Abstract
The development of human kidney is a complex process requiring intricate cell and tissue interactions to assure the concerted program of cell growth, differentiation, and morphogenesis. Although the molecular and cellular nature of each of these interactions remains currently unclear, significant findings regarding nephrogenesis and its completion among different animal species have been reported over the last two decades. Research so far indicates that there are differences regarding the completion of the process of nephrogenesis among different animal species. In human, sheep, and spiny mouse, nephrogenesis is completed prior to birth, while in rat, mouse, and swine, nephrogenesis continuous after birth.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Unilateral Ureteral Obstruction
- Kidney Development
- Spiny Mouse
- Wolffian Duct
- Ureteropelvic Junction Obstruction
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
Introduction
The development of human kidney is a complex process requiring intricate cell and tissue interactions to assure the concerted program of cell growth, differentiation, and morphogenesis. Although the molecular and cellular nature of each of these interactions remains currently unclear, significant findings regarding nephrogenesis and its completion among different animal species have been reported over the last two decades. Research so far indicates that there are differences regarding the completion of the process of nephrogenesis among different animal species. In human, sheep, and spiny mouse, nephrogenesis is completed prior to birth, while in rat, mouse, and swine, nephrogenesis continuous after birth [1–7]. Nevertheless, the unrecognized morphological or functional peculiarities characterizing other animal species help the scientific community to reveal and understand the physiological mechanisms during nephrogenesis in human. This has been achieved mainly due to the increased use of animal models in renal basic science laboratories, as well as to the increased expertise of researchers who study kidney development. In the present chapter we aim at presenting and reviewing the existing knowledge on kidney development acquired from experimental studies.
Novel Structural/Molecules Components that Extend Knowledge on Kidney Development
The Pine-Cone Body
The mature kidney of mammals is the final product of three embryonic excretory organs, the pronephros, the mesonephros, and the metanephros. The latest originates from two main components, the ureteric bud and the mesenchymal cells of the metanephric mesenchyme [7, 8]. Recent studies using light electron microscopy reported that in the subcapsular regions of the outer portions of renal cortex, characterized by active nephrogenesis, some cap mesenchymal aggregates showed variability in shape and morphology of their cells. The center of the cap aggregates was occupied by a roundish cell, while their outer regions were characterized by the presence of thin curved shaped cell types twisted around a fixed central cluster, resembling a pine-cone-shaped structure [9].
Although early studies on nephrogenesis speculated that the sequence of morphological events leading to glomerulogenesis and tubulogenesis might start with the outgrowth of the primary nephric duct and the ureteric buds, which invade the metanephric mesenchyme and induce the differentiation of the renal epithelial precursors [10, 11], similar changes in the size and appearance of developing renal cells may be correlated to the various stages of cellular differentiation occurring during cap mesenchymal development [9]. These curved cells which may evolve from the ovoid cells found in the central area of the same aggregate could account for changes in transmembrane signaling and consequently for changes of cellular metabolic activity [12, 13]. Moreover, the presence of prominent and pleomorphic nucleoli may indicate a significant increased cellular metabolic activity associated with cellular differentiation during cap mesenchymal development [14]. These findings suggest the “pine-cone body” formation as an intermediate stage between the condensed mesenchymal nodule to the renal vesicle during conversion of mesenchyme to epithelium. At cellular level, the entire cap developmental process seems to represent the final event of a complex balance between specific intercellular signals involved in the regulation of protein synthesis, cell proliferation, cell motility, and apoptosis [9]. However, further research is necessary in order to better investigate the intimate significance of this new developmental structure.
Wnt Glycoproteins
Wnt-4 belongs to the Wnt family of secretory glycoproteins that are implicated in signaling processes operating during metanephric development. Wnt-4 is expressed in pretubular mesenchyme cells shortly before their aggregation and transformation to simple epithelial tubules [15]. Kispert et al. [16] showed that mesenchymally derived Wnt-4 is not only required, but also sufficient for induction of tubulogenesis in the mammalian kidney and can elicit the complete program of tubular differentiation in isolated metanephric mesenchyme. Interestingly, the activity of Wnt-4 contrasts with other factors thought to regulate mesenchymal development but proved not sufficient or not essential for tubulogenesis [17–23].
Wnt-4 may have a later function in tubulogenesis which is masked in the earlier requirement to form a tubule as Wnt-4 expression in the metanephric mesenchyme is initiated in the aggregating mesenchyme and maintained in the comma shaped bodies before it is downregulated in S-shaped bodies. Wnt-4 probably acts as a trigger to start an intrinsic program in the mesenchymal cells which then proceed to form complex nephron like structures. Considering that a permissive signal from the ureter to the mesenchyme triggers survival and tubulogenesis in the mesenchyme, it can be concluded that kidney tubulogenesis is a multi-step process with a hierarchy of signaling systems. In general, the role of Wnt-4 in tubulogenesis reflects that additional signaling systems control the ratio between interstitial and metanephrogenic cells, between condensing and non-condensing cells, and the maintenance of the mesenchymal stem cells in the periphery [16].
Wnt-9b is another glycoprotein expressed in the Wolffian duct and its derivative that has been implicated in the induction of the mammalian kidney development. Wnt-9b is expressed in the inductive epithelia and is essential for the development of mesonephric and metanephric tubules and caudal extension of the Müllerian duct as it is required for the earliest inductive response in metanephric mesenchym [24]. In addition, Wnt-9b-expressing cells can functionally substitute for the ureteric bud in these interactions. Interestingly, Wtn-9b acts upstream of Wnt-4, demonstrating the major role of Wnt signaling pathway in the organization of the mammalian urogenital system. Wtn-9b-dependent activation of Wnt-4 expression in the metanephric mesenchyme plays a central role in completing the process of tubule induction. Although Wnt-9b and Wnt-4 may act through distinct receptors, existing evidence suggest that Wnt-9b encodes a permissive signal, the region-specific response being governed by either the interplay of additional signaling factors or preprogramming of the target cell response by early patterning processes [24].
MUC-1
Although human MUC-1 mucin interest has mainly been focused on its role in carcinogenesis and tumor progression, its role in human and non-human embryogenesis was unclear until now. However, recent research in mouse embryos and neonates has shown, among other organs, increased MUC-1 expression in kidney as well [25]. In kidney, MUC-1 expression was mainly restricted to the apical part of the epithelial cells, in line with the characteristic pattern of MUC-1 in adult rat epithelial tissues [26, 27]. Although non-human studies related to MUC-1 have been mainly developed to obtain animal models useful for the comprehension of cancer, MUC-1 could play a relevant role during epithelia cellular differentiation and proliferation.
