Abstract
Stressful stimuli abound in modern society and have shaped evolution through altering reproductive development, behavior, and physiology. The recent identification of kisspeptin as an important component of the hypothalamic regulatory circuits involved in reproductive homeostasis sparked a great deal of research interest that subsequently implicated kisspeptin signaling in the relay of metabolic, environmental, and physiological cues to the hypothalamo–pituitary–gonadal axis. However, although it is widely recognized that exposure to stress profoundly impacts on reproductive function, the roles of kisspeptin within the complex mechanisms underlying stress regulation of reproduction remain poorly understood. We and others have recently demonstrated that a variety of experimental stress paradigms downregulate the expression of kisspeptin ligand and receptor within the reproductive brain. Coincidently, these stressors also inhibit gonadotropin secretion and delay pubertal onset—processes that rely on kisspeptin signaling. However, a modest literature is inconsistent with an exclusively suppressive influence of stress on the reproductive axis and suggests that complicated neural interactions and signaling mechanisms translate the stress response into reproductive perturbations. The purpose of this chapter is to review the evidence for a novel role of kisspeptin signaling in the modulation of reproductive function by stress and to broaden the understanding of this timely phenomenon.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
Introduction
Kisspeptin has been widely recognized as a key regulator of the hypothalamo–pituitary–gonadal (HPG) axis, and thus reproductive development and function. The roles of kisspeptin in the control of sexual differentiation, puberty, surge, and pulsatile modes of gonadotropin secretion, gonadal steroid hormone feedback, pregnancy, lactation, and reproductive senescence have been well studied in a wide variety of clinical and animal models, as well as in vitro. However, the discovery of kisspeptin was associated with research on metastasis suppression mechanisms in malignant melanoma cells [1], and kisspeptin has been implicated in several peripheral, as well as central, processes, both physiological and pathological, that have little direct relevance to reproduction, including hippocampal seizures [2], cardiovascular vasoconstriction [3], renal fluid homeostasis [4], and pancreatic glucose-induced insulin secretion [5].
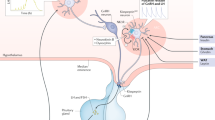
Although, by far, the most significant populations of kisspeptin-expressing neurons are found in the arcuate nucleus (ARC) and preoptic area (including the anteroventral periventricular (AVPV) and preoptic periventricular (PeN) nuclei in rodents) of the hypothalamus, both chiefly involved in regulation of reproductive functions, kisspeptin fibers are abundant in the paraventricular nucleus (PVN) of the hypothalamus [6], where perikarya of neurons that secrete corticotropin-releasing factor (CRF, a key neuroendocrine mediator of the stress response) and the stress-associated peptide hormones, arginine vasopressin (AVP) and oxytocin, are located [7]. Furthermore, numerous kisspeptin neurons project to limbic structures (namely the bed nucleus of the stria terminalis (BNST) and the medial nucleus of the amygdala (MeA)) [6], which innervate the PVN via gamma-aminobutyric acid (GABA)ergic inputs [8]. Therefore mammalian neuroanatomy potentially permits an intimate interaction between the HPG and stress axes, within which kisspeptin signaling may play a key role.
Experimental interventions commonly used so simulate a range of stressful situations and evoke a physiological stress response are referred to as stress paradigms. Administration of the Escherichia coli endotoxin, lipopolysaccharide (LPS), elicits reproducible acute inflammation that serves as a paradigm of immunological stress. Restraint of experimental animals is a well-defined acute psychological stress model. Social isolation has been used to replicate the effects of psychosocial stress, and is considered a mild stressor. Social status or rank reflects a more complex and chronic psychosocial stressor. The paradigms of metabolic stress are comparatively more diverse: nutritional disbalance, short-term fasting, chronic malnutrition, insulin-induced hypoglycemia, and exercise are all considered to exert physiological stress on individuals, although perhaps through different mechanisms. These have been extensively reviewed in the context of pubertal onset [9, 10] and reproductive function in adults [11]. Numerous other stress paradigms are routinely employed in research, and many share overlapping effects on the stress response and reproductive processes; a comprehensive review of each is beyond the scope of this chapter. Therefore we focused our discussion on the restraint, LPS, insulin-induced hypoglycemia, and social isolation experimental stress paradigms.
Puberty, Stress, and Kisspeptin
One major facet of reproductive research that concerns the effects of both kisspeptin and stress is puberty. Characterized as the transition from juvenile to adult state of reproductive development, growth, and adrenal maturation, pubertal timing in mammals (including man) is controlled by a multiplicity of complex interactions between genetic and environmental factors, with the latter providing fine tuning to maximize reproductive potential to fit the prevailing or predicted environment. There is unequivocal evidence that chronic stress exposure suppresses the activity of the HPG axis and delays puberty. However, less well recognized is the advancement of puberty by environmental factors, such as psychosocial stress within the family domain, including absence of father, as well as parental and mother–daughter conflict [12], with striking parallels in an animal model of weak parent–offspring bonding [13]. The age at which girls are reaching puberty has been trending downwards in recent decades, coincident with the increasing prevalence of overweight and obesity; this is in keeping with evidence that overnutrition advances puberty [14] and body fatness and a rapid elevation in BMI are predictors of earlier onset of puberty. However, recent studies reveal that this downward trend is evident irrespective of BMI, suggesting that other factors are involved [14, 15]. Animal models of delayed puberty (e.g., intrauterine growth retardation [16, 17] or neonatal exposure to LPS [18]) or advanced puberty (e.g., low maternal care [13] or high-fat diet [19]) also fails to show a clear correlation between body weight, body fat, or its central signaling biomarker, leptin, and the timing of puberty.
Kisspeptin/Kiss1r signaling is a prerequisite for physiological development of the reproductive system, since inactivating mutations in KISS1 [20] or KISS1R [21, 22] result in pubertal failure and hypogonadotropic hypogonadism in humans. Kiss1- and Kiss1r-knockout mouse models largely produce a similar reproductive phenotype [23–25], although Kiss1-knockout mouse model results in a less severe phenotype [26]. However, a recent report challenged the dogma that kisspeptin signaling is required for puberty and adult fertility in mice [27]. Nevertheless, levels of hypothalamic Kiss1 and Kiss1r expression peak at puberty (Fig. 20.1) [18, 28, 29], and kisspeptin administration stimulates precocious puberty in rats [30]. Furthermore, polymorphisms in the KISS1 gene [31] and activating mutations in KISS1R [32] are associated with central precocious puberty in humans. A variety of well-defined acute and chronic stress paradigms and experimental parameters of pubertal development have facilitated in vivo research aiming to elucidate the effects of stress on reproductive maturation. However, to this end, few studies have directly addressed the involvement of kisspeptin in the alteration of pubertal dynamics in response to stress.
Effects of neonatal lipopolysaccharide (LPS, 50 μg/kg ip) or saline control given at postnatal day (pnd) 3–5 on kisspeptin (Kiss1) mRNA expression in the medial preoptic area (mPOA) (a) and arcuate nucleus (ARC) (c) and on kisspeptin receptor (Kiss1r) mRNA expression in the mPOA (b) and ARC (d) in female rats at pnd 14, pnd 32, (the day of vaginal opening (dVO)), and at 11 weeks of age (Adult). Kiss1 and Kiss1r mRNA levels were measured in brain micropunch samples from the mPOA or ARC using real-time reverse transcriptase–polymerase chain reaction. Quantification for Kiss1, Kiss1r, and 28S rRNA was carried out on all samples; the values are expressed as a ratio of Kiss1 mRNA and 28S rRNA, or Kiss1r mRNA and 28S rRNA (mean ± SEM). *P > 0.05 vs. the respective treatment group at different time points; # P > 0.05 vs. saline control at same time point; n = 5–9 per group (from Knox AM, Li XF, Kinsey-Jones JS, Wilkinson ES, Wu XQ, Cheng YS, et al. Neonatal lipopolysaccharide exposure delays puberty and alters hypothalamic Kiss1 and Kiss1r mRNA expression in the female rat. J Neuroendocrinol. 2009 Aug;21(8):683–9. Reprinted with permission from John Wiley & Sons)
Exposure to an immune challenge, such as LPS, in the early neonatal period has been shown to have profound and long-lasting effects on the stress response throughout later life in the rat, evident through increased CRF gene expression in the PVN of the hypothalamus and an increase in the pulse frequency and amplitude of corticosterone (CORT) release [33]. We have shown that neonatal exposure to LPS delays puberty and disrupts estrous cyclicity, concordant with downregulation of Kiss1, but not Kiss1r, mRNA expression in the medial preoptic area (mPOA) (Fig. 20.1) [18, 34]. This decrease in Kiss1 expression could provide a mechanism for the observed delay of puberty. By contrast, the lack of effect of neonatal LPS treatment on Kiss1 or Kiss1r expression in the ARC would indicate that kisspeptin/Kiss1r signaling in this brain region is not an obvious contributing factor to pubertal delay. Interestingly, the postponement of LPS treatment from postnatal days 3 and 5 to postnatal days 7 and 9 failed to delay puberty, suggesting there is a discrete developmental time window that is sensitive to immunological challenge [18].
