Abstract
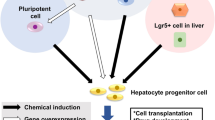
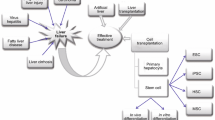
Hepatocytes are liver parenchymal cells involved in performing various metabolic reactions. During the development of therapeutic drugs, toxicological assays are conducted using hepatocyte cultures before clinical trials. However, since primary hepatocytes cannot proliferate and rapidly lose their functions in vitro, many efforts have been put into modifying culture conditions to expand primary hepatocytes and induce hepatocyte functions in intrinsic and extrinsic stem/progenitor cells. In this chapter, we summarize recent advances in preparing hepatocyte cultures and induction of hepatocytes from various cellular sources.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Miyajima A, Tanaka M, Itoh T (2014) Stem/progenitor cells in liver development, homeostasis, regeneration, and reprogramming. Cell Stem Cell 14(5):561–574. https://doi.org/10.1016/j.stem.2014.04.010
Furuyama K, Kawaguchi Y, Akiyama H et al (2011) Continuous cell supply from a Sox9-expressing progenitor zone in adult liver, exocrine pancreas and intestine. Nat Genet 43(1):34–41. https://doi.org/10.1038/NG.722
Español-Suñer R, Carpentier R, Van Hul N et al (2012) Liver progenitor cells yield functional hepatocytes in response to chronic liver injury in mice. Gastroenterology 143(6). https://doi.org/10.1053/J.GASTRO.2012.08.024
Gadd VL, Aleksieva N, Forbes SJ (2020) Epithelial plasticity during liver injury and regeneration. Cell Stem Cell 27(4):557–573. https://doi.org/10.1016/J.STEM.2020.08.016
Tanimizu N, Mitaka T (2017) Which is better source for functional hepatocytes? Stem Cell Investig 4:12. https://doi.org/10.21037/SCI.2017.02.08
Katsuda T, Hosaka K, Matsuzaki J et al (2020) Transcriptomic dissection of hepatocyte heterogeneity: linking ploidy, zonation, and stem/progenitor cell characteristics. CMGH 9(1):161–183. https://doi.org/10.1016/J.JCMGH.2019.08.011
Rombaut M, Boeckmans J, Rodrigues RM et al (2021) Direct reprogramming of somatic cells into induced hepatocytes: cracking the Enigma code. J Hepatol 75(3):690–705. https://doi.org/10.1016/J.JHEP.2021.04.048
Luce E, Messina A, Duclos-Vallée J et al (2021) Advanced techniques and awaited clinical applications for human pluripotent stem cell differentiation into hepatocytes. Hepatology 74(2):1101–1116. https://doi.org/10.1002/hep.31705
Mitaka T, Mikami M, Sattler GL et al (1992) Small cell colonies appear in the primary culture of adult rat hepatocytes in the presence of nicotinamide and epidermal growth factor. Hepatology 16(2):440–447. https://doi.org/10.1002/hep.1840160224
Gj G, Wb C, Jw G (2000) Temporal analysis of hepatocyte differentiation by small hepatocyte-like progenitor cells during liver regeneration in retrorsine-exposed rats. Am J Pathol 157(3):771–786. https://doi.org/10.1016/S0002-9440(10)64591-9
Sasaki K, Kon J, Mizuguchi T et al (2008) Proliferation of hepatocyte progenitor cells isolated from adult human livers in serum-free medium. Cell Transplant 17(10–11):1221–1230. https://doi.org/10.3727/096368908787236666
Tanimizu N, Ichinohe N, Ishii M et al (2016) Liver progenitors isolated from adult healthy mouse liver efficiently differentiate to functional hepatocytes in vitro and repopulate liver tissue. Stem Cells 34(12):2889–2901. https://doi.org/10.1002/STEM.2457
Tanimizu N, Ichinohe N, Sasaki Y et al (2021) Generation of functional liver organoids on combining hepatocytes and cholangiocytes with hepatobiliary connections ex vivo. Nat Commun 12(1). https://doi.org/10.1038/S41467-021-23575-1