Glial Cell Line-Derived Neurotrophic Factor
Glial cell line-derived neurotrophic factor (GDNF) was shown to play a key role in kidney development through actions at the RET and GFR 1 receptor and coreceptor by initiating budding of the ureteric duct from the Wolffian duct, branching of the ureteric epithelium within the metanephric mesenchyme, and the formation of new nephrons at the branch tips [28–32]. In the late 1990s, knockout studies indicated that GDNF gene dosage influenced kidney development, with the loss of one allele being sufficient to cause a significant renal phenotype [33–40]. Recently, Cullen-McEwen et al. [41] found that the kidneys of GDNF heterozygous mice at 30 days of age were 25 % smaller than their wild-type littermates despite similar body weights, while stereologic estimates of nephron number identified a 30 % decrease in nephron endowment in young heterozygous GDNF mice compared with wild-type mice [42].
Although it was hypothesized that reductions in glomerular number lead to hypertrophy of the remaining glomeruli with time, evidence indicated that such hypertrophy also occurs when glomerular numbers are reduced genetically. Cullen-McEwen et al. [42] reported that by 14 months of age, glomeruli of GDNF heterozygotes were significantly hypertrophied such that the total glomerular volume was no longer different between wild-type and heterozygous littermates. Thus, the results found in this low nephron-number mouse are in accordance with the hypothesis of Brenner et al. [43] that a reduction in nephron number from birth leads to the development of hypertension and hyperfiltration.
Sodium Transporters
Although experimental studies have so far firmly established that the prenatal environment can modify the adult blood pressure [44–47], the mechanisms in humans are poorly understood. Nevertheless, several experimental models [44, 46–49] indicate that the various manipulations work through a common pathway.
Manning et al. [50] examined the expression of 4 key apical Na transport proteins that are critical for the regulation of Na balance and extracellular volume and found that upregulation of BSC1 and TSC, the apical Na transporters of TAL and DCT, respectively, occurs at both the mRNA and the protein level, reflecting increased Na reabsorption in these two segments. Moreover, NHE3 expression was not changed, suggesting that proximal tubule Na transport, at least the major fraction mediated by NHE3, is not affected by the prenatal programming; NHE3 may be upregulated by mechanisms not associated with altered protein abundance. Interestingly, the Na transporters were not downregulated after the hypertension became manifest, at 8 week of age. Considering that downregulation of TSC is an important component of the pressure-natriuresis response designed to correct hypertension by increasing renal Na excretion [51], prenatal programming of the Na transporters may override the normal pressure-natriuresis mechanism. Although the signal(s) from mother to fetus that result in transporter upregulation remain unknown, the fetal overexposure to maternal glucocorticoids due to decreased placental activity of the 11β-hydroxysteroid dehydrogenase type 2 enzyme was implicated as a proposed explanation [52, 53]. Indeed, maturation of renal Na transport, measured as Na-K-ATPase expression, is regulated by glucocorticoids and, therefore, abnormal glucocorticoid exposure could therefore have a direct effect on the maturing kidney [54].
Influential Factors of Kidney Development
Maternal Nutrition
The relationship between nutrition and nephrogenesis has been adequately established on animal models with experimental studies showing that maternal nutrition may have an important influence on renal programming [55]. In rats, a restricted supply of nutrients to the mother during the critical window in which nephrogenesis occurs led to a reduced number of glomeruli per kidney, activation of the renin–angiotensin system, glomerular enlargement, and hypertension in later life [47], while in another study, early postnatal overfeeding increased the number of postnatal nephrons and decreased glomerular volume, suggesting that global filtration surface area remains unchanged [56]. Under these circumstances, glomerular hyperfiltration to meet excretory demands due to early postnatal overfeeding could contribute to elevated blood pressure, proteinuria, and progressive glomerulosclerosis in aging overfed males than overfed females. Although the reasons as to why the influence of postnatal nutrition on nephron endowment is limited to male gender are unknown, it has been speculated that hyperleptinemia associated with early postnatal overfeeding may influence renal functions through specific effects involving renal sympathetic hyperactivity and decreased sodium excretion, partially due to an upregulation of Na-K-ATPase [57]. In either case, altered nephrogenesis plays an important role in the early origins of cardiovascular and renal diseases in adulthood [58–61]. Considering that hypertension may be observed in the absence of glomerular number reduction, it is possible that mechanisms different from inborn nephron number deficit to be involved. Of note, early postnatal overfeeding during the suckling period has been demonstrated to induce obesity and cardiovascular and metabolic disorders in adult rats, such as hyperinsulinism and insulin resistance, impairing vascular dilatation capacity through endothelial dysfunction [62–64].
Vitamin A has been proposed as a determinant in fetal renal programming in rats in view of its capacity to closely modulate nephron number and vascular supply [65, 66]. Moreover, the role of vitamin A in renal formation is considered essential since null mice for these genes exhibited renal agenesis or rudimental kidneys [67], while recently, vitamin A supply restored nephron endowment to normal in offspring of rat mothers exposed to protein restriction [68]. In this study, offspring exposed to maternal protein restriction during pregnancy and lactation had a significantly reduced body weight, kidney size, and nephron endowment at weaning, suggesting that administration of retinoic acid during pregnancy, early in gestation, is able to stimulate nephrogenesis per volume of kidney tissue over and above control levels [67]. Although the mechanisms by which retinoic acid stimulates nephrogenesis are not fully understood, studies suggest that it mediates its effects on nephrogenesis by stimulating ureteric branching morphogenesis [69, 70]. The same investigators suggested that the likely molecular candidate mediating these early nephrogenic effects is GDNF, acting via its cell-surface receptor GDNF-α and subsequently activating the receptor tyrosine kinase c-ret which is known to lead to increased branching morphogenesis of the ureteric bud and in turn enhance nephron formation [29, 30, 67, 71, 72]. Alternatively, administration of retinoic acid may mediate its effects on nephrogenesis via stimulation of the metanephric mesenchyme [73].