A variety of stressors that suppress GnRH pulse generator frequency, including LPS, downregulate hypothalamic Kiss1 and Kiss1r expression in adult rats [35, 36]. Although the neural inputs to the mPOA and ARC that mediate the stress-induced suppression of Kiss1 and Kiss1r expression within these loci remain to be determined, CRF is a prime candidate, not only because of its pivotal role in stress-induced suppression of the GnRH pulse generator [37–41], but also with respect to data showing that intracerebroventricular (ICV) administration of CRF profoundly decreased Kiss1 and Kiss1r mRNA levels in both the mPOA and ARC [35]. Moreover, we have shown that ICV administration of CRF or CRF antagonist delays or advances puberty, respectively, without altering the circulating levels of CORT, suggestive of CRF regulation of kisspeptin at puberty in the female rat [42]. Indeed, the delay in puberty consequent to administration of CRF was associated with a marked reduction in Kiss1 mRNA expression in the mPOA, but not the ARC [42]. Interestingly, we have shown a reduction in CRF, CRF receptor type 1 (CRF-R1), and CRF receptor type 2 (CRF-R2) mRNA expression in the PVN, the core regulatory component of the HPA axis, across pubertal transition in female rats (Fig. 20.2) [42]. Since bilateral lesions of the PVN do not alter the response of the HPG axis to stress in adult rats [43], the site and mechanism of action of the endogenous CRF tone that plays a critical role in the timing of puberty remain elusive. In the Japanese quail, genetic selection for high or low HPA axis stress responsivity delays or advances puberty, respectively [44]. A decrease in CRF and CRF-R1 expression was observed also in the mPOA, with no change in the ARC, across the pubertal transition in the rat (Fig. 20.2) [42]. However, possible interaction between CRF and kisspeptin signaling systems in the mPOA remains to be examined.
Developmental changes in CRF, CRF-R1, and CRF-R2 across puberty in the medial preoptic area (mPOA) (a–c), hypothalamic paraventricular nucleus (PVN) (d–f respectively), and arcuate nucleus (ARC) (g–i respectively). Time points include postnatal day 14 (d14), 32 (d32), day of vaginal opening (dVO: 40.9 ± 0.9 days, mean ± SEM), and adult (postnatal day 77). CRF, CRF-R1, and CRF-R2 mRNA levels were measured in brain micropunch samples from the mPOA, PVN, and ARC using a real-time reverse transcriptase–polymerase chain reaction. Note the peak in CRF mRNA levels in the mPOA and PVN in the late prepubertal phase that has receded by the time of puberty and the gradual decline in CRF-R1 expression in the mPOA across the pubertal transition. Quantification for CRF, CRF-R1, CRF-R2, and HPRT1 mRNA was carried out on all samples and the values are expressed as a ratio of CRF, CRF-R1, or CRF-R2 to HPRT1 mRNA (mean ± SEM). *P > 0.05 vs. other time points; # P > 0.05 vs. dVO; $P > 0.05 vs. adult; n = 6–10 per group (from Kinsey-Jones JS, Li XF, Knox AM, Lin YS, Milligan SR, Lightman SL, et al. Corticotrophin-releasing factor alters the timing of puberty in the female rat. J Neuroendocrinol. 2010 Feb;22(2):102-9. Reprinted with permission from John Wiley & Sons)
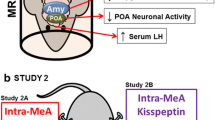
The importance of the limbic brain, in particular the amygdaloid complex, in the control of reproductive function and stress responsivity is well recognized [8, 45]. Overexpression of CRF in the central nucleus of the amygdala (CeA) disrupts estrous cyclicity and reduces GnRH expression [46]. Further, there is upregulation of CRF in the CeA with delayed puberty in neonatal LPS-treated rats (Li XF and O’Byrne KT; unpublished observation). The MeA is also a major regulator of the HPG and HPA axes [47], and there are extensive reciprocal connections between the MeA and CeA [48, 49]. Stimulation and ablation studies in prepubertal rats have revealed a critical role for the MeA in the timing of puberty, with lesions advancing puberty [50] and stimulation delaying puberty [51]. Moreover, we have shown that intra-MeA administration of CRF delays puberty in female rats (Li XF and O’Byrne KT; unpublished observation). Although extensive projections from the MeA to the mPOA [49] provide an anatomical substrate for a potential interaction with kisspeptin signaling systems that may mediate this inhibitory effect on pubertal timing, their neurochemical phenotype and modus operandi remain unknown.
Recent studies have shown that kisspeptin neurons project to many brain loc., including the PVN, which are not considered components of the HPG axis [6]. Although kisspeptin administration did not alter glucocorticoid secretion in vivo in monkeys [52] and rats [53], it did decrease CRF mRNA expression in a PVN neural cell line, thus raising the possibility of a novel mechanism for the regulation of the HPA axis by kisspeptin, as proposed by Rao and colleagues [53]. Indeed, the inverse relationship between PVN CRF and mPOA Kiss1 expression across the pubertal transition in the female rat (Figs. 20.1 and 20.2) is striking, though causality is unknown. In conclusion, a variety of stressors impact on pubertal timing, potentially by interfering with hypothalamic kisspeptin/Kiss1r signaling, though further research is required to elucidate the neural mechanisms involved in this interaction. The dynamics of pubertal development constitute a powerful correlate of HPG axis function vulnerable to stress, and the wealth of evidence for the involvement of kisspeptin makes the developing reproductive system a useful tool for the study of interactions between stress and kisspeptin signaling.
The GnRH Pulse Generator, Stress, and Kisspeptin
The dynamics of the pulsatile secretion of GnRH are believed to be controlled by a neural construct, probably resident within the mediobasal hypothalamus (MBH), termed the “GnRH pulse generator” [54]. The discovery of kisspeptin as a powerful and indispensible GnRH secretagogue, and the ensuing surge of academic discoveries linked to kisspeptin signaling, provide ample grounds on which to base the hypothesis that ARC kisspeptin neurons that coexpress neurokinin B (NKB), dynorphin A (Dyn), and the alpha subtype of the estrogen receptor (ERα) are the substrate of the GnRH pulse generator. These so-called KNDy neurons generate stimulatory and inhibitory signals to downstream mediators of reproductive function, provide estradiol-sensitive feedback to GnRH neurons, and seem to relay a wide variety of physiological and environmental stimuli to the HPG axis. Furthermore, the hypophysial GnRH and systemic LH pulses, as well as multiple electrophysiological manifestations of the GnRH pulse generator, serve as components of what can be described as a detailed bioassay for the many extrinsic stimuli that influence the HPG axis. For this reason, the study of the GnRH pulse generator is an indispensible tool for addressing the interactions of the stress system and the HPG axis.
The regulation of kisspeptin signaling by stress neural networks is evident in adult as well as peripubertal animals, despite a decline in ARC and mPOA kisspeptin expression following puberty [18, 55]. In adult female rats treated with LPS, levels of Kiss1 and Kiss1r mRNAs were decreased in the ARC and mPOA, in association with a suppression of GnRH pulse generator frequency (Figs. 20.3 and 20.4) [35]. Administration of kisspeptin reversed the reduction in serum LH levels associated with acute inflammation, and the LPS-induced suppression of LH secretion and Kiss1 mRNA expression are blocked by the anti-inflammatory drug, indomethacin [56]. Adult male rats treated with LPS have less abundant kisspeptin-immunoreactive cell bodies in the ARC than saline-injected controls, and the LPS-induced reduction in LH and testosterone (T) secretion in this animal model is independent of the anorexic effects of inflammation [57].
Effects of restraint, insulin-induced hypoglycemia (IIH), and lipopolysaccharide (LPS) stress on pulsatile LH secretion in ovariectomized estradiol (E2)-replaced rats. Representative examples showing (a) normal LH pulses in a rat in the absence of restraint stress, (b) restraint (1 h) stress-induced interruption of LH pluses, (c) normal LH pulses in a rat receiving an intravenous injection of vehicle (0.3 mL saline), (d) the inhibitory effects of insulin-induced hypoglycemic (insulin, 0.25 IU/kg in 0.3 mL saline i.v.) on LH pulses, (e) normal LH pulses in a rat receiving an intravenous injection of vehicle (0.3 mL saline) for the immunological stress, and (f) the inhibitory effects of LPS (0.5 μg/kg in 0.3 mL saline i.v.) on LH pulses. (g) Summaries showing the effects the three different stress paradigms on pulsatile LH secretion. *P > 0.05 vs. 2-h baseline control period within the same treatment group; n = 8 per group (from Kinsey-Jones JS, Li XF, Knox AM, Lin YS, Milligan SR, Lightman SL, et al. Corticotrophin-releasing factor alters the timing of puberty in the female rat. J Neuroendocrinol. 2010 Feb;22(2):102-9. Reprinted with permission from John Wiley & Sons)
Effects of restraint, insulin-induced hypoglycemia (IIH), and lipopolysaccharide (LPS) stress on kisspeptin (Kiss1) mRNA expression in the medial preoptic area (mPOA) (a) and arcuate nucleus (ARC) (b), and on kisspeptin receptor (Kiss1r) mRNA expression in the mPOA (c) and ARC (d) in ovariectomized estradiol (E2)-replaced rats. Kiss1 and Kiss1r mRNA levels were measured in brain micropunch samples from the mPOA or ARC using real-time RT-PCR. Quantification for Kiss1, Kiss1r, and 28S rRNA was carried out on all samples and the values are expressed as a ratio of Kiss1 mRNA and 28S rRNA, or Kiss1r mRNA and 28S rRNA (mean ± SEM). *P > 0.05 vs. respective control. # P > 0.05 vs. restraint or LPS controls; n = 8 per group (from Kinsey-Jones JS, Li XF, Knox AM, Wilkinson ES, Zhu XL, Chaudhary AA, et al. Down-regulation of hypothalamic kisspeptin and its receptor, Kiss1r, mRNA expression is associated with stress-induced suppression of luteinising hormone secretion in the female rat. J Neuroendocrinol. 2009 Jan;21(1):20-9. Reprinted with permission from John Wiley & Sons)
Adult female rats treated neonatally with LPS show decreased Kiss1 but elevated Kiss1r mRNA expression in the mPOA (Fig. 20.1) [18]. The same repercussions are observed following acute or chronic CORT administration in adult female rats but with identical changes in Kiss1/Kiss1r expression extending to the ARC (Fig. 20.5) [35]. Furthermore, such early life stress exposure programs the stress response in adulthood by inducing chronic hypercorticosteronemia [33] and upregulating the mPOA expression of CRF-R1 mRNA in response to acute homotypic stress exposure [58]. Such programming evidently sensitizes the animals to stress exposure in later life, with augmented stress-induced CORT secretion [33], disrupted estrous cyclicity [34], and suppression of the GnRH pulse generator [58] in rats treated neonatally with LPS than in saline-treated controls. On the contrary, neonatal LPS challenge in male rat pups attenuated the response to homotypic stress challenge in adulthood by restricting the increase in hypothalamic and testicular expression of mRNA encoding the proinflammatory cytokines TNF-α and IL-1β in response to LPS injection in adulthood, and thus preventing inflammatory suppression of LH secretion [59]. Indeed, the HPA axis is differentially modulated by the male and female gonadal steroids: hypothalamic activation of ERα augments the diurnal and stress-induced rises in circulating CORT, thus impairing glucocorticoid negative feedback on the HPA axis [60], while T enhances this feedback mechanism by increasing the availability of bioactive CORT, thereby decreasing circulating glucocorticoid levels [61]. In summary, neonatal LPS challenge modulates kisspeptin/Kiss1r signaling in adults and differentially programs responsiveness to stress later in adulthood in males and females.
