Abstract
Scientific reports underscore the importance of measuring the health-related quality of life in sarcoidosis patients. The present study seeks to define how sarcoidosis patients’ quality of life, daily physical activity, and physical performance are related to each other. Seventeen patients (mean age 46.8 ± 8.8 years) suffering from sarcoidosis completed the following questionnaires: the fatigue assessment scale (FAS), the quality of life scale (SF-36 questionnaire), and the Borg dyspnea scale. Physical activity (PA) was assessed using accelerometry. Respiratory function, consisting of forced expiratory volume in one second (FEV1), forced vital capacity (FVC), forced expiratory volume in one second as a percentage of vital capacity (FEV1/%FVC), and diffusing capacity of the lungs for carbon monoxide (DLCO), were assessed. In addition, performance in 6-min walk test (MWT), aerobic capacity assessed from maximal oxygen uptake (VO2max), and the metabolic equivalent of task (MET) were evaluated. We found that daily PA (4566 ± 2378 steps/day) and VO2max (21.8 ± 5.9 ml/kg/min) were lower in sarcoidosis patients than the known predicted values in healthy age-matched individuals. There were significant inverse associations between the FAS score and 6MWT (r = −0.62; p < 0.01), and between SF-36 score and 6MWT (r = −0.55; p < 0.03). In contrast, SF-36 scores associated with fatigue and dyspnea scores (r = 0.72; p < 0.001 and r = 0.85; p < 0.001). These findings imply that sarcoidosis patients are less active compared with healthy subjects. The FAS and SF-36 scales seem to be effective tools for assessing the severity of fatigue in sarcoidosis patients.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
1 Introduction
Sarcoidosis, a multi-organ disease, is the second most frequent pathological condition involving the respiratory system in young and middle-aged persons after asthma (De Vries et al. 2004). Its clinical picture shows the presence of granulomas in the lymph glands, lungs, eyes, skin, and in other organs. Sarcoidosis may give no symptoms, or have an acute or chronic course. The unspecific symptoms of sarcoidosis include elevated body temperature, muscle pain, general weakness, perspiration, and weight loss (Baughmann et al. 2011). The organ manifestations of respiratory sarcoidosis – the most frequent form of this condition – include the development of dyspnea and progressing circulatory and respiratory insufficiency. Other manifestations include the involvement of lung parenchyma and hilar lymph glands, erythema nodosum in the skin, fever, and joint pain and swelling. All these symptoms comprise the Löfgren syndrome (Judson 2008). Around 10% of sarcoidosis patients are diagnosed with pleural effusion and the involvement of the upper respiratory tract with airway obstruction symptoms. Spirometry shows reduced maximal expiratory flows at MEF50%FVC and MEF25%FVC (Radwan et al. 1999). Another element of the respiratory system affected by sarcoidosis is the pulmonary vessels. Clinical conditions that can impair breathing capacity, leading also to lower exercise tolerance and fatigue, are pulmonary hypertension, pulmonary embolism, and granulomatosis with polyangiitis. Reports from studies on sarcoidosis patients point to reduced capacity for physical work and reluctance toward mental work. The psychophysical condition of these patients significantly influences their self-assessment of health and quality of life regardless of the severity of the symptoms (De Kleijn et al. 2009; Drent et al. 1998; Ebrahim 1995). It has been demonstrated that performing the quality-of-life assessment, in addition to functional and clinical assessments, is essential to determine the efficacy of therapies for many chronic conditions, including sarcoidosis (De Vries et al. 2010; Michielsen et al. 2007; Smith et al. 1999). In view of the circumstances outlined above, the present study seeks to define how sarcoidosis patients’ quality of life, daily physical activity, and physical performance are related to each another.
2 Methods
2.1 Subjects
The study protocol was approved by the Bioethics Commission of the Medical University of Silesia in Poland. All participants were familiarized with the rules and goals of the study and signed informed consent. The study was conducted at the Clinic for Pulmonary Diseases and Tuberculosis in Zabrze, Poland The study sample consisted of 17 persons (7 women and 10 men) aged 46.8 ± 8.8 years, with the mean body mass of 81.6 ± 15.1 kg (59% of them were overweight), who suffered from sarcoidosis for no longer than 4 years. All patients were diagnosed with sarcoidosis according to the criteria developed by the American Thoracic Society/World Association for Sarcoidosis ATS/ERS/WASOG (Hunninghake et al. 1999).
