Abstract
Pulmonary hypertension (PH) is a rare condition. Data on adult PH patients is abundant, but data on pediatric PH are scarce. Nevertheless, in the past decade, increasing data concerning pediatric PH are becoming available, enabling this review of the epidemiology, characterization, and outcome of pediatric pulmonary hypertension.
PH is a condition that is associated with a variety of diseases. It is a rare condition in children with a complex and age-specific presentation. Transient forms of pulmonary arterial hypertension (PAH), i.e., potentially reversible PAH, specifically occur in children and form the largest group of pediatric PH. Advanced PAH in children is predominantly idiopathic or associated with congenital heart disease. Other forms of PAH seldom occur in children. WHO PH groups 2–5 are rare in childhood; however, they may be underreported.
The clinical presentation of pediatric PH is relatively nonspecific as it is in adults, with dyspnea on exertion as the most common presenting symptom. However, the clinical presentation of pediatric PH includes symptoms specific for children such as syncope. Pediatric PH frequently co-occurs with genetic and syndromal abnormalities, including Down syndrome. Right heart failure is less common in children despite a severe hemodynamic profile.
PAH is a detrimental disease with a poor prognosis. Outcome of pediatric PAH differs between patients with different types of congenital heart disease. In the last decades, new PAH-targeted therapies have been developed, which have improved outcome in pediatric pulmonary arterial hypertension. However, currently reported survival rates vary and critical appraisal of patient populations, survival data, and proposed treatment approaches is necessary.
Access provided by Autonomous University of Puebla. Download reference work entry PDF
Similar content being viewed by others
Keywords
- Pulmonary Hypertension
- Pulmonary Arterial Hypertension
- Pulmonary Vascular Resistance
- Pulmonary Blood Flow
- Pulmonary Arterial Hypertension Patient
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
Introduction
Pulmonary hypertension, an increased pressure in the pulmonary artery, is a symptom of a variety of related diseases. Pulmonary hypertension is defined as a mean pulmonary arterial pressure equal to or more than 25 mmHg, measured during right heart catheterization [1]. Pulmonary hypertension can occur at any age, including childhood. However, the presentation of pulmonary hypertension and its associated diseases is age specific (Fig. 119.1) and may differ between children and adults [2]. This chapter will provide an overview of the currently known data concerning the epidemiology, characterization, and outcome of pediatric pulmonary hypertension.
Age of presentation in pediatric PAH. Graphical overview of the age at diagnosis for the different pulmonary hypertension diagnoses, and the percentage of females, congenital heart defects (CHD), and associated syndromal abnormalities (Syndromes) per diagnosis [2]. PPHN Persistent pulmonary hypertension of the newborn, Flow PAH flow-associated pulmonary arterial hypertension without increased pulmonary vascular resistance, Adv. PAH Advanced PAH, iPAH idiopathic PAH, PAH-CHD PAH associated with congenital heart disease, PAH-CTD PAH associated with connective tissue disease, PVOD/PCH Pulmonary veno-occlusive disease/pulmonary capillary hemangiomatosis, HD heart disease, Resp respiratory disease, CTEPH chronic thromboembolic pulmonary hypertension
Classification of Pulmonary Hypertension
Pulmonary hypertension can be clinically classified according to an internationally recognized classification. This classification was proposed and optimized during the successive World Symposium on Pulmonary Hypertension in Evian [3], Venice [4], and Dana Point [5]. It is currently known as the Dana Point classification, and will be reevaluated in Nice in 2013. The Dana Point classification includes five categories based on shared pathophysiological mechanisms: (1) pulmonary arterial hypertension (PAH), (2) pulmonary hypertension owing to left heart disease, (3) pulmonary hypertension owing to lung disease and/or hypoxia, (4) chronic thromboembolic pulmonary hypertension, and (5) pulmonary hypertension with unclear multifactorial mechanisms (Table 119.1) [5].
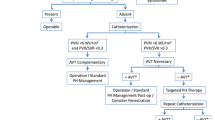
The characterization of PH according to this clinical classification is an essential part of the diagnostic workup of PH (Fig. 119.2) [1, 6, 7]. The treatment strategy and prognosis of pediatric PH largely depend on its subclass and associated conditions. It is therefore of utmost importance to correctly characterize the type of PH using a standardized diagnostic workup.
Diagnostic approach for pediatric PH. Graphic overview of the diagnostic approach for pediatric pulmonary hypertension (Adapted from Barst et al. [6]). P(A)H pulmonary (arterial) hypertension, CXR chest x-ray, Dl CO diffusing capacity of the lung for carbon monoxide, CT computed tomography, HIV human immunodeficiency virus
Although classifying PH by identifying associated conditions may seem rather straightforward, the characterization of pediatric PH is complex. Often, more than one associated condition can be identified, which leaves it to the clinician to determine the contribution of each condition to the PH and to decide on which condition therapy should be focused [8]. Therefore, elaborate specialist knowledge and experience with pulmonary hypertension in children is mandatory in the characterization of the disease, supporting the recommendations of the international guidelines to centralize the care for pulmonary hypertension patients in specialized referral centers [1].
PAH
PAH (group 1) distinguishes itself from the other four categories of the clinical classification by its characteristic pattern of pulmonary vascular remodeling, progressive nature, and response to specific medical therapy. The pulmonary vascular remodeling that is characteristic for PAH involves adventitial thickening, medial hypertrophy, and intimal proliferation, including the formation of concentric laminar intimal fibrosis and plexiform lesions [9–11]. The vascular remodeling leads to arterial wall thickening and occlusion of small distal pulmonary arteries. Together with several other mechanisms including vasoconstriction, inflammation, and thrombosis, the vascular wall thickening and occlusion will consequently increase pressure and pulmonary vascular resistance. This increase in right ventricular afterload increases right ventricular workload, eventually resulting in right ventricular failure and death.
