Abstract
Type 1 diabetes mellitus is a complex autoimmune disease process encompassing a number of stages, the most significant of which is the loss of immunological tolerance and the initiation of immune dysfunction resulting in the selective destruction of pancreatic β cells. Although exogenous insulin therapy has proven efficacious, it does not address the underlying cause of the disease. A treatment strategy encompassing immunosuppressive and β cell replacement therapy that will promote immunological tolerance, without toxicity or the induction of lymphopenia is required for treatment of patients with hypoglycaemic unawareness. Importantly, this combination strategy must harness a therapy that provides a replacement source of insulin producing β cells without toxic side-effects associated with long term immunosuppression and induces tolerance to the replacement β cells in order to prevent destruction by allo- and autoreactive T cells. Here we discuss the current immunosuppressive therapies and potential sources of replacement β cells and review the pitfalls in current combined immunosuppression and islet transplant therapy. Finally we examine possible combination strategies including stem cells that are likely to succeed in fulfilling the above criteria for the treatment of diabetes in the future.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
1 Introduction
Type I diabetes mellitus (T1DM) is an autoimmune disease in which autoreactive T cells target the pancreatic insulin producing β cells. Destruction of β cells leads to insulin paucity, blood glucose dysregulation and subsequent hyperglycaemia which in turn result in a number of long term micro and macro-vascular complications [1]. Diabetes is fast becoming a common childhood disease with the incidence set to double in children under the age of 5 by 2020 [2]. On a global scale, the World Health Organisation (WHO) estimate that 220 million people suffer from diabetes worldwide, a number which is set to increase two fold by 2030. The costs of treatment and the clinical management of the associated complications are substantial. The need for a preventative or regenerative therapy is perhaps at its most urgent since the discovery and development of insulin in the 1920s by Banting, Best, Collip and Macleod. Existing therapies include insulin therapy, cell-based therapy and solid organ transplantation as well as immunotherapy [3]. Although insulin therapy revolutionised the treatment of diabetes, there are limitations, particularly in the group of patients with hypoglycaemic unawareness. As insulin therapy does not address the cause of the disease, there is need for a therapy which has the capacity to address the autoimmune response, the replacement of insulin producing β cells and, if necessary, the problem of alloreactivity evoked by the replacement therapy.
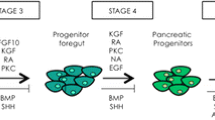
A combination of genetic susceptibility [4] and environmental factors trigger changes in the immune system leading to immune dysregulation and subsequent autoimmunity accompanied by the development of islet specific autoantibodies and autoreactive T cells. The disease process starts with genetic susceptibility [4] (stage 1) followed by triggering events (stage 2). Immune dysregulation and environmental triggering (stage 3) are followed by the loss of β cell function detected by abnormal glucose tolerance test (stage 4). At diabetes onset (stage 5) almost 80 % of the beta cells are already lost. The final stage of this process (stage 6) is the total loss of β cells with patients dependent on insulin therapy for survival [5] (Fig. 16.1).
Stages of Type 1 Diabetes. Diabetes is thought to be initiated by interactions between genetic susceptibility and environmental factors (1). Evidence suggests that triggering events such as enterovirus infection contribute to the pathogenesis of T1DM (2). Loss of immunological tolerance coincides with immune dysregulation (3) resulting in the activation of autoreactive T cells and subsequent destruction of β cells leading to loss of β cell function (4) and significantly decreased β cell mass signifying the onset of diabetes (5) which inevitably results in insulin dependence (6). Treatments are specifically targeted to stage (3) using immunosuppressive tolerance induction strategies and importantly stage (4/5) utilising β cell replacement therapy in an attempt to prevent insulin dependence
2 Current Therapeutic Strategies for Type 1 Diabetes Mellitus
A number of potential therapeutics have been investigated in preclinical models of diabetes with many demonstrating efficacy in prevention or reversal of T1DM, however, in the majority of cases, these results do not extrapolate to humans. Factors including variations in genetic predisposition, environmental triggers as well as inter-individual heterogeneity in disease pathogenesis all effect therapeutic outcomes [6–8]. Additionally, a major issue concerning the current replacement therapy for T1DM, namely islet or pancreas transplantation, is the problem of recurrent autoreactive T cells [9] which seem to be resistant to suppression by conventional immunosuppressive drugs. Here we discuss the immunotherapies and potential sources of β cells for the treatment of diabetes patients focussing on the possibility of combination therapies of immunosuppressive agents that will effectively address autoimmunity and alloreactivity (Fig. 16.2).
Strategies of combination therapy for T1DM. The onset of diabetes is thought to be initiated by multiple factors involving genetic and environmental factors as well as triggering events which induce β cell death, initiating the process of autoimmunity—in which autoantigen and autoreactive T cells play a key role. Current therapy consisting of donor allogeneic islet transplant and conventional immunosuppressive drugs induce a state of leukopenia and promotes the homeostatic expansion and activation of pre-existing autoreactive T cells that target the transplanted islets for destruction and result in graft failure. Future therapy involving an ES cell, iPS cell or adult stem cell-derived β cell source in conjunction with a combination immunotherapy consisting of anti-CD3, MSCs, Treg, autoantigen therapy or non-depleting immunosuppressive drugs may provide a more successful outcome through avoidance of leukopenia and induction of tolerance
3 Immunotherapy
3.1 Global Immunosuppression
Randomised trials initiated in the 1980s tested the effects of global immunosuppressive drugs in modulating autoimmune diabetes, including cyclosporine [10, 11], azathioprine alone [12], or in combination with prednisone [13], anti-thymocyte globulin and prednisone [14] and rituximab (humanised monoclonal antibody (mAb) specific for CD20) [15]. All of these strategies led to improved endogenous β cell function and a decrease in insulin requirements in patients with new onset diabetes. However, the beneficial effects were limited to the duration of the treatment and the side effects associated with cyclosporine in particular [16] suggested that global immunosuppressive therapy alone was unsuitable for treatment of T1DM.