Previous studies reported that in male rats, exposure to maternal protein restriction either in utero or whilst suckling can have profound effects on kidney telomere lengths and on urine albumin excretion during much of adult life [74]. These rats appeared to be relatively protected against future nephron damage not only due to the absence of the nephrotoxic effects of urine albumin, but, also, because of their kidney telomere length. Telomere shortening has been implicated in renal diseases, while reduced renal telomere shortening is associated with increased levels of antioxidant enzymes, suggesting the beneficial effects of protein restriction on the development of kidney [75]. On the other hand, fetal exposure to a maternal low-protein diet is associated with disproportionate patterns of fetal growth and later elevation of blood pressure in the rat, suggesting that maternal undernutrition may program the renal nephron number and hence impact upon adult blood pressure and the development of renal disease [76]. Of note, in another study in rats exposed to a maternal low-protein diet in utero, renal morphometry and creatinine clearance at older ages were not influenced by prenatal diet, although blood pressure was elevated at all ages in the low-protein-exposed offspring [77]. However, blood urea N, urinary output, and urinary albumin excretion were significantly greater in low-protein-exposed rats than in control rats at 20 weeks of age, suggesting a progressive deterioration of renal function in hypertensive rats exposed to mild maternal protein restriction during fetal life. Although the mechanisms of protein restriction-induced adulthood hypertension are not well understood, Woods et al. reported that perinatal protein restriction in the rat suppresses the newborn intrarenal renin–angiotensin system and leads to a reduced number of glomeruli, glomerular enlargement, and hypertension in the adult [47]. Nevertheless, additional mechanisms may be involved in kidney development of protein-restricted mammals. Holemans et al. [78] investigated the hypothesis that malnutrition in pregnant rats may lead to altered cardiovascular function in adult female offspring and found that food restriction during the second half of pregnancy and/or lactation does not induce hypertension in adult offspring, but may effect subtle changes in vascular function. Interestingly, two other studies showed a very pronounced blunting of the response to acetylcholine in the neonatal vasculature from offspring of streptozotocin-diabetic rats on a high-fat diet and in the adult offspring of streptozotocin-diabetic rats [79, 80]. Brawley et al. [81] assessed isolated resistance artery function from adult male offspring of control and protein-restricted pregnant dams at two different ages and reported that dietary protein restriction in pregnancy induces hypertension and vascular dysfunction in male offspring. These disorders may be mediated via nitric oxide–cGMP pathway-induced abnormalities in endothelium-dependent and -independent relaxation, reducing vasodilation, and elevating systolic blood pressure [82]. Nevertheless, disturbances in the l-arginine–nitric oxide system and blastocyst abnormalities may contribute to the early appearance of hypertension in the offspring of mothers submitted to significant food restriction during pregnancy [83–87].
Intrauterine undernutrition also increases the oxidative stress by affecting the activity of various enzymes. In a study of pregnant rats submitted to intrauterine undernutrition, Franco et al. [88] tested the participation of certain enzymes on radical generation and found that NADPH oxidase inhibition attenuated superoxide anion generation and ameliorated vascular function. Indeed, release of the superoxide anion in the kidney can be deleterious as it inactivates NO, resulting in excess Na reabsorption and enhanced TGF feedback and thus hypertension [89–91]. In addition, inactivation of NO with oxygen radical forms peroxynitrite which can nitrosylate tyrosine residues, causing renal damage and increasing renal vascular resistance [92–97]. Furthermore, studies have also shown that oxygen radical causes direct vasoconstriction in preglomerular vasculature and in the renal cortical and medullary circulation, and increases intracellular calcium in vascular smooth muscle and endothelial cells, causing renal vasoconstriction and renal damage [98–104]. Accordingly, Franco Mdo et al. [105] reported that treatment with vitamins C and E reduced oxidative stress and high blood pressure levels, and improved vascular function in intrauterine-undernourished rats.
Studies in which oxidative stress was experimentally induced, caused increases in oxidative stress and hypertension, providing strong evidence for either an initiating or a sustaining role of reactive oxygen species in hypertension [94, 98, 106–116]. In Sprague–Dawley rats that received a high Na diet for 8 weeks, a period which is much longer than that in the above-mentioned studies, the arterial pressure increased significantly, and urinary albumin excretion and renal inflammation increased, suggesting that hypertension develops slowly when Na intake is increased in normotensive rats, and the blood pressure elevations are paralleled by increases in ROS and renal damage [117]. Based on the aforementioned data, it seems that long-term exposure to intrauterine oxidative stress may cause renal inflammation, renal damage, and arterial pressure postnatally. Oxidative stress, inflammation, and arterial hypertension participate in a self-perpetuating cycle which, if not interrupted, can lead to progressive cardiovascular disease and renal complications [118].
Nephrotoxic Agents
The administration of nephrotoxic agents may seriously affect renal development when performed prior to completion of nephrogenesis. Nathanson et al. [119] examined the potential adverse effects of ampicillin, amoxicillin, and ceftriaxone in rat kidney development and reported that both penicillins altered renal development in a dose-dependent manner, while ceftriaxone weakly impaired in vitro nephrogenesis; at a dose of 1,000 mg/ml kidney development is completely blocked. In young animals exposed to penicillins in utero, a mild oligonephronia was present and cystic tubule dilation was observed in newborn and in young animals as well. Gilbert et al. [120] analyzed, in vitro, the potential direct effect of gentamicin on early nephrogenesis and found that gentamicin induced a significant reduction in the number of nephrons in metanephric explants and that this effect was more important on less differentiated metanephroi. Smaoui et al. [121–123] studied the effect of gentamicin on the renal handling and transport of proteins in proximal tubular cells and reported that gentamicin, entering the proximal tubular cells via the endocytic pathway, decreased the tubular reabsorption of proteins, thus increasing urinary protein excretion and, consequently, nephrotoxicity.
Other drugs which probably have major embryo-fetal toxic effects are the nonsteroidal anti-inflammatory drugs (NSAIDs) which cross the placenta, reach the fetal circulation, and cause a spectrum of changes in the kidneys of the offspring [124]. Hasan et al. [125] examined the hypothesis that early postnatal ibuprofen has less adverse effects on neonatal rat renal prostanoids, COX-2 expression, and angiotensin II than indomethacin in newborn rats and found that indomethacin exhibited more potent suppressive effects on renal COX-2 and vasodilator prostanoids which are important regulators of renal development and function. Kent et al. [126] studied the type of renal changes found on light and electron microscopy following administration of indomethacin, ibuprofen, and gentamicin in a neonatal rat model and reported vacuolization of the epithelial proximal tubules, interstitial edema, intratubular protein deposition but no significant glomerular changes. Moreover, they found pleomorphic mitochondria and loss of microvilli in the tubules and extensive foot process effacement and irregularities of the glomerular basement membrane, concluding that these drugs cause significant change in glomerular and tubular structure in the neonatal rat model.
A number of studies have demonstrated the effect of angiotensin-converting enzyme (ACE) inhibition on systolic blood pressure and renal and uterine blood flow. Olsson et al. [127] studied the effects of intravenous captopril in goats during the last months of pregnancy and lactation and reported a more pronounced fall in arterial blood pressure and a larger increase in plasma renin activity during pregnancy when compared with the lactating period or with the nonpregnant state. It is quite interesting though that in a study evaluating the effect of the Renin Angiotensin System inhibition on the blood pressure and the mesenteric arteriolar reactivity of the intrauterine-undernourished rats, use of Angiotensin System inhibitors normalized the cardiovascular alterations induced by intrauterine undernutrition [128]. Blood pressure may be elevated in young rats following intrauterine exposure to a maternal low-protein diet in order to maintain glomerular filtration rate against a background of fewer nephrons via the increased expression of AT(1) receptors, which may arise as a result of the direct effect of protein restriction or in response to the reported decrease in renal tissue angiotensin II concentration [129].