The inclusion criteria were as follows:
-
a stable period of the disease, without infections or exacerbation in the preceding month;
-
glucocorticosteroids and immunosuppressants not administered in the past;
-
baseline medical examination showing no indications for treatment;
-
cardiorespiratory function satisfying the requirements of a graded exercise test;
-
motor function satisfying the requirements of a graded exercise test.
The exclusion criteria included:
-
ischaemic heart disease, heart failure, and severe pulmonary hypertension;
-
serious liver dysfunction and diabetes;
-
cerebral stroke;
-
addiction to cigarettes, drugs, or alcohol;
-
dementia;
-
motor or neurological dysfunction preventing exercise;
-
reluctance or lack of consent to cooperate.
2.2 Assessment of Pulmonary Function
All subjects were tested for pulmonary function using a Jaeger-Masterlab spirometer (Erich Jaeger GmbH; Warzburg, Germany). Three lung function parameters were measured: forced expiratory volume in one second (FEV1), forced vital capacity (FVC), and forced expiratory volume in one second as a percentage of vital capacity (FEV1/%FVC). The diffusing capacity of the lungs for carbon monoxide (DLCO) was measured using a single-breath method. Results were normalized to the reference values proposed by the European Community for Coal and Steel and were presented as percentage of the predicted values (Quanjer et al. 1993).
2.3 Assessment of Physical Capacity
All the patients performed a graded treadmill exercise test during which their maximal oxygen uptake (VO2max) and the metabolic equivalent of task (MET) were measured. To assess physical efficiency, a six-minute walk test (6MWT) was employed. The 6MWT was conducted according to the 2002 American Thoracic Society guidelines which consider the distance walked in meters (Frost et al. 2005; Gibbons et al. 2001). Heart rate (HR) was monitored and the spirometric and gasometric parameters were recorded at rest, during, and post-exercise (Ergospirometr Metalyzer 3B-2R; Cortex, Leipzig, Germany). After a three-minute warm-up on the treadmill, exercise intensity was increased according to the Bruce protocol. Participants exercised until they reached the maximum workload they could tolerate or until voluntary muscle failure. Maximal oxygen uptake (VO2max) was determined based on the maximum heart rate criterion (HRmax) and the expiratory exchange ratio (RER) exceeding a value of 1.1 (ACSM 2014; Golding 2000).
2.4 Assessment of Physical Activity
Physical activity (PA) of patients was measured using an Actigraph GT3X+ device (Actigraph; Pensacola, FL) that monitors the number of steps and the amount of energy expended during daily physical activity. The primary indicator of PA, i.e., the number of steps/d, was enhanced by daily energy expenditure (kcal/kg/d). The device was activated after the participants were instructed on how to use it and was worn by them for 7 days, from 7 a.m. to 22 p.m. On day 7, the recorded data were downloaded for analysis by a dedicated software (Actilife 6; Actigraph, Pensacola, FL). The analysis was performed by the same investigator who supervised the duration of measurements. The energy expenditure and the number of steps obtained from the accelerometer were compared with values recommended for the age-group investigated (Tudor-Locke et al. 2002).
2.5 Questionnaires
All the partients were asked to complete questionnaires assessing their:
-
fatigue (the Fatigue Assessment Scale – FAS) with the following score intervals: (10–21 – fatigue is not perceived); (22–34 – fatigue is perceived); (35–50 – a very strong feeling of fatigue) (De Vries et al. 2004);
-
dyspnea (the modified analog Borg dyspnoea scale (0–10));
-
quality of life (the SF-36 questionnaire enabling the self-assessment of quality of life with respect to the physical domain (SF-physical) and mental domain (SF-mental) divided into 8 subscales). According to the Polish interpretation of the SF-36, the higher the composite score on the questionnaire’s 0–100 scale, the lower quality of life (Tylka and Piotrowicz 2009).
