Pappata S, Molko N, Chabriat H (2001) Diffusion tensor imaging: concepts and applications. J Magn Reson Imaging 13:534–546
Lemaitre B, Nicolas E, Michaut L, Reichhart JM, Hoffmann JA (1996) The dorsoventral regulatory gene cassette spatzle/toll/cactus controls the potent antifungal response in Drosophila adults. Cell 86:973–983
Leshner AI (1997) Addiction is a brain disease, and it matters. Science 278:45–47
Lewerenz J, Hewett SJ, Huang Y, Lambros M, Gout PW, Kalivas PW, Massie A, Smolders I, Methner A, Pergande M, Smith SB, Ganapathy V, Maher P (2013) The cystine/glutamate antiporter system x(c)(-) in health and disease: from molecular mechanisms to novel therapeutic opportunities. Antioxid Redox Signal 18:522–555
Lim JC, Donaldson PJ (2011) Focus on molecules: the cystine/glutamate exchanger (System x(c)(-)). Exp Eye Res 92:162–163
Lim KO, Choi SJ, Pomara N, Wolkin A, Rotrosen JP (2002) Reduced frontal white matter integrity in cocaine dependence: a controlled diffusion tensor imaging study. Biol Psychiatry 51:890–895
Lim KO, Wozniak JR, Mueller BA, Franc DT, Specker SM, Rodriguez CP, Silverman AB, Rotrosen JP (2008) Brain macrostructural and microstructural abnormalities in cocaine dependence. Drug Alcohol Depend 92:164–172
Lu L, Wang X, Wu P, Xu C, Zhao M, Morales M, Harvey BK, Hoffer BJ, Shaham Y (2009) Role of ventral tegmental area glial cell line-derived neurotrophic factor in incubation of cocaine craving. Biol Psychiatry 66:137–145
Luscher C, Malenka RC (2011) Drug-evoked synaptic plasticity in addiction: from molecular changes to circuit remodeling. Neuron 69:650–663
Mameli M, Luscher C (2011) Synaptic plasticity and addiction: learning mechanisms gone awry. Neuropharmacology 61:1052–1059
Mameli M, Halbout B, Creton C, Engblom D, Parkitna JR, Spanagel R, Luscher C (2009) Cocaine-evoked synaptic plasticity: persistence in the VTA triggers adaptations in the NAc. Nat Neurosci 12:1036–1041
Mann K, Kiefer F, Spanagel R, Littleton J (2008) Acamprosate: recent findings and future research directions. Alcohol Clin Exp Res 32:1105–1110
Martinez D, Narendran R (2010) Imaging neurotransmitter release by drugs of abuse. Curr Top Behav Neurosci 3:219–245
Masliah E, Alford M, DeTeresa R, Mallory M, Hansen L (1996) Deficient glutamate transport is associated with neurodegeneration in Alzheimer’s disease. Ann Neurol 40:759–766
McFarland K, Lapish CC, Kalivas PW (2003) Prefrontal glutamate release into the core of the nucleus accumbens mediates cocaine-induced reinstatement of drug-seeking behavior. J Neurosci 23:3531–3537
McGinty VB, Hayden BY, Heilbronner SR, Dumont EC, Graves SM, Mirrione MM, du Hoffmann J, Sartor GC, Espana RA, Millan EZ, Difeliceantonio AG, Marchant NJ, Napier TC, Root DH, Borgland SL, Treadway MT, Floresco SB, McGinty JF, Haber S (2011) Emerging, reemerging, and forgotten brain areas of the reward circuit: notes from the 2010 motivational neural networks conference. Behav Brain Res 225:348–357
Melendez RI, Hicks MP, Cagle SS, Kalivas PW (2005) Ethanol exposure decreases glutamate uptake in the nucleus accumbens. Alcohol Clin Exp Res 29:326–333