Anatomical/Congenital Malformations
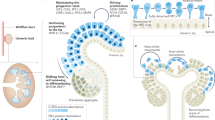
A number of animal models have been developed to study the pathophysiology of congenital hydronephrosis. These include ureteral obstruction in the fetal sheep, as well as in the postnatal opossum, pig, rabbit, and rodent [130–134]. In addition, the renal cellular and functional consequences of complete unilateral ureteral obstruction in the neonatal rat and mouse have been examined, which bear many similarities to human obstructive nephropathy [135, 136]. Based on previous studies showing that impairment of renal growth is directly dependent on the duration of temporary complete unilateral ureteral obstruction in the neonatal rat [137], Thornhill et al. [138] have recently developed a new model of variable partial unilateral ureteral obstruction in the neonatal rat that will aid in the elucidation of the mechanisms underlying the renal consequences of congenital ureteropelvic junction obstruction. The authors concluded that renal growth is impaired by a critical degree of partial unilateral ureteral obstruction. Persistent partial unilateral ureteral obstruction progressively reduces the number of nephrons during the period of nephron maturation (after the completion of nephrogenesis). Fixed partial ureteropelvic junction obstruction leads to a progressive dilatation of the renal pelvis and proximal ureter, tubular atrophy and interstitial fibrosis that are correlated with tubular apoptosis and are developed before detectable pelvic dilatation. Persistent moderate partial unilateral ureteral obstruction leads to a marked reduction in ipsilateral glomerular filtration rate and increased protein excretion before significant impairment of renal growth. Partial unilateral ureteral obstruction has a delayed stimulatory effect on adaptive growth of the contralateral kidney when compared to complete unilateral ureteral obstruction, and finally partial neonatal unilateral ureteral obstruction impairs somatic growth (Fig. 7.1).
(a) Fourteen-day-old rat with partial unilateral ureteral obstruction (UUO) at ureteropelvic junction (UPJ). Kidney is at upper left side, and renal pelvis has been filled with India ink, which traversed the obstruction and is visible in distal ureter (mm units on ruler). (b) Longitudinal section of ureter of 14-day-old rat showing the ureteral lumen (arrow indicates direction of urine flow) and cross-section of ligature (∗). The proximal ureter is dilated, and there is virtually no inflammatory response to the ligature. (c) Bisected representative kidneys from 14-day-old rats subjected to sham operation or partial UUO within the first 48 h of life. The contralateral kidney is shown on the upper row and the obstructed kidney on the bottom row. The luminal diameter of the partial obstruction is shown below each pair of kidneys (from [138] with permission)
Conclusion
Although the exact mechanisms governing renal development remain unclear, the increased use of animal models in renal basic science laboratories has extended our knowledge on this remarkable process. These promising results not only clarify many of the dark areas of nephrogenesis, but also they will boost the scientific efforts towards the elucidation of this phenomenon.
References
Gerosa C, Fanos V, Fanni D, Nemolato S, Locci A, Xanthos T, Papalois A, Faa G, Iacovidou N. Towards nephrogenesis in the pig kidney: the composite tubule-glomerular nodule. J Matern Fetal Neonatal Med. 2011;24 Suppl 2:52–4.
Ratliff B, Rodebaugh J, Sekulic M, Solhaug M. Glomerular eNOS gene expression during postnatal maturation and AT1 receptor inhibition. Pediatr Nephrol. 2007;22:1135–42.
Moritz KM, Wintour EM. Functional development of the meso- and metanephros. Pediatr Nephrol. 1999;13:171–8.
Dickinson H, Walker DW, Cullen-McEwen L, Wintour EM, Moritz K. The spiny mouse (Acomys cahirinus) completes nephrogenesis before birth. Am J Physiol Renal Physiol. 2005;289:F273–9.
Pohlenz JF, Winter KR, Dean-Nystrom EA. Shiga-toxigenic Escherichia coli-inoculated neonatal piglets develop kidney lesions that are comparable to those in humans with hemolytic-uremic syndrome. Infect Immun. 2005;73:612–6.
Yu B, Li S, Lin Z. Changes in β1 integrin in renal tubular epithelial cells after intrauterine asphyxia of rabbit pups. J Perinat Med. 2009;37:59–65.
Poladia DP, Kish K, Kutay B, Hains D, Kegg H, Zhao H, Bates CM. Role of fibroblast growth factor receptors 1 and 2 in the metanephric mesenchyme. Dev Biol. 2006;291:325–39.
Dressler GR. Epigenetics, development, and the kidney. J Am Soc Nephrol. 2008;19:2060–7.
Piludu M, Fanos V, Congiu T, Piras M, Gerosa C, Mocci C, Fanni D, Nemolato S, Muntoni S, Iacovidou N, Faa G. The pine-cone body: an intermediate structure between the cap mesenchyme and the renal vesicle in the developing nod mouse kidney revealed by an ultrastructural study. J Matern Fetal Neonatal Med. 2012;25 Suppl 5:72–5.
Faa G, Gerosa C, Fanni D, Monga G, Zaffanello M, Van Eyken P, Fanos V. Morphogenesis and molecular mechanisms involved in human kidney development. J Cell Physiol. 2012;227:1257–68.
Faa GGC, Fanni D, Nemolato S, Monga G, Fanos V. Kidney embryogenesis: how to look at old things with new eyes. In: Fanos VCR, Faa G, Cataldi L, editors. Developmental nephrology: from embryology to metabolomics. Quartu Sant’Elena: Hygeia Press; 2011. p. 23–45.
Ben-Ze’ev A. Animal cell shape changes and gene expression. Bioessays. 1991;13:207–12.
Ben-Ze’ev A. The role of changes in cell shape and contacts in the regulation of cytoskeleton expression during differentiation. J Cell Sci Suppl. 1987;8:293–312.
Hernandez-Verdun D, Roussel P, Thiry M, Sirri V, Lafontaine DL. The nucleolus: structure/function relationship in RNA metabolism. Wiley Interdiscip Rev RNA. 2010;1:415–31.
Stark K, Vainio S, Vassileva G, McMahon AP. Epithelial transformation of metanephric mesenchyme in the developing kidney regulated by Wnt-4. Nature. 1994;372:679–83.
Kispert A, Vainio S, McMahon AP. Wnt-4 is a mesenchymal signal for epithelial transformation of metanephric mesenchyme in the developing kidney. Development. 1998;125(21):4225–34.
Dudley AT, Lyons KM, Robertson EJ. A requirement for bone morphogenetic protein-7 during development of the mammalian kidney and eye. Genes Dev. 1995;9:2795–807.
Koseki C, Herzlinger D, Al-Awqati Q. Apoptosis in metanephric development. J Cell Biol. 1992;119:1327–33.
Luo G, Hofman C, Bronckers ALLJ, Sohocki M, Bradley A, Karsenty G. BMP-7 is an inducer of nephrogenesis, and is required for eye development and skeletal patterning. Genes Dev. 1995;9:2808–20.
Perantoni AO. Induction of tubules in rat metanephrogenic mesenchyme in the absence of an inductive tissue. Differentiation. 1991;48:25–31.
Perantoni AO, Dove LF, Karavanova I. Basic fibroblast growth factor can mediate the early inductive events in renal development. Proc Natl Acad Sci U S A. 1995;92:4696–700.
