Abstract
This chapter provides an extensive review of the normal size of the ascending aorta, for different body surface areas including tall people. The different imaging techniques, by means of echocardiography, magnetic resonance and computed tomography, are extensively discussed, as well as pitfalls in size measurements. The size of the ascending aorta may increase due to aging or pathologic conditions. The authors consider an aortic root or ascending aorta diameter above 4.0 cm as abnormal. From a diameter of >4.0 cm begins a monitor-zone for extended diagnostic evaluation, treatment advices and pre-pregnancy counselling. From a diameter >4.5 cm, operative treatment of the ascending aorta is advised in patients with connective tissue disorders who have risk factors. From a diameter of >5.0 cm, operative treatment is advised in other cases of connective tissue disorders and in cases of bicuspid aortic valve with risk factors. From a diameter of >5.5 cm, operative treatment is advised in bicuspid aortic valve without risk factors and in all other cases.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords/Phrases
- Dilatation of the Ascending Aorta
- Normal Aortic Diameter
- Aortic size and aging
- Aortic growth and pathologic conditions
- Imaging techniques
- Thoracic Aorta Aneurysm
- Aortic dissection
- Intervention thresholds
Introduction
Acute dissection or rupture of the ascending aorta is often lethal. Even when emergency surgery can be performed, associated morbidity and mortality are high. Dissection and rupture are mainly related to aneurysm size, aortic diameter and expansion rate. Aneurysms remain silent as long as there are no complications. To prevent dissection or rupture of the ascending aorta, prophylactic operation of a, most often, asymptomatic patient with a known dilatation of the ascending aorta is advised, along with other supportive measures [1–3]. It is crucial to monitor patients with a dilated ascending aorta from an early stage, to choose the right moment for surgical repair.
Normal Diameters of the Ascending Aorta
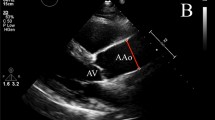
Standard levels and methods for the echocardiographic measurement of ascending aortic have been described (Fig. 4.1) [4]. Aneurysm formation can occur at the level of the sinus of Valsalva (e.g. Marfan syndrome {MFS}) as well as superior of the supravalvular aortic ridge, in the tubular part of the ascending aorta (e.g. Familial Thoracic Aortic Aneurysm and Dissection {TAAD}). The prerequisite for diagnosis and monitoring are reference values. In the past, several studies have tried to establish upper limit of normal (ULN) values, using transthoracic echocardiography (TTE) [4, 5], transesophageal echocardiography (TEE) [6, 7], magnetic resonance imaging (MRI) [8] and computed tomography (CT) [9]. However “normal” dimensions of the ascending aorta are still not well defined.
Standard levels and methods for the echocardiographic measurement of ascending aortic (From Roman et al [4]). Left: Schematic illustration of the aortic root in the 2-dimensional parasternal long-axis view. Measurements were obtained at four levels, including the annulus, sinuses of Valsalva, supraaortic ridge, proximal ascending aorta. Right: measurement were made perpendicular to the long axis of the aorta, using the leading edge technique
Aortic Growth and Aging
During life the size of the aorta increases. In childhood and young adulthood this is caused by an increase of the luminal diameter. In adulthood, the aortic size is related to exercise and workload. Whereas the elastin content in the ascending aorta is high, aging of the aorta is accompanied by a loss of compliance and an increase in wall stiffness. The media displays loss of smooth muscle cells and fragmentation of elastic fibres with the appearance of cystic spaces, filled with mucoid material. This process, called cystic media degeneration, ‘normally’ occurs with aging. A growth of 1 mm per 10 years is regarded as a normal aortic growth rate [5, 10]. Recent longitudinal data from the Framingham Heart Study in 4,542 individuals indicated that the aortic root gradually increases by 0.89 mm in men and 0.68 mm in woman for each decade of life, assuming a normal BMi and adjusting for blood pressure. The presence of hypertension or obesity was associated with greater mean aortic root size over time [11] (Figs. 4.2 and 4.3).
Predicted mean aortic root growth curves in men with and without obesity or hypertension(From Lam et al. [11])
Predicted mean aortic root growth curves in women with and without obesity or hypertension (From Lam et al. [11])
At younger ages, cystic media necrosis is associated with various connective tissue diseases, such as MFS, Loeys Dietz syndrome (LDS) and TAAD. So more or less the same process is acting in the aortic wall in aging as well as in pathological conditions.
What Is an Abnormal Diameter? Echocardiographic Methods
An aneurysm is defined as a cross sectional diameter of more than 1.5 times its normal value. For the ascending aorta this definition does not seem to be so useful. The ascending aorta begins with a natural dilatation at the level of the Sinus of Valsalva. So there is no proximal reference diameter available, as is the case in the distal aorta or in muscular arteries. Mean diameter with confidence intervals derived from a normal population are better applicable. The size of the ascending aorta is related most strongly to body surface area (BSA) and age [4, 5]. Relation with sex and height is conflicting. Therefore, BSA may be used to predict aortic root diameter in several age intervals. In 52 children and 135 adults, Roman et al. established normal values in three age strata: younger than 20 years, 20–40 years, and older than 40 years by published equations (Figs. 4.4 and 4.5). These values with 95 % confidence have been included in guidelines as reference values to date [1, 3, 12].
Aortic diameter at the sinuses of Valsalva in Children (From Roman et al. [4]). Left: Relation of body surface area to aortic root diameter at the sinuses of Valsalva in normal infants and children. Right: 95 % normal confidence limits for aortic root at the sinuses of Valsalva in relation to body surface area in normal infants and children
Aortic diameter at the sinuses of Valsalva in Adults. Ninety five percent normal confidence limits for aortic root diameter at the level of the sinuses of Valsalva in relation to BSA. Left in adult younger than 40 years of age. Right in adults 40 years of age and older (From Roman et al. [4])
However, the sample size of the study of Roman et al. was limited and a sufficient number of healthy subjects whose height exceeds the 95th percentile, as is usually the case in MFS patients, was not included. Data for children and for adults under the age of 40 with a large BSA were extrapolated, not based on real measurements! In an adjusted nomogram for tall children, developed by Rozendaal et al., a wider range of aortic root diameter is considered to be normal [13] (Fig. 4.6). Radonic et al. examined 38 healthy controls with a large BSA and found a maximal aortic root diameter of 38 mm [14]. The aortic root diameter tends to plateau at 40 mm (Fig. 4.7). This has also been demonstrated in tall men and women [15] and in athletes [16, 17]. Radonic et al. conclude, referring to other publications, that with the use of the Z-score, the diagnosis of MFS wrongly would be missed in patients with a large BSA. So, the authors are critical against the use of these nomograms of Roman et al. in adults.
