Abstract
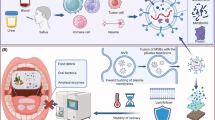
Saliva is a complex oral biofluid composed of various biological molecules secreted by major and minor salivary glands, as well as by-products of host oral cells, oral bacteria, small extracellular vesicles (sEVs), and gingival crevicular fluid. Recently, salivary small extracellular vesicles and salivary multi-omics (microbiome, transcriptome, DNA methylome and proteome) are emerging as potential diagnostic tools for oral diseases, including the highly prevalent periodontitis. Here, we describe the methodologies for how to isolate salivary sEVs using the size exclusion chromatography method, and how to perform salivaomics, which may guide future dental research.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Kc S, Wang XZ, Gallagher JE (2020) Diagnostic sensitivity and specificity of host-derived salivary biomarkers in periodontal disease amongst adults: systematic review. J Clin Periodontol. 47(3):289–308. https://doi.org/10.1111/jcpe.13218
Giannobile WV (2012) Salivary diagnostics for periodontal diseases. J Am Dent Assoc 143(10 Suppl):6s–11s. https://doi.org/10.14219/jada.archive.2012.0341
Dawes C, Wong DTW (2019) Role of saliva and salivary diagnostics in the advancement of oral health. J Dent Res 98(2):133–141. https://doi.org/10.1177/0022034518816961
Jiao K, Walsh LJ, Ivanovski S, Han P (2021) The emerging regulatory role of circular rnas in periodontal tissues and cells. Int J Mol Sci 22(9):4636. https://doi.org/10.3390/ijms22094636
Han P, Bartold PM, Ivanovski S (2021) The emerging role of small extracellular vesicles in saliva and gingival crevicular fluid as diagnostics for periodontitis. J Periodont Res 57(1):219–231. https://doi.org/10.1111/jre.12950
Han P, Ivanovski S (2020) Saliva-friend and foe in the COVID-19 outbreak. Diagnostics 10(5):290. https://doi.org/10.3390/diagnostics10050290
Lapić I, Šegulja D, Rogić D (2021) Assessment of salivary antibody response to BNT162b2 mRNA COVID-19 vaccination. J Med Virol 93(9):5257–5259. https://doi.org/10.1002/jmv.27096
Han P, Bartold PM, Salomon C, Ivanovski S (2020) Salivary small extracellular vesicles associated miRNAs in periodontal status – a pilot study. Int J Mol Sci 21(8):2809. https://doi.org/10.3390/ijms21082809
Han P, Lai A, Salomon C, Ivanovski S (2020) Detection of salivary small extracellular vesicles associated inflammatory cytokines gene methylation in gingivitis. Int J Mol Sci 21(15):5273. https://doi.org/10.3390/ijms21155273
Hua S, Bartold PM, Gulati K, Moran CS, Ivanovski S, Han P (2021) Periodontal and dental pulp cell-derived small extracellular vesicles: a review of the current status. Nanomaterials 11(7):1858. https://doi.org/10.3390/nano11071858
Han P, Bartold PM, Salomon C, Ivanovski S (2021) Salivary outer membrane vesicles and DNA methylation of small extracellular vesicles as biomarkers for periodontal status: a pilot study. Int J Mol Sci 22(5):2423. https://doi.org/10.3390/ijms22052423
Pappa E, Kousvelari E, Vastardis H (2019) Saliva in the “omics” era: a promising tool in paediatrics. Oral Dis 25(1):16–25. https://doi.org/10.1111/odi.12886
Li X, Zhao Q, Wei W, Lin Q, Magnan C, Emami MR et al (2019) The DNA modification N6-methyl-2’-deoxyadenosine (m6dA) drives activity-induced gene expression and is required for fear extinction. Nature Neuroscience 22(4):534–544. https://doi.org/10.1038/s41593-019-0339-x
Théry C, Witwer KW, Aikawa E, Alcaraz MJ, Anderson JD, Andriantsitohaina R et al (2018) Minimal information for studies of extracellular vesicles 2018 (MISEV2018): a position statement of the International Society for Extracellular Vesicles and update of the MISEV2014 guidelines. J Extracell Vesicles 7(1):1535750. https://doi.org/10.1080/20013078.2018.1535750
Lee RSB, Hamlet SM, Moon HJ, Ivanovski S (2021) Re-establishment of macrophage homeostasis by titanium surface modification in type II diabetes promotes osseous healing. Biomaterials 267:120464. https://doi.org/10.1016/j.biomaterials.2020.120464
Han P, Ivanovski S (2019) Effect of saliva collection methods on the detection of periodontium-related genetic and epigenetic biomarkers – a pilot study. Int J Mol Sci 20(19):4729. https://doi.org/10.3390/ijms20194729
Papapanou PN, Sanz M, Buduneli N, Dietrich T, Feres M, Fine DH et al (2018) Periodontitis: consensus report of workgroup 2 of the 2017 world workshop on the classification of periodontal and peri-implant diseases and conditions. J Periodontol 89(Suppl 1):S173–S182. https://doi.org/10.1002/JPER.17-0721
Han P, Liu T, Vaquette C, Frazer D, Anderson G, Ivanovski S (2022) Iron accumulation is associated with periodontal destruction in a mouse model of HFE-related haemochromatosis. J Periodont Res 57(2):294–304. https://doi.org/10.1111/jre.12959
Chee B, Park B, Bartold PM (2013) Periodontitis and type II diabetes: a two-way relationship. Int J Evid Based Healthc 11(4):317–329. https://doi.org/10.1111/1744-1609.12038
Li Y, Zhou X, John MARS, Wong DTW (2004) RNA profiling of cell-free saliva using microarray technology. J Dent Res 83(3):199–203. https://doi.org/10.1177/154405910408300303
Lau WW, Hardt M, Zhang YH, Freire M, Ruhl S (2021) The human salivary proteome wiki: a community-driven research platform. J Dent Res 100(13):1510–1519. https://doi.org/10.1177/00220345211014432
Acknowledgments
This work was supported by the Australian Dental Research Foundation (grant number 2741-2020 to PH, XL, WW, SI), the National Science Foundation of China (82001420 to XL; 82171517 to WW), and the Research Foundation of medical Sci-Tech innovation platform of Zhongnan Hospital (PTXM2021006).
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2023 The Author(s), under exclusive license to Springer Science+Business Media, LLC, part of Springer Nature
About this protocol
Cite this protocol
Han, P., Li, X., Wei, W., Ivanovski, S. (2023). Saliva Diagnosis Using Small Extracellular Vesicles and Salivaomics. In: Seymour, G.J., Cullinan, M.P., Heng, N.C., Cooper, P.R. (eds) Oral Biology. Methods in Molecular Biology, vol 2588. Humana, New York, NY. https://doi.org/10.1007/978-1-0716-2780-8_3
Download citation
DOI: https://doi.org/10.1007/978-1-0716-2780-8_3
Published:
Publisher Name: Humana, New York, NY
Print ISBN: 978-1-0716-2779-2
Online ISBN: 978-1-0716-2780-8
eBook Packages: Springer Protocols