Vukicevic S, Kopp JB, Luyten FP, Sampath TK. Induction of nephrogenic mesenchyme by osteogenic protein 1 (bone morphogenetic protein 7). Proc Natl Acad Sci U S A. 1996;93:9021–6.
Weller A, Sorodin L, Illgen E-M, Ekblom P. Development and growth of mouse embryonic kidney in organ culture and modulation of developmental by soluble growth factor. Dev Biol. 1991;144:248–61.
Carroll TJ, Park JS, Hayashi S, Majumdar A, McMahon AP. Wnt9b plays a central role in the regulation of mesenchymal to epithelial transitions underlying organogenesis of the mammalian urogenital system. Dev Cell. 2005;9(2):283–92.
Lacunza E, Ferretti V, Barbeito C, Segal-Eiras A, Croce MV. Immunohistochemical evidence of Muc1 expression during rat embryonic development. Eur J Histochem. 2010;54(4):e49.
Braga VMM, Pemberton LF, Duhig T, Gendler SJ. Spatial and temporal expression of an epithelial mucin, Muc-1, during mouse development. Development. 1992;115:427–37.
Lacunza E, Bara J, Segal-Eiras A, Croce MV. Expression of conserved mucin domains by epithelial tissues in various mammalian species. Res Vet Sci. 2009;86:68–77.
Treanor JJ, Goodman L, de Sauvage F, Stone DM, Poulsen KT, Beck CD, Gray C, Armanini MP, Pollock RA, Hefti F, Phillips HS, Goddard A, Moore MW, Buj-Bello A, Davies AM, Asai N, Takahashi M, Vandlen R, Henderson CE, Rosenthal A. Characterization of a multicomponent receptor for GDNF. Nature. 1996;382:80–3.
Vega QC, Worby CA, Lechner MS, Dixon JE, Dressler GR. Glial cell line-derived neurotrophic factor activates the receptor tyrosine kinase RET and promotes kidney morphogenesis. Proc Natl Acad Sci U S A. 1996;93:10657–61.
Sainio K, Suvanto P, Davies J, Wartiovaara J, Wartiovaara K, Saarma M, Arumae U, Meng X, Lindahl M, Pachnis V, Sariola H. Glial-cell-line-derived neurotrophic factor is required for bud initiation from ureteric epithelium. Development. 1997;124:4077–87.
Pepicelli CV, Kispert A, Rowitch DH, McMahon AP. GDNF induces branching and increased cell proliferation in the ureter of the mouse. Dev Biol. 1997;192:193–8.
Towers PR, Woolf AS, Hardman P. Glial cell line-derived neurotrophic factor stimulates ureteric bud outgrowth and enhances survival of ureteric bud cells in vitro. Exp Nephrol. 1998;6:337–51.
Mackenzie HS, Lawler EV, Brenner BM. Congenital oligonephropathy: the fetal flaw in essential hypertension? Kidney Int Suppl. 1996;55:S30–4.
Pichel JG, Shen L, Sheng HZ, Granholm AC, Drago J, Grinberg A, Lee EJ, Huang SP, Saarma M, Hoffer BJ, Sariola H, Westphal H. Defects in enteric innervation and kidney development in mice lacking GDNF. Nature. 1996;382:73–6.
Pichel JG, Shen L, Sheng HZ, Granholm AC, Drago J, Grinberg A, Lee EJ, Huang SP, Saarma M, Hoffer BJ, Sariola H, Westphal H. GDNF is required for kidney development and enteric innervation. Cold Spring Harb Symp Quant Biol. 1996;61:445–57.
Moore MW, Klein RD, Farinas I, Sauer H, Armanini M, Phillips H, Reichardt LF, Ryan AM, Carver-Moore K, Rosenthal A. Renal and neuronal abnormalities in mice lacking GDNF. Nature. 1996;382:76–9.
Sanchez MP, Silos-Santiago I, Frisen J, He B, Lira SA, Barbacid M. Renal agenesis and the absence of enteric neurons in mice lacking GDNF. Nature. 1996;382:70–3.
Schuchardt A, D’Agati V, Larsson-Blomberg L, Costantini F, Pachnis V. Defects in the kidney and enteric nervous system of mice lacking the tyrosine kinase receptor Ret. Nature. 1994;367:380–3.
Enomoto H, Araki T, Jackman A, Heuckeroth RO, Snider WD, Johnson Jr EM, Milbrandt J. GFR alpha1-deficient mice have deficits in the enteric nervous system and kidneys. Neuron. 1998;21:317–24.
Cacalano G, Farinas I, Wang LC, Hagler K, Forgie A, Moore M, Armanini M, Phillips H, Ryan AM, Reichardt LF, Hynes M, Davies A, Rosenthal A. GFRalpha1 is an essential receptor component for GDNF in the developing nervous system and kidney. Neuron. 1998;21:53–62.
Cullen-McEwen LA, Drago J, Bertram JF. Nephron endowment in glial cell line-derived neurotrophic factor (GDNF) heterozygous mice. Kidney Int. 2001;60:31–6.
Cullen-McEwen LA, Kett MM, Dowling J, Anderson WP, Bertram JF. Nephron number, renal function, and arterial pressure in aged GDNF heterozygous mice. Hypertension. 2003;41(2):335–40.
Brenner BM, Garcia DL, Anderson S. Glomeruli and blood pressure: less of one, more the other? Am J Hypertens. 1988;1:335–47.
Langley-Evans SC, Welham SJM, Sherman RC, Jackson AA. Weanling rats exposed to maternal low-protein diets during discrete periods of gestation exhibit differing severity of hypertension. Clin Sci (Lond). 1996;91:607–15.
Manning J, Vehaskari VM. Low birth weight-associated adult hypertension in the rat. Pediatr Nephrol. 2001;16:417–22.
Vehaskari VM, Aviles DH, Manning J. Prenatal programming of adult hypertension in the rat. Kidney Int. 2001;59:238–45.
Woods LL, Ingelfinger JR, Nyengaard JR, Rasch R. Maternal protein restriction suppresses the newborn renin–angiotensin system and programs adult hypertension in rats. Pediatr Res. 2001;49:460–7.
Dodic M, May CN, Wintour EM, Coghlan JP. An early prenatal exposure to excess glucocorticoid levels leads to hypertensive offspring in sheep. Clin Sci (Lond). 1998;94:149–55.
Ortiz LA, Quan A, Weinberg A, Baum M. Effect of prenatal dexamethasone on rat renal development. Kidney Int. 2001;59:1663–9.
Manning J, Beutler K, Knepper MA, Vehaskari VM. Upregulation of renal BSC1 and TSC in prenatally programmed hypertension. Am J Physiol Renal Physiol. 2002;283(1):F202–6.
Wang XY, Masilamani S, Nielsen J, Kwon TH, Brooks HL, Nielsen S, Knepper MA. The renal thiazide-sensitive Na-Cl cotransporter as mediator of the aldosterone-escape phenomenon. J Clin Invest. 2001;108:215–22.