The standard immunosuppression used in whole pancreas transplantation can vary between different centres, however, a protocol involving thymoglobulin as induction, with tacrolimus, mycophenolate mofetil (MMF) and prednisone for maintenance therapy, results in 80–85 % of grafts maintaining function after 1 year [17]. In contrast, utilisation of the Edmonton immunosuppressive protocol (optimised over a number of years) in conjunction with transplantation of allogeneic human islets has proven successful in rendering 100 % of patients (n = 7) with T1DM insulin independent for at least 1 year and provides a prime example of the potential of immunosuppressive drugs (discussed in more detail below) [18].
3.2 Antigen-Specific Therapies
A number of diabetes related autoantigens including insulin, pro-insulin, insulin peptides, glutamic acid decarboxylase (GAD) and hsp60 and hsp peptides p277 have been utilised in tolerance induction strategies. The NOD mouse has provided a useful platform to test the efficacy of antigen-specific therapy in diabetes. Studies have demonstrated the ability of exogenous insulin, pro-insulin or insulin peptides delivered orally, subcutaneously, or intranasally to prevent or suppress diabetes [19–23]. Delivery of GAD [24–27] or hsp60 and hsp60 p277 peptide [28, 29] through similar routes, also revealed promising results in NOD mice. Extrapolation of these antigen-specific therapies from the NOD mouse into human clinical trials has, however, proven difficult. Trials performed in new onset diabetes patients using oral insulin or an altered peptide ligand of the 9–23 insulin B chain peptide (NBI-6,024) demonstrated no effect [30, 31].
3.3 T cell and Co-Stimulation Targeting Agents
A number of monoclonal antibodies targeting CD3, CD4, CD8 and αβ T cells as well as major histocompatibility complex (MHC) class II, CD28 and CD154 have been examined for their capacity to prevent or reverse T1DM [32–38]. However, among these; anti-CD3 therapy has prevailed as the most promising so far.
3.4 Anti-CD3 Therapy
Anti-CD3 mAb therapy has successfully induced a permanent state of disease remission in a rodent model of T1DM. In these studies antigen-specific tolerance was induced with mice regaining full immune competence after a few weeks of treatment [33, 39]. Clinical trials tested the efficacy of two humanised Fc engineered monoclonal anti-CD3 antibodies called teplizumab (Hokt3γ1 (Ala-Ala)) [40, 41] and otelixizumab (ChAglyCD3) [42, 43]. A multi-centre, Phase II placebo-controlled trial consisting of 80 patients with new onset T1DM receiving a 6 day treatment of either otelixizumab or placebo was carried out. This trial demonstrated that the anti-CD3 antibody preserved β cell function. Patients receiving the antibody maintained significantly higher levels of endogenous insulin secretion than placebo controls at 6, 12, 18 and 48 months after treatment [42, 43]. However, after 24 months, the beneficial effect diminished over time with a decline in β cell function and increase in insulin dependence [43]. Similar results were observed in the teplizumab trail which entailed a 12 or 14 day mAb treatment with 2–4 days of incremental dose escalation to 10 days of a full dose of drug mAb. There were significant improvements in C-peptide responses accompanied by reduced haemoglobin A1c (HbA1c) and insulin requirements in patients receiving the mAb, however, the effects waned after 2 years [40]. Furthermore a small open labelled phase IIb clinical trial demonstrated that a higher dose (40 % higher) of teplizumab resulted in increased adverse events without an improved efficacy of the drug [44].
It seems likely that autoreactivity was only transiently suppressed in these trials leading to the subsequent loss of additional β cells and the increased requirement for exogenous insulin with time after cessation of the therapy. A study carried out by Albamunits et al. clearly demonstrated that β cell replication is reduced after immune therapy using an anti-CD3 mAb resulting in progressive loss of β cell mass [45], similar to the functional decline observed in humans after treatment with anti-CD3 [43]. The mode of action of the anti-CD3 mAb remains unclear but alteration of lymphocyte migration or trafficking, rather than depletion, has been suggested [44].
Although this therapy has been the most promising to date, it is likely that a combination of immunomodulatory agents coupled with a β cell replacement strategy (or β cell regeneration strategy in patients with a small but sufficient β cell mass) will be more efficacious in addressing the multiple factors associated with current allogeneic islet transplantation and future β cell replacement providing a more successful outcome.
3.5 Regulatory T cell Therapy
Autoimmune diabetes manifests from the loss of immunological tolerance. T1DM patients as well as NOD mice, exhibit a decreased frequency of regulatory T cells (Treg) with alterations in function [46–49] and IL-2/IL-2R signalling pathway [50]. There is evidence to suggest that NOD mice have Treg that prevent diabetes development early on, but the functional capacity of the Treg is lost over time [51], allowing dysregulated autoimmune attack of insulin producing β cells [52, 53]. Similarly, Treg cells taken from peripheral blood of T1DM patients also exhibit defective suppressive functions in vitro [54].
Although it seems likely that endogenous naturally occurring Treg are functionally defective in diabetic mice, adaptive Treg present in NOD mice have been shown to suppress autoreactive T cells mediated by TGF-β [51] and therefore represent a possible target for tolerance induction in vivo. Treatment with anti-CD3ε antibody induced tolerance in NOD mice through the activation of adaptive Treg in a TGF-β-dependent manner [55], highlighting the possibility of driving a tolerance induction pathway through mAbs. TGF-β-producing Treg have also been implicated in tolerance induction strategies involving immunisation with plasmid DNA encoding GAD65, IL-4 and IL-10 [56] in a NOD mouse model.