Relation between aortic root diameter and body surface area (BSA) (empty circles) and 95 % reference limits for aortic root diameter in relation to BSA (solid lines), in subjects aged 3.2–18.4 years (From Rozendaal et al. [13]). The upper and lower limits of normal of the standard nomogram (4) are shown in dashed lines
Correlation of BSA (m2) and aortic root diameters in 38 healthy volunteers (From Radonic et al. [14])
The clinician has to be aware that the diameters are measured in different ways. Roman et al. measured aortic diameters enddiastolic using the leading edge to leading edge technique (with inclusion of the anterior wall) conform the 2005 ASE-recommendations for adults [18]. The 2010 ASE guideline for paediatric echocardiography on the other hand recommends measurements to be done midsystolic and inner edge to inner edge [19]. The 2010 ACCF/AHA Guideline for Thoracic Aortic Disease also recommends the internal diameter (whereas for CT and MRI the external diameter is advised) [3].
Transthoracic echocardiography (TTE) suffices to quantify maximum aortic root and proximal ascending aorta diameters when the acoustic window is adequate. For the mid- and distal part of the ascending aorta other techniques may be needed. TEE overcomes problems with a bad acoustic window, except for a small portion of the distal ascending aorta [20]. But also CT en MRI are increasingly used, but for the aortic root, they are not well suitable, when performed without ECG-gating.
The revised Ghent nosology for the diagnosis of MFS has made a Z-score of ≥2 for the aortic root an important diagnostic criterium [12]. For childhood and young adulthood standardization to body surface (BSA) is usual, although aortic dimensions seem to have good correlation with height also [21]. Newer reference values for children based on measurements in larger groups have been developed for both leading edge method (also in diastole) [22] and the inner edge method (in systole) [23]. From these reference values, scores can be calculated. For adults however application of the Z-score may not be a good approach.
Aortic Size and CT
CT is increasingly used nowadays for diagnosis or exclusion of dilatation of the ascending aorta. Earlier studies were limited by sample size, only pure axial slices and non-contemporary imaging technology [9]. In recent years newer reference values have been developed, not only in patients referred for various cardiac and non-cardiovascular reasons [26, 27] but also in the general population [28]. Age, gender, and especially BSA were the major determinants of ascending aortic diameters. Data of several studies are summarized in Tables 4.1 and 4.2.
The clinician must be aware that also in CT different methods of measurement are used: enddiastolic (Kälsch et al. [28] or endsystolic (Mao et al. [26], with inclusion Kälsch et al. [28] or without inclusion Mao et al. [26] of the aortic wall. Traditionally cross sectional imaging with CT or MRI includes the vessel wall. For contrast enhanced CT or MR however intraluminal diameter measurements are used. In 107 healthy persons Mao et al. showed that the mean diameter of the ascending aorta was endsystolic 1.7 mm greater than enddiastolic. The mean aortic wall thickness in 85 persons appeared to be 1.2 mm (range 0.75–1.75). So the luminal diameter was 2.4 mm less than the total diameter.
The clinician must also be careful to perform accurate measurements perpendicular to the long axis of the aorta. Especially in cases of an elongated thoracic aorta, the plane of the aortic valve can be nearly vertical instead of horizontal; the ascending aorta also gets more of a C-shape. Double oblique reformatted images, obtained perpendicular to the aortic lumen (i.e. true short axis images of the aorta) allow a more accurate measurement of the aortic diameter [29]. When comparing cross-sectional dimensions in standard axial planes and in reformatted double oblique planes, Mendoza et al. demonstrated significant size differences with impact for surgical decision making [30]. During hypovolaemic shock aortic diameters may be decreased [31].
Aortic Growth and Pathologic Conditions
At younger ages, dilatation of the ascending aorta is often associated with various connective tissue diseases and has a hereditary cause, either syndromal (e.g. MFS, Loeys Dietz syndrome [LDS], Ehlers Danlos syndrome type IV) or non-syndromal (e.g. TAAD). Osteoarthritis Aneurysm syndrome is a recently recognized autosomal dominant syndromic form of thoracic aortic aneurysms and dissections characterised by the presence of arterial aneurysms and tortuosity, mild craniofacial, skeletal and cutaneous anomalies, and early-onset osteoarthritis. It is caused by mutations in SMAD 3 [32–34]. Other causes of aortic dilatation are hypertension, chronic dissection, aortic surgery (false aneurysm), cardiopulmonary resuscitation and lastly infectious and non-infectious aortitis. Atherosclerosis more often causes aneurysms of the descending aorta and particularly aneurysms of the abdominal aorta, not the ascending aorta [7, 35].
There is evidence that many patients with bicuspid aortic valve (BAV) or Aortic Coarctation (CoA) have disorders of vascular connective tissue as well, involving loss of elastic tissue and leading to dilatation of the proximal aorta [36, 37]. The exact mechanism behind dilatation of the proximal aorta in isolated BAV is however still a matter of debate, For a long time this has been attributed to a genetic cause. Lately there is increasing evidence for a haemodynamic mechanism, either a poststenotic dilatation, or abnormal flow patterns and asymmetrically increased wall stress by a clinically normal BAV. Probably, it is a combination of these aforementioned components, because also different phenotypic forms of aortopathy have been described: dilatation of only the tubular part of the ascending aorta, dilatation of only the aortic root and combinations with dilatation of the aortic arch [38–42].