Langley-Evans SC. Maternal carbenoxolone treatment lowers birthweight and induces hypertension in the offspring of rats fed a protein-replete diet. Clin Sci (Lond). 1997;93:423–9.
Shams M, Kilby MD, Somerset DA, Howie AJ, Gupta A, Wood PJ, Afnan A, Stewart PM. 11Beta-hydroxysteroid dehydrogenase type 2 in human pregnancy and reduced expression in intrauterine growth restriction. Hum Reprod. 1998;13:799–804.
Celsi G, Nishi A, Akusjarvi G, Aperia A. Abundance of Na+-K+-ATPase mRNA is regulated by glucocorticoid hormones in infant rat kidneys. Am J Physiol. 1991;260:F192–7.
Barker DJ, Osmond C, Simmonds SJ, Wield GA. The relation of small head circumference and thinness at birth to death from cardiovascular disease in adult life. BMJ. 1993;306:422–6.
Boubred F, Buffat C, Feuerstein JM, Daniel L, Tsimaratos M, Oliver C, Lelièvre-Pégorier M, Simeoni U. Effects of early postnatal hypernutrition on nephron number and long-term renal function and structure in rats. Am J Physiol Renal Physiol. 2007;293(6):F1944–9.
Beltowski J, Jamroz-Wisniewska A, Borkowska E, Wojcicka G. Upregulation of renal Na, K ATPase: the possible novel mechanism of leptin-induced hypertension. Pol J Pharmacol. 2004;56:213–22.
Doyle LW, Faber B, Callanan C, Morley R. Blood pressure in late adolescence and very low birth weight. Pediatrics. 2003;111:252–7.
Hoy WE, Hughson MD, Bertram JF, Douglas-Denton R, Amann K. Nephron number, hypertension, renal disease, and renal failure. J Am Soc Nephrol. 2005;16:2557–64.
Johansson S, Iliadou A, Bergvall N, Tuvemo T, Norman M, Cnattingius S. Risk of high blood pressure among young men increases with the degree of immaturity at birth. Circulation. 2005;112:3430–6.
Keijzer-Veen MG, Finken MJ, Nauta J, Dekker FW, Hille ET, Frolich M, Wit JM, van der Heijden AJ, Dutch POPS19 Collaborative Study Group. Is blood pressure increased 19 years after intrauterine growth restriction and preterm birth? A prospective follow-up study in The Netherlands. Pediatrics. 2005;116:725–31.
You S, Götz F, Rohde W, Dörner G. Early postnatal overfeeding and diabetes susceptibility. Exp Clin Endocrinol. 1990;96:301–6.
Plagemann A, Harder T, Rake A, Voits M, Fink H, Rohde W, Dorner G. Perinatal elevation of hypothalamic insulin, acquired malformation of hypothalamic galaninergic neurons, and syndrome X-like alterations in adulthood of neonatally overfed rats. Brain Res. 1999;836:146–55.
Shinozaki K, Kashiwagi A, Masada M, Okamura T. Molecular mechanisms of impaired endothelial function associated with insulin resistance. Curr Drug Targets Cardiovasc Haematol Disord. 2004;4:1–11.
Puddu M, Fanos V, Podda F, Zaffanello M. The kidney from prenatal to adult life: perinatal programming and reduction of number of nephrons during development. Am J Nephrol. 2009;30(2):162–70.
Bhat PV, Manolescu DC. Role of vitamin A in determining nephron mass and possible relationship to hypertension. J Nutr. 2008;138:1407–10.
Lelièvre-Pégorier M, Vilar J, Ferrier ML, Moreau E, Freund N, Gilbert T, Merlet-Bénichou C. Mild vitamin A deficiency leads to inborn nephron deficit in the rat. Kidney Int. 1998;54:1455–62.
Makrakis J, Zimanyi MA, Black MJ. Retinoic acid enhances nephron endowment in rats exposed to maternal protein restriction. Pediatr Nephrol. 2007;22:1861–7.
Vilar J, Gilbert T, Moreau E, Merlet-Benichou C. Metanephros organogenesis is highly stimulated by vitamin A derivatives in organ culture. Kidney Int. 1996;49:1478–87.
Moreau E, Vilar J, Lelievre-Pegorier M, Merlet-Benichou C, Gilbert T. Regulation of c-ret expression by retinoic acid in rat metanephros: implication in nephron mass control. Am J Physiol. 1998;275:F938–45.
Mendelsohn C, Batourina E, Fung S, Gilbert T, Dodd J. Stromal cells mediate retinoid-dependent functions essential for renal development. Development. 1999;126:1139–48.
Batourina E, Gim S, Bello N, Shy M, Clagett-Dame M, Srinivas S, Costantini F, Mendelsohn C. Vitamin A controls epithelial/mesenchymal interactions through Ret expression. Nat Genet. 2001;27:74–8.
Welham SJ, Wade A, Woolf AS. Protein restriction in pregnancy is associated with increased apoptosis of mesenchymal cells at the start of rat metanephrogenesis. Kidney Int. 2002;61:1231–42.
Petry CJ, Jennings BJ, James LA, Hales CN, Ozanne SE. Suckling a protein-restricted rat dam leads to diminished albuminuria in her male offspring in adult life: a longitudinal study. BMC Nephrol. 2006;7:14.
Tarry-Adkins JL, Joles JA, Chen JH, Martin-Gronert MS, van der Giezen DM, Goldschmeding R, Hales CN, Ozanne SE. Protein restriction in lactation confers nephroprotective effects in the male rat and is associated with increased antioxidant expression. Am J Physiol Regul Integr Comp Physiol. 2007;293(3):R1259–66.
Langley-Evans SC, Welham SJ, Jackson AA. Fetal exposure to a maternal low protein diet impairs nephrogenesis and promotes hypertension in the rat. Life Sci. 1999;64(11):965–74.
Nwagwu MO, Cook A, Langley-Evans SC. Evidence of progressive deterioration of renal function in rats exposed to a maternal low-protein diet in utero. Br J Nutr. 2000;83(1):79–85.
Holemans K, Gerber R, Meurrens K, De Clerck F, Poston L, Van Assche FA. Maternal food restriction in the second half of pregnancy affects vascular function but not blood pressure of rat female offspring. Br J Nutr. 1999;81(1):73–9.
Koukkou E, Lowy C, Poston L. The offspring of diabetic rats fed a high saturated fat diet demonstrate abnormal vascular function. J Soc Gynecol Investig. 1997;4:115A. Abstr.
Holemans K, Gerber RT, Van Assche FA, Poston L. Adult offspring from diabetic Wistar rats show abnormal endotheliumdependent relaxation and reduced heart rate. J Vasc Res. 1998;35 Suppl 1:6. Abstr.
Brawley L, Itoh S, Torrens C, Barker A, Bertram C, Poston L, Hanson M. Dietary protein restriction in pregnancy induces hypertension and vascular defects in rat male offspring. Pediatr Res. 2003;54(1):83–90.
