Abstract
Increasing body of evidence indicates that neuron-neuroglia interaction may play a key role in determining the progression of neurodegenerative diseases including Parkinson’s disease (PD), a chronic pathological condition characterized by selective loss of dopaminergic (DA) neurons in the substantia nigra. We have previously reported that guanosine (GUO) antagonizes MPP+-induced cytotoxicity in neuroblastoma cells and exerts neuroprotective effects against 6-hydroxydopamine (6-OHDA) and beta-amyloid-induced apoptosis of SH-SY5Y cells. In the present study we demonstrate that GUO protected C6 glioma cells, taken as a model system for astrocytes, from 6-OHDA-induced neurotoxicity. We show that GUO, either alone or in combination with 6-OHDA activated the cell survival pathways ERK and PI3K/Akt. The involvement of these signaling systems in the mechanism of the nucleoside action was strengthened by a reduction of the protective effect when glial cells were pretreated with U0126 or LY294002, the specific inhibitors of MEK1/2 and PI3K, respectively. Since the protective effect on glial cell death of GUO was not affected by pretreatment with a cocktail of nucleoside transporter blockers, GUO transport and its intracellular accumulation were not at play in our in vitro model of PD. This fits well with our data which pointed to the presence of specific binding sites for GUO on rat brain membranes. On the whole, the results described in the present study, along with our recent evidence showing that GUO when administered to rats via intraperitoneal injection is able to reach the brain and with previous data indicating that it stimulates the release of neurotrophic factors, suggest that GUO, a natural compound, by acting at the glial level could be a promising agent to be tested against neurodegeneration.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
1 Introduction
Parkinson’s disease (PD) is a chronic and progressive neurodegenerative pathological condition characterized by selective loss of dopaminergic (DA) neurons in the substantia nigra (Dauer and Przedborski 2003; Birkmayer and Hornykiewicz 1961). Although different mechanisms have been considered influential for the PD pathogenesis, including inflammation, oxidative stress, excitotoxicity, protein misfolding, or apoptosis, none has been indicated as the primary cause of the disease, since all of them may likely act in a complex integrated pathway to promote neurodegeneration (Fujita et al. 2013; Barnum and Tansey 2010). Therapies for PD are mainly based on DA replacement by L-3,4-dihydroxyphenylalanine (L-DOPA), an approach which is effective in reducing motor handicap and alleviating the disease-associated depression and pain. However, chronic administration of L-DOPA often causes motor and psychiatric side effects which are reported to be as debilitating as PD itself (Andrew et al. 1993; Curtius et al. 1974).
In vitro treatment of cells with 6-hydroxydopamine (6-OHDA) and in vivo administration of this neurotoxin to laboratory animals represent one of the most used experimental models of PD. Moreover, 6-OHDA content is increased in the brain and urine of patients with PD treated with L-DOPA (Andrew et al. 1993; Curtius et al. 1974) and a role for this neurotoxin in the pathogenesis of the disease has been suggested.
We have recently reported that guanosine (GUO) protected SH-SY5Y neuroblastoma cells when exposed to neurotoxins, including MPP+ and 6-OHDA (Giuliani et al. 2012b; Pettifer et al. 2007). We have also reported that in a clinically relevant chronic animal model of PD, developed by using a proteasome inhibitor (McNaught et al. 2004), GUO treatment: (i) reduced apoptosis; (ii) increased tyrosine hydroxylase positive DA neurons; and (iii) ameliorated symptoms (Su et al. 2009). Increasing body of evidence indicates that neuron-neuroglia interaction may play a key role in determining the progression of neurodegenerative diseases, including PD (McGeer and McGeer 2008; Mena and Garcia de Yebenes 2008).