2.6 Statistical Analysis
For the quantitative interval variables, descriptive statistics such as means, medians, standard deviations, and extreme values were calculated and then tested for normal distribution using the Shapiro-Wilk test. For the qualitative categorical variables, the number and percentage distributions were determined. Variable correlations for patients’ clinical status, experienced fatigue, physical capacity, and quality of life were estimated with the use of canonical correlation analysis, multiple regression analysis, analysis of variance, and non-parametric tests (Spearman’s rank correlation, Kruskal-Wallis analysis of variance and chi-square (χ2) tests of independence). A p-value < 0.05 defined statistical significance. Statistical analysis of the data was performed using Statistica v12.5 (StatSoft Polska, Cracow, Poland).
3 Results
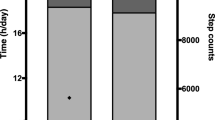
The sarcoidosis patients’ somatic characteristics and results of spirometry examinations are shown in Table 1. The mean FVC amounted to 85.9 ± 35.8%predicted. Symptoms of mild airway obstruction, with FEV1/FVC > 0.7, were recognized in five of the patients. The assessment of the patients’ physical performance is shown in Table 2. VO2max obtained from the graded exercise test (ExTest) was 21.8 ± 5.9 (ml/kg/min) and constituted 72.9 ± 21.8% of its predicted value; and HRmax exceeded 90% of the predicted value. The mean daily PA consisting of 4566 ± 2378 steps/day was lower than predicted. The patients were the least active on Sundays (Fig. 1). The result of their 6MWT amounted to 544.3 ± 45.5 m, which was lower than the standard 600.2 ± 102.0 m for their age-group.
The patients had a distinct, albeit moderate, perception of fatigue and dyspnea, with the scores of 29.0 ± 4.0 and 4.1 ± 2.2 points on the FAS and Borg scales, respectively. The Borg score associated with that of FAS (r = 0.74; p < 0.001) (Fig. 2).
The patients scored 62.0 ± 19.1 on the SF-36. Physical and mental domain scores (53.1 ± 19.3 and 23.5 ± 12.9, respectively) associated with each other (r = 0.74; p < 0.001), and both mental domain and fatigue scores associated inversely with 6MWT (r = −0.51; p < 0.04 and r = −0.62; p < 0.01, respectively) (Fig. 3).
The inverse associations between the performance in 6MWT, on the one side, and SF-36 score (r = −0.50; p = 0.03) and its mental domain (r = −0.51; p = 0.04), on the other side, were significant (Fig. 3). Both the Borg score of dyspnea and the FAS score of fatigue associated with the SF-36 score; r = 0.84 (p < 0.0001; Fig. 4) and r = 0.72 (p = 0.001; Fig. 5), respectively.
We failed to find any appreciable associations between the sarcoidosis patients’ VO2max and self-assessed quality of life or MET. HRmax obtained from the exercise test showed a tendency for inverse associations with both fatigue (r = −0.37) and SF-36 quality of life scores (r = −0.37) (p = 0.10).
4 Discussion
Fatigue associated with sarcoidosis, clinically difficult to diagnose and classify, is a recognized issue in its treatment. Nonetheless, research has failed to explain how fatigue relates to the clinical course of sarcoidosis (Jastrzębski et al. 2015; Costabel 2011). The present study was undertaken to assess the efficacy of methods measuring fatigue in sarcoidosis patients and to determine how the patients’ self-assessments of fatigue, physical capacity, and performance relate to each other. We demonstrate that a poor performance in 6MWT significantly associated with fatigue and lower SF-36-assessed quality of life and its mental sphere. In addition, dyspnea significantly associated with greater fatigue and lower quality of life. The results of graded exercise and 6-min walk tests demonstrate that the assessment of fatigue is most reliable in the judgment on physical functioning in sarcoidosis patients. The patients’ performance in 6MWT in the present study was akin to that reported by Alhamed (2009), who has also found that the 6MWT distance and the Borg dyspnea score are inversely correlated. The fatigue results reported in other studies also show that these patients find physical activity onerous regardless of the level of pulmonary dysfunction, the stage of treatment, or the level of immunological markers (Drent et al. 2012; De Kleijn et al. 2011).