Franco Mdo C, Arruda RM, Fortes ZB, de Oliveira SF, Carvalho MH, Tostes RC, Nigro D. Severe nutritional restriction in pregnant rats aggravates hypertension, altered vascular reactivity, and renal development in spontaneously hypertensive rats offspring. J Cardiovasc Pharmacol. 2002;39(3):369–77.
Alves GM, Barão MA, Odo LN, Nascimento Gomes G, Franco Md Mdo C, Nigro D, Lucas SR, Laurindo FR, Brandizzi LI, Zaladek Gil F. l-Arginine effects on blood pressure and renal function of intrauterine restricted rats. Pediatr Nephrol. 2002;17(10):856–62.
Gil FZ, Lucas SR, Gomes GN, Cavanal Mde F, Coimbra TM. Effects of intrauterine food restriction and long-term dietary supplementation with l-arginine on age-related changes in renal function and structure of rats. Pediatr Res. 2005;57(5 Pt 1):724–31.
Racasan S, Braam B, van der Giezen DM, Goldschmeding R, Boer P, Koomans HA, Joles JA. Perinatal l-arginine and antioxidant supplements reduce adult blood pressure in spontaneously hypertensive rats. Hypertension. 2004;44(1):83–8.
de Queiroz DB, Ramos-Alves FE, Fernandes RL, Zuzu CP, Duarte GP, Xavier FE. Perinatal l-arginine and antioxidant supplements reduce adult blood pressure but not ameliorate the altered vascular function in spontaneously hypertensive rats. J Physiol Biochem. 2010;66(4):301–9.
Kwong WY, Wild AE, Roberts P, Willis AC, Fleming TP. Maternal undernutrition during the preimplantation period of rat development causes blastocyst abnormalities and programming of postnatal hypertension. Development. 2000;127(19):4195–202.
Franco Mdo C, Akamine EH, Di Marco GS, Casarini DE, Fortes ZB, Tostes RC, Carvalho MH, Nigro D. NADPH oxidase and enhanced superoxide generation in intrauterine undernourished rats: involvement of the renin–angiotensin system. Cardiovasc Res. 2003;59(3):767–75.
Manning Jr RD, Hu L, Reckelhoff JF. Role of nitric oxide in arterial pressure and renal adaptations to long-term changes in sodium intake. Am J Physiol. 1997;272:R1162–9.
Manning Jr RD, Hu L, Mizelle HL, Montani JP, Norton MW. Cardiovascular responses to long-term blockade of nitric oxide synthesis. Hypertension. 1993;22:40–8.
Tan DY, Meng S, Manning Jr RD. Role of neuronal nitric oxide synthase in Dahl salt-sensitive hypertension. Hypertension. 1999;33:456–61.
Gryglewski RJ, Palmer RMJ, Moncada S. Superoxide anion plays a role in the breakdown of endothelium-derived relaxing factor. Nature. 1986;320:454–6.
Garvin JL, Ortiz PA. The role of reactive oxygen species in the regulation of tubular function. Acta Physiol Scand. 2003;179:225–32.
Vaziri ND, Wang XQ, Oveisi F, Rad B. Induction of oxidative stress by glutathione depletion causes severe hypertension in normal rats. Hypertension. 2000;36(1):142–6.
Vaziri ND, Ni Z, Oveisi F, Trnavsky-Hobbs DL. Effect of antioxidant therapy on blood pressure and NO synthase expression in hypertensive rats. Hypertension. 2000;36(6):957–64.
Wesseling S, Joles JA, van Goor H, Bluyssen HA, Kemmeren P, Holstege FC, Koomans HA, Braam B. Transcriptome-based identification of pro- and antioxidative gene expression in kidney cortex of nitric oxide-depleted rats. Physiol Genomics. 2007;28(2):158–67.
Vaziri ND, Ni Z, Oveisi F. Upregulation of renal and vascular nitric oxide synthase in young spontaneously hypertensive rats. Hypertension. 1998;31(6):1248–54.
Meng S, Roberts LJ, Cason GW, Curry TS, Manning Jr RD. Superoxide dismutase and oxidative stress in Dahl salt-sensitive and -resistant rats. Am J Physiol. 2002;283:R732–8.
Meng S, Cason GW, Gannon AWRL, Manning Jr RD. Oxidative stress in Dahl salt-sensitive hypertension. Hypertension. 2003;41:1346–52.
Tian N, Thrasher KD, Gundy PD, Hughson MD, Manning Jr RD. Antioxidant treatment prevents renal damage and dysfunction and reduces arterial pressure in salt-sensitive hypertension. Hypertension. 2005;45:934–9.
Schnackenberg CG, Welch WJ, Wilcox CS. TP receptor-mediated vasoconstriction in microperfused afferent arterioles: roles of O(2)(−) and NO. Am J Physiol. 2000;279:F302–8.
Zou AP, Li N, Cowley Jr AW. Production and actions of superoxide in the renal medulla. Hypertension. 2001;37:547–53.
Lounsbury KM, Hu Q, Ziegelstein RC. Calcium signaling and oxidant stress in the vasculature. Free Radic Biol Med. 2000;28:1362–9.
Touyz RM. Oxidative stress and vascular damage in hypertension. Curr Hypertens Rep. 2000;2:98–105.
Franco Mdo C, Akamine EH, Aparecida de Oliveira M, Fortes ZB, Tostes RC, Carvalho MH, Nigro D. Vitamins C and E improve endothelial dysfunction in intrauterine-undernourished rats by decreasing vascular superoxide anion concentration. J Cardiovasc Pharmacol. 2003;42(2):211–7.
Ding Y, Gonick HC, Vaziri ND. Lead promotes hydroxyl radical generation and lipid peroxidation in cultured aortic endothelial cells. Am J Hypertens. 2000;13:552–5.
Ding Y, Gonick HC, Vaziri ND, Liang K, Wei L. Lead-induced hypertension. III. Increased hydroxyl radical production. Am J Hypertens. 2001;14:169–73.
Vaziri ND, Ding Y. Effect of lead on nitric oxide synthase expression in coronary endothelial cells: role of superoxide. Hypertension. 2001;37:223–6.
Vaziri ND, Liang K, Ding Y. Increased nitric oxide inactivation by reactive oxygen species in lead-induced hypertension. Kidney Int. 1999;56:1492–8.
Zhou XJ, Vaziri ND, Wang XQ, Silva FG, Laszik Z. Nitric oxide synthase expression in hypertension induced by inhibition of glutathione synthase. J Pharmacol Exp Ther. 2002;300:762–7.
Welch WJ, Solis G, Chabrashvili T, Aslam S, Chen Y, Wilcox CS. The role of superoxide dismutase on blood pressure regulation during prolonged low dose angiotensin II infusion. Hypertension 2006;48:934–41.