When Can Aortic Dissection Occur?
Although a virulent disease, thoracic aortic aneurysm (TAA) is an indolent process. Yale data pointed out that a thoracic aneurysm grows very slowly, approximately 0.12 cm per year (ascending aorta 0.1 cm/year, descending aorta 0.3 cm/year [43].
TAA-patients with positive family trees (but no MFS) show a higher growth rate than patients with sporadic TAA or MFS [44, 45]. Aortic dilatation may lead to aortic dissection or aortic rupture. The risk of aortic dissection is related to the aortic diameter. In 2002, Davies et al. [46] identified that the median aortic diameter at the time of rupture for the ascending or aortic arch was 6.0 cm. This diameter is still considered a ‘hinge point’ at which dissection or rupture can occur and yearly rate of rupture, dissection or death reaches maximal levels [43, 47] (Figs. 4.8 and 4.9). Intraoperative experiments with epiaortic echography has shown that as the aorta enlarges, distensibility of the aortic wall decreases, so that by approximately 6 cm in size, the aorta becomes a rigid tube [48]. There is, however, also evidence that a substantial number of patients have aortic diameters of less than 5.5 cm at the time of dissection; 15 % of the MFS patients have aortic dissection at a size of less than 5.0 cm [49]. In the analysis of Parish et al. 42 % (74/177) of patients without MFS or BAV had diameter <5 cm at moment of type A dissection [50]. In the International Registry of Acute Aortic Dissections (IRAD), more or less the same results: nearly 60 % of the 591 type A dissection patients had diameters <5.5 cm, and 40 % had diameters <5.0 cm [51] (Fig. 4.10). Given these facts, the aortic diameter alone is not sufficient to explain aortic dissection, and there is need for additional risk markers. Aortic elasticity has been identified as an additional risk factor for aortic dissection [52]. Whether this has implications for management has to be awaited.
Estimated effect of ascending aortic aneurysm size on risk of complications. Cumulative lifetime likelihood of rupture or dissection (y-axis) plotted against aortic size (x-axis). Note the abrupt “hinge point” at 6 cm (Adapted from Coady et al. [47])
Yearly rates of rupture, dissection, death, and combined events, related to aortic size. Note again the critical criterion dimension of 6 cm (From Elefteriades et al. [43])
Distribution of aortic size at time of presentation with acute type A aortic dissection (cm). Shaded bars indicate 59 % of patients with diameters <5.5 cm (From Pape et al. [51])
Aortic Dissection and BAV
Early publications indicated that aortic dissections occur more frequently in patients with BAV compared with tricuspid aortic valve (TAV) [53], even after AVR when there was a seemingly normal ascending aorta diameter at time of surgery [54]. Dissections occurred in patients with BAV at smaller size than 5.0 cm [49] and at a younger age [55]. However, in the IRAD-data it was unclear if the results were corrected for the effect of hypertension with and without BAV compared with TAV [56].
Recent studies however indicate that the dissection rate in patients with BAV is low [37, 57–59], does not differ from patients with TAV [60] and that life expectancy of adults is not shortened, when compared with the general population [57, 58]. Also after isolated AVR, dissection rate is low for patients with preoperative ascending aorta diameter of <50 mm [61, 62] or 40–50 mm [63, 64] (Table 4.3). Aortic enlargement may still occur post AVR, but appeared not to be a predictor for adverse aortic events [61–65]. Only the small subgroup with a ‘root phenotype’ seemed to be at higher risk [38, 65–67].
When Is Operation Indicated in Asymptomatic Patients? What do the Guidelines Say?
Until recently, it was generally agreed that prophylactic replacement of the aortic root should be performed at a diameter of 5.5 cm in patients with MFS [47, 68]. In the recommendations from the ESC Task Force on Aortic Dissection in 2001, this was broadened to all cases of dilated ascending aorta with inherited disease (MFS, EDS, annulo aortic ectasia) [1]. In cases with a family history of type A-dissection, the replacement of the aortic root should be performed earlier, at a diameter of ≤5.0 cm [1]. These ESC guidelines received ACC endorsement in 2001.
Between 2006 and 2008, four guidelines were published, not focussed on aortic dissection/dilatation, but with additional advice for patients with Dilated Ascending Aorta in combination with MFS, BAV or Aortic regurgitation. The 2006 ACC/AHA Guidelines for the management of Valvular Heart Disease (VHD) [69], the 2007 ESC Guidelines on the management of VHD [70], the 2008 ACC/AHA Guidelines for the management of Adults with Congenital Heart Disease [71] and the 2010 ESC Guidelines for the management of Grown-Up Congenital Heart Disease (GUCH) [72]. All guidelines give practically the same recommendations: (1) Repair of the aortic root (ARR), or replacement of the ascending aorta (AAR) if the diameter of the aortic root or the ascending aorta exceeds 5.0 cm or if the rate of increase is 0.5 cm/year or more. (2) In patients undergoing AVR, ARR, or AAR is indicated if the diameter is greater than 4.5 cm. (3) Lower thresholds may be considered for patients of small stature [69]. (4) Prepregnancy counselling is advised at 4.0/4.5 cm.
The ESC Guidelines on GUCH gives this recommendation for MFS. The other three Guidelines gives the same recommendations for BAV, which has been criticized by many authors [56, 64, 73, 74] and is still matter of debate [53, 75]. Because the low risk of aortic dissection with BAV, the size of the BAV population and (often) the impossibility of valve sparing surgery, the ESC has become recently more conservative in her policy towards aortic root dilatation with BAV. The Revised ESC Guidelines on VHD (version 2012) advices operative treatment of the aortic root at a size ≥5.0 cm only if risk factors are present (family history, systemic hypertension, aortic coarctation, increase in aortic diameter >2 mm/year) [76]. Without risk-factors operative treatment is adviced at a diameter ≥5.5 cm, just as for other patients. In MFS, also family history, size increase 2 mm/year, severe AR, desire to become pregnant, are risk factors to consider operative treatment for aortic root diameter ≥4.5 cm instead of 5.0 cm in MFS without risk factors [76].