6-OHDA, beside its extracellular-mediated cytotoxic effects, damages catecholaminergic neurons following its uptake into the cells by DA transporters (Blum et al. 2000). Both monoamine oxidase (MAO) and catechol-O-methyl-transferase (COMT) are present in astroglial cells (Fitzgerald et al. 1990; Hansson and Sellstrom 1983; Pelton et al. 1981), suggesting that astrocyte uptake systems are likely to play an important role. It has been reported that not only catecholaminergic neurons but also astrocytes are able to take up DA by high-affinity Na+-dependent and Na+-independent systems (Pelton et al. 1981) and by EMT, which is an extraneuronal Na+-independent monoamine transporter system (Inazu et al. 1999a, b).
The role of astrocytes in DA neurons’ function is of interest as the glia/neurons ratio in the substantia nigra is the lowest in the brain (Damier et al. 1996; Makar et al. 1994; Sagara et al. 1993). This suggests that DA neurons could less rely on glial cells in case of different kinds of insults and that agents able to damage glial cells may contribute to the onset and progression of disease. Therefore, given the emerging role of astrocytes in the pathophysiology of PD and the need of evaluating novel therapeutic strategies for this disorder, in the present study we used C6 glioma cell cultures to investigate the neuroprotective effects of GUO in 6-OHDA-induced neurotoxicity.
2 Methods
The study was approved by the Ethics Committee of Chieti University in Italy.
2.1 Agents
6-OHDA, cells media, L-glutamine, poly-L-lysine, GUO, 6-[(4-nitrobenzyl)thio]-9-β-D-ribofuranosylpurine (NBTI), propentofylline (PPF), dipyridamole (DYP), 2-(4-morpholinyl)-8-phenyl-1(4H)-benzopyran-4-one hydrochloride (LY294002), and 1,4-diamino-2,3-dicyano-1,4-bis(o-aminophenylmercapto)butadiene monoethanolate (U0126) were purchased from Sigma Aldrich (Milano, Italy). Fetal bovine serum (FBS), penicillin/streptomycin (10,000 units/ml penicillin G sodium and 10,000 μg/ml streptomycin sulfate in 0.85 % saline), trypsin 10X liquid were obtained from Invitrogen (Milano, Italy). Antibody against phosphorylated-Akt (Ser473) and ERK1/2 were purchased from Cell Signaling Technology (CELBIO S.p.A, Milano, Italy). Anti-Actin (I-19) antibody was obtained from Santa Cruz Biotechnology (D.B.A. Italia S.r.l., Milano, Italy). Donkey anti-rabbit HPR-conjugated and chemiluminescence (ECL) detection kit was purchased from GE Healthcare (Milano, Italy).
2.2 C6 Glioma Cell Cultures
C6 glioma cells, were grown in DMEM containing 10 % FBS and 1 % penicillin/streptomycin in a humidified 5 % CO2 incubator at 37 °C. The culture medium was changed every other day and cells prepared at an appropriate density depending on the kind of experiment to be performed. In all the experiments, GUO was dissolved in NaOH 0.1 M and added to the culture medium at a final concentration of 0.001 M NaOH. Some cells were exposed to 0.001 M NaOH, but, as previously reported by Pettifer et al. (2007), no modification was observed.
2.3 Cell Viability Assay
Cell viability was evaluated by the MTS assay using the CellTiter 96 AQueous One Solution Cell Proliferation Assay kit (Promega, Milano, Italy). The assay is based on the cleavage of the yellow tetrazolium salt [3-(4,5-dimethylthiazol-2-yl)-5-(3-carboxymethoxyphenyl)-2-(4-sulfophenyl)-2H-tetrazolium] to purple formazan crystals by metabolically active cells. Cultured cells were starved by serum removal for 24 h and then treated with 6-OHDA at different concentrations (ranging from 5 to 200 μM) for 24 h. The EC50 value was used to treat the cells in combination with 300 μM GUO (co-treatment).
Inhibitors of the nucleoside transporters (10 μM NBTI plus 100 μM PPF plus 10 μM DYP) were added to the medium 1 h before the 6-OHDA/GUO co-treatment until the end of the experiment. After treatment, 20 μl of the One-Solution Reagent were added to each well and the plates were incubated at 37 °C for 2 h. The optical density at 490 nm was measured using a Packard SpectraCount™ microplate reader. The value of viability of treated cells was expressed as a percentage of that from the corresponding control cells.