Chu Y, Iida S, Lund DD, Weiss RM, DiBona GF, Watanabe Y, Faraci FM, Heistad DD. Gene transfer of extracellular superoxide dismutase reduces arterial pressure in spontaneously hypertensive rats: role of heparin-binding domain. Circ Res. 2003;92:461–8.
Nakamura T, Lozano PR, Ikeda Y, Iwanaga Y, Hinek A, Minamisawa S, Cheng CF, Kobuke K, Dalton N, Takada Y, Tashiro K, Ross JJ, Honjo T, Chien KR. Fibulin-5/DANCE is essential for elastogenesis in vivo. Nature. 2002;415:171–5.
Yanagisawa H, Davis EC, Starcher BC, Ouchi T, Yanagisawa M, Richardson JA, Olson EN. Fibulin-5 is an elastin-binding protein essential for elastic fibre development in vivo. Nature. 2002;415:168–71.
Lenda DM, Sauls BA, Boegehold MA. Reactive oxygen species may contribute to reduced endothelium-dependent dilation in rats fed high salt. Am J Physiol. 2000;279:H7–14.
Liu Y, Rusch NJ, Lombard JH. Loss of endothelium and receptor-mediated dilation in pial arterioles of rats fed a short-term high salt diet. Hypertension. 1999;33:686–8.
Gu J-W, Bailey A, Shparago M. Long-term high salt diet causes hypertension and alters renal pro-inflammatory gene expression profiles in Sprague–Dawley rats. FASEB J. 2005;19:A1587.
Vaziri ND, Rodríguez-Iturbe B. Mechanisms of disease: oxidative stress and inflammation in the pathogenesis of hypertension. Nat Clin Pract Nephrol. 2006;2(10):582–93.
Nathanson S, Moreau E, Merlet-Benichou C, Gilbert T. In utero and in vitro exposure to beta-lactams impair kidney development in the rat. J Am Soc Nephrol. 2000;11(5):874–84.
Gilbert T, Gaonach S, Moreau E, Merlet-Benichou C. Defect of nephrogenesis induced by gentamicin in rat metanephric organ culture. Lab Invest. 1994;70(5):656–66.
Smaoui H, Mallie JP, Cheignon M, Borot C, Schaeverbeke J. Glomerular alterations in rat neonates after transplacental exposure to gentamicin. Nephron. 1991;59(4):626–31.
Smaoui H, Mallie JP, Schaeverbeke M, Robert A, Schaeverbeke J. Gentamicin administered during gestation alters glomerular basement membrane development. Antimicrob Agents Chemother. 1993;37(7):1510–7.
Smaoui H, Schaeverbeke M, Mallié JP, Schaeverbeke J. Transplacental effects of gentamicin on endocytosis in rat renal proximal tubule cells. Pediatr Nephrol. 1994;8(4):447–50.
Antonucci R, Pilloni MD, Fanos V. Antenatal non-steroidal anti-inflammatory drugs and the neonatal kidney. In: Fanos V, Chevalier RL, Faa G, Castaldi L, editors. Developmental nephrology: from embryology to metabolomics. Quartu S. Elena (Cagliari): Hygeia Press; 2011. p. 115–29.
Hasan J, Beharry KD, Gharraee Z, Stavitsky Y, Abad-Santos P, Abad-Santos M, Aranda JV, Modanlou HD. Early postnatal ibuprofen and indomethacin effects in suckling and weanling rat kidneys. Prostaglandins Other Lipid Mediat. 2008;85(3–4):81–8.
Kent AL, Maxwell LE, Koina ME, Falk MC, Willenborg D, Dahlstrom JE. Renal glomeruli and tubular injury following indomethacin, ibuprofen, and gentamicin exposure in a neonatal rat model. Pediatr Res. 2007;62(3):307–12.
Olsson K, Fyhrquist F, Benlamlih S, Dahlborn K. Effects of captopril on arterial blood pressure, plasma renin activity and vasopressin concentration in sodium-repleted and sodium-deficient goats: a serial study during pregnancy, lactation and anestrus. Acta Physiol Scand. 1984;121:73–80.
Ceravolo GS, Franco MC, Carneiro-Ramos MS, Barreto-Chaves ML, Tostes RC, Nigro D, Fortes ZB, Carvalho MH. Enalapril and losartan restored blood pressure and vascular reactivity in intrauterine undernourished rats. Life Sci. 2007;80(8):782–7.
Sahajpal V, Ashton N. Renal function and angiotensin AT1 receptor expression in young rats following intrauterine exposure to a maternal low-protein diet. Clin Sci (Lond). 2003;104(6):607–14.
Chung KH, Chevalier RL. Arrested development of the neonatal kidney following chronic ureteral obstruction. J Urol. 1996;155:1139–44.
Medjebeur AA, Bussieres L, Gasser B, et al. Experimental bilateral urinary obstruction in fetal sheep: transforming growth factorbeta1 expression. Am J Physiol Renal Physiol. 1997;273:F372–9.
Steinhardt GF, Salinas-Madrigal L, Demello D, et al. Experimental ureteral obstruction in the fetal opossum: histologic assessment. J Urol. 1994;152:2133–8.
Eskild-Jensen A, Frokiaer J, Djurhuus JC, et al. Reduced number of glomeruli in kidneys with neonatally induced partial ureteropelvic obstruction in pigs. J Urol. 2002;167:1435–9.
Mcvary KT, Maizels M. Urinary obstruction reduces glomerulogenesis in the developing kidney: a model in the rabbit. J Urol. 1989;142:646–51.
Chevalier RL, Kim A, Thornhill BA, Wolstenholme JT. Recovery following relief of unilateral ureteral obstruction in the neonatal rat. Kidney Int. 1999;55:793–807.
Chevalier RL, Thornhill BA, Chang AY. Unilateral ureteral obstruction in neonatal rats leads to renal insufficiency in adulthood. Kidney Int. 2000;58:1987–95.
Chevalier RL, Thornhill BA, Wolstenholme JT, Kim A. Unilateral ureteral obstruction in early development alters renal growth: dependence on the duration of obstruction. J Urol. 1999;161:309–13.
Thornhill BA, Burt LE, Chen C, Forbes MS, Chevalier RL. Variable chronic partial ureteral obstruction in the neonatal rat: a new model of ureteropelvic junction obstruction. Kidney Int. 2005;67(1):42–52.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2014 Springer Science+Business Media New York
About this chapter
Cite this chapter
Chalkias, A., Syggelou, A., Fanos, V., Xanthos, T., Iacovidou, N. (2014). Lessons on Kidney Development from Experimental Studies. In: Faa, G., Fanos, V. (eds) Kidney Development in Renal Pathology. Current Clinical Pathology. Humana Press, New York, NY. https://doi.org/10.1007/978-1-4939-0947-6_7
Download citation
DOI: https://doi.org/10.1007/978-1-4939-0947-6_7
Published:
Publisher Name: Humana Press, New York, NY
Print ISBN: 978-1-4939-0946-9
Online ISBN: 978-1-4939-0947-6
eBook Packages: MedicineMedicine (R0)