In between, the 2010 ACCF/AHA Guidelines for the management of Thoracic Aortic Disease were published. They recommended similar thresholds for surgery. New in was the statement that for patients with LDS or confirmed TGFBR1 or TGFBR2 mutation, it is reasonable to undergo aortic repair when the aorta diameter exceeds 4.5 cm [3]. The experience of the surgical team may influence this decision making.
Given the recent data about type A dissection at diameters <5.0 cm, the lowered operative risk in large surgical centres, and the current possibilities of valve-sparing surgery, operative treatment at a diameter of 4.5 cm or more may be advised in some cases of connective tissue disease, especially when pregnancy is desired, when there is a family history of dissection, or when there is an indication for elective aortic valve replacement [3, 22, 35, 49, 50, 54, 69–72, 77] (Table 4.4). Replacement of the aortic root has also been suggested starting from 4.0 cm in LDS (in particular when it can be done valve-sparing) [78–80] and when there is an indication for elective aortic valve replacement [35].
Management and Follow-Up in Case of Aortic Dilatation
For adults the authors consider an aortic root (AR) or tubular ascending aorta (AA) diameter above 4.0 cm as abnormal. This is supported by many authors: Pellicia 2010 AR [17], Reed 2010 AR [15], Kinoshita 2000 AR [16], Radonic2011 AR [14], Agarwal 2009 AA [29] and many published reference values (Hager 2002 AA [81], Kaplan 2007 AA [82], Lin 2008 AA [83], Mao 2008 AA [26], Lu 2009 AR+AA [84], Mendoza 2011 AR+AA [30]).
In our opinion dilatation due to aging is not a normal process. Aortic sizes of young adults might be taken as reference value for older adults as well. Also for tall persons the aortic root diameter does not increase linearly with increasing BSA but tends to plateau. For women a value somewhat below 4.0 cm may be considered as upper limit of normal. The same applies to persons with small stature [69].
Last but not least, the tight hinge point for dissection at 6.0 cm, the solid criteria for surgical intervention from 5.0 to 5.5 cm and in some cases earlier, ask for a tight upper limit of normal size.
From a dilatation of the ascending aorta above 4.0 cm, the patient should be monitored regularly. Evaluation of a possible connective tissue disease should be performed by a multidisciplinary team (cardiologist, geneticist, and ophthalmologist). Patient and family history should be investigated, physical examination should be undertaken, and eventually DNA testing should be carried out. TTE should be performed to examine the aortic valve and to quantify aortic regurgitation. It cannot be stressed enough that also the entire aorta should be visualized using MRI or CT [85, 86]. Especially in TAAD or BAV patients, aneurysms tend to occur more frequently in the tubular ascending aorta, which may be difficult to visualize by TTE. Risk factors such as hypertension, cigarette smoking, and hypercholesterolemia should be managed. Blood pressure level should be lowered to 120/80 mmHg or less. Presently, beta-blockers are still the preferred medical therapy [35, 87, 88], but large prospective multicenter trials on the effect of ATII receptor antagonists or ACE inhibitors on aortic growth in patients with Marfan syndrome are being performed worldwide [35, 88, 89]. An overview of current studies has recently been published by den Hartog et al. [89] (Table 4.5).
Moderate restriction of physical activity should be advised [1, 88]. Patients should avoid exertion at maximal capacity and specifically, should not engage in competitive, contact, or isometric sports [90, 91]. Yearly follow up of the aortic diameter by TTE and/or by means of MRI or CT should be performed. In case of LDS or TGFBR1/TGFBR2 mutation, MRI of the thoracic, abdominal, cervical and cerebral vessels should be performed more frequently. Patients with LDS often have a more widespread and malignant course of aneurysmal disease.
Operative Treatment
The aortic valve and ascending aorta are replaced simultaneously by using a so-called composite valve graft with reimplantation of the coronary ostia into the prosthesis. The most frequent cause of late death is aneurysmal formation at the downstream aorta. The draw-back of composite graft replacement are thrombo-embolic, infectious and bleeding complications. With BAV as exception, valve sparing aortic root replacement is now first choice with excellent medium-term results. In the remodelling technique described by Yacoub [92], the graft is sewn to the remaining aortic wall around the commissures. This creates neo-sinuses and leaves the annulus mobile but unsupported. In the re-implantation or David technique, [93] the graft is fixed at the subannular level, and the valve and commissures are reimplanted inside the fabric. Both procedures offer a reasonable alternative to composite valve grafting with excellent short- and medium-term results, but long-term durability is not yet established. All aspects of surgery are treated in more detail in other chapters.
Genetic Counseling
Most connective tissue disorders are inherited in an autosomal dominant manner, which means that first degree relatives have a 50 % risk of inheriting the disease, although the severity cannot be predicted. For BAV, the genetics are complex and studies have demonstrated that BAV is likely related to mutations in different genes. First-degree relatives, also of patients with BAV, should, therefore, be evaluated for manifestations of connective tissue disorder, including a comprehensive clinical examination and TTE [71, 76]. If a disease-causing mutation in the index patient is known, molecular genetic testing of family members is possible, and prenatal testing can be performed.
Conclusion
An ascending aortic diameter above 4.0 cm should always be considered as abnormal. The clinician should be aware of the need for an aggressive preventive approach in patients with aortic dilatation, specifically in case of a connective tissue disorder. Due to recent insights, criteria for operative treatment of aortic dilatation have been liberalized in the relevant guidelines. Furthermore, the clinician should realize that first-degree relatives of patients with thoracic aortic dilatation are also at risk and should be evaluated for manifestations of connective tissue disorders.
References
Erbel R, Alfonso F, Boileau C, Dirsch O, Eber B, Haverich A, et al. Diagnosis and management of aortic dissection. Eur Heart J. 2001;22(18):1642–81.
Cozijnsen L, Braam RL, Waalewijn RA, Schepens MA, Loeys BL, van Oosterhout MF, et al. What is new in dilatation of the ascending aorta? Review of current literature and practical advice for the cardiologist. Circulation. 2011;123(8):924–8.