The other option available involving Treg therapy, is the selective ex vivo expansion of polyclonal or antigen-specific Treg [57]. Tang et al. [58] have demonstrated that in vitro expanded antigen-specific Treg cells suppress autoimmune diabetes in the NOD mouse with greater potency than expanded polyclonal Treg. Utilising a humanised mouse model, our lab has demonstrated the capacity of ex vivo expanded human Treg to prevent rejection of a life sustaining human islet allograft in streptozotocin induced diabetic mice (Wu, Wieckiewicz and Wood unpublished results). The data from animal models of diabetes supports the use of human Treg in the treatment of autoimmune diabetes, however, the major discrepancy is the ability to generate human antigen-specific Treg directed against autoantigen. Additionally, although Treg have proven efficacious in the NOD mouse, extrapolation to the clinic will not be without difficulty and it is likely that a combination therapy of Treg and a short-acting immunosuppressive drug like anti-CD3 may be efficacious in breaking autoimmunity or preventing islet/stem cell-derived β cell rejection.
3.6 Mesenchymal Stem Cells
Mesenchymal Stem Cells (MSCs) are adult stem cells found within the bone marrow (as well as many other tissues and organs) whose primary functions are to provide stromal support for hematopoietic stem cells and to act as a reservoir for the continuous turnover of mesenchymal lineages under regular conditions. Moreover, MSCs possess immunosuppressive characteristics which make these cells an attractive source for cellular immunotherapy both in transplantation and autoimmunity settings.
In the context of autoimmunity, MSCs have been shown to be efficacious in suppressing autoreactive T cell responses in mouse models of colitis [59], experimental autoimmune encephalomyelitis (EAE) [60] and collagen induced arthritis (CIA) [61] among others.
Furthermore, MSCs have proven therapeutically beneficial in a mouse model of T1DM [62, 63]. Administration of MSCs derived from BALB/c or non-obese resistant strain but not non-obese diabetic (NOD) mice, delayed diabetes onset in pre-diabetic recipients. This delay in disease onset was thought to be associated with the expression of PD-L1 by MSCs and the promotion of a Th2 type response in treated NOD mice [62]. Importantly, this study highlights the important fact that MSCs isolated from diabetic patients may not have the same immunosuppressive capacity as MSCs from healthy patients and, therefore, use of allogeneic MSCs may need to be considered in this case.
Considerable evidence supports the ability of MSCs to prevent allogeneic graft rejection [64]. A number of in vivo studies demonstrate the ability of MSCs to suppress alloreactive responses both in skin and heart allograft models [65, 66]. In a fully MHC-mismatched baboon skin transplant model, a single dose of donor MSCs administered intravenously resulted in prolonged skin graft survival (11.3 ± 0.3 days compared to 7.0 days in untreated controls). However, this effect was non-specific as third party grafts were also prolonged in a similar time scale [65]. Casiraghi and colleagues report that both donor and recipient derived MSCs have the capacity to prolong cardiac allograft survival in a semi-allogeneic but not a fully MHC-mismatched cardiac allograft model. Protection of cardiac allografts was associated with the expansion of Treg cells and the abrogation of anti-donor Th1 activity. Significantly, this study highlighted the differences between donor and recipient derived MSCs and shows that pre-transplant intraportal administration of a single dose of MSCs proved more efficacious than the intravenous route [66]. Unfortunately, this is not something that we can test in human subjects and therefore we must learn what we can from the successful use of MSCs in steroid refractory graft versus host disease (GvHD) patients, which involves intravenous administration of MSCs of autologous or allogeneic origin [67].
The capacity of MSCs to prevent donor allogeneic islet graft rejection was investigated utilising a life-preserving mouse islet allograft model. This streptozotocin induced diabetes model allowed us to examine the effect of MSCs in suppressing an alloreactive effector T cell attack on transplanted allogeneic islets in an immunodeficient mouse. In the absence of MSCs, donor allogeneic islet grafts were rejected with a mean survival time of 30 days, however, in the presence of MSCs islet grafts were maintained long term with stable normoglycemia. The ability of MSCs to prevent rejection in this study is likely an attribute of co-localisation of MSCs with the islet graft associated with the provision of a local immunosuppressive milieu by MSCs in the locality of the islet graft. In this local microenvironment MSCs produce soluble factors, in particular MMP-2 and 9 which impair alloreactive T cell activation and expansion [68].
In addition to suppression of autoreactivity, MSCs also potently modulate alloantigen specific responses and thus provide a promising therapeutic strategy for the treatment of type 1 diabetes. MSCs are unique as a cellular therapy in that they have the capacity to address both the problem of autoimmunity and alloreactivity against a cell replacement therapy for diabetes patients. However, although MSC therapy has shown much promise in controlling both allo- and autoreactivity, there is little doubt that MSCS therapy alone will not be sufficient and will likely be more efficacious as a combination therapy; with a single dose of, for example, anti-CD3.
4 β Cell Replacement Therapy
4.1 Islet Transplantation
By far the most forward-moving of the cell replacement therapies is allogeneic islet therapy, which involves the transplantation of deceased donor-derived islets percutaneously into the portal vein of the liver, combined with immunosuppressive drugs. Islet therapy has recently improved in efficacy through introduction of the Edmonton protocol [18]. The success of the Edmonton team involved an improved islet isolation technique combined with infusion of large numbers of freshly isolated islets. In addition, an altered immunosuppressive regimen avoiding steroids (glucocorticoid therapy), and combining a reduced dose of tacrolimus (a calcineurin inhibitor which can inhibit insulin secretion) with the addition of sirolimus (mTOR inhibitor) [18] was implemented. Under this regimen, 68 % of patients receiving islet allografts maintained insulin independence at year 1. Unfortunately, insulin independence was not sustained long term with less than 10 % of patients remaining insulin independent at year 5. However, 80 % of patients had measurable levels of C-peptide indicating the continuous low level production of insulin [69], which allows improved glycemic control. The benefits associated with islet transplantation although small, supports the utility of this procedure in a select group of patients experiencing hypoglycaemic unawareness (patients who have lost significant β cell mass). Problems associated with this therapy are the inefficient isolation procedure and the requirement of at least two pancreatic donors, for which there are simply not enough donors available. This lack of islet tissue has lead to the proposed use of adult, embryonic or induced pluripotent stem (iPS) cells for replacement therapy.