PAH can occur in association with several conditions, including congenital heart diseases (PAH-CHD), connective tissue disease (PAH-CTD), and portal hypertension. Furthermore, PAH can be hereditary (HPAH), either based on familial occurrence of PAH or based on genetic mutations [1]. Germ-line gene mutations have been identified in association with hereditary PAH: bone morphogenetic protein receptor type-2 (BMPR-2), activin-like kinase-1 (ALK-1), and endoglin mutations [12]. Furthermore, recently gene defects in members of the bone morphogenetic protein pathway (SMAD-family pathway) and a caveolin-1 mutation were reported in association with PAH [13, 14]. BMPR-2 is the most common germ-line mutation associated with pediatric PAH. A BMPR-2 mutation can be identified in 10–21 % of the pediatric IPAH/HPAH patients [2, 8, 15].
Finally, PAH can occur without any identifiable causes, which is classified as idiopathic PAH (IPAH). It is important to realize that one or more of the associated conditions included in the clinical classification may be present in PAH patients, although regarded to not sufficiently explain the PAH. In children, it is reported that in 25 % of the cases in which associated conditions could be identified, these were regarded not to be a sufficient explanation for the PAH [8]. In these cases, it is important to consider the possibility of concomitant intrinsic pulmonary vascular disease. Several authors have classified these patients accordingly as “idiopathic-like” PAH patients [8, 16].
IPAH and HPAH are often described together as IPAH/HPAH, because of similarities in presentation and plausible overlap between both disease groups. In 11–40 % of the patients thought to have IPAH, a PAH-associated gene mutation may be present, which would reclassify these patients as HPAH patients [5]. Furthermore, if no familial cases are present, IPAH and HPAH are indistinguishable without screening for known mutations. However, screening for mutations in PAH is not a standard practice, but should be considered with a family history of PAH [1]. Therefore, data concerning IPAH may frequently include HPAH patients, explaining the frequent combined analysis of both groups.
PAH-CHD
PAH-CHD is a progressive vascular disease associated with a broad variety of congenital heart defects. These congenital heart defects are associated with systemic to pulmonary shunts, including ventricular septal defect (VSD), atrial septal defect (ASD), and persistent ductus arteriosus (PDA), but also more complex lesions, such as atrio-ventricular septal defects and univentricular hearts [8, 17]. However, although PAH-CHD is predominantly shunt related, there is a small subset of patients with PAH-CHD associated with adequately repaired obstructive left heart disease, without shunts [2, 17].
In congenital heart defects with systemic to pulmonary shunt, the shunt causes increased pulmonary blood flow. The increased pulmonary blood flow induces vascular wall shear stress, leading to pulmonary vascular remodeling. When congenital heart defects are corrected at an early stage of the disease process, the vascular remodeling can reverse and thus the development of progressive PAH is prevented in most cases.
In contrast, when shunt defects are not corrected, PAH progresses into an advanced stage, which is considered irreversible. Furthermore, correction of shunt defects once PAH is irreversible may cause accelerated deterioration of clinical condition with worse outcome than when the shunt remains uncorrected [2]. Therefore, early correction of congenital systemic to pulmonary shunts, when the vascular remodeling is still reversible, is of major importance. However, the point of no return at which the pulmonary vascular remodeling becomes irreversible is difficult to determine. There is a gray area in which it is unclear whether the vascular remodeling is still reversible or not. In clinical practice, the pulmonary hemodynamic response to acute vasodilator challenge has been used to assess the reversibility of the vascular disease. Empirically, in patients with congenital heart disease, lack of acute response to vasodilator challenges is regarded as an indicator of irreversible disease [18, 19]. However, internationally accepted guidelines for assessing the vasodilator response for this purpose are lacking. Once the pulmonary vascular remodeling progresses into advanced irreversible disease, it is referred to as PAH-CHD.
The evolution of PAH-CHD and the age at which it presents itself depends on the type of shunt (Fig. 119.3) [20]. In patients with a shunt at pre-tricuspid level (for instance, atrial septal defects), there is an increased pulmonary volume load with a normal pressure load. From these patients, only 5–20 % develops advanced PAH, and usually not until the third to fourth decade of life [21, 22]. In patients with nonrestrictive shunts at post-tricuspid level, the increased pulmonary volume load is accompanied by an increased pressure load due to pressure equilibration over the shunt defect. In these patients, PAH usually develops more rapidly, during the first few years of life [20].
Development of PAH in congenital heart defects. Illustration of the development of pulmonary vascular disease in patients with congenital heart disease, separated for the type of shunt. The image shows the variability in the evolution of pulmonary vascular disease based on the type of congenital heart disease. Accelerated PAH-CHD accelerated development of advanced PAH-CHD, Classic Eisenmenger development of Eisenmenger syndrome in patients with post-tricuspid shunt, I-like PAH idiopathic-like PAH, development of PAH in patients with small and initially restrictive shunts, pre-tricuspid shunt development of PAH in pre-tricuspid shunt patients (Adapted from van Loon et al. [20])
However, recently, there have been reports of pediatric PAH patients who developed persistent severe PAH associated with a post-tricuspid shunt already within the first weeks and months of life [8]. These patients have been referred to as accelerated PAH-CHD patients [2, 8]. In these patients, etiological factors in addition to the shunt defect are believed to be present, increasing the susceptibility for pulmonary vascular disease.