Hiratzka LF, Bakris GL, Beckman JA, Bersin RM, Carr VF, Casey Jr DE, et al. 2010 ACCF/AHA/AATS/ACR/ASA/SCA/SCAI/SIR/STS/SVM guidelines for the diagnosis and management of patients with Thoracic Aortic Disease: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines, American Association for Thoracic Surgery, American College of Radiology, American Stroke Association, Society of Cardiovascular Anesthesiologists, Society for Cardiovascular Angiography and Interventions, Society of Interventional Radiology, Society of Thoracic Surgeons, and Society for Vascular Medicine. Circulation. 2010;121(13):e266–369.
Roman MJ, Devereux RB, Kramer-Fox R, O’Loughlin J. Two-dimensional echocardiographic aortic root dimensions in normal children and adults. Am J Cardiol. 1989;64(8):507–12.
Vasan RS, Larson MG, Levy D. Determinants of echocardiographic aortic root size. Framingham Heart Study Circ. 1995;91(3):734–40.
Drexler M, Erbel R, Muller U, Wittlich N, Mohr-Kahaly S, Meyer J. Measurement of intracardiac dimensions and structures in normal young adult subjects by transesophageal echocardiography. Am J Cardiol. 1990;65(22):1491–6.
Agmon Y, Khandheria BK, Meissner I, Schwartz GL, Sicks JD, Fought AJ, et al. Is aortic dilatation an atherosclerosis-related process? Clinical, laboratory, and transesophageal echocardiographic correlates of thoracic aortic dimensions in the population with implications for thoracic aortic aneurysm formation. J Am Coll Cardiol. 2003;42(6):1076–83.
Garcier JM, Petitcolin V, Filaire M, Mofid R, Azarnouch K, Ravel A, et al. Normal diameter of the thoracic aorta in adults: a magnetic resonance imaging study. Surg Radiol Anat. 2003;25(3–4):322–9.
Aronberg DJ, Glazer HS, Madsen K, Sagel SS. Normal thoracic aortic diameters by computed tomography. J Comput Assist Tomogr. 1984;8(2):247–50.
Gerstenblith G, Frederiksen J, Yin FC, Fortuin NJ, Lakatta EG, Weisfeldt ML. Echocardiographic assessment of a normal adult aging population. Circulation. 1977;56(2):273–8.
Lam CS, Xanthakis V, Sullivan LM, Lieb W, Aragam J, Redfield MM, et al. Aortic root remodeling over the adult life course: longitudinal data from the Framingham Heart Study. Circulation. 2010;122(9):884–90.
Loeys BL, Dietz HC, Braverman AC, Callewaert BL, De BJ, Devereux RB, et al. The revised Ghent nosology for the Marfan syndrome. J Med Genet. 2010;47(7):476–85.
Rozendaal L, Groenink M, Naeff MS, Hennekam RC, Hart AA, Van Der Wall EE, et al. Marfan syndrome in children and adolescents: an adjusted nomogram for screening aortic root dilatation. Heart. 1998;79(1):69–72.
Radonic T, de Witte P, Groenink M, de Bruin-Bon R, Timmermans J, Scholte A, et al. Critical appraisal of the revised Ghent criteria for diagnosis of Marfan syndrome. Clin Genet. 2011;80:346–53.
Reed CM, Richey PA, Pulliam DA, Somes GW, Alpert BS. Aortic dimensions in tall men and women. Am J Cardiol. 1993;71(7):608–10.
Kinoshita N, Mimura J, Obayashi C, Katsukawa F, Onishi S, Yamazaki H. Aortic root dilatation among young competitive athletes: echocardiographic screening of 1929 athletes between 15 and 34 years of age. Am Heart J. 2000;139(4):723–8.
Pelliccia A, Di Paolo FM, De BE, Quattrini FM, Pisicchio C, Guerra E, et al. Prevalence and clinical significance of aortic root dilation in highly trained competitive athletes. Circulation. 2010;122(7):698–706, 3.
Lang RM, Bierig M, Devereux RB, Flachskampf FA, Foster E, Pellikka PA, et al. Recommendations for chamber quantification: a report from the American Society of Echocardiography’s Guidelines and Standards Committee and the Chamber Quantification Writing Group, developed in conjunction with the European Association of Echocardiography, a branch of the European Society of Cardiology. J Am Soc Echocardiogr. 2005;18(12):1440–63.
Lopez L, Colan SD, Frommelt PC, Ensing GJ, Kendall K, Younoszai AK, et al. Recommendations for quantification methods during the performance of a pediatric echocardiogram: a report from the Pediatric Measurements Writing Group of the American Society of Echocardiography Pediatric and Congenital Heart Disease Council. J Am Soc Echocardiogr. 2010;23(5):465–95.
Evangelista A, Flachskampf FA, Erbel R, Antonini-Canterin F, Vlachopoulos C, Rocchi G, et al. Echocardiography in aortic diseases: EAE recommendations for clinical practice. Eur J Echocardiogr. 2010;11(8):645–58.
Sheil ML, Jenkins O, Sholler GF. Echocardiographic assessment of aortic root dimensions in normal children based on measurement of a new ratio of aortic size independent of growth. Am J Cardiol. 1995;75(10):711–5.
Gautier M, Detaint D, Fermanian C, Aegerter P, Delorme G, Arnoult F, et al. Nomograms for aortic root diameters in children using two-dimensional echocardiography. Am J Cardiol. 2010;105(6):888–94.
Pettersen MD, Du W, Skeens ME, Humes RA. Regression equations for calculation of z scores of cardiac structures in a large cohort of healthy infants, children, and adolescents: an echocardiographic study. J Am Soc Echocardiogr. 2008;21(8):922–34.
Kaiser T, Kellenberger CJ, Albisetti M, Bergstrasser E, Valsangiacomo Buechel ER. Normal values for aortic diameters in children and adolescents—assessment in vivo by contrast-enhanced CMR-angiography. J Cardiovasc Magn Reson. 2008;10:56.