2.4 Hoechst 33258 Staining
After treatment with 30 μM 6-OHDA in the presence or absence of 300 μM GUO for 24 h, the cells were harvested and fixed for 30 min with gentle agitation in pre-chilled phosphate buffered saline (PBS) containing 4 % paraformaldehyde. After fixation at room temperature, C6 glioma cells were washed with pre-chilled PBS and then exposed to Hoechst 33258 2 mg/l in PBS at room temperature for 5 min. After washing, all samples were analyzed with a fluorescence microscope (Leica DM RXA2).
2.5 DNA Fragmentation
Specific apoptotic DNA fragmentation was evaluated by measuring the amount of cytosolic oligonucleosomes using a Cell Death ELISA kit (Roche Molecular Biochemicals; Milano, Italy) and it was carried out according to the manufacturer’s instruction. After the exposure of the culture to 30 μM 6-OHDA alone or in combination with 300 μM GUO, cells were isolated for analysis of DNA fragmentation as described by Pettifer et al. (2007). Briefly, 10,000 viable cells/treatment were lysed and centrifuged to isolate fragmented oligonucleosomal DNA. The cytosolic fractions of cell lysates were transferred into streptavidin-coated microplate wells, and a mixture of biotin-linked anti-histone antibody and peroxidase-linked anti-DNA antibody was added and incubated for 2 h at room temperature. Plates were washed with the incubation buffer to remove the unfixed anti-DNA antibody and the peroxidase activity was determined spectrophotometrically with 2,2′-azino-bis[3-ethylbenzthiazoline-6-sulfonic acid] (ABTS) as substrate (absorbance of 405 nm). The amount of DNA fragmentation was expressed as a percentage of the positive control provided with the kit.
2.6 Western Blot Analysis
Western blot analysis was used to detect phosphorylated Akt (p-Akt) and ERK1/2 (p-ERK1/2). Cultured cells were rendered quiescent by serum removal for 24 h and treated with 30 μM 6-OHDA and 300 μM GUO alone or in combination. Inhibitors of nucleoside transporters (10 μM NBTI plus 100 μM PPF plus 10 μM DYP) were added to the medium 1 h before the 6-OHDA/GUO co-treatment until the end of experiment. At the end of the treatment, cells were washed twice with ice-cold PBS and then harvested at 4 °C in a lysis buffer (25 mM Tris buffer, pH 7.4, containing 150 mM NaCl, 100 μM sodium orthovanadate, 1.5 mM MgCl2, 1.0 mM EDTA, 1.0 mM EGTA, 1 % NP40, 10 % glycerol, 1 mM PMSF, 5 μg/ml leupeptin, 5 μg/ml aprotinin). After 20 min on ice, cells were centrifuged at 14,000 rpm for 10 min at 4 °C. Supernatant aliquots were used for the determination of protein concentrations by the method of Bradford (Bio-Rad; Milano-Italy).
Proteins were diluted in Laemli-SDS sample buffer and boiled for 5 min. Equal amounts of proteins were loaded onto each lane of SDS-PAGE gel (12 % resolving gel, 4 % stacking gel) and resolved at 120 V constant. Gels were transferred onto PVDF membrane (Bio-Rad, Milano-Italy) at 100 V constant for 90 min at room temperature, and membranes were blocked in blocking buffer (PBS, 0.1 % Tween-20 with 5 % w/v non-fat dry milk) for 2 h. Blots were incubated overnight at 4 °C with specific primary antibodies. All primary antibodies were diluted 1:1,000 in primary antibody dilution buffer (PBS, 0.1 % Tween-20 with 2,5 % w/v non-fat dry milk) except for β-actin that was diluted 1:1,500. After washing three times for 15 min with wash buffer (PBS, 0.1 % Tween-20), membranes were exposed to a secondary antibody diluted 1:2,500 for 1 h at room temperature. The immunocomplexes were visualized using an enhancing ECL detection system. Densitometric analysis was performed for the quantification of the immunoblots using the Quantity One 1-D Analysis software (Bio-Rad; Milano, Italy).
