Abstract
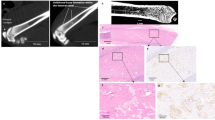
Many types of solid tumors metastasize to the bone, where it causes significant morbidity and mortality in patients with advanced disease. Bone metastases are not only incurable but also affect bone health which impairs patients’ quality of life. In order to understand the mechanisms and develop effective treatments for bone-metastatic disease, it is first necessary to develop animal models that permit the assessment of tumor growth in the bone and progressive structural changes of the bone simultaneously. Longitudinal analysis of bone tumor progression is generally performed by bioluminescent imaging; however, this method is not able to assess progressive structural changes of the bone. Here, we describe a simple method for assessment of bone lesions using a scoring system that takes into account disease burden and bone destruction using longitudinal radiographs.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Charhon SA, Chapuy MC, Delvin EE, Valentin-Opran A, Edouard CM, Meunier PJ (1983) Histomorphometric analysis of sclerotic bone metastases from prostatic carcinoma special reference to osteomalacia. Cancer 51(5):918–924. https://doi.org/10.1002/1097-0142(19830301)51:5<918::aid-cncr2820510526>3.0.co;2-j
Mundy GR (2002) Metastasis to bone: causes, consequences and therapeutic opportunities. Nat Rev Cancer 2(8):584–593. https://doi.org/10.1038/nrc867
Coleman R, Body JJ, Aapro M, Hadji P, Herrstedt J, Group EGW (2014) Bone health in cancer patients: ESMO clinical practice guidelines. Ann Oncol 25(suppl 3):iii124–iii137. https://doi.org/10.1093/annonc/mdu103
Tsuzuki S, Park SH, Eber MR, Peters CM, Shiozawa Y (2016) Skeletal complications in cancer patients with bone metastases. Int J Urol 23(10):825–832. https://doi.org/10.1111/iju.13170
O’Neill K, Lyons SK, Gallagher WM, Curran KM, Byrne AT (2010) Bioluminescent imaging: a critical tool in pre-clinical oncology research. J Pathol 220(3):317–327. https://doi.org/10.1002/path.2656
Shearer RF, Saunders DN (2015) Experimental design for stable genetic manipulation in mammalian cell lines: lentivirus and alternatives. Genes Cells 20(1):1–10. https://doi.org/10.1111/gtc.12183
Honore P, Luger NM, Sabino MA, Schwei MJ, Rogers SD, Mach DB, O’Keefe PF, Ramnaraine ML, Clohisy DR, Mantyh PW (2000) Osteoprotegerin blocks bone cancer-induced skeletal destruction, skeletal pain and pain-related neurochemical reorganization of the spinal cord. Nat Med 6(5):521–528. https://doi.org/10.1038/74999
Bloom AP, Jimenez-Andrade JM, Taylor RN, Castaneda-Corral G, Kaczmarska MJ, Freeman KT, Coughlin KA, Ghilardi JR, Kuskowski MA, Mantyh PW (2011) Breast cancer-induced bone remodeling, skeletal pain, and sprouting of sensory nerve fibers. J Pain 12(6):698–711. https://doi.org/10.1016/j.jpain.2010.12.016
Grenald SA, Doyle TM, Zhang H, Slosky LM, Chen Z, Largent-Milnes TM, Spiegel S, Vanderah TW, Salvemini D (2017) Targeting the S1P/S1PR1 axis mitigates cancer-induced bone pain and neuroinflammation. Pain 158(9):1733–1742. https://doi.org/10.1097/j.pain.0000000000000965
Thompson ML, Jimenez-Andrade JM, Chartier S, Tsai J, Burton EA, Habets G, Lin PS, West BL, Mantyh PW (2015) Targeting cells of the myeloid lineage attenuates pain and disease progression in a prostate model of bone cancer. Pain 156(9):1692–1702. https://doi.org/10.1097/j.pain.0000000000000228
Park SH, Eber MR, Shiozawa Y (2019) Models of prostate cancer bone metastasis. Methods Mol Biol 1914:295–308. https://doi.org/10.1007/978-1-4939-8997-3_16
Acknowledgments
This work is directly supported by the National Cancer Institute (R01-CA238888, Y.S.), Department of Defense (W81XWH-17-1-0541, Y.S.; W81XWH-19-1-0045, Y.S.; and W81XWH-17-1-0542, C.M.P.), and the Wake Forest Baptist Comprehensive Cancer Center Internal Pilot Funding (Y.S.). This work is also supported by the National Cancer Institute’s Cancer Center Support Grant award number P30-CA012197 issued to the Wake Forest Baptist Comprehensive Cancer Center. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Cancer Institute.
Conflict of Interests
Y.S. has received research funding from TEVA Pharmaceuticals but not relevant to this study.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2022 Springer Science+Business Media, LLC, part of Springer Nature
About this protocol
Cite this protocol
Eber, M.R., Jiménez-Andrade, J.M., Peters, C.M., Shiozawa, Y. (2022). A Method of Bone-Metastatic Tumor Progression Assessment in Mice Using Longitudinal Radiography. In: Deep, G. (eds) Cancer Biomarkers. Methods in Molecular Biology, vol 2413. Humana, New York, NY. https://doi.org/10.1007/978-1-0716-1896-7_1
Download citation
DOI: https://doi.org/10.1007/978-1-0716-1896-7_1
Published:
Publisher Name: Humana, New York, NY
Print ISBN: 978-1-0716-1895-0
Online ISBN: 978-1-0716-1896-7
eBook Packages: Springer Protocols