Effects of acute (2 mg/kg, s.c. injection) or chronic (2 × 200 mg 21-day release s.c. pellets) CORT administration on kisspeptin (Kiss1) mRNA expression in the medial preoptic area (mPOA) (a) and arcuate nucleus (ARC) (b), and on Kiss1r mRNA expression in the mPOA (c) and ARC (d) in ovariectomized estradiol (E2)-replaced rats. Kiss1 and Kiss1r mRNA levels were measured in brain micropunch samples from the mPOA or ARC using real-time RT-PCR. Quantification for Kiss1, Kiss1r, and 28S rRNA was carried out on all samples and the values are expressed as a ratio of Kiss1 mRNA and 28S rRNA, or Kiss1r mRNA and 28S rRNA (mean ± SEM). *P > 0.05 vs. respective controls; n = 6–8 per group (from Kinsey-Jones JS, Li XF, Knox AM, Wilkinson ES, Zhu XL, Chaudhary AA, et al. Down-regulation of hypothalamic kisspeptin and its receptor, Kiss1r, mRNA expression is associated with stress-induced suppression of luteinising hormone secretion in the female rat. J Neuroendocrinol. 2009 Jan;21(1):20-9. Reprinted with permission from John Wiley & Sons)
Intravenous administration of insulin dramatically decreases plasma glucose, inducing acute hypoglycemia—a well-established paradigm of metabolic stress. Such stress rapidly elevates serum cortisol and suppresses both the endocrine and the electrophysiological correlates of the GnRH pulse generator in ovariectomized rhesus monkeys [62]. The inhibitory effect of insulin-induced hypoglycemia on pulsatile secretion of LH in adult female monkey and rats is CRF-dependent [38, 62], and involves CRF-R2, but not CRF-R1, at least in the rat [40]. Like other stressors, such as restraint (psychological) and LPS (immunological), hypoglycemia downregulates Kiss1 mRNA expression in the ARC and Kiss1r mRNA expression in the ARC and mPOA (Figs. 20.3 and 20.4) [35]. However, since kisspeptin expression is sensitive to metabolic cues [10], overnight fasting alone was sufficient to decrease basal levels of the mPOA Kiss1 message, an effect that was not amplified by insulin administration (Fig. 20.4) [35]. In fact, prolonged (72 h) fasting suppresses ARC kisspeptin expression and LH secretion, and prolongs the estrous cycle in gonadal intact adult female rats [63]. In summary, the suppression of the ARC kisspeptin expression by acute metabolic deprivation appears responsible for the inhibition of pulsatile LH secretion and the subsequent prolongation of the estrous cycle, and may be mediated by CRF-R2.
Psychological stress is often harder to define than other forms of stress, although restraint stress applied to experimental animals has long been employed as a model for a range of emotional and behavioral disturbances and psychiatric disorders. Clinically relevant psychological stressors stimulate the HPA axis and the sympathetic nervous system, as does acute restraint. Furthermore, this stress paradigm effectively suppresses the HPG axis, as is evident from disrupted LH pulsatility and downregulation of ARC Kiss1 and mPOA Kiss1 and Kiss1r mRNA expression following restraint in adult female rats (Figs. 20.3 and 20.4) [35]. However, unlike other stressors, restraint has no effect on ARC expression of Kiss1r [35]. The restraint-induced suppression of the LH pulse in adult female rats is blocked by direct injections of a nonselective CRF antagonist into the locus ceruleus; however, such treatment did not affect the hypoglycemic stress-induced suppression of LH secretion [64]. ICV administration of either type-specific (CRF-R1 or CRF-R2) CRF-R antagonists also blocked the inhibitory effects of restraint stress on pulsatile LH secretion in this animal model [39, 40]. Since the ARC and mPOA expression of Kiss1 and Kiss1r mRNA is robustly downregulated by icv administration of CRF [35], it is logical to hypothesize that the effects of restraint stress on LH secretion are downstream of the CRF-induced suppression of kisspeptin/Kiss1r signaling.
Isolation has been widely accepted as a mild social stressor. In female mice the stress of chronic isolation increases anxiety [65], undermines the regularity of estrous cyclicity, and downregulates mPOA Kiss1r expression [66]. Adult rat social isolates display a dysregulated CORT response, with acute stress (predator odor) markedly exacerbating the rise in CORT compared to grouped animals—an effect that is enhanced with age [67]. Individual reactivity or vulnerability to stress can reflect differences in dominance status among social animals. Variation in basal glucocorticoid levels has been identified to be dependent upon social rank in numerous species. Dominant female squirrel monkeys [68], cynomolgus monkeys [69], and baboons [70] demonstrate reduced cortisol levels compared with subordinates in the same social group, an effect that is also observed in the teleost fish (Haplochromis burtoni) [71], the naked mole rat (Heterocephalus glaber) [72], pig [73], and horse [74]. Similarly, subordinate mice [75] and rats [76] display higher basal CORT release than their dominant counterpart. In response to stress, however, subordinate rats displayed a significantly reduced, or even completely absent, CORT response as compared to their dominant counterparts [76]. This outcome is not uncommon in other species, including primates (e.g., olive baboon) [77], although this phenotype can be markedly modified subject to particular stylistic traits of social behavior in primate species [77]. Thus, subordination may result in changes in both the basal and stress-induced activity of the HPA axis. Generally, these facets have been interpreted as reflecting the chronic stress of social subordinance.
Social status is important in determining reproductive function in addition to stress reactivity in a wide variety of species. The common marmoset is a well-studied primate model of socially mediated infertility, in which subordinate females display impaired hypothalamic GnRH secretion and anovulation [78], and receipt of aggression from female conspecifics reduces LH pulse frequency [79]. The role of kisspeptin signaling in socially induced infertility in the common marmoset or other primates has not been reported. However, subordination in other species, including the naked mole rat, which exhibit extreme socially induced suppression of the HPG axis [80] displays downregulated kisspeptin in the AVPV [81]. Similarly, in the teleost fish, Astatotilapia burtoni, reduced Kiss1r expression was observed in whole brain of reproductively suppressed subordinate males [82].
Naturally, there are many caveats in extrapolating these data to humans. Nevertheless, it is of note that about 35% of women presenting with secondary amenorrhea are diagnosed with functional hypothalamic amenorrhea. In these women, effective stress management results in reversal of the extant low LH pulse frequency and hypercortisolism, and restoration of fertility in the vast majority [83]. The cynomolgus monkey has proved an exquisite primate model of functional hypothalamic amenorrhea, in which CRF-R1 antagonism restores normal GnRH pulse generator frequency suppressed by a combination of mild psychosocial and metabolic stressors that simulate the stressor indices of functional hypothalamic amenorrhea in women [84, 85]. Although the role of kisspeptin signaling has not been examined in this primate model, intermittent kisspeptin administration stimulates gonadotropin release in women with hypothalamic amenorrhea [86]. Furthermore, continuous kisspeptin infusion restores pulsatile LH secretion in men with hypogonadotropic hypogonadism resulting from loss-of-function mutations in NKB ligand and receptor [87].
A vast body of literature supports the notion that the GnRH pulse generator, as well as other reproductive networks within which kisspeptin signaling plays a key role, is exquisitely sensitive to changes within the environment, either as a direct consequence of perceived stressful stimuli or through autonomic suppression of nonessential physiological processes. Kisspeptin has widely been dubbed a central gatekeeper of reproductive function; however, such a moniker does not adequately befit the suitor in the context of stress suppression of the HPG axis. Kisspeptin and/or its receptor is downregulated by a variety of stressors and mediators of the stress response, “surrendering” gracelessly at the mere sight of “intruders” and thus allowing the instillation of a suppressive “regime.” It is perhaps this submissive nature of the kisspeptin/Kiss1r system that allows stressful stimuli to deregulate reproductive processes and, in some individuals, lets this develop into reproductive pathologies. To consolidate the grounds for an interaction between kisspeptin signaling and the stress response, we proceed to reviewing recent data that suggest potential neural mechanisms for this interaction.