The assessments of fatigue and quality of life are effective tools in predicting the capability of physical functioning in patients suffering from sarcoidosis. We demonstrate that sarcoidosis patients had moderate aerobic insufficiency and failed to achieve the VO2max levels and 6MWT performance typical of their age-group. The patients’ daily physical activity was lower than recommended, as also was exercise capacity when compared with the ACSM (2014) and Golding (2000) standards of percent predicted MET. Sarcoidosis is a chronic condition associated with unsolved problems relating to its pathogenesis, treatment, and management. Studies show that a high percentage of sarcoidosis patients have reduced exercise tolerance and perceive tiredness (De Vries et al. 2004). There are no reports pointing to associations between the results of clinical tests, such as pulmonary function, radiography, or inflammatory markers – IL-2 receptors, C-reactive protein, amyloid A – and fatigue. Interestingly, the only variable in this group of patients that correlates with fatigue is a lower diffusing capacity of the lungs for carbon monoxide. The outcomes of other questionnaire surveys involving sarcoidosis patients show that the perception of fatigue, general weakness, and short breath during daily activities erodes the patient motivation for work. Dyspnea and fatigue adversely influence quality of life and, in some cases, lead to depression (Valeyre and Humbert 2012; Sharma 1999; Drent et al. 1998).
It is known that exercise training can improve health, physical capacity, and respiratory muscle function in patients with respiratory conditions, and it can alleviate their feeling of fatigue and dyspnea (Spruit et al. 2013; Langer et al. 2012; Hospes et al. 2009; Baugmann et al. 2007). The research on rehabilitation of patients with respiratory insufficiency demonstrates that accelerometry provides a precise measurement of daily physical activity. The advantage of the method is that it records data over a relatively long period and it enables a 3D analysis of motion (Lores et al. 2006; Nguyen et al. 2006; Coronado et al. 2003; Steele et al. 2003). Daily physical activity of patients with obstructive lung disease correlates with their performance in 6MWT and it is lower compared with that in control subjects (Lores et al. 2006). The association between 6MWT results, which are indicative of exercise tolerance, and self-assessed duration of daily physical activity is reported to be high and positive (Zieleźnik et al. 2015). The knowledge of physical dysfunction and lower quality of life perceived by sarcoidosis patients may be useful in setting the appropriate rehabilitative strategies for them (Lingner et al. 2015).
Michielsen et al. (2007) have studied 150 middle-aged sarcoidosis patients. More than 80% of those patients experienced fatigue and one half of them reported a reduced exercise tolerance. The main causes of lower quality of life in that study were fatigue, dyspnea, reduced physical capacity, and a joint pain. It is noteworthy that fatigue is a major predictor of quality of life and both physical and mental health. In the present study, reduced exercise tolerance also was accompanied by an enhanced perception of fatigue and a reduced quality of life, particularly in its mental dimension. Other authors have found similar associations in sarcoidosis patients, with a somehow higher score on the fatigue assessment scale than that obtained in the present study (Fleisher et al. 2014; Hinz et al. 2011).
In conclusion, the present study demonstrates a substantial reduction in physical capacity and a lower exercise tolerance in middle-aged sarcoidosis patients. Patients’ physical capacity was below the standard recommended for age-matched healthy subjects. The fatigue assessment scale and the SF-36 quality of life questionnaire proved useful tools in denoting the self-perceived capability of physical and metal functioning in sarcoidosis patients.