Miguel-Hidalgo JJ (2005) Lower packing density of glial fibrillary acidic protein-immunoreactive astrocytes in the prelimbic cortex of alcohol-naive and alcohol-drinking alcohol-preferring rats as compared with alcohol-nonpreferring and Wistar rats. Alcohol Clin Exp Res 29:766–772
Miyazaki I, Asanuma M, Diaz-Corrales FJ, Miyoshi K, Ogawa N (2004) Direct evidence for expression of dopamine receptors in astrocytes from basal ganglia. Brain Res 1029:120–123
Mookherjee P, Green PS, Watson GS, Marques MA, Tanaka K, Meeker KD, Meabon JS, Li N, Zhu P, Olson VG, Cook DG (2011) GLT-1 loss accelerates cognitive deficit onset in an Alzheimer’s disease animal model. J Alzheimers Dis 26:447–455
Morgello S, Uson RR, Schwartz EJ, Haber RS (1995) The human blood-brain barrier glucose transporter (GLUT1) is a glucose transporter of gray matter astrocytes. Glia 14:43–54
Moussawi K, Kalivas PW (2010) Group II metabotropic glutamate receptors (mGlu2/3) in drug addiction. Eur J Pharmacol 639:115–122
Moussawi K, Riegel A, Nair S, Kalivas PW (2011) Extracellular glutamate: functional compartments operate in different concentration ranges. Front Syst Neurosci 5:94
Myers KM, Carlezon WA, Jr. (2012) D-cycloserine effects on extinction of conditioned responses to drug-related cues. Biol Psychiatry 71:947–955
Nagasawa K, Kawasaki F, Tanaka A, Nagai K, Fujimoto S (2007) Characterization of guanine and guanosine transport in primary cultured rat cortical astrocytes and neurons. Glia 55:1397–1404
Najlerahim A, Francis PT, Bowen DM (1990) Age-related alteration in excitatory amino acid neurotransmission in rat brain. Neurobiol Aging 11:155–158
Narayana PA, Ahobila-Vajjula P, Ramu J, Herrera J, Steinberg JL, Moeller FG (2009) Diffusion tensor imaging of cocaine-treated rodents. Psychiatry Res 171:242–251
Navarrete M, Araque A (2008) Endocannabinoids mediate neuron-astrocyte communication. Neuron 57:883–893
Navarrete M, Araque A (2010) Endocannabinoids potentiate synaptic transmission through stimulation of astrocytes. Neuron 68:113–126
Nestler EJ, Aghajanian GK (1997) Molecular and cellular basis of addiction. Science 278:58–63
O’Malley EK, Sieber BA, Black IB, Dreyfus CF (1992) Mesencephalic type I astrocytes mediate the survival of substantia nigra dopaminergic neurons in culture. Brain Res 582:65–70
O’Neill CE, LeTendre ML, Bachtell RK (2012) Adenosine A2A receptors in the nucleus accumbens bi-directionally alter cocaine seeking in rats. Neuropsychopharmacology 37:1245–1256
Ohno M, Watanabe S (1996) D-cycloserine, a glycine site agonist, reverses working memory failure by hippocampal muscarinic receptor blockade in rats. Eur J Pharmacol 318:267–271
Olive MF, Cleva RM, Kalivas PW, Malcolm RJ (2012) Glutamatergic medications for the treatment of drug and behavioral addictions. Pharmacol Biochem Behav 100:801–810
Ossipov MH, Lai J, King T, Vanderah TW, Porreca F (2005) Underlying mechanisms of pronociceptive consequences of prolonged morphine exposure. Biopolymers 80:319–324
Paolone G, Botreau F, Stewart J (2009) The facilitative effects of D-cycloserine on extinction of a cocaine-induced conditioned place preference can be long lasting and resistant to reinstatement. Psychopharmacology (Berl) 202:403–409
Parpura V, Heneka MT, Montana V, Oliet SH, Schousboe A, Haydon PG, Stout RF, Jr., Spray DC, Reichenbach A, Pannicke T, Pekny M, Pekna M, Zorec R, Verkhratsky A (2012) Glial cells in (patho)physiology. J Neurochem 121:4–27