2.7 Statistical Analysis
Data were analyzed with a two-tailed t-test and expressed as means ± SE. All experiments were performed at least three times. P < 0.05 was considered statistically significant.
3 Results
3.1 Effect of 6-OHDA on C6 Glioma Cell Viability
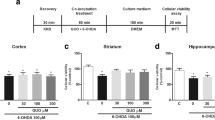
C6 glioma cells were treated with various concentrations of 6-OHDA (5–200 μM) for 24 h and cell viability was evaluated by conventional MTS reduction assay. As shown in Fig. 1, the proportion of viable cells was reduced by 6-OHDA in a concentration-dependent manner. The half maximal effective concentration (EC50) of approximately 30 μM 6-OHDA was used in the experiments aimed at studying the protective effects of GUO.
3.2 Protective Effect of Guanosine on 6-OHDA-Mediated Toxicity
C6 glioma cells were treated with 30 μM 6-OHDA for 24 h in the presence or absence of 300 μM GUO. The concentration of the guanine nucleoside was chosen on the basis of our previous results showing its neuroprotective effects in different cell types, including glial and neuroblastoma cells (Di Iorio et al. 2004; Pettifer et al. 2004). The addition of 30 μM 6-OHDA led to the expected reduction in C6 glioma cell viability (Fig. 2). GUO (300 μM) added along with the toxin (co-treatment) effectively attenuated (by about 60 %) the 6-OHDA-induced cytotoxicity as determined by MTS reduction assay (Fig. 2).
Effect of guanosine (GUO) on C6 glioma cell cytotoxicity induced by 6-hydroxydopamine (6-OHDA). The effect of 300 μM guanosine on the toxicity induced by 30 μM 6-OHDA for 24 h was evaluated in the presence or absence of nucleoside transporter blockers. The blocker cocktail [10 μM 6-[(4-nitrobenzyl)thio]-9-β-D-ribofuranosylpurine (NBTI), 100 μM propentofylline (PPF), and 10 μM dipyridamole (DYP)] was added to the culture medium 1 h before 6-OHDA/GUO co-treatment. The C6 cell viability was determined by MTS assay as described in Methods. Each column represents the mean ± SE of at least six independent experiments. ###P < 0.001 vs. untreated cells (control); *P < 0.05 vs. 6-OHDA-treated cells
To evaluate whether the protective effects of GUO were mediated by intracellular mechanisms following the nucleoside uptake, the cells were pretreated for 1 h with a cocktail of known nucleoside transporter blockers (10 μM NBTI, 100 μM PPF, and 10 μM DYP) (Parkinson et al. 2006). As shown in Fig. 2, the protective effect of GUO was not affected by cell pretreatment with these drugs.
3.3 6-OHDA -Induced Apoptotic Death in C6 Glioma Cells
To determine the capability of the chosen 6-OHDA concentration to cause apoptosis, DNA-sensitive dye Hoechst 33258 staining and DNA fragmentation assay by oligonucleosomal ELISA were used. The Hoechst 33258 staining was used to assess changes in nuclear morphology following cell treatment with 30 μM 6-OHDA for 24 h in the presence or absence of 300 μM GUO. As shown in Fig. 3A, nuclei in normal C6 glioma cells exhibited diffused Hoechst 33258 staining of chromatin. In contrast, about 27 % of nuclei in cells treated with 6-OHDA showed condensed chromatin (Fig. 3A, B). No protection was reported when 300 μM GUO was added to the cell medium along with the neurotoxin.