References
ACSM (2014) ACSM’s guidelines for exercise testing and prescription, 9th edn. Lippincott Williams & Wilkins, Baltimore
Alhamed EH (2009) The six-minute walk test in patients with pulmonary sarcoidosis. Ann Thorac Med 4(2):60–64
Baughmann RP, Culver DA, Judson MA (2011) A concise review of pulmonary sarcoidosis. Am J Respir Crit Care Med 183(5):573–581
Baugmann RP, Sparkman BK, Lower EE (2007) Six minute walk test and health status assessment in sarcoidosis. Chest 132(1):207–213
Coronado M, Janssens JP, de Muralt B, Terrier P, Schutz Y, Fitting JW (2003) Walking activity measured by accelerometry during respiratory rehabilitation. J Cardpulm Rehabil 23:357–364
Costabel U (2011) Skeletal muscle weakness, fatigue and sarcoidosis. Curr Probl Psychiatry 12(2):141–145
De Kleijn WP, Elfferich MD, De Vries J, Jonker GJ, Lower EE, Baugmann RP, King TE Jr, Drent M (2009) Fatigue in sarcoidosis: American versus Dutch patients. Sarcoidosis Vasc Diffuse Lung Dis 26(2):92–97
De Kleijn WP, Drent M, Vermunt JK, Shigemitsu H, De Vries J (2011) Types of fatigue in sarcoidosis patients. J Psychosom Res 71(6):416–422
De Vries J, Michielsen HJ, Van Heck GL, Drent M (2004) Measuring fatique in sarcoidosis: the fatigue assessment scale (FAS). Br J Health Psychol 9(3):279–291
De Vries J, Lower EE, Drent M (2010) Quality of life in sarcoidosis: assessment and management. Semin Respir Crit Care Med 31(4):485–493
Drent M, Wrinsberger RM, Breteler MH, Kock LM, de Vries J, Wouters EF (1998) Quality of life and depressive symptoms in patients suffering from sarcoidosis. Sarcoidosis Vasc Diffuse Lung Dis 15(1):59–66
Drent M, Lower EE, De Vries J (2012) Sarcoidosis-associated fatigue. Eur Respir J 40(1):255–263
Ebrahim S (1995) Clinical and public health perspectives and applications of health-related quality of life measurement. Soc Sci Med 41(10):1383–1394
Fleisher M, Hinz A, Brahler E, Wirtz H, Bosse-Henc A (2014) Factors associated with fatigue in sarcoidosis. Respir Care 59(7):1086–1094
Frost AE, Langleben D, Oudiz R, Hill N, Horn E, McLaughlin V, Robbins IM, Shapiro S, Tapson VF, Zwicke D, DeMarco T, Schilz R, Rubenfire M, Barst RJ (2005) The 6-min walk test (6MW) as an efficacy endpoint in pulmonary arterial hypertension clinical trials: demonstration of a ceiling effect. Vasc Pharmacol 43(1):36–39
Gibbons WJ, Fruchter N, Sloan S, Levy RD (2001) Reference values for a multiple repetition 6-minute walk test in healthy adults older than 20 years. J Cardpulm Rehabil 21(2):87–93
Golding LA (2000) YMCA fitness testing and assessment manual, 4th edn. Human Kinetics, Champaign
Hinz A, Fleischer M, Brähler E, Wirtz H, Bosse-Henck A (2011) Fatigue in patients with sarcoidosis, compared with the general population. Gen Hosp Psychiatry 33(5):462–468
Hospes G, Bossenbroek L, den Hacken NH, van Hengel P, de Greef MH (2009) Enhancement of daily physical activity increases physical fitness of outclinic COPD patients: results of an exercise counseling program. Patient Educ Couns 75(2):274–278
Hunninghake GW, Costabel U, Ando M, Baughman R et al (1999) ATS/ERS/WASOG statement on sarcoidosis. Sarcoidosis Vasc Diffuse Lung Dis 16(2):149–173
Jastrzębski D, Ziora D, Lubecki M, Zieleźnik K, Maksymiak M, Hanzel J, Początek A, Kolczyńska A, Nguyen Thi L, Żebrowska A, Kozielski J (2015) Fatique in sarcoidosis an exercise tolerance, dyspnea, and quality of life. Adv Exp Med Biol 833:31–36
Judson MA (2008) Sarcoidosis: clinical presentation, diagnosis, and approach to treatment. Am J Med Sci 335(1):26–33