4.2 Embryonic Stem Cells
Embryonic stem (ES) cells are pluripotent cells derived from the inner cell mass of the blastocyst with the capacity for unlimited self-renewal in an undifferentiated state, and the ability to undergo induced differentiation into all three germ layers in vitro and in vivo. The ability of mouse ES cells to differentiate in vitro into functional insulin producing cells or islet like clusters which can recover and maintain normoglycemia in streptozotocin-induced diabetic mice has been demonstrated by a number of groups [70, 71]. Human ES cell differentiation into insulin producing cells has proven more difficult due to an inability of ES cells to generate definitive endoderm. However, Baetge’s group have generated a protocol that promotes differentiation of human ES cell derived endodermal cells into cells expressing pancreatic markers [72]. Although this protocol did not lead to glucose responsive insulin producing cells in vitro, implantation of human ESC derived—endodermal derived—insulin positive cells in immunodeficient mice resulted in the production of insulin in response to glucose several months after transplantation [73]. This study was the first of its kind to demonstrate that insulin producing cells derived from human ES cells could maintain normoglycemia in a mouse model of streptozotocin-induced diabetes. However, this study also highlights the fact that further research is required in order to fully optimise the differentiation protocol and to ensure phenotypically and functionally stable insulin producing cells are induced.
Importantly, the issues that these studies do not address is that of autoimmune and alloreactive attack. In the case of alloreactivity against ES cell-derived tissue, it is likely that these cells/tissues will be recognised as foreign and subsequently rejected by the immune response. The immune response directed against fully differentiated insulin producing tissue derived from mouse ES cells was examined using a mouse model of streptozotocin-induced diabetes. In this study, functional insulin producing cells were rejected in immunocompetent hosts and this response was mediated primarily by T cells [74] with evidence for involvement of both innate and adaptive components of the immune system [75–77] .
4.3 Induced Pluripotent Stem cells
Ground breaking research describing the factors required to reprogram adult cells back into iPS cells in 2006 [78] has paved the way for tissue engineering and therapeutic application. Initial problems concerning homogeneity and efficiency of the reprogramming process are now being addressed promptly by a number of groups. However, clinical application of iPS cell-derived tissue remains a long way off with safety concerns regarding the stability of the cells in vivo and the possibility of tumour formation. Recently Tateishi et al. reported that human iPS cells derived from skin fibroblasts could be differentiated into islet like clusters, which expressed insulin. Of four iPS cell lines, two differentiated into islet like cell clusters and one of these released low levels of C-peptide in response to glucose stimulation [79]. iPS cells have also been derived from adult cells from patients with disease and one group have reported the differentiation of skin biopsy-derived iPS cells into insulin producing cells. This study was more convincing with evidence that cells released human C-peptide (5 fold increase) in response to glucose stimulation, suggesting that insulin producing cells were functional [80].
4.4 Adult Stem Cells
Bone marrow-derived cells can differentiate into a number of lineages and have been demonstrated to play a role in regeneration and repair and therefore represent an attractive source for tissue engineering in T1DM. Transplantation of bone marrow-derived cells into streptozotocin-treated mice led to the instigation of endogenous pancreatic tissue regeneration resulting in insulin production and improved survival [81]. In contrast, a number of studies have suggested that bone marrow-derived cells differentiated into insulin positive cells, however, the stem cell community is still not convinced that this lineage switch is possible. Nonetheless, two studies in particular have demonstrated that bone marrow-derived islet like clusters transplanted into streptozotocin induced diabetic rodents have the capacity to control blood glucose and maintain normoglycemia which was reversed after removal of the graft [82, 83].
Umbilical cord blood has stimulated interest both as an immunomodulatory therapy and as a potential source of insulin producing cells for use in T1DM. Islet like clusters derived from human Wharton’s jelly MSCs in umbilical cord matrix produced low levels of insulin and have some effect in controlling blood glucose and maintaining normoglycemia in vivo [84]. Overall, it seems likely that adult stem cells may have the capacity to differentiate into insulin producing islet like cells, however, the process of trans-differentiation is as yet an unproven phenomenon and therefore it is unlikely that adult cells will provide the most useful/optimal source of replacement β cells.