Effect of 6-hydroxydopamine (6-OHDA) alone or in combination with guanosine (GUO) on C6 glioma cell apoptosis. Cultured cells were exposed to 30 μM 6-OHDA for 24 h in the presence or absence of 300 μM GUO. Untreated (control) and treated cells were stained with the fluorescent nuclear dye Hoechst 33258 (Panel A) and the statistical analysis of apoptotic cells was reported (Panel B). The apoptosis was also evaluated measuring the oligonucleosome formation by ELISA assay (Panel C). Photomicrographs are representative results taken from ten different fields from randomly selected slides. Each column value represents the mean ± SE of six independent experiments. #p < 0.05 vs. untreated cells (control)
These results were confirmed by DNA fragmentation assay. 6-OHDA caused a 46 % increase in oligonucleosmal formation (Fig. 3C) and GUO (300 μM) added concomitantly with 6-OHDA was unable to reduce the toxin-mediated oligonucleosome formation (Fig. 3C).
3.4 ERK and PI3K/Akt Pathways Involvement in Neuroprotection by Guanosine Against 6-OHDA-Mediated Toxicity in C6 Glioma Cells
It has been reported that GUO induces a rapid increase in ERK1/2 and Akt phosphorylation in different cell types including PC12, microglia, and astrocytes (D’Alimonte et al. 2007; Di Iorio et al. 2004; Pettifer et al. 2004). To evaluate the involvement of the above mentioned cell survival pathways in GUO-mediated neuroprotection, we examined the effect of LY294002 (30 μM) an inhibitor of phosphoinositide-3-kinase (PI3K), an upstream of Akt, and U0126 (10 μM), an inhibitor of mitogen-activated protein kinase (MEK1/2), in glioma cell cultures co-treated with 30 μM 6-OHDA for 24 h. As shown in Fig. 4, both LY294002 and U0126 significantly reduced the effect of GUO on 6-OHDA-induced cytotoxicity as determined by MTS reduction assay. Consistent with the results obtained by MTS reduction assay, Western blotting analysis showed that 300 μM GUO was able to increase p-ERK1/2 and p-Akt – immunoreactivity in C6 glioma cells treated with the nucleoside for 15 min (Fig. 5A, C). As already reported for other cell types, including C6 glioma cells (Lee et al. 2011), also 6-OHDA increased p-ERK immunoreactivity (Fig. 5A).
Effects of PI3-kinase inhibitor (LY294002) and MEK1/2 inhibitor (U0126) on the protective effect of 300 μM guanosine (GUO) on 6-hydroxydopamine (6-OHDA)-induced toxicity. LY294002 (30 μM) or U0126 (10 μM) were added 1 h prior to the co-treatment with 300 μM GUO plus 30 μM 6-OHDA for 24 h. The C6 cell viability was determined by MTS assay as described in Methods. Each column represents the mean ± SE of at least six independent experiments. ###P < 0.001 vs. untreated cells (control); *P < 0.05 vs. 6-OHDA-treated cells; §P < 0.05 vs. the 6-OHDA/GUO co-treatment
Effect of 6-hydroxydopamine (6-OHDA), guanosine (GUO), or the combined treatment on the phosphorylation of ERK1/2 (Panels A & B) and Akt (Panel C) in C6 glioma cells. Cultured cells were incubated for 15 min with 30 μM 6-OHDA, 300 μM (GUO) or 6-OHDA/GUO co-treatment and harvested for western blot analysis. The protein expression of phosphorylated ERK1/2 (p-ERK1/2) or Akt (p-Akt), and β-actin were determined by using specific antibodies as described in Methods. To evaluate the time course of ERK1/2 activation induced by the co-treatment, cells were incubated for 5, 15, and 60 min with 30 μM 6-OHDA plus 300 μM GUO (Panel B). For each signaling pathway, a representative immunoblot is shown. Each column represents the mean ± SE of three independent experiments. #P < 0.05, ##P < 0.01, ###P < 0.001 vs. untreated cells (control); *P < 0.05 vs. 6-OHDA treated cells
It has been reported that sustained activation of ERK1/2 does not protect against either L-DOPA- or 6-OHDA-induced cytotoxicity (Jin et al. 2010). Thus, in an attempt to better define the characteristics of ERK activation mediated by co-treatment of C6 glioma cells with 30 μM 6-OHDA plus 300 μM GUO, analysis of the kinetics of ERK phosphorylation was performed. As shown in Fig. 5B, co-treatment significantly increased p-ERK1/2 level within 5 min, peaking at 15 min after administration, and strongly decreased it by 60 min.