Mechanisms Integrating Stress Networks and Kisspeptin Signaling
Despite many similarities in which various stressors activate the HPA axis and/or the sympathetic nervous system, as well as inhibit the HPG axis, a number of disparities are also evident from current literature. First, the central mediators of the stress response are differentially implicated in the suppression of the GnRH pulse generator. Consistent with a CRF-dependent mechanism of stress suppression of the HPG axis are the findings that, in the female rat, (1) ICV administration of CRF [38] or a selective CRF-R2 agonist [39] prolongs the LH pulse interval; (2) CRF-R2 antagonism blocks the suppression of pulsatile LH secretion induced by restraint [39], insulin-induced hypoglycemia, and LPS [40]; and (3) the inhibitory effect of restraint stress on LH secretion is blocked by a selective CRF-R1 antagonist [40]. However, blockade of CRF-R1 did not affect the hypoglycemia- and LPS-induced suppression of the GnRH pulse generator [40]. Furthermore, while CRF, insulin-induced hypoglycemia, and LPS downregulated the expression of both kisspeptin and its receptor in the ARC and mPOA, restraint did not affect the ARC expression of Kiss1r [35]. These findings point at the notion that different stressors employ differential neural mechanisms for the activation of the stress response and suppression of the reproductive axis.
Second, while various stress paradigms, as well as ICV CRF administration, potently downregulate Kiss1 and Kiss1r mRNA expression in the ARC and mPOA, concomitant with suppression of pulsatile LH secretion, both acute and chronic administration of physiological CORT downregulate Kiss1, but upregulate Kiss1r expression, with no net effect on LH pulses [35]. Indeed, acute stress-induced CORT release has no effect on pulsatile LH secretion in the monkey [88]. Further, treatment with metyrapone, an inhibitor of adrenal steroidogenesis that prevented the CRF-induced rise in CORT levels, did not reverse the inhibitory effects of CRF on GnRH pulse generator frequency in the rhesus monkey [89]. The decrease in the ARC expression of Kiss1 mRNA following CORT administration has also been shown in male mice, and CORT was hypothesized to influence kisspeptin neurons directly, in light of the expression of glucocorticoid receptors (GR) by these cells [36], despite previous reports that gonadal GR mediate the stress-induced CORT feedback on the HPG axis [90]. In mice, however, CORT did decrease LH levels, albeit at a pharmacological dose [36]. Kisspeptin, on the other hand, affects neither CORT nor adrenocorticotropin hormone (ACTH) levels under basal or restraint stress conditions, in adult male rats [53]. It is apparent, therefore, that central and peripheral processes of the HPA axis modulate hypothalamic kisspeptin signaling in different ways. It is important to note that components of the stress axis do not act in isolation in vivo, and hence multiple parameters of the stress response need to be considered when extrapolating conclusions regarding the stress feedback to the kisspeptin/Kiss1r system.
Third, different neuronal populations appear to mediate the suppressive effects of different types of stress. In addition to the aforementioned involvement of CRF-R1 and CRF-R2 in the suppression of pulsatile LH secretion under various stress paradigms, neurons projecting from the locus ceruleus [64], the BNST [41], and the amygdala [45], as well as several neuropeptides, including AVP, Dyn, and calcitonin gene-related peptide (CGRP), along with the chiefly inhibitory amino acid neurotransmitter γ-aminobutyric acid (GABA), have all been shown to play key roles in the stress-induced suppression of reproductive function. These mechanisms are further discussed below. Finally, while stress is commonly known to confer an energetic advantage to an organism at the expense of its nonessential bodily functions, e.g., reproduction, in some scenarios, stressful stimuli may serve to enhance the functions of the HPG axis and, in particular, induce premature LH surges and ovulation [91, 92]. These observations hint at a complex network of stress-reactive neurons spanning numerous regions of the brain, without a clearly identified central mediator of the integration of stress stimuli with reproductive function, in the context of kisspeptin signaling.
To date, various limbic structures have been differentially implicated in the modulation of the effects of different stressors on the HPA axis [8]. We have recently shown evidence for the involvement of the MeA and CeA in psychogenic and immunological stress-induced suppression of the GnRH pulse generator, respectively [45]. Adult female rats in which the MeA was chemically lessoned showed an attenuated restraint-induced, but not hypoglycemia- or LPS-induced, decrease in LH pulse frequency [45]. The extent of the LPS-induced suppression of pulsatile LH secretion was strongly reduced in CeA-lesioned animals vs. intact controls, though the CeA lesions had no effect on the LH pulse following restraint or hypoglycemic stress [45]. These data suggest that these two amygdaloid loci are not involved in mediating the hypoglycemic stress-induced suppression of the LH pulse. Indeed, we have previously shown that removal of the area postrema of the caudal brainstem prevents insulin-induced glucoprivic suppression of pulsatile LH secretion [93].
CRF neurons of the BNST connect the PVN with the amygdala, hippocampus, and prefrontal cortex [94]. Further, non-CRF interneurons project to mPOA GnRH perikarya [95]. When stimulated electrochemically, lateral BNST neurons prevent ovulation by abrogating the preovulatory surge of LH, while medial BNST neurons advanced the LH surge in proestrus rats [96]. Administration of CRF directly into the dorsolateral BNST of adult female rats dose dependently suppresses pulsatile LH secretion and activates GABA neurons in the mPOA [41]. Furthermore, intra-BNST injection of a selective CRF-R2 antagonist blocked the restraint-induced, but not IIH-induced, suppression of pulsatile LH secretion [41].
The brainstem noradrenergic locus ceruleus is innervated by CRF neurons projecting from CeA [97], BNST [98], and PVN [99]. Bilateral electrolytic lesions of the locus ceruleus disrupt both the pulsatile [100] and surge [101] modes of LH release. Intra-cerulear administration of CRF to adult OVX rats dose dependently suppresses pulsatile LH secretion and activates GABA neurons in the mPOA [64]. These effects are amplified by estradiol [64]. Furthermore, intra-cerulear injection of a nonselective CRF receptor antagonist blocked the restraint-induced, but not glucoprivic, suppression of pulsatile LH secretion [64].
Although CRF signaling appears indispensible in mediating stress-induced suppression of the HPG axis, other neuropeptide and amino acid signaling molecules have also been implicated in the inhibition of GnRH neurons. AVP and CRF, both expressed by parvocellular neurons of the PVN, act synergistically to stimulate ACTH secretion from the anterior pituitary, although different mechanisms are involved in regulating AVP and CRF expression in response to acute and chronic stress exposure [102]. AVP neurons of the suprachiasmatic nucleus (SCN) of the hypothalamus innervate the kisspeptin neuron population in the AVPV, and estradiol has been shown to increase the number of these monosynaptic connections [103]. Moreover, ICV administration of kisspeptin increases plasma AVP levels in rats [104], although without altering the firing rate of AVP/oxytocin neurons of the supraoptic nucleus of the hypothalamus [105]. This could suggest that kisspeptin is involved in a feedback mechanism bridging the stress response with reproductive function.
CGRP neurons project from the caudal aspect of the organum vasculosum of the lamina terminalis (OVLT), via the AVPV, to the medial preoptic nucleus [106], and form direct contacts with CRF neurons of the CeA [107, 108]. Central administration of CGRP induces c-fos expression in the CeA [109], mPOA, and PVN [110]. Moreover, CGRP-treated rats demonstrate elevated circulating CORT levels [110, 111] and GnRH pulse generator inhibition [110, 112], effects that are dependent on CRF-R1 signaling [109]. Administered intra-mPOA, CGRP dose dependently suppressed LH pulse frequency [112], while intra-PVN administration of CGRP stimulates ACTH and CORT release [111]. A GnRH cell line expresses CGRP receptors, and CGRP dose dependently suppresses GnRH release in vitro [113]. These data strongly implicate hypothalamic CGRP signaling in the inhibition of the GnRH pulse generator in response to HPA axis activation.
The endogenous opioid peptide, Dyn, is coexpressed with kisspeptin and NKB in ARC KNDy neurons that project to GnRH neurons [114, 115]. Central administration of a Dyn analog, selective for the kappa-subtype of the opioid receptor (KOR), suppresses pulsatile LH secretion in female rats [116], and KOR antagonism blocks the CGRP- and NKB-mediated suppression of pulsatile LH secretion [116, 117]. Because endogenous opioid peptides play an important role in stress-induced suppression of the reproductive axis, and since KNDy neurons express KOR, Dyn might inhibit the GnRH pulse generator through autocrine inhibition of the kisspeptin tone.
RF-amide-related peptide type-3 (RFRP-3), a member of the same RF-amine superfamily as kisspeptin and a mammalian ortholog of avian gonadotropin-inhibitory hormone (GnIH), is inhibitory to both GnRH neuron firing [118, 119] and LH secretion [120, 121], while RFRP receptor antagonists are stimulatory to LH secretion [122, 123]. In addition to the widespread distribution of RFRP-3 neuron fibers in the hypothalamus, with abundant close appositions to GnRH cells [124], these fibers are also present in the hypothalamic PVN and limbic areas, including the BNST and MeA [120, 125]. Taken together, these data provide an anatomical substrate for the hypothesis that stress-induced suppression of the HPG axis is mediated, in part, by RFRP-3.