In uncorrected systemic to pulmonary shunts, the pulmonary vascular disease is progressive, steadily increasing the pulmonary vascular resistance. When the pulmonary vascular resistance exceeds the systemic vascular resistance, the shunt reverses to a pulmonary to systemic shunt with hypoxemia and cyanosis. This condition is referred to as the Eisenmenger syndrome [1].
Associated PAH
As stated previously, PAH can either be idiopathic, hereditary, associated with congenital heart disease, or associated with several other conditions. These conditions include connective tissue diseases, such as systemic sclerosis, systemic lupus erythematosus, and mixed connective tissue disease [5]. Furthermore, PAH may be associated with HIV infection, portal hypertension, schistosomiasis, chronic hemolytic anemia, and can be drug or toxin induced [5].
Within the Dana Point classification, pulmonary veno-occlusive disease (PVOD) and pulmonary capillary hemangiomatosis (PCH) are classified distinct from but related to PAH. Both conditions share histopathologic changes, clinical presentation, and risk factors with PAH, but on the other hand differ in their response to treatment. In example, in PAH, vasodilators can provide successful treatment; however, in PVOD and PCH, they may cause deterioration of the patient’s condition [23]. Therefore, PVOD and PCH are categorized as group 1′, a distinct category but not completely separated from PAH.
Transient PAH
In general, PAH (group 1 PH) is a progressive fatal disease. Transient PAH is a pulmonary vascular disease that is reversible or self-limiting, but nevertheless is classified in group 1, PAH, according to the current clinical classification. Transient forms of PAH are specific for the pediatric age group and do virtually not occur in adult patients.
Persistent Pulmonary Hypertension of the Newborn (PPHN) is a condition of the newborn characterized by pulmonary hypertension and reduced pulmonary blood flow [24]. In utero, the pulmonary vasculature is subdued to pulmonary arteriolar vasoconstriction and high pulmonary vascular resistance. Due to the high pulmonary vascular resistance, blood shunts from right to left through the foramen ovale and ductus arteriosus. After birth, in the normal lung, pulmonary vascular resistance drops due to lung inflation, nitric oxide release, and increased pulmonary oxygen tension, resulting in a dramatic increase in pulmonary blood flow, and cessation of right to left shunting. In PPHN however, pulmonary vascular resistance remains high, either due to maladaptation, underdevelopment, or maldevelopment of the pulmonary vasculature. In these cases, pulmonary vascular resistance and pulmonary arterial pressure do not decrease, the right to left shunts remain, and pulmonary blood flow will therefore be limited, causing respiratory distress, hypoxemia, and acidosis [24]. Therapy for PPHN includes treatment of underlying disorders, supporting the systemic and pulmonary circulation, optimizing oxygenation and medical therapy to establish pulmonary vasodilatation [24]. Despite therapy, overall mortality and morbidity in patients with PPHN is high (reported as 36 % and 65 %, respectively) [25]. However, if treatment is successful, PPHN fully resolves and is therefore regarded as a reversible or transient form of PAH.
Flow-associated PAH without increased pulmonary vascular resistance includes patients with a left to right shunt based on congenital heart defects, or in rare cases patients with increased pulmonary blood flow due to systemic arteriovenous blood vessel malformations or unilateral pneumonectomy (in whom there is an increased pulmonary blood flow due to redistribution of flow to the remaining lung). In patients with a shunt at pre-tricuspid level or a restrictive shunt at post-tricuspid level, pulmonary blood flow is increased. In normal subjects, the pulmonary circulation can accommodate up to five times the normal cardiac output, without an increase in pulmonary arterial pressure. Therefore, when PH is present in patients with increased pulmonary blood flow without a pressure equilibrating shunt, an abnormal pulmonary vascular response to increased flow should be considered. This may be a sign of intrinsic pulmonary vascular disease. In patients with nonrestrictive shunts at post-tricuspid level, an increased pulmonary blood flow is accompanied by pulmonary and systemic arterial pressure equilibration across the shunt defect. The pressure equilibration causes an increase in pulmonary arterial pressure and hence PH, although in the presence of low pulmonary vascular resistance.
Flow-associated PAH is an early stage of advanced PAH associated with congenital heart disease. In flow-associated PAH, vascular remodeling is likely to be present, due to shear stress of the increased pulmonary blood flow, but may be reversible when the heart defect is corrected. Whereas in advanced PAH, the vascular disease is irreversible, and will progress even after correction of the underlying heart defect. Early correction of the congenital shunt defect in the stage of flow-associated PAH with reversible vascular disease will prevent development of progressive PAH and will resolve the PH. Nevertheless, 3 % of the patients with previously closed systemic to pulmonary shunts were reported to develop PAH during follow-up, which might be due to late correction of the defect [26].
Group 2–5 PH
In PH owing to left heart disease (group 2), PH is caused by left ventricular or valvular dysfunction or total abnormal pulmonary venous return, leading to elevated left atrial and pulmonary venous pressures [5]. The elevated pulmonary venous pressure is transmitted to the lungs, causing increased pulmonary arterial pressure. In this condition, pulmonary vascular resistance initially is normal or near normal.
Group 3 PH is caused by alveolar hypoxia due to lung disease, impaired breathing, or chronic residence at high altitude [5]. The alveolar hypoxia leads to hypoxic vasoconstriction, increasing pulmonary vascular resistance and pulmonary arterial pressure. In childhood, pulmonary developmental disorders may not only cause alveolar hypoxia and hypoxic vasoconstriction, but also include lung hypoplasia and morphological vascular abnormalities with decreased total cross-sectional area of pulmonary vessels, contributing to the increased pulmonary vascular resistance and pressures [27].