Wei Y, Wang YG, Jia Y et al (2021) Liver homeostasis is maintained by midlobular zone 2 hepatocytes. Science 371(6532). https://doi.org/10.1126/science.abb1625
He L, Pu W, Liu X et al (2021) Proliferation tracing reveals regional hepatocyte generation in liver homeostasis and repair. Science 371(6532). https://doi.org/10.1126/science.abc4346
Katsuda T, Kawamata M, Hagiwara K et al (2017) Conversion of terminally committed hepatocytes to culturable bipotent progenitor cells with regenerative capacity. Cell Stem Cell 20(1):41–55. https://doi.org/10.1016/j.stem.2016.10.007
Zhang K, Zhang L, Liu W et al (2018) In vitro expansion of primary human hepatocytes with efficient liver repopulation capacity. Cell Stem Cell 23(6):806–819.e4. https://doi.org/10.1016/j.stem.2018.10.018
Katsuda T, Matsuzaki J, Yamaguchi T et al (2019) Generation of human hepatic progenitor cells with regenerative and metabolic capacities from primary hepatocytes. eLife 8. https://doi.org/10.7554/ELIFE.47313
Chuan PW, Kraaier LJ, Kluiver TA (2021) Hepatocyte organoids and cell transplantation: what the future holds. Exp Mol Med. https://doi.org/10.1038/s12276-021-00579-x
Hu H, Gehart H, Artegiani B et al (2018) Long-term expansion of functional mouse and human hepatocytes as 3D organoids. Cell 175(6):1591–1606.e19. https://doi.org/10.1016/j.cell.2018.11.013
Peng WC, Logan CY, Fish M et al (2018) Inflammatory cytokine TNFα promotes the long-term expansion of primary hepatocytes in 3D culture. Cell 175(6):1607–1619.e15. https://doi.org/10.1016/j.cell.2018.11.012
Yanger K, Zong Y, Maggs LR et al (2013) Robust cellular reprogramming occurs spontaneously during liver regeneration. Genes Dev 27(7):719–724. https://doi.org/10.1101/gad.207803.112
Yimlamai D, Christodoulou C, Galli GG et al (2014) Hippo pathway activity influences liver cell fate. Cell 157(6):1324–1338. https://doi.org/10.1016/j.cell.2014.03.060
Tarlow BD, Pelz C, Naugler WE et al (2014) Bipotential adult liver progenitors are derived from chronically injured mature hepatocytes. Cell Stem Cell 15(5):605–618. https://doi.org/10.1016/j.stem.2014.09.008
Tanimizu N, Nishikawa Y, Ichinohe N et al (2014) Sry HMG box protein 9-positive (Sox9+) epithelial cell adhesion molecule-negative (EpCAM−) biphenotypic cells derived from hepatocytes are involved in mouse liver regeneration. J Biol Chem 289(11):7589–7598. https://doi.org/10.1074/JBC.M113.517243
Choi T, Ninov N, Stainier DYR et al (2014) Extensive conversion of hepatic biliary epithelial cells to hepatocytes after near total loss of hepatocytes in zebrafish. Gastroenterology 146(3):776–788. https://doi.org/10.1053/j.gastro.2013.10.019
Raven A, Lu W, Man TY et al (2017) Cholangiocytes act as facultative liver stem cells during impaired hepatocyte regeneration. Nature 547(7663):350–354. https://doi.org/10.1038/nature23015
Schaub JR, Huppert KA, Kurial SNT et al (2018) De novo formation of the biliary system by TGFβ-mediated hepatocyte transdifferentiation. Nature 557(7704):247–251. https://doi.org/10.1038/s41586-018-0075-5
Sekiya S, Suzuki A (2011) Direct conversion of mouse fibroblasts to hepatocyte-like cells by defined factors. Nature 475(7356):390–395. https://doi.org/10.1038/nature10263
Huang P, He Z, Ji S et al (2011) Induction of functional hepatocyte-like cells from mouse fibroblasts by defined factors. Nature 475(7356):386–389. https://doi.org/10.1038/nature10116