Indeed, there are numerous PVN CRF neurons with close RFRP-3 fiber appositions [126] and there is abundant expression of GPR147 mRNA, encoding the putative RFRP receptor, in the PVN [127]. Further, central administration of RFRP-3 evokes c-fos expression in the PVN, increases ACTH release, and induces anxiety in the rat [127]. It has also been suggested that RFRP-3 plays a key role in stress-induced suppression of gonadotropin secretion, since an increase in hypothalamic RFRP mRNA expression was associated with reduced LH secretion in response to immobilization stress in the rat [128]. In addition, hypothalamic RFRP-3 neurons express CRF-R1 and GR [128], and CRF per se increased GPR147 mRNA expression, concomitant with reduced GNRH1 mRNA levels in the GnRH-expressing N39 cells in vitro [129]. Moreover, RFRP-3 blocks kisspeptin-induced activation of GnRH neurons [119]. It is conceivable that functional interactions between the excitatory kisspeptin and inhibitory GnIH signaling pathways fine-tune the response of the GnRH neural system to stressors, thus minimizing reproductive dysfunction.
GABAergic transmission underlies a significant proportion of inhibitory stimuli in the brain, including those at GnRH neurons [130, 131]. Activity of GABA neurons in the mPOA is stimulated by central CRF administration [41, 64], as well as by a range of stress paradigms [45, 132–134]. We have recently shown mPOA GABA receptors (GABAAR and GABABR) to be differentially involved in mediating the suppressive effects of immunological and psychological stress on LH secretion, respectively [135]. Furthermore, both GABAAR and GABABR antagonists block the inhibition of the LH pulse by CRF [135]. Therefore, the CRF neurons projecting to the mPOA seem to mediate the GABA receptor-dependent effects of stress on the GnRH neural system. Since AVPV kisspeptin neurons are predominantly GABAergic [136] and GABAAR antagonism potently induces kisspeptin secretion in the stalk-median eminence of prepubertal monkeys [137], the balance between stimulatory kisspeptin and inhibitory GABA inputs appears to govern marked changes in the pattern of GnRH neurosecretion. Indeed, the pubertal increase in GnRH release is preceded by a reduction in GABAergic inhibition, and disinhibition of GnRH secretion through GABAAR antagonism induces precocious puberty in juvenile monkeys [138]. Thus, it is probable that stress-induced suppression of GnRH secretion is secondary to the inhibition of kisspeptin and/or GnRH neurons by GABA.
Conclusion
The complexity of the neural networks and signaling mechanisms involved in the translation of sensory stimuli into a stress response, complicated further by peripheral feedback mechanisms (CORT and ACTH), as well as evidence for the convergence of multiple stimulatory and inhibitory neuronal populations, makes a reductionist approach to the interpretation of the interactions between stress and reproduction suboptimal. Direct neural pathways are not a prerequisite for stress suppression of kisspeptin signaling. Synaptic transmission through interneurons [139], and/or paracrine volume transmission of neuropeptidergic signals [140], may also be involved in the regulation of GnRH neurosecretion by signaling systems associated with the stress response. Hypotheses arising through anatomical observations must be consolidated by functional data; however, intracellular events should also be taken into consideration. While considerable effort has been made to untangle the individual neural pathways that may contribute to the stress suppression of reproductive function, revealing the true complexity of the networks in question, a meaningful model of the complex interaction between stress and reproduction is warranted. Perhaps future mathematical modeling will aid the assembly of the components of the stress and reproductive systems brought to light to date and, ultimately, provide a better understanding of the neural connectivity and signaling mechanisms involved. In summary, kisspeptin signaling is a novel component of the stress neurocircuitry implicated in the perturbation of reproductive development and function under stress conditions.
References
Lee JH, Miele ME, Hicks DJ, Phillips KK, Trent JM, Weissman BE et al (1996) KiSS-1, a novel human malignant melanoma metastasis-suppressor gene. J Natl Cancer Inst 88(23):1731–1737
Arai AC (2009) The role of kisspeptin and GPR54 in the hippocampus. Peptides 30(1):16–25
Mead EJ, Maguire JJ, Kuc RE, Davenport AP (2007) Kisspeptins are novel potent vasoconstrictors in humans, with a discrete localization of their receptor, G protein-coupled receptor 54, to atherosclerosis-prone vessels. Endocrinology 148(1):140–147
Nakamura Y, Aoki S, Xing Y, Sasano H, Rainey WE (2007) Metastin stimulates aldosterone synthesis in human adrenal cells. Reprod Sci 14(8):836–845
Bowe JE, King AJ, Kinsey-Jones JS, Foot VL, Li XF, O’Byrne KT et al (2009) Kisspeptin stimulation of insulin secretion: mechanisms of action in mouse islets and rats. Diabetologia 52(5):855–862
Clarkson J, d'Anglemont de Tassigny X, Colledge WH, Caraty A, Herbison AE (2009) Distribution of kisspeptin neurones in the adult female mouse brain. J Neuroendocrinol 21(8):673–682
Landgraf R, Neumann ID (2004) Vasopressin and oxytocin release within the brain: a dynamic concept of multiple and variable modes of neuropeptide communication. Front Neuroendocrinol 25(3–4):150–176
Herman JP, Ostrander MM, Mueller NK, Figueiredo H (2005) Limbic system mechanisms of stress regulation: hypothalamo-pituitary-adrenocortical axis. Prog Neuropsychopharmacol Biol Psychiatry 29(8):1201–1213
Cameron JL (1991) Metabolic cues for the onset of puberty. Horm Res 36(3–4):97–103
Castellano JM, Bentsen AH, Mikkelsen JD, Tena-Sempere M (2010) Kisspeptins: bridging energy homeostasis and reproduction. Brain Res 1364:129–138
Aubert ML, Pierroz DD, Gruaz NM, d’Alleves V, Vuagnat BA, Pralong FP et al (1998) Metabolic control of sexual function and growth: role of neuropeptide Y and leptin. Mol Cell Endocrinol 140(1–2):107–113
Deardorff J, Ekwaru JP, Kushi LH, Ellis BJ, Greenspan LC, Mirabedi A et al (2011) Father absence, body mass index, and pubertal timing in girls: differential effects by family income and ethnicity. J Adolesc Health 48(5):441–447
Cameron NM, Champagne FA, Parent C, Fish EW, Ozaki-Kuroda K, Meaney MJ (2005) The programming of individual differences in defensive responses and reproductive strategies in the rat through variations in maternal care. Neurosci Biobehav Rev 29(4–5):843–865
Aksglaede L, Juul A, Olsen LW, Sorensen TI (2009) Age at puberty and the emerging obesity epidemic. PLoS One 4(12):e8450
Morris DH, Jones ME, Schoemaker MJ, Ashworth A, Swerdlow AJ (2010) Determinants of age at menarche in the UK: analyses from the Breakthrough Generations Study. Br J Cancer 103(11):1760–1764
Engelbregt MJ, van Weissenbruch MM, Popp-Snijders C, Lips P, Delemarre-van de Waal HA (2001) Body mass index, body composition, and leptin at onset of puberty in male and female rats after intrauterine growth retardation and after early postnatal food restriction. Pediatr Res 50(4):474–478
Iwasa T, Matsuzaki T, Murakami M, Fujisawa S, Kinouchi R, Gereltsetseg G et al (2010) Effects of intrauterine undernutrition on hypothalamic Kiss1 expression and the timing of puberty in female rats. J Physiol 588(Pt 5):821–829
Knox AM, Li XF, Kinsey-Jones JS, Wilkinson ES, Wu XQ, Cheng YS et al (2009) Neonatal lipopolysaccharide exposure delays puberty and alters hypothalamic Kiss1 and Kiss1r mRNA expression in the female rat. J Neuroendocrinol 21(8):683–689
Boukouvalas G, Gerozissis K, Kitraki E (2010) Fat feeding of rats during pubertal growth leads to neuroendocrine alterations in adulthood. Cell Mol Neurobiol 30(1):91–99
Topaloglu AK, Tello JA, Kotan LD, Ozbek MN, Yilmaz MB, Erdogan S et al (2012) Inactivating KISS1 mutation and hypogonadotropic hypogonadism. N Engl J Med 366(7):629–635
Seminara SB, Messager S, Chatzidaki EE, Thresher RR, Acierno JS Jr, Shagoury JK et al (2003) The GPR54 gene as a regulator of puberty. N Engl J Med 349(17):1614–1627
de Roux N, Genin E, Carel JC, Matsuda F, Chaussain JL, Milgrom E (2003) Hypogonadotropic hypogonadism due to loss of function of the KiSS1-derived peptide receptor GPR54. Proc Natl Acad Sci U S A 100(19):10972–10976
Funes S, Hedrick JA, Vassileva G, Markowitz L, Abbondanzo S, Golovko A et al (2003) The KiSS-1 receptor GPR54 is essential for the development of the murine reproductive system. Biochem Biophys Res Commun 312(4):1357–1363