Chronic thromboembolic PH (group 4 PH) comprises PH due to obstruction of pulmonary vessels by thromboemboli. And group 5 PH includes forms of PH for which the etiology is multifactorial or unclear [5].
A distinct presentation of PH is the acute pulmonary hypertensive crisis. Generally accepted criteria to define a pulmonary hypertensive crisis are lacking. However, it is often described as a rapid increase in pulmonary vascular resistance, with a pulmonary arterial pressure exceeding systemic blood pressure, accompanied by right ventricular failure, and a decrease in systemic blood pressure [24, 28]. The acute increase in pulmonary vascular resistance is caused by pulmonary vasoconstriction, which can be triggered by hypoxia, hypercarbia, acidosis, or noxious stimuli [28]. Clinically, a PH crisis can typically be recognized by a fall in systemic output accompanied by signs of acute right ventricular failure, with or without cyanosis [2]. PH crisis can occur as a perioperative complication or as a complication of respiratory disease. Specific patient groups, including patients with congenital heart disease, and syndromal abnormalities, may have increased risk of developing PH crisis [2].
Incidence and Prevalence of Pediatric PH
Research covering PH mostly focuses on adult patients, and until recently, data on epidemiology of PH among children was lacking. In the past few years, national cohort studies and registry-based studies were conducted and enabled reports on epidemiology and characterization of pediatric PH. Epidemiologic data may be limited by selection bias. Registry studies in general cover a selected number of referral centers, whose data depend on referral patterns and the used inclusion criteria, whereas hospital registry studies can be hampered by possible coding errors. Van Loon et al. have addressed both issues for pediatric PH in 2011 [2].
The overall yearly incidence of all forms of pediatric PH in the national Netherlands registry was estimated as 64 per million children [2]. The overall incidence rate for pediatric PAH (excluding the transient forms of PAH) was estimated 3.0 cases per million children with a prevalence of 20 cases per million [2]. These numbers are comparable to the reported incidence and prevalence rates of PAH among adults, which have been estimated to range between 2.4–7.6 and 15–52 cases per million adults, respectively [29, 30].
PAH in children is most often caused by IPAH/HPAH or PAH-CHD [8, 17]. The estimated incidence rate of IPAH/HPAH is 0.5–0.7 cases per million children, with a prevalence of 2.1–4.4 cases per million children [2, 31]. This is lower than the reported incidence and prevalence rates of IPAH/HPAH among adults, in whom the incidence rate has been reported as 1.0–3.3 and the prevalence rate as 6.5–25 cases per million adults [29, 30].
The reported incidence rate of PAH-CHD in childhood is 2.2 cases per million children, with a prevalence rate of 15.6 million [2, 31]. In adults, the reported incidence and prevalence rates are lower for PAH-CHD (0.3–2.2 and 1.7–12 cases per million adults, respectively) [29, 30].
In children, PAH is reported to be idiopathic or hereditary in 46–70 % of the cases, making it the largest subgroup of PAH (Fig. 119.4) [8, 17, 32, 33]. PAH-CHD is the second largest subgroup of PAH in children, occurring in 24–37 % of the cases [8, 17, 32, 33]. Compared to the IPAH/HPAH subgroup, this percentage is lower than one would expect based on the prevalence numbers reported on both subgroups. This may be due to the origin of the data. The incidence and prevalence numbers originate from a national epidemiological study, whereas the percentages are reported by large referral centers for pediatric PAH. Incomplete referral of PAH-CHD patients to the referral centers and selection bias due to inclusion criteria of these studies may cause this disparity [2].
Characterization of pediatric PH. Characterization of pediatric pulmonary hypertension, based on the most recent epidemiologic data. (A) and (1) van Loon et al. [2] (2) Berger et al. [17] (3) Fraisse et al. [32] (4) Van Loon et al. [8] (5) Barst et al. [33]. PAH pulmonary arterial hypertension, HD heart disease, CTEPH chronic thromboembolic pulmonary hypertension, CTD connective tissue disease, PVOD/PCH pulmonary vascular occlusive disease/pulmonary capillary hemangiomatosis, PoHT portal hypertension
Pediatric PAH-CHD may present with a broad variety of congenital heart diseases, including isolated shunt defects, partially abnormal pulmonary venous return, complete atrio-ventricular septal defects, transposition of the great arteries without ventricular septal defect, truncus arteriosus, single ventricles, and complex combinations of the mentioned defects. Eisenmenger syndrome is reported in 57 % of pediatric PAH-CHD patients, which is comparable to adult PAH-CHD [8, 26].
PAH associated with conditions other than congenital heart disease is very rare in children [17, 33]. PAH associated with connective tissue disease accounts for only 2–5 % of all pediatric PAH cases [2, 8, 17, 32, 33]. Pulmonary vascular occlusive disease or pulmonary capillary hemangiomatosis (PVOD/PCH) is reported in 2 % of cases [2, 17]. However, since diagnosis of PVOD/PCH is difficult and depends on post-mortal biopsy at autopsy, they may be underdiagnosed [23]. Therefore, the reported percentage may be an underestimation of the actual prevalence of the disease. PAH associated with chronic liver disease and portal hypertension is reported in 1–2 % of the pediatric PAH patients and PAH associated with HIV infection in 0–1 % of the cases [2, 17, 33]. Incidence and prevalence rates of these PAH subgroups are thus far not reported.
