Abstract
Tuberous Sclerosis Complex (TCS) is a neurocutaneous syndrome affecting the skin, central nervous system, heart, kidney, lung and other sites of the human body. The onset of facial angiofibromas (FA) is at about 5 years old and becomes more evident later. After puberty, FA lesions grow and may bleed, often causing discomfort. The primary treatments for FA include: lasers, dermabrassion, electrosurgery, podophyllin, photodynamic therapy followed by pulsed dye laser and topical rapamycin. An advantage of cryosurgery is that it can be performed without anesthesia. Cryosurgery is rarely documented as a treatment for FA in general. We treated four female patients affected by TSC and FA with cryosurgery. All patients improved after a series of treatments. In our experience, cryosurgery is effective, efficient, relatively inexpensive and easy to perform. Furthermore, according to the patient’s clinical evolution, it can be repeatable from time to time.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
Introduction
Tuberous Sclerosis Complex (TSC) is a neurocutaneous syndrome affecting the skin, central nervous system, heart, kidneys, lungs and other sites of the human body. It is an autosomal dominant genetic condition related to two tumor suppressor genes located on chromosome 9 or chromosome 16 [1]. Cutaneous manifestations of TSC are considered to be part of the major features required for its diagnosis [1].
Description of the Disease
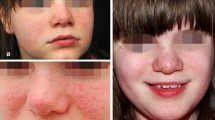
Among skin features, facial angiofibromas (FA) develop at approximately the age of 5 years and become more evident later in life. At first, FA are small pink or red papules, usually located on the cheeks, nasolabial folds, nose and chin. After puberty they grow, may bleed, and often cause discomfort for patients and their parents. For this reason, various modalities of treatment have been adopted
Therapeutic Alternatives
Laser [2] dermabrassion, electrosurgery, photodynamic therapy followed by pulsed dye laser [3]; recently tincture of podophyllin [4] and topical rapamycin [5] have been proposed as treatment. These destructive procedures, done repeatedly, can have acceptable cosmetic results. All surgical methods need previous local anesthesia, consisting of regional nerve block or EMLA application under occlusion over the affected area. Sometimes, general anesthesia may be required. Lately occasional experiences have suggested the use of a topical drug, rapamycin (sirolimus) [5], which would act on the vascular component of angiofibromas.
Rapamycin inhibits mTOR (mammalian target of rapamycin) a well documented protein in the pathogenesis of TSC. Oral rapamycin’s ability to induce regression of visceral TSC-related tumors is well-established and its use is prevalently dedicated to treatment of Subependymal Giant Cell Astrocytoma (SEGA).
Cryosurgery
Only cryosurgery, among the different surgical techniques mentioned above, can be used without anesthesia. Cryosurgery is only anecdotally cited in the treatment of FA in patients with TSC, and is rarely documented for FA in general [6]. On the other hand, it is widely used in dermatology to destroy several types of benign lesions [7].
Methodology (How Do I Do It)
Thin nozzles are used to emit an open spray of LN and the application is repeated after several minutes. In our recent experience, we found it easy to tolerate without local anesthesia, or just using topical formulations of lidocaine, or regional nerve blocks, as its administration produces only an initial mild pain that disappears in a few minutes [8].
Success Rates
We recently treated four young TSC females for FA (Fig. 120.1a, b). All patients easily tolerated the intervention and only reported a mild burning sensation during the application. A mild erythema over the treated area may persist for up to 1 h. Patients improved significantly after a series of treatments and reported feeling satisfied with the results of the therapy (Fig. 120.2a, b).
Conclusions
In select patients, such as the four in this report, cryosurgery will not require hospitalization or day surgery. In our experience, cryosurgery is efficient, cost-effective, easy to administer, convenient and can be used repeatedly, according to the clinical evolution [8]. Its side effects are minimal and predictable; moreover it can be used in conjunction with other available treatments, such as lasers, in case of need.
References
Schwartz RA, Fernández G, Kotulska K, Józwiak S. Tuberous sclerosis complex: advances in diagnosis, genetics, and management. J Am Acad Dermatol. 2007;57:189–202.
Kaufman AJ, Grekin RC, Geisse JK, Frieden IJ. Treatment of adenoma sebaceum with the copper vapour laser. J Am Acad Dermatol. 1995;33:770–4.
Weinberger CH, Endrizzi B, Hook KP, Lee P. Treatment of Angiofibromas of Tuberous Sclerosis with 5-Aminolevulinic acid blue light photodynamic therapy followed by immediate pulsed dye laser. Dermatol Surg. 2009;35:1849–51.
Türkmen M, Ertam I, Ünal I, Dereli T. Facial angiofibromas of Tuberous Sclerosis: successful treatment with podophyllin. JEADV. 2009;23:713–4.
Haemel AK, O’Brian AL, Teng JM. A novel approach to facial angiofibromas in tuberous sclerosis. Arch Dermatol. 2010;146(7):715–8.
Dvir E, Hirshowitz B. The use of cryosurgery in treating the fibrous papules of Tuberous Sclerosis. Ann Plast Surg. 1980;4:158–60.
Thai KE, Sinclair RD. Cryosurgery of benign skin lesions. Australas J Dermatol. 1999;40:175–86.
Schepis C, Siragusa M. Cryosurgery: an easy and cheap therapy for facial angiofibromas in tuberous sclerosis. Eur J Dermatol. 2010;20:506–7.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer-Verlag London
About this chapter
Cite this chapter
Schepis, C. (2016). The Tuberous Sclerosis Complex. In: Abramovits, W., Graham, G., Har-Shai, Y., Strumia, R. (eds) Dermatological Cryosurgery and Cryotherapy. Springer, London. https://doi.org/10.1007/978-1-4471-6765-5_120
Download citation
DOI: https://doi.org/10.1007/978-1-4471-6765-5_120
Published:
Publisher Name: Springer, London
Print ISBN: 978-1-4471-6764-8
Online ISBN: 978-1-4471-6765-5
eBook Packages: MedicineMedicine (R0)