Burman ED, Keegan J, Kilner PJ. Aortic root measurement by cardiovascular magnetic resonance: specification of planes and lines of measurement and corresponding normal values. Circ Cardiovasc Imag. 2008;1(2):104–13.
Mao SS, Ahmadi N, Shah B, Beckmann D, Chen A, Ngo L, et al. Normal thoracic aorta diameter on cardiac computed tomography in healthy asymptomatic adults: impact of age and gender. Acad Radiol. 2008;15(7):827–34.
Wolak A, Gransar H, Thomson LE, Friedman JD, Hachamovitch R, Gutstein A, et al. Aortic size assessment by noncontrast cardiac computed tomography: normal limits by age, gender, and body surface area. JACC Cardiovasc Imag. 2008;1(2):200–9.
Kalsch H, Lehmann N, Mohlenkamp S, Becker A, Moebus S, Schmermund A, et al. Body-surface adjusted aortic reference diameters for improved identification of patients with thoracic aortic aneurysms: results from the population-based Heinz Nixdorf Recall study. Int J Cardiol. 2011;163(1):72–8.
Agarwal PP, Chughtai A, Matzinger FR, Kazerooni EA. Multidetector CT of thoracic aortic aneurysms. Radiographics. 2009;29(2):537–52.
Mendoza DD, Kochar M, Devereux RB, Basson CT, Min JK, Holmes K, et al. Impact of image analysis methodology on diagnostic and surgical classification of patients with thoracic aortic aneurysms. Ann Thorac Surg. 2011;92(3):904–12.
Jonker FH, van Keulen JW, Schlosser FJ, Indes JE, Moll FL, Verhagen HJ, et al. Thoracic aortic pulsatility decreases during hypovolemic shock: implications for stent-graft sizing. J Endovasc Ther. 2011;18(4):491–6.
van de Laar IM, van der Linde D, Oei EH, Bos PK, Bessems JH, Bierma-Zeinstra SM, et al. Phenotypic spectrum of the SMAD3-related aneurysms-osteoarthritis syndrome. J Med Genet. 2012;49(1):47–57.
van der Linde D, van de Laar IM, Bertoli-Avella AM, Oldenburg RA, Bekkers JA, Mattace-Raso FU, et al. Aggressive cardiovascular phenotype of aneurysms-osteoarthritis syndrome caused by pathogenic SMAD3 variants. J Am Coll Cardiol. 2012;60(5):397–403.
van der Linde D, Bekkers JA, Mattace-Raso FU, van de Laar IM, Moelker A, van den Bosch AE, et al. Progression rate and early surgical experience in the new aggressive aneurysms-osteoarthritis syndrome. Ann Thorac Surg. 2012;95(2):563–9.
Tadros TM, Klein MD, Shapira OM. Ascending aortic dilatation associated with bicuspid aortic valve: pathophysiology, molecular biology, and clinical implications. Circulation. 2009;119(6):880–90.
Verheugt CL, Uiterwaal CS, Grobbee DE, Mulder BJ. Long-term prognosis of congenital heart defects: a systematic review. Int J Cardiol. 2008;131(1):25–32.
Oliver JM, Alonso-Gonzalez R, Gonzalez AE, Gallego P, Sanchez-Recalde A, Cuesta E, et al. Risk of aortic root or ascending aorta complications in patients with bicuspid aortic valve with and without coarctation of the aorta. Am J Cardiol. 2009;104(7):1001–6.
Della CA, Bancone C, Quarto C, Dialetto G, Covino FE, Scardone M, et al. Predictors of ascending aortic dilatation with bicuspid aortic valve: a wide spectrum of disease expression. Eur J Cardiothorac Surg. 2007;31(3):397–404.
Della CA, Bancone C. Multiple aortopathy phenotypes with bicuspid aortic valve: the importance of terminology and definition criteria. Eur J Cardiothorac Surg. 2012;41(6):1404.
Fazel SS, Mallidi HR, Lee RS, Sheehan MP, Liang D, Fleischman D, et al. The aortopathy of bicuspid aortic valve disease has distinctive patterns and usually involves the transverse aortic arch. J Thorac Cardiovasc Surg. 2008;135(4):901–7, 907.
Schaefer BM, Lewin MB, Stout KK, Gill E, Prueitt A, Byers PH, et al. The bicuspid aortic valve: an integrated phenotypic classification of leaflet morphology and aortic root shape. Heart. 2008;94(12):1634–8.
Cotrufo M, Della CA. The association of bicuspid aortic valve disease with asymmetric dilatation of the tubular ascending aorta: identification of a definite syndrome. J Cardiovasc Med (Hagerstown). 2009;10(4):291–7.
Elefteriades JA, Farkas EA. Thoracic aortic aneurysm clinically pertinent controversies and uncertainties. J Am Coll Cardiol. 2010;55(9):841–57.
Albornoz G, Coady MA, Roberts M, Davies RR, Tranquilli M, Rizzo JA, et al. Familial thoracic aortic aneurysms and dissections—incidence, modes of inheritance, and phenotypic patterns. Ann Thorac Surg. 2006;82(4):1400–5.
Coady MA, Davies RR, Roberts M, Goldstein LJ, Rogalski MJ, Rizzo JA, et al. Familial patterns of thoracic aortic aneurysms. Arch Surg. 1999;134(4):361–7.
Davies RR, Goldstein LJ, Coady MA, Tittle SL, Rizzo JA, Kopf GS, et al. Yearly rupture or dissection rates for thoracic aortic aneurysms: simple prediction based on size. Ann Thorac Surg. 2002;73(1):17–27.
Coady MA, Rizzo JA, Hammond GL, Mandapati D, Darr U, Kopf GS, et al. What is the appropriate size criterion for resection of thoracic aortic aneurysms? J Thorac Cardiovasc Surg. 1997;113(3):476–91.
Koullias G, Modak R, Tranquilli M, Korkolis DP, Barash P, Elefteriades JA. Mechanical deterioration underlies malignant behavior of aneurysmal human ascending aorta. J Thorac Cardiovasc Surg. 2005;130(3):677–83.