The distribution of associated conditions differs between children and adults with PAH. In adults, IPAH/HPAH is also the largest group, accounting for 43–58 % of cases; however, PAH associated with connective tissue disease is much more common among adults (15–35 %), whereas PAH-CHD is a smaller group in adult PAH (11–25 %) compared to children [29, 30]. In adult patients, both PAH associated with portal hypertension and with HIV infection are more common (10.4 % and 6.2 %, respectively) compared to PAH in children [29]. PAH is associated with drugs and toxins in 9.5 % of the adult cases of PAH, whereas the pediatric PAH registries report no patients with PAH associated with drugs and toxins [17, 29].
In pediatric PH, transient forms of PAH were reported to have the highest incidence rates [2]. PPHN is estimated to be responsible for 47 % of all cases of pediatric PH, occurring in 1–2 per 1,000 live births [2, 24, 34]. The incidence of PPHN is reported to be 30 cases per million children. PPHN may be associated with the development of progressive PAH at a later stage. A large international registry for pediatric PH reported 2 % of PH patients to have a previous history of PPHN. In these cases, PPHN either persisted or seemed to be resolved but subsequently recurred, after which PAH was confirmed [17]. Transient, flow-associated PAH without increased pulmonary vascular resistance is estimated to represent 34 % of all pediatric PH patients, with a reported incidence of 22 cases per million children.
In pediatric PH, 13 % of the cases are reported to be pulmonary hypertension classified within the groups 2–5 of the Dana Point Classification. However, since most referral centers and registry studies focus on PAH and often even exclude the other groups of PH, there may be underreporting of these diagnoses. PH due to left heart disease is thought to represent the most frequent cause of PH among adults, but is reported to represent only 5 % of cases in pediatric PH [2, 5]. PH due to lung disease and hypoxia accounts for 8–11 % of the pediatric PH cases [2, 17].
Pediatric PH associated with lung disease and hypoxia results from obstructive or restrictive breathing disorders in 14–24% of cases, including laryngo-tracheomalacia, kyphoscoliosis, micrognathia and/or enlarged adenoid, tonsils or tongue [2, 17]. Residence at high altitude is reported to be responsible for 13 % and interstitial lung disease for 23 % of the cases [17]. Pulmonary developmental disorders are responsible for 58–76 % of the cases, including lung disease of prematurity (bronchopulmonary dysplasia), congenital pulmonary hypoplasia, and congenital diaphragmatic hernia [2, 17]. This is of special interest since pulmonary developmental disorders, such as bronchopulmonary dysplasia, have been reported to be associated with abnormal pulmonary vascular development [27]. Therefore, characterization of PH associated with pulmonary developmental disorders may differ from the group 3 PH in adult patients, and consequently, treatment cannot be extrapolated from adult treatment guidelines. Children with bronchopulmonary dysplasia and PH are at high risk of death, and the treatment approach is not yet clear [35]. Furthermore, the population of patients with PH and bronchopulmonary dysplasia is likely to increase due to improved neonatal care. Therefore, studies focusing on PH based on lung developmental disorders are a necessity.
Chronic thromboembolic PH (group 4) and PH with multifactorial causes (group 5) are very rare in children, representing less than 1 % of the cases of pediatric PH [2, 17]. PH crisis has been reported to occur most often in patients with preexisting PAH (14 % of progressive PAH and 17 % of flow PAH patients), either perioperatively or during respiratory tract infection. However, in rare cases, PH crisis may also occur during respiratory infection without a previous diagnosis of PH [2]. In 19 % of these cases, patients have a syndromal abnormality.
Clinical Presentation
Symptoms and Functional Status
The clinical presentation of pediatric pulmonary hypertension is nonspecific and age dependent. The most common presenting symptom is reduced exercise capacity presented by dyspnea during exercise (65–98 % of patients) [8, 17, 31, 32]. In young infants, a reduced exercise capacity can present with feeding problems and failure to thrive. Other symptoms include fatigue, cyanosis with exercise or at rest, cough, and chest pain. Signs of right ventricular failure are relatively rare in children with PH, which is in contrast to adult patients in whom signs of right ventricular failure are common [36]. Syncope as a presenting symptom is specific for pediatric pulmonary hypertension. Syncope is reported in 25–31 % of pediatric PAH patients, which is twice the percentage in adult patients and is most frequent in patients without a shunt defect [17, 31, 37]. There is often a long delay between onset of symptoms and diagnosis, which may be due to the low specificity of the presenting symptoms and the rarity of the disease. Because of the progressive nature of pediatric PAH, early identification and diagnosis of patients is important. Therefore, screening of patients belonging to high-risk groups based on underlying conditions or family members with PAH is advised.
The functional status of PAH patients, concerning exercise capacity and symptoms, can be classified using the World Health Organization (WHO) functional classification of pulmonary hypertension [1]. Generally, children with PAH present with WHO functional class II or III (72–80 % of cases), which is in contrast to adults who generally present in WHO functional class III [8, 17, 31, 32]. Nevertheless, a substantial group of pediatric patients can be classified in the advanced functional classes III and IV at diagnosis, which is probably due to the delay between disease onset and diagnosis, underlining the importance of early diagnosis in pediatric PAH [8, 17]. In adult patients, treatment effect can be measured using changes in WHO functional class; however, in pediatric patients, the value of WHO functional class in assessing treatment effect is less clear.
A measurement of exercise capacity is the 6-minute walk distance, the distance a patient walks within 6 minutes under standardized conditions [1]. In adults, the 6-mininute walk distance is commonly used to assess exercise capacity and disease severity in PAH. However, in children, its value is limited since it is often not feasible, especially in the young children and children with syndromal abnormalities including mental retardation. Children also frequently lack the ability to focus during the examination.