d'Anglemont de Tassigny X, Fagg LA, Dixon JP, Day K, Leitch HG, Hendrick AG et al (2007) Hypogonadotropic hypogonadism in mice lacking a functional Kiss1 gene. Proc Natl Acad Sci U S A 104(25):10714–10719
Chan YM, Broder-Fingert S, Wong KM, Seminara SB (2009) Kisspeptin/Gpr54-independent gonadotrophin-releasing hormone activity in Kiss1 and Gpr54 mutant mice. J Neuroendocrinol 21(12):1015–1023
Lapatto R, Pallais JC, Zhang D, Chan YM, Mahan A, Cerrato F et al (2007) Kiss1-/- mice exhibit more variable hypogonadism than Gpr54-/- mice. Endocrinology 148(10):4927–4936
Mayer C, Boehm U (2011) Female reproductive maturation in the absence of kisspeptin/GPR54 signaling. Nat Neurosci 14(6):704–710
Navarro VM, Castellano JM, Fernandez-Fernandez R, Barreiro ML, Roa J, Sanchez-Criado JE et al (2004) Developmental and hormonally regulated messenger ribonucleic acid expression of KiSS-1 and its putative receptor, GPR54, in rat hypothalamus and potent luteinizing hormone-releasing activity of KiSS-1 peptide. Endocrinology 145(10):4565–4574
Shahab M, Mastronardi C, Seminara SB, Crowley WF, Ojeda SR, Plant TM (2005) Increased hypothalamic GPR54 signaling: a potential mechanism for initiation of puberty in primates. Proc Natl Acad Sci U S A 102(6):2129–2134
Navarro VM, Fernandez-Fernandez R, Castellano JM, Roa J, Mayen A, Barreiro ML et al (2004) Advanced vaginal opening and precocious activation of the reproductive axis by KiSS-1 peptide, the endogenous ligand of GPR54. J Physiol 561(Pt 2):379–386
Luan X, Zhou Y, Wang W, Yu H, Li P, Gan X et al (2007) Association study of the polymorphisms in the KISS1 gene with central precocious puberty in Chinese girls. Eur J Endocrinol 157(1):113–118
Teles MG, Bianco SD, Brito VN, Trarbach EB, Kuohung W, Xu S et al (2008) A GPR54-activating mutation in a patient with central precocious puberty. N Engl J Med 358(7):709–715
Shanks N, Windle RJ, Perks PA, Harbuz MS, Jessop DS, Ingram CD et al (2000) Early-life exposure to endotoxin alters hypothalamic-pituitary-adrenal function and predisposition to inflammation. Proc Natl Acad Sci U S A 97(10):5645–5650
Wu XQ, Li XF, Ye B, Popat N, Milligan SR, Lightman SL et al (2011) Neonatal programming by immunological challenge: effects on ovarian function in the adult rat. Reproduction 141(2):241–248
Kinsey-Jones JS, Li XF, Knox AM, Wilkinson ES, Zhu XL, Chaudhary AA et al (2009) Down-regulation of hypothalamic kisspeptin and its receptor, Kiss1r, mRNA expression is associated with stress-induced suppression of luteinising hormone secretion in the female rat. J Neuroendocrinol 21(1):20–29
Wang O, Lanjuin A, Basko J, Dulac C, Majzoub J (2011) Glucocorticoids inhibit kisspeptin neurons during stress-induced reproductive inhibition. Endocr Rev 32(03_MeetingAbstracts):P3–P141
Rivier C, Vale W (1984) Influence of corticotropin-releasing factor on reproductive functions in the rat. Endocrinology 114(3):914–921
Cates PS, Li XF, O’Byrne KT (2004) The influence of 17beta-oestradiol on corticotrophin-releasing hormone induced suppression of luteinising hormone pulses and the role of CRH in hypoglycaemic stress-induced suppression of pulsatile LH secretion in the female rat. Stress 7(2):113–118
Li XF, Bowe JE, Lightman SL, O’Byrne KT (2005) Role of corticotropin-releasing factor receptor-2 in stress-induced suppression of pulsatile luteinizing hormone secretion in the rat. Endocrinology 146(1):318–322
Li XF, Bowe JE, Kinsey-Jones JS, Brain SD, Lightman SL, O’Byrne KT (2006) Differential role of corticotrophin-releasing factor receptor types 1 and 2 in stress-induced suppression of pulsatile luteinising hormone secretion in the female rat. J Neuroendocrinol 18(8):602–610
Li XF, Lin YS, Kinsey-Jones JS, Milligan SR, Lightman SL, O’Byrne KT (2011) The role of the bed nucleus of the stria terminalis in stress-induced inhibition of pulsatile luteinising hormone secretion in the female rat. J Neuroendocrinol 23(1):3–11
Kinsey-Jones JS, Li XF, Knox AM, Lin YS, Milligan SR, Lightman SL et al (2010) Corticotrophin-releasing factor alters the timing of puberty in the female rat. J Neuroendocrinol 22(2):102–109
Rivest S, Rivier C (1991) Influence of the paraventricular nucleus of the hypothalamus in the alteration of neuroendocrine functions induced by intermittent footshock or interleukin. Endocrinology 129(4):2049–2057
Satterlee DG, Marin RH, Jonest RB (2002) Selection of Japanese quail for reduced adrenocortical responsiveness accelerates puberty in males. Poult Sci 81(7):1071–1076
Lin Y, Li X, Lupi M, Kinsey-Jones JS, Shao B, Lightman SL et al (2011) The role of the medial and central amygdala in stress-induced suppression of pulsatile LH secretion in female rats. Endocrinology 152(2):545–555
Keen-Rhinehart E, Michopoulos V, Toufexis DJ, Martin EI, Nair H, Ressler KJ et al (2009) Continuous expression of corticotropin-releasing factor in the central nucleus of the amygdala emulates the dysregulation of the stress and reproductive axes. Mol Psychiatry 14(1):37–50
Solomon MB, Jones K, Packard BA, Herman JP (2010) The medial amygdala modulates body weight but not neuroendocrine responses to chronic stress. J Neuroendocrinol 22(1):13–23
Jolkkonen E, Pitkanen A (1998) Intrinsic connections of the rat amygdaloid complex: projections originating in the central nucleus. J Comp Neurol 395(1):53–72
Usunoff KG, Schmitt O, Itzev DE, Haas SJ, Lazarov NE, Rolfs A et al (2009) Efferent projections of the anterior and posterodorsal regions of the medial nucleus of the amygdala in the mouse. Cells Tissues Organs 190(5):256–285
Relkin R (1971) Relative efficacy of pinealectomy, hypothalamic and amygdaloid lesions in advancing puberty. Endocrinology 88(2):415–418
Bar-Sela M, Critchlow V (1966) Delayed puberty following electrical stimulation of amygdala in female rats. Am J Physiol 211(5):1103–1107
Ramaswamy S, Gibbs RB, Plant TM (2009) Studies of the localisation of kisspeptin within the pituitary of the rhesus monkey (Macaca mulatta) and the effect of kisspeptin on the release of non-gonadotropic pituitary hormones. J Neuroendocrinol 21(10):795–804
Rao YS, Mott NN, Pak TR (2011) Effects of kisspeptin on parameters of the HPA axis. Endocrine 39(3):220–228
Knobil E (1988) The hypothalamic gonadotrophic hormone releasing hormone (GnRH) pulse generator in the rhesus monkey and its neuroendocrine control. Hum Reprod 3(1):29–31
Bentsen AH, Ansel L, Simonneaux V, Tena-Sempere M, Juul A, Mikkelsen JD (2010) Maturation of kisspeptinergic neurons coincides with puberty onset in male rats. Peptides 31(2):275–283
Iwasa T, Matsuzaki T, Murakami M, Shimizu F, Kuwahara A, Yasui T et al (2008) Decreased expression of kisspeptin mediates acute immune/inflammatory stress-induced suppression of gonadotropin secretion in female rat. J Endocrinol Invest 31(7):656–659
Castellano JM, Bentsen AH, Romero M, Pineda R, Ruiz-Pino F, Garcia-Galiano D et al (2010) Acute inflammation reduces kisspeptin immunoreactivity at the arcuate nucleus and decreases responsiveness to kisspeptin independently of its anorectic effects. Am J Physiol Endocrinol Metab 299(1):E54–E61
Li XF, Kinsey-Jones JS, Knox AM, Wu XQ, Tahsinsoy D, Brain SD et al (2007) Neonatal lipopolysaccharide exposure exacerbates stress-induced suppression of luteinizing hormone pulse frequency in adulthood. Endocrinology 148(12):5984–5990
Iwasa T, Matsuzaki T, Murakami M, Kinouchi R, Ogata R, Kuwahara A et al (2009) Neonatal lipopolysaccharide exposure attenuates the homotypic stress-induced suppression of LH secretion in adulthood in male rat. Int J Dev Neurosci 27(4):345–349
Weiser MJ, Handa RJ (2009) Estrogen impairs glucocorticoid dependent negative feedback on the hypothalamic-pituitary-adrenal axis via estrogen receptor alpha within the hypothalamus. Neuroscience 159(2):883–895
Viau V, Meaney MJ (2004) Testosterone-dependent variations in plasma and intrapituitary corticosteroid binding globulin and stress hypothalamic-pituitary-adrenal activity in the male rat. J Endocrinol 181(2):223–231
Chen MD, Ordog T, O’Byrne KT, Goldsmith JR, Connaughton MA, Knobil E (1996) The insulin hypoglycemia-induced inhibition of gonadotropin-releasing hormone pulse generator activity in the rhesus monkey: roles of vasopressin and corticotropin-releasing factor. Endocrinology 137(5):2012–2021