Contrary to what was found for ERK1/2 phosphorylation, the neurotoxin was unable to enhance the levels of p-Akt in the same cells (Fig. 5C), whereas following the co-treatment with GUO and 6-OHDA, p-Akt levels increased by 39 % compared with the control values. The effect of cell co-treatment with 300 μM GUO and 30 μM 6-OHDA on p-ERK1/2 and p-Akt immunoreactivity was not affected by C6 glioma cell pretreatment with the cocktail of the nucleoside transporter blockers reported above (10 μM NBTI, 100 μM PPF, and 10 μM DYP) (Fig. 6A, B).
Effect of the nucleoside transporter blockers on the phosphorylation of ERK1/2 (Panel A) and Akt (Panel B) induced by the C6 cell co-treatment with 6-hydroxydopamine (6-OHDA)/guanosine (GUO). Cultured cells were incubated for 15 min with 30 μM 6-OHDA plus 300 μM GUO. When used, the blocker cocktail [10 μM 6-[(4-nitrobenzyl)thio]-9-β-D-ribofuranosylpurine (NBTI), 100 μM propentofylline (PPF), and 10 μM dypiridamole (DYP)] was added to the culture medium 1 h before 6-OHDA/GUO cotreatment. The protein expression of phosphorylated ERK1/2 (p-ERK1/2) or Akt (p-Akt) and β-actin were determined by using specific antibodies as described in Methods. For each signaling pathway, a representative immunoblot is shown. Each column represents the mean ± SE of three independent experiments. #P < 0.05, ###P < 0.001 vs. untreated cells (control)
4 Discussion
In the present study we demonstrate that 6-OHDA, a neurotoxin used to induce experimental models of PD, caused cytotoxicity in a concentration-dependent manner in C6 glioma cells, taken as a model system for astrocytes. We also report that 300 μM GUO concomitantly administered with 6-OHDA counteracted the toxin-induced loss of viability in this in vitro model of PD. It has been shown that GUO and its metabolic product guanine are taken up into both neurons and astrocytes mainly via the equilibrative nucleoside transporter (Parkinson et al. 2006). Thus, to determine whether GUO-mediated cytoprotection was due to intracellular effects following its uptake by the cells, a cocktail of uptake inhibitors was used. In agreement with previous findings observed in primary cultures of astrocytes (Di Iorio et al. 2004), the results show that the transport of GUO and its consequent intracellular accumulation was not required for protecting the cells in our in vitro model of PD. This fits well with our previous data which pointed to the presence of specific binding sites for GUO on rat brain membranes (Traversa et al. 2002, 2003).
The mechanisms underlying neurodegenerative processes in PD are still unclear. However, increasing evidence indicates that apoptosis is involved in the loss of dopaminergic neurons. We recently reported that GUO (300 μM) protected SH-SY5Y neuroblastoma cells when they were exposed to 6-OHDA, promoting their survival by (i) reducing the neurotoxin-mediated activation of p-38 and JNK; (ii) causing an early increase in phosphorylation of the anti-apoptotic kinase Akt; (iii) inactivating the pro-apoptotic factor GSK3β; and (iv) increasing the expression of the anti-apoptotic Bcl-2 protein (Giuliani et al. 2012b).
Apoptotic cells can be recognized by characteristic morphological changes, which are similar across cell types and species (Häcker 2000; Leist et al. 1997). The assessment of cell death by using Hoechst 33252 staining and oligonulceosomal formation is a combination of simple and reproducible methods to distinguish among viable and apoptotic cells. In the present work, we found that 6-OHDA induced apoptosis in C6 glioma cell but, unlike to what has been reported in neuroblastoma cells, GUO was unable to protect glial cultures against this kind of toxin-induced cell death.