Hemodynamic Profile
Severely increased pulmonary arterial pressure and pulmonary vascular resistance characterize the hemodynamic profile in pediatric PH. In pediatric patients, the right atrial pressure and cardiac index are generally preserved, which is in contrast to PH in adult patients [2, 17, 38].
The prevalence of acute pulmonary vasodilator response in children with PAH has been a topic of debate. It has long been assumed that children show more response to vasodilator challenge than adult patients, due to less extensive pulmonary vascular disease. The proportion of patients with an acute pulmonary vasodilator response was reported to be 42–56 % in children compared to 5–17 % in adult patients [7, 39–42]. However, in children, different response criteria were used instead of the internationally advised response criteria used in adult patients. A recent study directly comparing the proportion of acute responders in adult and pediatric patients using the same criteria showed that the prevalence of acute response in children is comparable to that in adults (8 % in children according to the current criteria) [42].
Comorbidities
Pediatric pulmonary hypertension frequently co-occurs with genetic disorders (17–43 % of cases; illustrated by Fig. 119.5), including specific syndromal, chromosomal, or genetic abnormalities and dysmorphism and/or mental retardation without a specified syndromal diagnosis [2, 8, 17]. Down syndrome is the most common concomitant syndrome (12–21 % of cases) and is reported to be more common in group 3 PH than in progressive PAH [2, 17]. Focusing on progressive PAH patients, trisomy-21 occurs most frequently within the PAH-CHD patient group [8]. Patients with Down syndrome are at higher risk for developing PH due to several potential causes for PH, including disordered breathing due to upper airway obstruction, congenital heart defects, sleep disordered breathing, silent aspiration, and pulmonary hypoplasia. Furthermore, Down syndrome patients have been suggested to have an increased susceptibility for intrinsic pulmonary vascular disease.
Syndromal abnormalities in pediatric PH. Illustration of the types and numbers of syndromal abnormalities found in a national cohort of pediatric pulmonary hypertension patients, separated for diagnosis (Adapted from van Loon et al. [8]). PAH pulmonary arterial hypertension, CHD congenital heart disease, CTD connective tissue disease, RSH disorders of respiratory system and/or hypoxia, CTEPH chronic thromboembolic pulmonary hypertension, NOMID Neonatal onset multisystem inflammatory disease
In addition to trisomy-21, several other syndromes have been reported to co-occur with PH, such as Noonan, Velocardiofacial, Jacobsen, 1p36 deletion, and neonatal onset multisystem inflammatory disease syndromes [8]. Furthermore, it is recognized that a substantial number of pediatric PH patients have clinical signs of syndromal disorders, such as dysmorphic features and/or mental retardation, which cannot be explained by a known syndromal diagnosis [8]. The frequent occurrence of syndromal and chromosomal abnormalities in pediatric PAH, especially those without a syndromal diagnosis, suggests the existence of still unknown genetic pathways involved in the disease process of PH.
Considering the age-specific forms of PAH, the complex presentation and the variety of associated conditions and comorbidities specific for pediatric PH, there is debate on whether the current classification of PH is suitable for pediatric PH. Several pediatric classifications have been proposed, but are not standard in the clinical care for children with PH [43, 44].
Outcomes
Pulmonary hypertension is a heterogeneous disease. The outcome of the different subgroups of pediatric pulmonary hypertension differs tremendously. In patients in the Dana Point groups 2–5, PH may resolve by treatment of the underlying disease.
In contrast, PAH (group 1) has no cure and outcome is therefore poor. In adult patients, the untreated median survival after diagnosis for IPAH/HPAH is estimated at 2.8 years [45]. Evidence-based reports on the untreated survival of pediatric PAH are lacking, but may be worse than in the adult patient group. The untreated median survival of pediatric PAH patients has been suggested to be 0.8 year, which has been reported following a study within the National Institutes of Health registry.
In the past decade, new medical PAH-targeted therapies have been introduced to treat PAH. Recently, three reports have described outcome and survival of pediatric PAH patients in the era in which PAH-targeted therapy has been available. There is a discrepancy between the survivals shown in these reports (Fig. 119.6). Comparing these studies, the 1-, 3-, and 5-year survival of pediatric PAH is in the range of 86–100 %, 71–88 %, and 66–72 %, respectively, for IPAH/HPAH and 87–96 %, 87 %, and 81 %, respectively, for PAH-CHD [33, 46–48]. In pediatric PAH, survival of IPAH/HPAH patients seems similar to PAH-CHD patients. However, within the PAH-CHD group, survival varies greatly, depending on the type of congenital heart defect. Patients with PAH-CHD persisting or recurring after shunt closure, and patients with accelerated PAH-CHD were reported to have significant reduced survival compared to patients with an uncorrected pre-tricuspid or post-tricuspid shunt [2].
Survival of pediatric PAH. Survival of pediatric pulmonary arterial hypertension patients in the era of PAH-targeted therapy (Adapted from (1) Van Loon et al. [46], (2) Haworth and Hislop [48], (3) Ivy et al. [47]), illustrating the variability in the presented survival rates for pediatric PAH. IPAH idiopathic pulmonary arterial hypertension, HPAH hereditary PAH, PAH-CHD PAH associated with congenital heart disease, APAH associated PAH including PAH-CHD, PH associated with respiratory disorders, and PAH associated with connective tissue disease, HIV infection, bone marrow transplantation, or metabolic disorders
Survival of pediatric PAH is reported to be improved after the introduction of PAH-targeted therapy, when compared to the predicted untreated survival [46]. However, data suggest that this improvement is more profound in prevalent cases than in incident cases, which underlines the importance of critical appraisal of the adult treatment guidelines when adapting them to the pediatric PAH population [46].