5 Strategies to Address Autoimmunity in β Cell Replacement Therapy
The prevailing issues that need to be addressed in the treatment of T1DM with β cell replacement therapy are the presence of autoreactive T and B cells specific for islet cell antigens (autoantigens), as well as lymphocytes with the capacity to respond to mismatched MHC antigens (alloantigens) of the β cell donor. Additionally, depending on the source of β cells, there may be other antigens, as in the case of ES cell-derived β cells which could evoke immune activation; for example ES and iPS cells express surface antigens that disappear at later stages of development and which are not expressed by adult cells [85, 86]. Graft failure has been reported in a minority of transplant patients and has been attributed to chronic rejection. However, another reason for graft failure is the recurrence of autoimmunity which was initially described in patients receiving pancreas graft from HLA-identical siblings with no or reduced immunosuppression [87, 88]. A large study examining 100 grafts described autoimmune diabetes recurrence in ~10 % of patients receiving donor grafts with immunosuppression [89]. More recently, the recurrence of T1DM after simultaneous pancreas-kidney transplantation, despite the use of immunosuppressive drugs, was reported to be associated with both autoantibodies and autoreactive T cells [9]. Furthermore, conventional immunosuppressive drugs currently used in allogeneic donor islet transplantation prevent rejection through the depletion of leukocytes. The immune system responds to this through production of common γ chain cytokines IL-7 and IL-15 which stimulate the expansion of any remaining lymphocytes in an effort to restore homeostasis [90–92]. This effect also results in the expansion of pre-existing autoreactive cells and can lead to destruction of transplanted islets [93, 94]. Indeed, the production of IL-7 was shown to promote the expansion of auto-reactive T cells in response to a lymphopenic environment [93]. Moreover, examination of the serum from T1DM patients after islet transplant, revealed the presence of increased concentrations of IL-7 and IL-15 [95]. There is some evidence to suggest that certain immunosuppressive drugs will promote homeostatic proliferation while others may inhibit it. Two patients receiving MMF plus tacrolimus in place of sirolimus plus tacrolimus (due to sirolimus intolerance) displayed reduced proliferation with no change in IL-7 expression, indicative of the capacity of MMF, but not sirolimus, to block cell proliferation [95]. This phenomenon was also observed in 3 patients who received kidney-pancreas transplant with anti-thymocyte globulin induction therapy followed by MMF plus cyclosporine A (CyA) or FK506 maintenance therapy [95], demonstrating that the immunosuppressive therapy utilised may impact on the outcome of islet or β cell replacement therapy [96].
A poor clinical outcome has also been associated with the presence of islet specific autoantibodies [97] indicating that assessment of autoantibodies present before transplant of replacement β cells will be important in the choice of (patient tailored) immunosuppressive therapy.
6 Conclusion
Although significant progress has been made in the field of immunotherapy to halt autoimmune T1DM, the development for a combination therapy encompassing both immunotherapy and β cell replacement therapy (currently donor islet transplantation but stem cell-derived β cell tissue in the future) has been somewhat elusive. Encouragingly, there are already a number of promising therapies available targeted at autoimmune diabetes, which, if combined, could provide a very successful therapy, the key to which is undoubtedly a tolerance induction strategy.
In summary, the issues which need to be addressed in the quest for this optimal therapy are (1) evaluation of the presence and scale of pre-existing autoreactive T cells in patients before transplant of replacement β cells; (2) examination of the effect of new immunosuppressive regimens on the activation and expansion of pre-existing autoreactive T cells after transplant and (3) development of new therapeutic agents that have the capacity to prevent rejection and regulate the pre-existing autoimmune response without inducing profound leukopenia.
References
Moore DJ, Gregory JM, Kumah-Crystal YA et al (2009) Mitigating micro-and macro-vascular complications of diabetes beginning in adolescence. Vasc Health Risk Manag 5:1015–1031
Patterson CC, Dahlquist GG, Gyurus E et al (2009) Incidence trends for childhood type 1 diabetes in Europe during 1989–2003 and predicted new cases 2005–20: a multicentre prospective registration study. Lancet 373:2027–2033
Powers AC (2008) Insulin therapy versus cell-based therapy for type 1 diabetes mellitus: what lies ahead? Nat Clin Pract Endocrinol Metab 4:664–665
Nejentsev S, Howson JM, Walker NM et al (2007) Localization of type 1 diabetes susceptibility to the MHC class I genes HLAHLA-B and HLA-A. Nature 450:887–892
Gianani R, Eisenbarth GS (2005) The stages of type 1A diabetes: 2005. Immunol Rev 204:232–249
Bruno G, Cerutti F, Merletti F et al (2005) Residual beta-cell function and male/female ratio are higher in incident young adults than in children: the registry of type 1 diabetes of the province of Turin, Italy, 1984–2000. Diabetes Care 28:312–317
Sabbah E, Savola K, Ebeling T et al (2000) Genetic, autoimmune, and clinical characteristics of childhood- and adult-onset type 1 diabetes. Diabetes Care 23:1326–1332