Svensson LG, Kim KH, Lytle BW, Cosgrove DM. Relationship of aortic cross-sectional area to height ratio and the risk of aortic dissection in patients with bicuspid aortic valves. J Thorac Cardiovasc Surg. 2003;126(3):892–3.
Parish LM, Gorman III JH, Kahn S, Plappert T, St John-Sutton MG, Bavaria JE, et al. Aortic size in acute type A dissection: implications for preventive ascending aortic replacement. Eur J Cardiothorac Surg. 2009;35(6):941–5.
Pape LA, Tsai TT, Isselbacher EM, Oh JK, O’gara PT, Evangelista A, et al. Aortic diameter > or = 5.5 cm is not a good predictor of type A aortic dissection: observations from the International Registry of Acute Aortic Dissection (IRAD). Circulation. 2007;116(10):1120–7.
Nollen GJ, Groenink M, Tijssen JG, Van Der Wall EE, Mulder BJ. Aortic stiffness and diameter predict progressive aortic dilatation in patients with Marfan syndrome. Eur Heart J. 2004;25(13):1146–52.
Bonow RO. Bicuspid aortic valves and dilated aortas: a critical review of the ACC/AHA practice guidelines recommendations. Am J Cardiol. 2008;102(1):111–4.
Russo CF, Mazzetti S, Garatti A, Ribera E, Milazzo A, Bruschi G, et al. Aortic complications after bicuspid aortic valve replacement: long-term results. Ann Thorac Surg. 2002;74(5):S1773–6.
Januzzi JL, Isselbacher EM, Fattori R, Cooper JV, Smith DE, Fang J, et al. Characterizing the young patient with aortic dissection: results from the International Registry of Aortic Dissection (IRAD). J Am Coll Cardiol. 2004;43(4):665–9.
Guntheroth WG. A critical review of the American College of Cardiology/American Heart Association practice guidelines on bicuspid aortic valve with dilated ascending aorta. Am J Cardiol. 2008;102(1):107–10.
Michelena HI, Desjardins VA, Avierinos JF, Russo A, Nkomo VT, Sundt TM, et al. Natural history of asymptomatic patients with normally functioning or minimally dysfunctional bicuspid aortic valve in the community. Circulation. 2008;117(21):2776–84.
Tzemos N, Therrien J, Yip J, Thanassoulis G, Tremblay S, Jamorski MT, et al. Outcomes in adults with bicuspid aortic valves. JAMA. 2008;300(11):1317–25.
Michelena HI, Khanna AD, Mahoney D, Margaryan E, Topilsky Y, Suri RM, et al. Incidence of aortic complications in patients with bicuspid aortic valves. JAMA. 2011;306(10):1104–12.
Davies RR, Kaple RK, Mandapati D, Gallo A, Botta Jr DM, Elefteriades JA, et al. Natural history of ascending aortic aneurysms in the setting of an unreplaced bicuspid aortic valve. Ann Thorac Surg. 2007;83(4):1338–44.
Borger MA, Preston M, Ivanov J, Fedak PW, Davierwala P, Armstrong S, et al. Should the ascending aorta be replaced more frequently in patients with bicuspid aortic valve disease? J Thorac Cardiovasc Surg. 2004;128(5):677–83.
Goland S, Czer LS, De Robertis MA, Mirocha J, Kass RM, Fontana GP, et al. Risk factors associated with reoperation and mortality in 252 patients after aortic valve replacement for congenitally bicuspid aortic valve disease. Ann Thorac Surg. 2007;83(3):931–7.
Girdauskas E, Disha K, Raisin HH, Secknus MA, Borger MA, Kuntze T. Risk of late aortic events after an isolated aortic valve replacement for bicuspid aortic valve stenosis with concomitant ascending aortic dilation. Eur J Cardiothorac Surg. 2012;42:832–7.
McKellar SH, Michelena HI, Li Z, Schaff HV, Sundt III TM. Long-term risk of aortic events following aortic valve replacement in patients with bicuspid aortic valves. Am J Cardiol. 2010;106(11):1626–33.
Girdauskas E, Borger MA, Secknus MA, Girdauskas G, Kuntze T. Is aortopathy in bicuspid aortic valve disease a congenital defect or a result of abnormal hemodynamics? A critical reappraisal of a one-sided argument. Eur J Cardiothorac Surg. 2011;39(6):809–14.
Girdauskas E, Disha K, Borger MA, Kuntze T. Relation of bicuspid aortic valve morphology to the dilatation pattern of the proximal aorta: focus on the transvalvular flow. Cardiol Res Pract. 2012;2012:478259.
Kallenbach K. Moderate aneuryms of the ascending aorta in stenotic bicuspid aortic valve—life threatening or merely an epiphenomenon? Eur J Cardiothorac Surg. 2012;42:838–9.
Groenink M, Lohuis TA, Tijssen JG, Naeff MS, Hennekam RC, Van Der Wall EE, et al. Survival and complication free survival in Marfan’s syndrome: implications of current guidelines. Heart. 1999;82(4):499–504.
Bonow RO, Carabello BA, Kanu C, de Leon ACJ, Faxon DP, Freed MD, et al. ACC/AHA 2006 guidelines for the management of patients with valvular heart disease: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (writing committee to revise the 1998 Guidelines for the Management of Patients With Valvular Heart Disease): developed in collaboration with the Society of Cardiovascular Anesthesiologists: endorsed by the Society for Cardiovascular Angiography and Interventions and the Society of Thoracic Surgeons. Circulation. 2006;114(5):e84–231.
Vahanian A, Baumgartner H, Bax J, Butchart E, Dion R, Filippatos G, et al. Guidelines on the management of valvular heart disease: The Task Force on the Management of Valvular Heart Disease of the European Society of Cardiology. Eur Heart J. 2007;28(2):230–68.
Warnes CA, Williams RG, Bashore TM, Child JS, Connolly HM, Dearani JA, et al. ACC/AHA 2008 Guidelines for the Management of Adults with Congenital Heart Disease: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (writing committee to develop guidelines on the management of adults with congenital heart disease). Circulation. 2008;118(23):e714–833.