Conclusion
Pulmonary hypertension (PH) in children is a rare condition with a complex age-specific presentation, including age-specific diagnoses. The occurrence of transient forms of PAH, i.e., potentially reversible PAH, is specific for PH in childhood and the most frequently occurring subgroup of pediatric PH. Advanced pediatric PAH is predominantly idiopathic or associated with congenital heart disease. PH groups 2–5 are rare in children; however, they may be underreported.
The clinical presentation of pediatric pulmonary hypertension is nonspecific, which may explain the delay between onset of symptoms and diagnosis. Characteristics that are uniquely associated with pediatric PH, in contrast to PH among adults, include lack of right heart failure in most children despite a severe hemodynamic profile and the occurrence of syncope as a presenting symptom. Pediatric PH frequently presents with comorbidities such as Down syndrome, chromosomal disorders, and other undefined syndromal abnormalities. This observation suggests the existence of still unknown genetic pathways involved in the disease process of PH.
Outcome of pulmonary arterial hypertension is poor. Adult treatment guidelines have yielded improved outcome among children with PAH. However, a critical appraisal of treatment guidelines and development of new therapies is necessary in children.
References
Authors/Task Force Members, Galie N, Hoeper MM et al (2009) Guidelines for the diagnosis and treatment of pulmonary hypertension: the task force for the diagnosis and treatment of pulmonary hypertension of the European Society of Cardiology (ESC) and the European Respiratory Society (ERS), endorsed by the International Society of Heart and Lung Transplantation (ISHLT). Eur Heart J 30:2493–2537
van Loon RL, Roofthooft MT, Hillege HL et al (2011) Pediatric pulmonary hypertension in the Netherlands: epidemiology and characterization during the period 1991 to 2005. Circulation 124:1755–1764
Fishman AP (1998) Etiology and pathogenesis of primary pulmonary hypertension: a perspective. Chest 114:242S–247S
Simonneau G, Galie N, Rubin LJ et al (2004) Clinical classification of pulmonary hypertension. J Am Coll Cardiol 43:5S–12S
Simonneau G, Robbins IM, Beghetti M et al (2009) Updated clinical classification of pulmonary hypertension. J Am Coll Cardiol 54:S43–S54
Barst RJ, Ertel SI, Beghetti M et al (2011) Pulmonary arterial hypertension: a comparison between children and adults. Eur Respir J 37:665–677
Rosenzweig EB, Widlitz AC, Barst RJ (2004) Pulmonary arterial hypertension in children. Pediatr Pulmonol 38:2–22
van Loon RL, Roofthooft MT, Osch-Gevers M et al (2009) Clinical characterization of pediatric pulmonary hypertension: complex presentation and diagnosis. J Pediatr 155:176–182
Humbert M, Morrell NW, Archer SL et al (2004) Cellular and molecular pathobiology of pulmonary arterial hypertension. J Am Coll Cardiol 43:13S–24S
Jeffery TK, Morrell NW (2002) Molecular and cellular basis of pulmonary vascular remodeling in pulmonary hypertension. Prog Cardiovasc Dis 45:173–202
Pietra GG, Capron F, Stewart S et al (2004) Pathologic assessment of vasculopathies in pulmonary hypertension. J Am Coll Cardiol 43:25S–32S
Harrison RE, Berger R, Haworth SG et al (2005) Transforming growth factor-beta receptor mutations and pulmonary arterial hypertension in childhood. Circulation 111:435–441
Nasim MT, Ogo T, Ahmed M et al (2011) Molecular genetic characterization of SMAD signaling molecules in pulmonary arterial hypertension. Hum Mutat 32:1385–1389
Austin ED, Ma L, Leduc C et al (2012) Whole exome sequencing to identify a novel gene (Caveolin-1) associated with human pulmonary arterial hypertension. Circ Cardiovasc Genet 5(3):336–343
Rosenzweig EB, Morse JH, Knowles JA et al (2008) Clinical implications of determining BMPR2 mutation status in a large cohort of children and adults with pulmonary arterial hypertension. J Heart Lung Transplant 27:668–674
Schulze-Neick I, Beghetti M (2008) Classifying pulmonary hypertension in the setting of the congenitally malformed heart–cleaning up a dog’s dinner. Cardiol Young 18:22–25
Berger RM, Beghetti M, Humpl T et al (2012) Clinical features of paediatric pulmonary hypertension: a registry study. Lancet 379:537–546
Berner M, Beghetti M, Spahr-Schopfer I et al (1996) Inhaled nitric oxide to test the vasodilator capacity of the pulmonary vascular bed in children with long-standing pulmonary hypertension and congenital heart disease. Am J Cardiol 77:532–535
Berger RM (2000) Possibilities and impossibilities in the evaluation of pulmonary vascular disease in congenital heart defects. Eur Heart J 21:17–27
van Loon RL, Roofthooft MT, Berger RM (2009) Pulmonary arterial hypertension in children with congenital heart disease. PVRI Rev 1:219–223
Andrews R, Tulloh R, Magee A et al (2002) Atrial septal defect with failure to thrive in infancy: hidden pulmonary vascular disease? Pediatr Cardiol 23:528–530
Tulloh RM (2005) Congenital heart disease in relation to pulmonary hypertension in paediatric practice. Paediatr Respir Rev 6:174–180