Valdes AM, Thomson G, Erlich HA et al (1999) Association between type 1 diabetes age of onset and HLAHLA among sibling pairs. Diabetes 48:1658–1661
Vendrame F, Pileggi A, Laughlin E et al (2010) Recurrence of type 1 diabetes after simultaneous pancreas-kidney transplantation, despite immunosuppression, is associated with autoantibodies and pathogenic autoreactive CD4 T-cells. Diabetes 59:947–957
Bougneres PF, Carel JC, Castano L et al (1988) Factors associated with early remission of type I diabetes in children treated with cyclosporine. N Engl J Med 318:663–670
Stiller CR, Dupre J, Gent M et al (1984) Effects of cyclosporine immunosuppression in insulin-dependent diabetes mellitus of recent onset. Science 223:1362–1367
Harrison LC, Colman PG, Dean B et al (1985) Increase in remission rate in newly diagnosed type I diabetic subjects treated with azathioprine. Diabetes 34:1306–1308
Silverstein J, Maclaren N, Riley W et al (1988) Immunosuppression with azathioprine and prednisone in recent-onset insulin-dependent diabetes mellitus. N Engl J Med 319:599–604
Eisenbarth GS, Srikanta S, Jackson R et al (1985) Anti-thymocyte globulin and prednisone immunotherapy of recent onset type 1 diabetes mellitus. Diabetes Res 2:271–276
Pescovitz MD, Greenbaum CJ, Krause-Steinrauf H et al (2009) Rituximab, B-lymphocyte depletion, and preservation of beta-cell function. N Engl J Med 361:2143–2152
Parving HH, Tarnow L, Nielsen FS et al (1999) Cyclosporine nephrotoxicity in type 1 diabetic patients. A 7-year follow-up study. Diabetes Care 22:478–483
Cicero A, Lappin JA (2010) Pancreas transplantation: experience at University of Texas, Houston. Transplant Proc 42:314–316
Shapiro AM, Lakey JR, Ryan EA et al (2000) Islet transplantation in seven patients with type 1 diabetes mellitus using a glucocorticoid-free immunosuppressive regimen. N Engl J Med 343:230–238
Bergerot I, Ploix C, Petersen J et al (1997) A cholera toxoid-insulin conjugate as an oral vaccine against spontaneous autoimmune diabetes. Proc Natl Acad Sci USA 94:4610–4614
Daniel D, Wegmann DR (1996) Protection of nonobese diabetic mice from diabetes by intranasal or subcutaneous administration of insulin peptide B-(9–23). Proc Natl Acad Sci USA 93:956–960
Harrison LC, Dempsey-Collier M, Kramer DR et al (1996) Aerosol insulin induces regulatory CD8 gamma delta T cells that prevent murine insulin-dependent diabetes. J Exp Med 184:2167–2174
Karounos DG, Bryson JS, Cohen DA (1997) Metabolically inactive insulin analog prevents type I diabetes in prediabetic NOD mice. J Clin Invest 100:1344–1348
Zhang ZJ, Davidson L, Eisenbarth G et al (1991) Suppression of diabetes in nonobese diabetic mice by oral administration of porcine insulin. Proc Natl Acad Sci USA 88:10252–10256
Goudy KS, Wang B, Tisch R (2008) Gene gun-mediated DNA vaccination enhances antigen-specific immunotherapy at a late preclinical stage of type 1 diabetes in nonobese diabetic mice. Clin Immunol 129:49–57
Kaufman DL, Clare-Salzler M, Tian J et al (1993) Spontaneous loss of T-cell tolerance to glutamic acid decarboxylase in murine insulin-dependent diabetes. Nature 366:69–72
Li AF, Escher A (2003) Intradermal or oral delivery of GAD-encoding genetic vaccines suppresses type 1 diabetes. DNA Cell Biol 22:227–232
Olcott AP, Tian J, Walker V et al (2005) Antigen-based therapies using ignored determinants of beta cell antigens can more effectively inhibit late-stage autoimmune disease in diabetes-prone mice. J Immunol 175:1991–1999
Elias D, Cohen IR (1994) Peptide therapy for diabetes in NOD mice. Lancet 343:704–706
Elias D, Reshef T, Birk OS et al (1991) Vaccination against autoimmune mouse diabetes with a T-cell epitope of the human 65-kDa heat shock protein. Proc Natl Acad Sci USA 88:3088–3091
Pozzilli P, Pitocco D, Visalli N et al (2000) No effect of oral insulin on residual beta-cell function in recent-onset type I diabetes (the IMDIAB VII). IMDIAB group. Diabetologia 43:1000–1004
Walter M, Philotheou A, Bonnici F et al (2009) No effect of the altered peptide ligand NBI-6024 on beta-cell residual function and insulin needs in new-onset type 1 diabetes. Diabetes Care 32:2036–2040
Boitard C, Michie S, Serrurier P et al (1985) In vivo prevention of thyroid and pancreatic autoimmunity in the BB rat by antibody to class II major histocompatibility complex gene products. Proc Natl Acad Sci USA 82:6627–6631
Chatenoud L, Thervet E, Primo J et al (1994) Anti-CD3 antibody induces long-term remission of overt autoimmunity in nonobese diabetic mice. Proc Natl Acad Sci USA 91:123–127
Hutchings P, O’Reilly L, Parish NM et al (1992) The use of a non-depleting anti-CD4 monoclonal antibody to re-establish tolerance to beta cells in NOD mice. Eur J Immunol 22:1913–1918
Lenschow DJ, Ho SC, Sattar H et al (1995) Differential effects of anti-B7-1 and anti-B7-2 monoclonal antibody treatment on the development of diabetes in the nonobese diabetic mouse. J Exp Med 181:1145–1155
Molano RD, Berney T, Li H et al (2001) Prolonged islet graft survival in NOD mice by blockade of the CD40-CD154 pathway of T-cell costimulation. Diabetes 50:270–276
Sempe P, Bedossa P, Richard MF et al (1991) Anti-alpha/beta T cell receptor monoclonal antibody provides an efficient therapy for autoimmune diabetes in nonobese diabetic (NOD) mice. Eur J Immunol 21:1163–1169
Wang B, Gonzalez A, Benoist C et al (1996) The role of CD8+ T cells in the initiation of insulin-dependent diabetes mellitus. Eur J Immunol 26:1762–1769