Matsuzaki T, Iwasa T, Kinouchi R, Yoshida S, Murakami M, Gereltsetseg G et al (2011) Fasting reduces the kiss1 mRNA levels in the caudal hypothalamus of gonadally intact adult female rats. Endocr J 58(11):1003–1012
Mitchell JC, Li XF, Breen L, Thalabard JC, O’Byrne KT (2005) The role of the locus coeruleus in corticotropin-releasing hormone and stress-induced suppression of pulsatile luteinizing hormone secretion in the female rat. Endocrinology 146(1):323–331
Palanza P, Gioiosa L, Parmigiani S (2001) Social stress in mice: gender differences and effects of estrous cycle and social dominance. Physiol Behav 73(3):411–420
Hasen NS, O’Leary KA, Auger AP, Schuler LA (2010) Social isolation reduces mammary development, tumor incidence, and expression of epigenetic regulators in wild-type and p53-heterozygotic mice. Cancer Prev Res (Phila) 3(5):620–629
Hermes GL, Delgado B, Tretiakova M, Cavigelli SA, Krausz T, Conzen SD et al (2009) Social isolation dysregulates endocrine and behavioral stress while increasing malignant burden of spontaneous mammary tumors. Proc Natl Acad Sci U S A 106(52):22393–22398
Gonzalez CA, Coe CL, Levine S (1982) Cortisol responses under different housing conditions in female squirrel monkeys. Psychoneuroendocrinology 7(2–3):209–216
Shively CA (1998) Social subordination stress, behavior, and central monoaminergic function in female cynomolgus monkeys. Biol Psychiatry 44(9):882–891
Sapolsky RM, Alberts SC, Altmann J (1997) Hypercortisolism associated with social subordinance or social isolation among wild baboons. Arch Gen Psychiatry 54(12):1137–1143
Fox HE, White SA, Kao MH, Fernald RD (1997) Stress and dominance in a social fish. J Neurosci 17(16):6463–6469
Clarke FM, Faulkes CG (1997) Dominance and queen succession in captive colonies of the eusocial naked mole-rat, Heterocephalus glaber. Proc Biol Sci 264(1384):993–1000
Fernandez X, Meunier-Salaun MC, Mormede P (1994) Agonistic behavior, plasma stress hormones, and metabolites in response to dyadic encounters in domestic pigs: interrelationships and effect of dominance status. Physiol Behav 56(5):841–847
Alexander SL, Irvine CH (1998) The effect of social stress on adrenal axis activity in horses: the importance of monitoring corticosteroid-binding globulin capacity. J Endocrinol 157(3):425–432
Fano E, Sanchez-Martin JR, Arregi A, Castro B, Alonso A, Brain P et al (2001) Social stress paradigms in male mice: Variations in behavior, stress and immunology. Physiol Behav 73(1–2):165–173
Blanchard DC, Spencer RL, Weiss SM, Blanchard RJ, McEwen B, Sakai RR (1995) Visible burrow system as a model of chronic social stress: behavioral and neuroendocrine correlates. Psychoneuroendocrinology 20(2):117–134
Virgin CE Jr, Sapolsky RM (1997) Styles of male social behavior and their endocrine correlates among low-ranking baboons. Am J Primatol 42(1):25–39
Abbott DH, Hodges JK, George LM (1988) Social status controls LH secretion and ovulation in female marmoset monkeys (Callithrix jacchus). J Endocrinol 117(3):329–339
O’Byrne KT, Lunn SF, Dixson AF (1989) Naloxone reversal of stress-induced suppression of LH release in the common marmoset. Physiol Behav 45(5):1077–1080
Faulkes CG, Abbott DH, Jarvis JU, Sherriff FE (1990) LH responses of female naked mole-rats, Heterocephalus glaber, to single and multiple doses of exogenous GnRH. J Reprod Fertil 89(1):317–323
Zhou S, Holmes MM, Forger NG, Goldman BD, Lovern MB, Caraty A et al (2010) Release from socially-induced reproductive suppression in eusocial naked mole-rats (Heterocephalus glaber) is marked by increased kisspeptin-immunoreactive cell bodies in the hypothalamic anteroventral periventricular nucleus. Society for Neuroscience, San Diego, CA, Contract No.: 594.16/HHH29
Grone BP, Maruska KP, Korzan WJ, Fernald RD (2010) Social status regulates kisspeptin receptor mRNA in the brain of Astatotilapia burtoni. Gen Comp Endocrinol 169(1):98–107
Berga SL, Marcus MD, Loucks TL, Hlastala S, Ringham R, Krohn MA (2003) Recovery of ovarian activity in women with functional hypothalamic amenorrhea who were treated with cognitive behavior therapy. Fertil Steril 80(4):976–981
Williams NI, Berga SL, Cameron JL (2007) Synergism between psychosocial and metabolic stressors: impact on reproductive function in cynomolgus monkeys. Am J Physiol Endocrinol Metab 293(1):E270–E276
Herod SM, Pohl CR, Cameron JL (2011) Treatment with a CRH-R1 antagonist prevents stress-induced suppression of the central neural drive to the reproductive axis in female macaques. Am J Physiol Endocrinol Metab 300(1):E19–E27
Jayasena CN, Nijher GM, Chaudhri OB, Murphy KG, Ranger A, Lim A et al (2009) Subcutaneous injection of kisspeptin-54 acutely stimulates gonadotropin secretion in women with hypothalamic amenorrhea, but chronic administration causes tachyphylaxis. J Clin Endocrinol Metab 94(11):4315–4323
Young J, George JT, Tello JA, Francou B, Bouligand J, Guiochon-Mantel A et al (2012) Kisspeptin Restores Pulsatile LH Secretion in Patients with Neurokinin B Signaling Deficiencies: Physiological. Pathophysiological and Therapeutic Implications, Neuroendocrinology
Chen MD, O’Byrne KT, Chiappini SE, Hotchkiss J, Knobil E (1992) Hypoglycemic ‘stress’ and gonadotropin-releasing hormone pulse generator activity in the rhesus monkey: role of the ovary. Neuroendocrinology 56(5):666–673
Williams CL, Nishihara M, Thalabard JC, Grosser PM, Hotchkiss J, Knobil E (1990) Corticotropin-releasing factor and gonadotropin-releasing hormone pulse generator activity in the rhesus monkey. Electrophysiological studies. Neuroendocrinology 52(2):133–137
Dong Q, Salva A, Sottas CM, Niu E, Holmes M, Hardy MP (2004) Rapid glucocorticoid mediation of suppressed testosterone biosynthesis in male mice subjected to immobilization stress. J Androl 25(6):973–981
Puder JJ, Freda PU, Goland RS, Ferin M, Wardlaw SL (2000) Stimulatory effects of stress on gonadotropin secretion in estrogen-treated women. J Clin Endocrinol Metab 85(6):2184–2188
Tarin JJ, Hamatani T, Cano A (2010) Acute stress may induce ovulation in women. Reprod Biol Endocrinol 8:53
Cates PS, O’Byrne KT (2000) The area postrema mediates insulin hypoglycaemia-induced suppression of pulsatile LH secretion in the female rat. Brain Res 853(1):151–155
Spencer SJ, Buller KM, Day TA (2005) Medial prefrontal cortex control of the paraventricular hypothalamic nucleus response to psychological stress: possible role of the bed nucleus of the stria terminalis. J Comp Neurol 481(4):363–376
Hahn JD, Kalamatianos T, Coen CW (2003) Studies on the neuroanatomical basis for stress-induced oestrogen-potentiated suppression of reproductive function: evidence against direct corticotropin-releasing hormone projections to the vicinity of luteinizing hormone-releasing hormone cell bodies in female rats. J Neuroendocrinol 15(8):732–742
Beltramino C, Taleisnik S (1980) Dual action of electrochemical stimulation of the bed nucleus of the stria terminalis on the release of LH. Neuroendocrinology 30(4):238–242
Van Bockstaele EJ, Colago EE, Valentino RJ (1998) Amygdaloid corticotropin-releasing factor targets locus coeruleus dendrites: substrate for the co-ordination of emotional and cognitive limbs of the stress response. J Neuroendocrinol 10(10):743–757
Van Bockstaele EJ, Peoples J, Valentino RJ (1999) A.E. Bennett Research Award. Anatomic basis for differential regulation of the rostrolateral peri-locus coeruleus region by limbic afferents. Biol Psychiatry 46(10):1352–1363
Curtis AL, Bello NT, Connolly KR, Valentino RJ (2002) Corticotropin-releasing factor neurones of the central nucleus of the amygdala mediate locus coeruleus activation by cardiovascular stress. J Neuroendocrinol 14(8):667–682
Anselmo-Franci JA, Rocha-Barros VM, Franci CR, McCann SM (1999) Locus ceruleus lesions block pulsatile LH release in ovariectomized rats. Brain Res 833(1):86–92
Helena CV, Franci CR, Anselmo-Franci JA (2002) Luteinizing hormone and luteinizing hormone-releasing hormone secretion is under locus coeruleus control in female rats. Brain Res 955(1–2):245–252
Ma XM, Aguilera G (1999) Transcriptional responses of the vasopressin and corticotropin-releasing hormone genes to acute and repeated intraperitoneal hypertonic saline injection in rats. Brain Res Mol Brain Res 68(1–2):129–140
Vida B, Deli L, Hrabovszky E, Kalamatianos T, Caraty A, Coen CW et al (2010) Evidence for suprachiasmatic vasopressin neurones innervating kisspeptin neurones in the rostral periventricular area of the mouse brain: regulation by oestrogen. J Neuroendocrinol 22(9):1032–1039