Langer D, Cebrià i Iranzo MA, Burtin C, Verleden SE, Vanaudenaerde BM, Troosters T, Decramer M, Verleden GM, Gosselink R (2012) Determinants of physical activity in daily life in candidates for lung transplantation. Respir Med 106(5):747–754
Lingner H, Großhennig A, Flunkert K, Buhr-Schinner H, Heitmann R, Tönnesmann U, van der Meyden J, Schultz K (2015) ProKaSaRe study protocol: a prospective multicenter study of pulmonary rehabilitation of patients with sarcoidosis. Adv Exp Med Biol 833:31–36
Lores V, García-Río F, Rojo B, Alcolea S, Mediano O (2006) Recording the daily physical activity of COPD patients with an accelerometer: an analysis of agreement and repeatability. Arch Broncopneumol 42(12):627–632
Michielsen HJ, Peros-Golubicic T, Drent M, De Vries J (2007) Relationship between symptoms and quality of life in a sarcoidosis population. Respiration 74(4):401–405
Nguyen HQ, Steele B, Benditt JO (2006) Use of accelerometers to characterize physical activity patterns with COPD exacerbations. Int J Chron Obstruct Pulmon Dis 1(4):455–460
Quanjer PH, Tammeling GJ, Cotes JE, Pedersen OF, Peslin R, Yernault JC (1993) Lung volumes and forced ventilatory flows. Report of working party standardization of lung function tests. European Community for steel and coal. Official statement of the European Respiratory Society. Eur Respir J Suppl 16:5–40
Radwan L, Zielonka TM, Maszczyk Z, Meleniewska-Maciszewska A, Hawryłkiewicz I (1999) Functional disturbances in patients with interstitial lung diseases without signs of restriction. Pneumonol Alergol Pol 67(5–6):180–188. (Article in Polish)
Sharma OP (1999) Fatigue and sarcoidosis. Eur Respir J 13(4):713–714
Smith KW, Avis NE, Assman SF (1999) Distinguishing between quality of life and health status in quality of life research: a meta-analysis. Qual Life Res 8:447–459
Spruit MA, Singh SJ, Garvey C et al (2013) An official American Thoracic Society/European Respiratory Society statement: key concepts and advances in pulmonary rehabilitation. Am J Respir Crit Care Med 188(8):e13–e64
Steele BG, Belza B, Hunziker J, Holt L, Legro M, Coppersmith J, Buchner D, Lakshminaryan S (2003) Monitoring daily activity during pulmonary rehabilitation using a triaxial accelerometer. J Cardpulm Rehabil 23:139–142
Tudor-Locke C, Ainsworth BE, Thompson RW, Matthews CE (2002) Comparison of pedometer and accelerometer measures of free-living physical activity. Med Sci Sports Exerc 34(12):2045–2051
Tylka J, Piotrowicz R (2009) Quality of life questionnaire SF-36 – Polish version. Kardiol Pol 67:1166–1169
Valeyre D, Humbert M (2012) Everything you always wanted to know about sarcoidosis… but were afraid to ask. Presse Med 41(6 Pt 2):e273–e274. doi:10.1016/j.lpm.2012.04.010
Zieleźnik K, Jastrzębski D, Ziora D (2015) Fatique in patients with inactive sarcoidosis does not correlate with lung ventilation ability or walking distance. Pilot study. Pneumon Alergol Pol 83:15–22
Conflicts of Interest
The authors declare no conflicts of interest in relation to this article.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2017 Springer International Publishing AG
About this chapter
Cite this chapter
Pilzak, K. et al. (2017). Physical Functioning and Symptoms of Chronic Fatigue in Sarcoidosis Patients. In: Pokorski, M. (eds) Clinical Research Involving Pulmonary Disorders. Advances in Experimental Medicine and Biology(), vol 1040. Springer, Cham. https://doi.org/10.1007/5584_2017_85
Download citation
DOI: https://doi.org/10.1007/5584_2017_85
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-74091-1
Online ISBN: 978-3-319-74092-8
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)