Rezvani M, Español-Suñer R, Malato Y et al (2016) In vivo hepatic reprogramming of myofibroblasts with AAV vectors as a therapeutic strategy for liver fibrosis. Cell Stem Cell 18(6):809–816. https://doi.org/10.1016/j.stem.2016.05.005
Song G, Pacher M, Balakrishnan A et al (2016) Direct reprogramming of hepatic myofibroblasts into hepatocytes in vivo attenuates liver fibrosis. Cell Stem Cell 18(6):797–808. https://doi.org/10.1016/j.stem.2016.01.010
Nakano Y, Kamiya A, Sumiyoshi H et al (2020) A deactivation factor of fibrogenic hepatic stellate cells induces regression of liver fibrosis in mice. Hepatology 71(4). https://doi.org/10.1002/hep.30965/suppinfo
Huang P, Zhang L, Gao Y et al (2014) Direct reprogramming of human fibroblasts to functional and expandable hepatocytes. Cell Stem Cell 14(3):370–384. https://doi.org/10.1016/j.stem.2014.01.003
Katayama H, Yasuchika K, Miyauchi Y et al (2017) Generation of non-viral, transgene-free hepatocyte like cells with piggyBac transposon. Sci Rep 7. https://doi.org/10.1038/srep44498
Guo R, Tang W, Yuan Q et al (2017) Chemical cocktails enable hepatic reprogramming of mouse fibroblasts with a single transcription factor. Stem Cell Rep 9(2):499. https://doi.org/10.1016/J.STEMCR.2017.06.013
Ballester M, Bolonio M, Santamaria R et al (2019) Direct conversion of human fibroblast to hepatocytes using a single inducible polycistronic vector. Stem Cell Res Ther 10(1). https://doi.org/10.1186/s13287-019-1416-5
Nitta S, Kusakari Y, Yamada Y et al (2020) Conversion of mesenchymal stem cells into a canine hepatocyte-like cells by Foxa1 and Hnf4a. Regen Ther 14:165–176. https://doi.org/10.1016/j.reth.2020.01.003
Odom DT, Zizlsperger H, Gordon DB et al (2004) Control of pancreas and liver gene expression by HNF transcription factors. Science 303(5662):1378–1381. https://doi.org/10.1126/science.1089769
Odom DT, Dowell RD, Jacobsen ES et al (2006) Core transcriptional regulatory circuitry in human hepatocytes. Mol Syst Biol 2. https://doi.org/10.1038/msb4100059
Horisawa K, Udono M, Ueno K et al (2020) The dynamics of transcriptional activation by hepatic reprogramming factors. Mol Cell 79(4):660–676.e8. https://doi.org/10.1016/j.molcel.2020.07.012
Yu B, He ZY, You P et al (2013) Reprogramming fibroblasts into bipotential hepatic stem cells by defined factors. Cell Stem Cell 13(3):328–340. https://doi.org/10.1016/j.stem.2013.06.017
Inada H, Udono M, Matsuda-Ito K et al (2020) Direct reprogramming of human umbilical vein- and peripheral blood-derived endothelial cells into hepatic progenitor cells. Nat Commun 11(1):5292. https://doi.org/10.1038/s41467-020-19041-z
Martin GR (1981) Isolation of a pluripotent cell line from early mouse embryos cultured in medium conditioned by teratocarcinoma stem cells. Proc Natl Acad Sci 78(12):7634–7638. https://doi.org/10.1073/PNAS.78.12.7634
Evans MJ, Kaufman MH (1981) Establishment in culture of pluripotential cells from mouse embryos. Nature 292(5819):154–156. https://doi.org/10.1038/292154a0
Takahashi K, Yamanaka S (2006) Induction of pluripotent stem cells from mouse embryonic and adult fibroblast cultures by defined factors. Cell 126(4):663–676. https://doi.org/10.1016/J.CELL.2006.07.024
Takahashi K, Tanabe K, Ohnuki M et al (2007) Induction of pluripotent stem cells from adult human fibroblasts by defined factors. Cell 131(5):861–872. https://doi.org/10.1016/j.cell.2007.11.019