Ten SC, Gu SY, Niu YF, An XF, Yan M, He M (2010) Central administration of kisspeptin-10 inhibits water and sodium excretion of anesthetized male rats and the involvement of arginine vasopressin. Endocr Res 35(3):128–136
Scott V, Brown CH (2011) Kisspeptin activation of supraoptic nucleus neurons in vivo. Endocrinology 152(10):3862–3870
Herbison AE (1992) Identification of a sexually dimorphic neural population immunoreactive for calcitonin gene-related peptide (CGRP) in the rat medial preoptic area. Brain Res 591(2):289–295
Harrigan EA, Magnuson DJ, Thunstedt GM, Gray TS (1994) Corticotropin releasing factor neurons are innervated by calcitonin gene-related peptide terminals in the rat central amygdaloid nucleus. Brain Res Bull 33(5):529–534
Dobolyi A, Irwin S, Makara G, Usdin TB, Palkovits M (2005) Calcitonin gene-related peptide-containing pathways in the rat forebrain. J Comp Neurol 489(1):92–119
Bowe JE, Li XF, Kinsey-Jones JS, Brain SD, Lightman SL, O’Byrne KT (2008) The role of corticotrophin-releasing hormone receptors in the calcitonin gene-related peptide-induced suppression of pulsatile luteinising hormone secretion in the female rat. Stress 11(4):312–319
Li XF, Bowe JE, Mitchell JC, Brain SD, Lightman SL, O’Byrne KT (2004) Stress-induced suppression of the gonadotropin-releasing hormone pulse generator in the female rat: a novel neural action for calcitonin gene-related peptide. Endocrinology 145(4):1556–1563
Dhillo WS, Small CJ, Jethwa PH, Russell SH, Gardiner JV, Bewick GA et al (2003) Paraventricular nucleus administration of calcitonin gene-related peptide inhibits food intake and stimulates the hypothalamo-pituitary-adrenal axis. Endocrinology 144(4):1420–1425
Li XF, Kinsey-Jones JS, Bowe JE, Wilkinson ES, Brain SD, Lightman SL et al (2009) A role for the medial preoptic area in CGRP-induced suppression of pulsatile LH secretion in the female rat. Stress 12(3):259–267
Kinsey-Jones JS, Li XF, Bowe JE, Brain SD, Lightman SL, O’Byrne KT (2005) Effect of calcitonin gene-related peptide on gonadotrophin-releasing hormone mRNA expression in GT1-7 cells. J Neuroendocrinol 17(9):541–544
Krajewski SJ, Anderson MJ, Iles-Shih L, Chen KJ, Urbanski HF, Rance NE (2005) Morphologic evidence that neurokinin B modulates gonadotropin-releasing hormone secretion via neurokinin 3 receptors in the rat median eminence. J Comp Neurol 489(3):372–386
Krajewski SJ, Burke MC, Anderson MJ, McMullen NT, Rance NE (2010) Forebrain projections of arcuate neurokinin B neurons demonstrated by anterograde tract-tracing and monosodium glutamate lesions in the rat. Neuroscience 166(2):680–697
Bowe JE, Li XF, Kinsey-Jones JS, Paterson S, Brain SD, Lightman SL et al (2005) Calcitonin gene-related peptide-induced suppression of luteinizing hormone pulses in the rat: the role of endogenous opioid peptides. J Physiol 566(Pt 3):921–928
Kinsey-Jones JS, Grachev P, Li XF, Lin YS, Milligan SR, Lightman SL et al (2012) The inhibitory effects of neurokinin B on GnRH pulse generator frequency in the female rat. Endocrinology 153(1):307–315
Ducret E, Anderson GM, Herbison AE (2009) RFamide-related peptide-3, a mammalian gonadotropin-inhibitory hormone ortholog, regulates gonadotropin-releasing hormone neuron firing in the mouse. Endocrinology 150(6):2799–2804
Wu M, Dumalska I, Morozova E, van den Pol AN, Alreja M (2009) Gonadotropin inhibitory hormone inhibits basal forebrain vGluT2-gonadotropin-releasing hormone neurons via a direct postsynaptic mechanism. J Physiol 587(Pt 7):1401–1411
Johnson MA, Tsutsui K, Fraley GS (2007) Rat RFamide-related peptide-3 stimulates GH secretion, inhibits LH secretion, and has variable effects on sex behavior in the adult male rat. Horm Behav 51(1):171–180
Clarke IJ, Qi Y, Puspita Sari I, Smith JT (2009) Evidence that RF-amide related peptides are inhibitors of reproduction in mammals. Front Neuroendocrinol 30(3):371–378
Pineda R, Garcia-Galiano D, Sanchez-Garrido MA, Romero M, Ruiz-Pino F, Aguilar E et al (2010) Characterization of the inhibitory roles of RFRP3, the mammalian ortholog of GnIH, in the control of gonadotropin secretion in the rat: in vivo and in vitro studies. Am J Physiol Endocrinol Metab 299(1):E39–E46
Caraty A, Blomenrohr M, Vogel GM, Lomet D, Briant C, Beltramo M (2012) RF9 powerfully stimulates gonadotrophin secretion in the ewe: Evidence for a seasonal threshold of sensitivity. J Neuroendocrinol 24(5):725–736
Clarke IJ (2011) Control of GnRH secretion: one step back. Front Neuroendocrinol 32(3):367–375
Yano T, Iijima N, Kakihara K, Hinuma S, Tanaka M, Ibata Y (2003) Localization and neuronal response of RFamide related peptides in the rat central nervous system. Brain Res 982(2):156–167
Qi Y, Oldfield BJ, Clarke IJ (2009) Projections of RFamide-related peptide-3 neurones in the ovine hypothalamus, with special reference to regions regulating energy balance and reproduction. J Neuroendocrinol 21(8):690–697
Kaewwongse M, Takayanagi Y, Onaka T (2011) Effects of RFamide-related peptide (RFRP)-1 and RFRP-3 on oxytocin release and anxiety-related behaviour in rats. J Neuroendocrinol 23(1):20–27
Kirby ED, Geraghty AC, Ubuka T, Bentley GE, Kaufer D (2009) Stress increases putative gonadotropin inhibitory hormone and decreases luteinizing hormone in male rats. Proc Natl Acad Sci U S A 106(27):11324–11329
Kageyama K, Hasegawa G, Akimoto K, Yamagata S, Tamasawa N, Suda T (2012) Differential regulation of gonadotropin-releasing hormone by corticotropin-releasing factor family peptides in hypothalamic N39 cells. Peptides 33(1):149–155
Clarkson J, Herbison AE (2006) Development of GABA and glutamate signaling at the GnRH neuron in relation to puberty. Mol Cell Endocrinol 254–255:32–38
Sliwowska JH, Billings HJ, Goodman RL, Lehman MN (2006) Immunocytochemical colocalization of GABA-B receptor subunits in gonadotropin-releasing hormone neurons of the sheep. Neuroscience 141(1):311–319
Akema T, He D, Sugiyama H (2005) Lipopolysaccharide increases gamma-aminobutyric acid synthesis in medial preoptic neurones in association with inhibition of steroid-induced luteinising hormone surge in female rats. J Neuroendocrinol 17(10):672–678
Sirivelu MP, Burnett R, Shin AC, Kim C, MohanKumar PS, MohanKumar SM (2009) Interaction between GABA and norepinephrine in interleukin-1beta-induced suppression of the luteinizing hormone surge. Brain Res 1248:107–114
Bowers G, Cullinan WE, Herman JP (1998) Region-specific regulation of glutamic acid decarboxylase (GAD) mRNA expression in central stress circuits. J Neurosci 18(15):5938–5947
Lin YS, Li XF, Shao B, Hu MH, Goundry AL, Jeyaram A et al (2012) The role of GABAergic signalling in stress-induced suppression of gonadotrophin-releasing hormone pulse generator frequency in female rats. J Neuroendocrinol 24(3):477–488
Cravo RM, Margatho LO, Osborne-Lawrence S, Donato J Jr, Atkin S, Bookout AL et al (2011) Characterization of Kiss1 neurons using transgenic mouse models. Neuroscience 173:37–56
Terasawa E, Kurian JR, Guerriero KA, Kenealy BP, Hutz ED, Keen KL (2010) Recent discoveries on the control of gonadotrophin-releasing hormone neurones in nonhuman primates. J Neuroendocrinol 22(7):630–638
Keen KL, Burich AJ, Mitsushima D, Kasuya E, Terasawa E (1999) Effects of pulsatile infusion of the GABA(A) receptor blocker bicuculline on the onset of puberty in female rhesus monkeys. Endocrinology 140(11):5257–5266
Neal-Perry G, Lebesgue D, Lederman M, Shu J, Zeevalk GD, Etgen AM (2009) The excitatory peptide kisspeptin restores the luteinizing hormone surge and modulates amino acid neurotransmission in the medial preoptic area of middle-aged rats. Endocrinology 150(8):3699–3708
Leng G, Ludwig M (2006) Jacques Benoit Lecture. Information processing in the hypothalamus: peptides and analogue computation. J Neuroendocrinol 18(6):379–392
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2013 Springer Science+Business Media, LLC
About this chapter
Cite this chapter
Grachev, P., Li, X.F., O’Byrne, K. (2013). Stress Regulation of Kisspeptin in the Modulation of Reproductive Function. In: Kauffman, A., Smith, J. (eds) Kisspeptin Signaling in Reproductive Biology. Advances in Experimental Medicine and Biology, vol 784. Springer, New York, NY. https://doi.org/10.1007/978-1-4614-6199-9_20
Download citation
DOI: https://doi.org/10.1007/978-1-4614-6199-9_20
Published:
Publisher Name: Springer, New York, NY
Print ISBN: 978-1-4614-6198-2
Online ISBN: 978-1-4614-6199-9
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)