Chatenoud L, Primo J, Bach JF (1997) CD3 antibody-induced dominant self tolerance in overtly diabetic NOD mice. J Immunol 158:2947–2954
Herold KC, Gitelman SE, Masharani U et al (2005) A single course of anti-CD3 monoclonal antibody hOKT3gamma1(Ala-Ala) results in improvement in C-peptide responses and clinical parameters for at least 2 years after onset of type 1 diabetes. Diabetes 54:1763–1769
Herold KC, Hagopian W, Auger JA et al (2002) Anti-CD3 monoclonal antibody in new-onset type 1 diabetes mellitus. N Engl J Med 346:1692–1698
Keymeulen B, Vandemeulebroucke E, Ziegler AG et al (2005) Insulin needs after CD3-antibody therapy in new-onset type 1 diabetes. N Engl J Med 352:2598–2608
Keymeulen B, Walter M, Mathieu C et al (2010) Four-year metabolic outcome of a randomised controlled CD3-antibody trial in recent-onset type 1 diabetic patients depends on their age and baseline residual beta cell mass. Diabetologia 53:614–623
Herold KC, Gitelman S, Greenbaum C et al (2009) Treatment of patients with new onset Type 1 diabetes with a single course of anti-CD3 mAb Teplizumab preserves insulin production for up to 5 years. Clin Immunol 132:166–173
Ablamunits V, Sherry NA, Kushner JA et al (2007) Autoimmunity and beta cell regeneration in mouse and human type 1 diabetes: the peace is not enough. Ann N Y Acad Sci 1103:19–32
Aoki CA, Borchers AT, Ridgway WM et al (2005) NOD mice and autoimmunity. Autoimmun Rev 4:373–379
Baecher-Allan C, Hafler DA (2006) Human regulatory T cells and their role in autoimmune disease. Immunol Rev 212:203–216
Homann D, von Herrath M (2004) Regulatory T cells and type 1 diabetes. Clin Immunol 112:202–209
Szypowska A, Stelmaszczyk-Emmel A, Demkow U, Luczynski W (2012) Low frequency of regulatory T cells in the peripheral blood of children with type 1 diabetes diagnosed under the age of five. Arch Immunol Ther Exp (Warsz) 60:307–313
Dendrou CA, Wicker LS (2008) The IL-2/CD25 pathway determines susceptibility to T1D in humans and NOD mice. J Clin Immunol 28:685–696
You S, Leforban B, Garcia C et al (2007) Adaptive TGF-beta-dependent regulatory T cells control autoimmune diabetes and are a privileged target of anti-CD3 antibody treatment. Proc Natl Acad Sci USA 104:6335–6340
Gregori S, Giarratana N, Smiroldo S et al (2003) Dynamics of pathogenic and suppressor T cells in autoimmune diabetes development. J Immunol 171:4040–4047
You S, Belghith M, Cobbold S et al (2005) Autoimmune diabetes onset results from qualitative rather than quantitative age-dependent changes in pathogenic T-cells. Diabetes 54:1415–1422
Lindley S, Dayan CM, Bishop A et al (2005) Defective suppressor function in CD4(+)CD25(+) T-cells from patients with type 1 diabetes. Diabetes 54:92–99
Belghith M, Bluestone JA, Barriot S et al (2003) TGF-beta-dependent mechanisms mediate restoration of self-tolerance induced by antibodies to CD3 in overt autoimmune diabetes. Nat Med 9:1202–1208
Pop SM, Wong CP, He Q et al (2007) The type and frequency of immunoregulatory CD4+ T-cells govern the efficacy of antigen-specific immunotherapy in nonobese diabetic mice. Diabetes 56:1395–1402
Marek-Trzonkowska N, Mysliwiec M, Dobyszuk A, Grabowska M, Techmanska I, Juscinska J, Wujtewicz MA, Witkowski P, Mlynarski W, Balcerska A, Mysliwska J, Trzonkowski P (2012) Administration of CD4+CD25highCD127- regulatory T cells preserves beta-cell function in type 1 diabetes in children. Diabetes Care
Tang Q, Henriksen KJ, Bi M et al (2004) In vitro-expanded antigen-specific regulatory T cells suppress autoimmune diabetes. J Exp Med 199:1455–1465
Zhang Q, Shi S, Liu Y et al (2009) Mesenchymal stem cells derived from human gingiva are capable of immunomodulatory functions and ameliorate inflammation-related tissue destruction in experimental colitis. J Immunol 183:7787–7798
Zappia E, Casazza S, Pedemonte E et al (2005) Mesenchymal stem cells ameliorate experimental autoimmune encephalomyelitis inducing T-cell anergy. Blood 106:1755–1761
Augello A, Tasso R, Negrini SM et al (2007) Cell therapy using allogeneic bone marrow mesenchymal stem cells prevents tissue damage in collagen-induced arthritis. Arthritis Rheum 56:1175–1186
Fiorina P, Jurewicz M, Augello A et al (2009) Immunomodulatory function of bone marrow-derived mesenchymal stem cells in experimental autoimmune type 1 diabetes. J Immunol 183:993–1004
Bassi EJ, Moraes-Vieira PM, Moreira Sa CS, Almeida DC, Vieira LM, Cunha CS, Hiyane MI, Basso AS, Pacheco-Silva A, Camara NO (2012) Immune regulatory properties of allogeneic adipose-derived mesenchymal stem cells in the treatment of experimental autoimmune diabetes. Diabetes
English K, French A, Wood KJ (2010) Mesenchymal stromal cells: facilitators of successful transplantation? Cell Stem Cell 7:431–442
Bartholomew A, Sturgeon C, Siatskas M et al (2002) Mesenchymal stem cells suppress lymphocyte proliferation in vitro and prolong skin graft survival in vivo. Exp Hematol 30:42–48
Casiraghi F, Azzollini N, Cassis P et al (2008) Pretransplant infusion of mesenchymal stem cells prolongs the survival of a semiallogeneic heart transplant through the generation of regulatory T cells. J Immunol 181:3933–3946
Le Blanc K, Frassoni F, Ball L et al (2008) Mesenchymal stem cells for treatment of steroid-resistant, severe, acute graft-versus-host disease: a phase II study. Lancet 371:1579–1586
Ding Y, Xu D, Feng G et al (2009) Mesenchymal stem cells prevent the rejection of fully allogenic islet grafts by the immunosuppressive activity of matrix metalloproteinase-2 and -9. Diabetes 58:1797–1806