Ivy DD, Feinstein JA, Humpl T et al (2009) Non-congenital heart disease associated pediatric pulmonary arterial hypertension. Prog Paediatr Cardiol 27:13–23
Stayer SA, Liu Y (2010) Pulmonary hypertension of the newborn. Best Pract Res Clin Anaesthesiol 24:375–386
Roofthooft MT, Elema A, Bergman KA et al (2011) Patient characteristics in persistent pulmonary hypertension of the newborn. Pulm Med 2011:858154
Duffels MG, Engelfriet PM, Berger RM et al (2007) Pulmonary arterial hypertension in congenital heart disease: an epidemiologic perspective from a Dutch registry. Int J Cardiol 120:198–204
Stenmark KR, Abman SH (2005) Lung vascular development: implications for the pathogenesis of bronchopulmonary dysplasia. Annu Rev Physiol 67:623–661
Carmosino MJ, Friesen RH, Doran A et al (2007) Perioperative complications in children with pulmonary hypertension undergoing noncardiac surgery or cardiac catheterization. Anesth Analg 104:521–527
Humbert M, Sitbon O, Chaouat A et al (2006) Pulmonary arterial hypertension in France: results from a national registry. Am J Respir Crit Care Med 173:1023–1030
Peacock AJ, Murphy NF, McMurray JJ et al (2007) An epidemiological study of pulmonary arterial hypertension. Eur Respir J 30:104–109
Moledina S, Hislop AA, Foster H et al (2010) Childhood idiopathic pulmonary arterial hypertension: a national cohort study. Heart 96:1401–1406
Fraisse A, Jais X, Schleich JM et al (2010) Characteristics and prospective 2-year follow-up of children with pulmonary arterial hypertension in France. Arch Cardiovasc Dis 103:66–74
Barst RJ, McGoon MD, Elliott CG et al (2012) Survival in childhood pulmonary arterial hypertension: insights from the registry to evaluate early and long-term pulmonary arterial hypertension disease management. Circulation 125:113–122
Walsh-Sukys MC, Tyson JE, Wright LL et al (2000) Persistent pulmonary hypertension of the newborn in the era before nitric oxide: practice variation and outcomes. Pediatrics 105:14–20
Khemani E, McElhinney DB, Rhein L et al (2007) Pulmonary artery hypertension in formerly premature infants with bronchopulmonary dysplasia: clinical features and outcomes in the surfactant era. Pediatrics 120:1260–1269
Rich S, Dantzker DR, Ayres SM et al (1987) Primary pulmonary hypertension. A national prospective study. Ann Intern Med 107:216–223
Le RJ, Fenstad ER, Maradit-Kremers H et al (2011) Syncope in adults with pulmonary arterial hypertension. J Am Coll Cardiol 58:863–867
Badesch DB, Raskob GE, Elliott CG et al (2010) Pulmonary arterial hypertension: baseline characteristics from the REVEAL registry. Chest 137:376–387
Barst RJ, Maislin G, Fishman AP (1999) Vasodilator therapy for primary pulmonary hypertension in children. Circulation 99:1197–1208
Barst RJ (1986) Pharmacologically induced pulmonary vasodilatation in children and young adults with primary pulmonary hypertension. Chest 89:497–503
Sitbon O, Humbert M, Jais X et al (2005) Long-term response to calcium channel blockers in idiopathic pulmonary arterial hypertension. Circulation 111:3105–3111
Douwes JM, van Loon RL, Hoendermis ES et al (2011) Acute pulmonary vasodilator response in paediatric and adult pulmonary arterial hypertension: occurrence and prognostic value when comparing three response criteria. Eur Heart J 32:3137–3146
van Albada ME, Berger RM (2008) Pulmonary arterial hypertension in congenital cardiac disease–the need for refinement of the Evian-Venice classification. Cardiol Young 18:10–17
Cerro MJ, Abman S, Diaz G et al (2011) A consensus approach to the classification of pediatric pulmonary hypertensive vascular disease: report from the PVRI Pediatric Taskforce, Panama 2011. Pulm Circ 1:286–298
D’Alonzo GE, Barst RJ, Ayres SM et al (1991) Survival in patients with primary pulmonary hypertension. Results from a national prospective registry. Ann Intern Med 115:343–349
van Loon RL, Roofthooft MT, Delhaas T et al (2010) Outcome of pediatric patients with pulmonary arterial hypertension in the era of new medical therapies. Am J Cardiol 106:117–124
Ivy DD, Rosenzweig EB, Lemarie JC et al (2010) Long-term outcomes in children with pulmonary arterial hypertension treated with bosentan in real-world clinical settings. Am J Cardiol 106:1332–1338
Haworth SG, Hislop AA (2009) Treatment and survival in children with pulmonary arterial hypertension: the UK Pulmonary Hypertension Service for Children 2001–2006. Heart 95:312–317
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2014 Springer-Verlag London
About this entry
Cite this entry
Douwes, J.M., Berger, R.M.F. (2014). Epidemiology of Pediatric Pulmonary Hypertension. In: Da Cruz, E., Ivy, D., Jaggers, J. (eds) Pediatric and Congenital Cardiology, Cardiac Surgery and Intensive Care. Springer, London. https://doi.org/10.1007/978-1-4471-4619-3_204
Download citation
DOI: https://doi.org/10.1007/978-1-4471-4619-3_204
Published:
Publisher Name: Springer, London
Print ISBN: 978-1-4471-4618-6
Online ISBN: 978-1-4471-4619-3
eBook Packages: MedicineReference Module Medicine