Pekny M, Nilsson M (2005) Astrocyte activation and reactive gliosis. Glia 50:427–434
Pfefferbaum A, Lim KO, Zipursky RB, Mathalon DH, Rosenbloom MJ, Lane B, Ha CN, Sullivan EV (1992) Brain gray and white matter volume loss accelerates with aging in chronic alcoholics: a quantitative MRI study. Alcohol Clin Exp Res 16:1078–1089
Pierce RC, Bari AA (2001) The role of neurotrophic factors in psychostimulant-induced behavioral and neuronal plasticity. Rev Neurosci 12:95–110
Pierre K, Pellerin L (2005) Monocarboxylate transporters in the central nervous system: distribution, regulation and function. J Neurochem 94:1–14
Pochon NA, Menoud A, Tseng JL, Zurn AD, Aebischer P (1997) Neuronal GDNF expression in the adult rat nervous system identified by in situ hybridization. Eur J Neurosci 9:463–471
Porter JT, McCarthy KD (1997) Astrocytic neurotransmitter receptors in situ and in vivo. Prog Neurobiol 51:439–455
Potier B, Billard JM, Riviere S, Sinet PM, Denis I, Champeil-Potokar G, Grintal B, Jouvenceau A, Kollen M, Dutar P (2010) Reduction in glutamate uptake is associated with extrasynaptic NMDA and metabotropic glutamate receptor activation at the hippocampal CA1 synapse of aged rats. Aging Cell 9:722–735
Qrunfleh AM, Alazizi A, Sari Y (2013) Ceftriaxone, a beta-lactam antibiotic, attenuates relapse-like ethanol-drinking behavior in alcohol-preferring rats. J Psychopharmacol 27:541–549
Radzishevsky I, Sason H, Wolosker H (2013) D-serine: physiology and pathology. Curr Opin Clin Nutr Metab Care 16:72–75
Reissner KJ, Kalivas PW (2010) Using glutamate homeostasis as a target for treating addictive disorders. Behav Pharmacol 21:514–522
Reissner KJ, Kalivas PW (2013) Cellular and molecular mechanisms of addiction. Neurobiology of mental illness, 4th edn
Reissner KJ, Brown RM, Spencer S, Tran SK, Thomas CA, Kalivas PW (2014) Chronic administration of the methylxanthine propentofylline impairs reinstatement to cocaine by a GLT-1 dependent mechanism. Neuropsychopharmacology (in press)
Rintala J, Jaatinen P, Kiianmaa K, Riikonen J, Kemppainen O, Sarviharju M, Hervonen A (2001) Dose-dependent decrease in glial fibrillary acidic protein-immunoreactivity in rat cerebellum after lifelong ethanol consumption. Alcohol 23:1–8
Rippeth JD, Heaton RK, Carey CL, Marcotte TD, Moore DJ, Gonzalez R, Wolfson T, Grant I, Group H (2004) Methamphetamine dependence increases risk of neuropsychological impairment in HIV infected persons. J Int Neuropsychol Soc 10:1–14
Rothstein JD, Patel S, Regan MR, Haenggeli C, Huang YH, Bergles DE, Jin L, Dykes Hoberg M, Vidensky S, Chung DS, Toan SV, Bruijn LI, Su ZZ, Gupta P, Fisher PB (2005) Beta-lactam antibiotics offer neuroprotection by increasing glutamate transporter expression. Nature 433:73–77
Saransaari P, Oja SS (1995) Age-related changes in the uptake and release of glutamate and aspartate in the mouse brain. Mech Ageing Dev 81:61–71
Sari Y, Smith KD, Ali PK, Rebec GV (2009) Upregulation of GLT1 attenuates cue-induced reinstatement of cocaine-seeking behavior in rats. J Neurosci 29:9239–9243
Sari Y, Sreemantula SN, Lee MR, Choi DS (2013) Ceftriaxone treatment affects the levels of GLT1 and ENT1 as well as ethanol intake in alcohol-preferring rats. J Mol Neurosci 51:779–787