Banas A, Yamamoto Y, Teratani T et al (2007) Stem cell plasticity: learning from hepatogenic differentiation strategies. Dev Dyn 236(12):3228–3241. https://doi.org/10.1002/dvdy.21330
Song Z, Cai J, Liu Y et al (2009) Efficient generation of hepatocyte-like cells from human induced pluripotent stem cells. Cell Res 19(11):1233–1242. https://doi.org/10.1038/cr.2009.107
Si-Tayeb K, Noto FK, Nagaoka M et al (2010) Highly efficient generation of human hepatocyte-like cells from induced pluripotent stem cells. Hepatology 51(1):297–305. https://doi.org/10.1002/hep.23354
Rashid ST, Corbineau S, Hannan N et al (2010) Modeling inherited metabolic disorders of the liver using human induced pluripotent stem cells. J Clin Invest 120(9):3127–3136. https://doi.org/10.1172/JCI43122
Takebe T, Sekine K, Enomura M et al (2013) Vascularized and functional human liver from an iPSC-derived organ bud transplant. Nature 499(7459):481–484. https://doi.org/10.1038/nature12271
Koui Y, Kido T, Ito T et al (2017) An in vitro human liver model by iPSC-derived parenchymal and non-parenchymal cells. Stem Cell Rep 9(2):490–498. https://doi.org/10.1016/J.STEMCR.2017.06.010
Overeem AW, Klappe K, Parisi S et al (2019) Pluripotent stem cell-derived bile canaliculi-forming hepatocytes to study genetic liver diseases involving hepatocyte polarity. J Hepatol 71(2):344–356. https://doi.org/10.1016/j.jhep.2019.03.031
Takeishi K, Hortet AC d l’, Wang Y et al (2020) Assembly and function of a bioengineered human liver for transplantation generated solely from induced pluripotent stem cells. Cell Rep 31(9):107711. https://doi.org/10.1016/J.CELREP.2020.107711
Treyer A, Müsch A (2013) Hepatocyte polarity. Compr Physiol 3(1):243–287. https://doi.org/10.1002/CPHY.C120009
Fu D, Wakabayashi Y, Lippincott-Schwartz J et al (2011) Bile acid stimulates hepatocyte polarization through a cAMP-Epac-MEK-LKB1-AMPK pathway. Proc Natl Acad Sci U S A 108(4):1403–1408. https://doi.org/10.1073/pnas.1018376108
Homolya L, Fu D, Sengupta P et al (2014) LKB1/AMPK and PKA control ABCB11 trafficking and polarization in hepatocytes. PLoS One 9(3):e91921. https://doi.org/10.1371/journal.pone.0091921
Belicova L, Repnik U, Delpierre J et al (2021) Anisotropic expansion of hepatocyte lumina enforced by apical bulkheads. J Cell Biol 220(10). https://doi.org/10.1083/JCB.202103003
Deguchi S, Shintani T, Harada K et al (2021) In vitro model for a drug assessment of cytochrome P450 family 3 subfamily A member 4 substrates using human induced pluripotent stem cells and genome editing technology. Hepatol Commun 5(8):1385–1399. https://doi.org/10.1002/hep4.1729
Haridass D, Yuan Q, Becker PD et al (2009) Repopulation efficiencies of adult hepatocytes, fetal liver progenitor cells, and embryonic stem cell-derived hepatic cells in albumin-promoter-enhancer urokinase-type plasminogen activator mice. Am J Pathol 175(4):1483–1492. https://doi.org/10.2353/AJPATH.2009.090117
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2022 The Author(s), under exclusive license to Springer Science+Business Media, LLC, part of Springer Nature
About this protocol
Cite this protocol
Okumura, A., Tanimizu, N. (2022). Preparation of Functional Human Hepatocytes Ex Vivo. In: Tanimizu, N. (eds) Hepatocytes. Methods in Molecular Biology, vol 2544. Humana, New York, NY. https://doi.org/10.1007/978-1-0716-2557-6_20
Download citation
DOI: https://doi.org/10.1007/978-1-0716-2557-6_20
Published:
Publisher Name: Humana, New York, NY
Print ISBN: 978-1-0716-2556-9
Online ISBN: 978-1-0716-2557-6
eBook Packages: Springer Protocols