Ryan EA, Paty BW, Senior PA et al (2005) Five-year follow-up after clinical islet transplantation. Diabetes 54:2060–2069
Schroeder IS, Rolletschek A, Blyszczuk P et al (2006) Differentiation of mouse embryonic stem cells to insulin-producing cells. Nat Protoc 1:495–507
Soria B, Roche E, Berna G et al (2000) Insulin-secreting cells derived from embryonic stem cells normalize glycemia in streptozotocin-induced diabetic mice. Diabetes 49:157–162
D’Amour KA, Bang AG, Eliazer S et al (2006) Production of pancreatic hormone-expressing endocrine cells from human embryonic stem cells. Nat Biotechnol 24:1392–1401
Kroon E, Martinson LA, Kadoya K et al (2008) Pancreatic endoderm derived from human embryonic stem cells generates glucose-responsive insulin-secreting cells in vivo. Nat Biotechnol 26:443–452
Wu DC, Boyd AS, Wood KJ (2008) Embryonic stem cells and their differentiated derivatives have a fragile immune privilege but still represent novel targets of immune attack. Stem Cells 26:1939–1950
Boyd AS, Wu DC, Higashi Y et al (2008) A comparison of protocols used to generate insulin-producing cell clusters from mouse embryonic stem cells. Stem Cells 26:1128–1137
Boyd AS, Wood KJ (2010) Characteristics of the immune response and relative immune privilege at the incipient stages following transplantation of ES cell derived insulin-producing cell clusters. PLoS ONE 5:e10965
Boyd AS, Wood KJ (2009) Variation in MHC expression between undifferentiated mouse ES cells and ES cell-derived insulin-producing cell clusters. Transplantation 87:1300–1304
Takahashi K, Yamanaka S (2006) Induction of pluripotent stem cells from mouse embryonic and adult fibroblast cultures by defined factors. Cell 126:663–676
Tateishi K, He J, Taranova O et al (2008) Generation of insulin-secreting islet-like clusters from human skin fibroblasts. J Biol Chem 283:31601–31607
Maehr R, Chen S, Snitow M et al (2009) Generation of pluripotent stem cells from patients with type 1 diabetes. Proc Natl Acad Sci USA 106:15768–15773
Hess D, Li L, Martin M et al (2003) Bone marrow-derived stem cells initiate pancreatic regeneration. Nat Biotechnol 21:763–770
Gabr MM, Sobh MM, Zakaria MM et al (2008) Transplantation of insulin-producing clusters derived from adult bone marrow stem cells to treat diabetes in rats. Exp Clin Transplant 6:236–243
Oh SH, Muzzonigro TM, Bae SH et al (2004) Adult bone marrow-derived cells trans-differentiating into insulin-producing cells for the treatment of type I diabetes. Lab Invest 84:607–617
Chao KC, Chao KF, Fu YS et al (2008) Islet-like clusters derived from mesenchymal stem cells in Wharton’s Jelly of the human umbilical cord for transplantation to control type 1 diabetes. PLoS ONE 3:e1451
Jacob F (1979) Cell surface and early stages of mouse embryogenesis. Curr Top Dev Biol 13:117–137
Zhao T, Zhang ZN, Rong Z, Xu Y (2011) Immunogenicity of induced pluripotent stem cells. Nature 474:212–215
Sibley RK, Sutherland DE, Goetz F et al (1985) Recurrent diabetes mellitus in the pancreas iso- and allograft. A light and electron microscopic and immunohistochemical analysis of four cases. Lab Invest 53:132–144
Sutherland DE, Sibley R, Xu XZ et al (1984) Twin-to-twin pancreas transplantation: reversal and reenactment of the pathogenesis of type I diabetes. Trans Assoc Am Physicians 97:80–87
Sibley RK, Sutherland DE (1987) Pancreas transplantation. An immunohistologic and histopathologic examination of 100 grafts. Am J Pathol 128:151–170
Barthlott T, Kassiotis G, Stockinger B (2003) T cell regulation as a side effect of homeostasis and competition. J Exp Med 197:451–460
Marleau AM, Sarvetnick N (2005) T cell homeostasis in tolerance and immunity. J Leukoc Biol 78:575–584
Surh CD, Boyman O, Purton JF et al (2006) Homeostasis of memory T cells. Immunol Rev 211:154–163
Calzascia T, Pellegrini M, Lin A et al (2008) CD4 T cells, lymphopenia, and IL-7 in a multistep pathway to autoimmunity. Proc Natl Acad Sci USA 105:2999–3004
Wood K (2008) Outlook for longer-lasting islets. Nat Med 14:1156–1157
Monti P, Scirpoli M, Maffi P et al (2008) Islet transplantation in patients with autoimmune diabetes induces homeostatic cytokines that expand autoreactive memory T cells. J Clin Invest 118:1806–1814
Long SA, Rieck M, Sanda S, Bollyky JB, Samuels PL, Goland R, Ahmann A, Rabinovitch A, Aggarwal S, Phippard D, Turka LA, Ehlers MR, Bianchine PJ, Boyle KD, Adah SA, Bluestone JA, Buckner JH, Greenbaum CJ (2012) Rapamycin/IL-2 combination therapy in patients with type 1 diabetes qaugments tregs yet transiently ibeta-cell function. Diabetes
Huurman VA, Hilbrands R, Pinkse GG et al (2008) Cellular islet autoimmunity associates with clinical outcome of islet cell transplantation. PLoS ONE 3:e2435
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2013 Springer Science+Business Media New York
About this chapter
Cite this chapter
English, K., Wood, K.J. (2013). Addressing the Challenge of Autoimmunity in the Treatment of Diabetes with Stem Cells. In: Fairchild, P. (eds) The Immunological Barriers to Regenerative Medicine. Stem Cell Biology and Regenerative Medicine. Humana Press, New York, NY. https://doi.org/10.1007/978-1-4614-5480-9_16
Download citation
DOI: https://doi.org/10.1007/978-1-4614-5480-9_16
Published:
Publisher Name: Humana Press, New York, NY
Print ISBN: 978-1-4614-5479-3
Online ISBN: 978-1-4614-5480-9
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)