Schaar DG, Sieber BA, Dreyfus CF, Black IB (1993) Regional and cell-specific expression of GDNF in rat brain. Exp Neurol 124:368–371
Schlaepfer TE, Lancaster E, Heidbreder R, Strain EC, Kosel M, Fisch HU, Pearlson GD (2006) Decreased frontal white-matter volume in chronic substance abuse. Int J Neuropsychopharmacol 9:147–153
Shao W, Zhang SZ, Tang M, Zhang XH, Zhou Z, Yin YQ, Zhou QB, Huang YY, Liu YJ, Wawrousek E, Chen T, Li SB, Xu M, Zhou JN, Hu G, Zhou JW (2013) Suppression of neuroinflammation by astrocytic dopamine D2 receptors via alphaB-crystallin. Nature 494:90–94
Shigetomi E, Tong X, Kwan KY, Corey DP, Khakh BS (2012) TRPA1 channels regulate astrocyte resting calcium and inhibitory synapse efficacy through GAT-3. Nat Neurosci 15:70–80
Sim ME, Lyoo IK, Streeter CC, Covell J, Sarid-Segal O, Ciraulo DA, Kim MJ, Kaufman MJ, Yurgelun-Todd DA, Renshaw PF (2007) Cerebellar gray matter volume correlates with duration of cocaine use in cocaine-dependent subjects. Neuropsychopharmacology 32:2229–2237
Simpson JE, Ince PG, Lace G, Forster G, Shaw PJ, Matthews F, Savva G, Brayne C, Wharton SB, Function MRCC, Ageing Neuropathology Study G (2010) Astrocyte phenotype in relation to Alzheimer-type pathology in the ageing brain. Neurobiol Aging 31:578–590
Sofroniew MV (2009) Molecular dissection of reactive astrogliosis and glial scar formation. Trends Neurosci 32:638–647
Sofroniew MV, Vinters HV (2010) Astrocytes: biology and pathology. Acta Neuropathol 119:7–35
Song P, Zhao ZQ (2001) The involvement of glial cells in the development of morphine tolerance. Neurosci Res 39:281–286
Sorg SF, Taylor MJ, Alhassoon OM, Gongvatana A, Theilmann RJ, Frank LR, Grant I (2012) Frontal white matter integrity predictors of adult alcohol treatment outcome. Biol Psychiatry 71:262–268
Soria G, Castane A, Ledent C, Parmentier M, Maldonado R, Valverde O (2006) The lack of A2A adenosine receptors diminishes the reinforcing efficacy of cocaine. Neuropsychopharmacology 31:978–987
Stuber GD, Hopf FW, Tye KM, Chen BT, Bonci A (2010) Neuroplastic alterations in the limbic system following cocaine or alcohol exposure. Curr Top Behav Neurosci 3:3–27
Tagliaferro P, Vega MD, Evrard SG, Ramos AJ, Brusco A (2002) Alcohol exposure during adulthood induces neuronal and astroglial alterations in the hippocampal CA-1 area. Ann N Y Acad Sci 965:334–342
Takeda H, Inazu M, Matsumiya T (2002) Astroglial dopamine transport is mediated by norepinephrine transporter. Naunyn Schmiedebergs Arch Pharmacol 366:620–623
Tawfik VL, Regan MR, Haenggeli C, Lacroix-Fralish ML, Nutile-McMenemy N, Perez N, Rothstein JD, DeLeo JA (2008) Propentofylline-induced astrocyte modulation leads to alterations in glial glutamate promoter activation following spinal nerve transection. Neuroscience 152:1086–1092
Thanos PK, Bermeo C, Wang GJ, Volkow ND (2009) D-cycloserine accelerates the extinction of cocaine-induced conditioned place preference in C57bL/c mice. Behav Brain Res 199:345–349
Turner JR, Ecke LE, Briand LA, Haydon PG, Blendy JA (2013) Cocaine-related behaviors in mice with deficient gliotransmission. Psychopharmacology (Berl) 226:167–176