Baumgartner H, Bonhoeffer P, De Groot NM, de Haan F, Deanfield JE, Galie N, et al. ESC Guidelines for the management of grown-up congenital heart disease (new version 2010). Eur Heart J. 2010;31(23):2915–57.
Guntheroth W. Risk of aortic dissection in patients with bicuspid aortic valves. Am J Cardiol. 2011;107(6):958.
Coady MA, Stockwell PH, Robich MP, Poppas A, Sellke FW. Should aortas in patients with bicuspid aortic valve really be resected at an earlier stage than tricuspid? CON Cardiol Clin. 2010;28(2):299–314.
Wald O, Korach A, Shapira OM. Should aortas in patients with bicuspid aortic valve really be resected at an earlier stage than tricuspid? PRO Cardiol Clin. 2010;28(2):289–98.
Vahanian A, Alfieri O, Andreotti F, Antunes MJ, Baron-Esquivias G, Baumgartner H, The Joint Task Force on the Management of Valvular Heart Disease of the European Society of Cardiology (ESC) and the European Association for Cardio-Thoracic Surgery (EACTS), et al. Guidelines on the management of valvular heart disease (version 2012). Eur J Cardiothorac Surg. 2012;33:2451–96.
Ates M. When should we replace the ascending aorta in Marfan syndrome? Eur J Cardiothorac Surg. 2007;31(2):331–2.
Loeys BL, Schwarze U, Holm T, Callewaert BL, Thomas GH, Pannu H, et al. Aneurysm syndromes caused by mutations in the TGF-beta receptor. N Engl J Med. 2006;355(8):788–98.
Aalberts JJ, van den Berg MP, Bergman JE, du Marchie Sarvaas GJ, Post JG, van Unen H, et al. The many faces of aggressive aortic pathology: Loeys-Dietz syndrome. Neth Heart J. 2008;16(9):299–304.
Williams JA, Loeys BL, Nwakanma LU, Dietz HC, Spevak PJ, Patel ND, et al. Early surgical experience with Loeys-Dietz: a new syndrome of aggressive thoracic aortic aneurysm disease. Ann Thorac Surg. 2007;83(2):S757–63.
Hager A, Kaemmerer H, Rapp-Bernhardt U, Blucher S, Rapp K, Bernhardt TM, et al. Diameters of the thoracic aorta throughout life as measured with helical computed tomography. J Thorac Cardiovasc Surg. 2002;123(6):1060–6.
Kaplan S, Aronow WS, Lai H, DeLuca AJ, Weiss MB, Dilmanian H, et al. Prevalence of an increased ascending and descending thoracic aorta diameter diagnosed by multislice cardiac computed tomography in men versus women and in persons aged 23 to 50 years, 51 to 65 years, 66 to 80 years, and 81 to 88 years. Am J Cardiol. 2007;100(10):1598–9.
Lin FY, Devereux RB, Roman MJ, Meng J, Jow VM, Jacobs A, et al. Assessment of the thoracic aorta by multidetector computed tomography: age- and sex-specific reference values in adults without evident cardiovascular disease. J Cardiovasc Comput Tomogr. 2008;2(5):298–308.
Lu TL, Huber CH, Rizzo E, Dehmeshki J, von Segesser LK, Qanadli SD. Ascending aorta measurements as assessed by ECG-gated multi-detector computed tomography: a pilot study to establish normative values for transcatheter therapies. Eur Radiol. 2009;19(3):664–9.
Mulder BJ. The distal aorta in the Marfan syndrome. Neth Heart J. 2008;16(11):382–6.
Engelfriet PM, Boersma E, Tijssen JG, Bouma BJ, Mulder BJ. Beyond the root: dilatation of the distal aorta in Marfan’s syndrome. Heart. 2006;92(9):1238–43.
Engelfriet P, Mulder B. Is there benefit of beta-blocking agents in the treatment of patients with the Marfan syndrome? Int J Cardiol. 2007;114(3):300–2.
Patel HJ, Deeb GM. Ascending and arch aorta: pathology, natural history, and treatment. Circulation. 2008;118(2):188–95.
Hartog AW, Franken R, Zwinderman AH, Groenink M, Mulder BJ. Current and future pharmacological treatment strategies with regard to aortic disease in Marfan syndrome. Expert Opin Pharmacother. 2012;13(5):647–62.
Maron BJ, Zipes DP. Introduction: eligibility recommendations for competitive athletes with cardiovascular abnormalities-general considerations. J Am Coll Cardiol. 2005;45(8):1318–21.
Maron BJ, Chaitman BR, Ackerman MJ, de Bayes LA, Corrado D, Crosson JE, et al. Recommendations for physical activity and recreational sports participation for young patients with genetic cardiovascular diseases. Circulation. 2004;109(22):2807–16.
Sarsam MA, Yacoub M. Remodeling of the aortic valve anulus. J Thorac Cardiovasc Surg. 1993;105(3):435–8.
David TE, Feindel CM. An aortic valve-sparing operation for patients with aortic incompetence and aneurysm of the ascending aorta. J Thorac Cardiovasc Surg. 1992;103(4):617–21.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2014 Springer-Verlag London
About this chapter
Cite this chapter
Cozijnsen, L., Braam, R.L., Schepens, M.A.A.M., Mulder, B.J.M. (2014). Size Matters: Intervention Thresholds for Dissection Prophylaxis in the Ascending Aorta. In: Bonser, R., Pagano, D., Haverich, A., Mascaro, J. (eds) Controversies in Aortic Dissection and Aneurysmal Disease. Springer, London. https://doi.org/10.1007/978-1-4471-5622-2_4
Download citation
DOI: https://doi.org/10.1007/978-1-4471-5622-2_4
Published:
Publisher Name: Springer, London
Print ISBN: 978-1-4471-5621-5
Online ISBN: 978-1-4471-5622-2
eBook Packages: MedicineMedicine (R0)