Tzingounis AV, Wadiche JI (2007) Glutamate transporters: confining runaway excitation by shaping synaptic transmission. Nat Rev Neurosci 8:935–947
Van den Oever MC, Spijker S, Smit AB (2012) The synaptic pathology of drug addiction. Adv Exp Med Biol 970:469–491
Vatassery GT, Lai JC, Smith WE, Quach HT (1998) Aging is associated with a decrease in synaptosomal glutamate uptake and an increase in the susceptibility of synaptosomal vitamin E to oxidative stress. Neurochem Res 23:121–125
Vongvatcharanon U, Mukem S, Udomuksorn W, Kumarsit E, Vongvatcharanon S (2010) Alcohol administration during adulthood induces alterations of parvalbumin and glial fibrillary acidic protein immunoreactivity in rat hippocampus and cingulate cortex. Acta Histochem 112:392–401
Wang X, Lou N, Xu Q, Tian GF, Peng WG, Han X, Kang J, Takano T, Nedergaard M (2006) Astrocytic Ca2+ signaling evoked by sensory stimulation in vivo. Nat Neurosci 9:816–823
Watkins LR, Hutchinson MR, Johnston IN, Maier SF (2005) Glia: novel counter-regulators of opioid analgesia. Trends Neurosci 28:661–669
Watkins LR, Hutchinson MR, Rice KC, Maier SF (2009) The “toll” of opioid-induced glial activation: improving the clinical efficacy of opioids by targeting glia. Trends Pharmacol Sci 30:581–591
Wheeler DD, Ondo JG (1986) Time course of the aging of the high affinity L-glutamate transporter in rat cortical synaptosomes. Exp Gerontol 21:159–168
Witcher MR, Kirov SA, Harris KM (2007) Plasticity of perisynaptic astroglia during synaptogenesis in the mature rat hippocampus. Glia 55:13–23
Wlaz P, Rolinski Z, Czuczwar SJ (1996) Influence of D-cycloserine on the anticonvulsant activity of phenytoin and carbamazepine against electroconvulsions in mice. Epilepsia 37:610–617
Woltjer RL, Duerson K, Fullmer JM, Mookherjee P, Ryan AM, Montine TJ, Kaye JA, Quinn JF, Silbert L, Erten-Lyons D, Leverenz JB, Bird TD, Pow DV, Tanaka K, Watson GS, Cook DG (2010) Aberrant detergent-insoluble excitatory amino acid transporter 2 accumulates in Alzheimer disease. J Neuropathol Exp Neurol 69:667–676
Xu J, DeVito EE, Worhunsky PD, Carroll KM, Rounsaville BJ, Potenza MN (2010) White matter integrity is associated with treatment outcome measures in cocaine dependence. Neuropsychopharmacology 35:1541–1549
Yang FY, Lee YS, Cherng CG, Cheng LY, Chang WT, Chuang JY, Kao GS, Yu L (2013) D-cycloserine, sarcosine and D-serine diminish the expression of cocaine-induced conditioned place preference. J Psychopharmacol 27:550–558
Zorec R, Araque A, Carmignoto G, Haydon PG, Verkhratsky A, Parpura V (2012) Astroglial excitability and gliotransmission: an appraisal of Ca2+ as a signalling route. ASN Neuro 4:e00080
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2014 Springer Science+Business Media New York
About this chapter
Cite this chapter
Reissner, K., Kalivas, P. (2014). Emerging Roles for Glial Pathology in Addiction. In: Parpura, V., Verkhratsky, A. (eds) Pathological Potential of Neuroglia. Springer, New York, NY. https://doi.org/10.1007/978-1-4939-0974-2_17
Download citation
DOI: https://doi.org/10.1007/978-1-4939-0974-2_17
Published:
Publisher Name: Springer, New York, NY
Print ISBN: 978-1-4939-0973-5
Online ISBN: 978-1-4939-0974-2
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)