We also reported that 6-OHDA induced a rapid phosphorylation of ERK1/2. Activation of the ERK pathway is known to contribute to neuronal cell survival in different models of neurotoxicity (Jin et al. 2002; Abe and Saito 2000; Han and Holtzman 2000), whereas sustained ERK phosphorylation has been shown to be involved in apoptosis processes and in a decrease of DA biosynthesis (Kulich and Chu 2001). Thus, our results are consistent with an attempt of glial cells to exert a defense response against the toxin. As our data indicate that GUO per se is able to cause a rapid and transient ERK phosphorylation, we hypothesize that the regulation of ERK phosphorylation might be involved in the mechanisms of GUO-induced cell survival.
Neuronal lesions caused by 6-OHDA are complex and the toxin can induce apoptosis and pre-necrotic lesions (Mayo et al. 1999). GUO could prevent the incipient signs of necrosis by enabling the cells to activate the recovery mechanisms. When the nucleoside was added to cultures along with 6-OHDA, a more intense early ERK phosphorylation, compared with that induced by the toxin alone, was observed. This ERK activation decreased toward the baseline level at 60 min. Inhibition of this pathway by U0126 significantly attenuated the protective effect of GUO as shown by the MTS reduction assay. This finding strengthens the notion that the ERK pathway might play a role in inducing survival of astrocytes by GUO.
Another finding of the present study was that 6-OHDA did not evoke phosphorylation of Akt, a key mediator downstream of PI3 kinase reported to be involved in several physiological cellular processes including metabolic cell responses and cell survival, GUO, on the other hand, increased p-Akt levels either when administered alone or in combination with the neurotoxin. When the PI3K/Akt pathway was blocked with the specific pharmacological inhibitor LY294002, we found a marked reduction of the protective action of GUO evaluated by MTS reduction assay, suggesting that also this protein kinase is involved in the mechanism necessary for the nucleoside to protect glia against 6-OHDA-induced cell death. Alterations in PI3k/Akt signaling have been associated with loss of DA neurons in PD (Timmons et al. 2009) and recently the ability of Myr-Akt to induce a robust, accurate, and functionally integrated axon regrowth in nigral DA neurons in a 6-OHDA animal model of PD has been demonstrated. These observations suggest that targeting the PI3K-Akt pathway may represent a pharmacological approach of a therapeutic interest in neurodegenerative disorders including PD.
The effects of GUO on both ERK and Akt phosphorylation, when administered in combination with 6-OHDA, were not affected by C6 glioma cell pretreatment with a cocktail of nucleoside uptake inhibitors, lending support for a notion that GUO acts through the activation of membrane receptor sites. A work is in progress in our laboratories to deorphanize a G-coupled orphan receptor which seems a good candidate as a novel purinergic receptor for guanine-based purines. We have also recently reported that GUO administered intraperitoneally to rats is able to pass the blood-brain barrier (Giuliani et al. 2012a) and stimulates the release of neurotrophic factors (Di Iorio et al. 2004). Taken together the present findings demonstrate that GUO might be of research interest as a novel therapeutic approach for treatment of PD.
References
Abe K, Saito H (2000) Neurotrophic effect of basic fibroblast growth factor is mediated by the p42/p44 mitogen-activated protein kinase cascade in cultured rat cortical neurons. Brain Res Dev Brain Res 122:81–85
Andrew R, Watson DG, Best SA, Midgley JM, Wenlong H, Petty RK (1993) The determination of hydroxydopamines and other trace amines in the urine of Parkinsonian patients and normal controls. Neurochem Res 18:1175–1177
Barnum CJ, Tansey MG (2010) Modeling neuroinflammatory pathogenesis of Parkinson’s disease. Prog Brain Res 184:113–132
Birkmayer W, Hornykiewicz O (1961) The L-3,4-dihydroxyphenylalanine (DOPA)-effect in Parkinson-akinesia. Wien Klin Wochenschr 73:787–788
Blum D, Torch S, Nissou MF, Benabid AL, Verna JM (2000) Extracellular toxicity of 6-hydroxydopamine on PC12 cells. Neurosci Lett 283:193–196
Curtius HC, Wolfensberger M, Steinmann B, Redweik U, Siegfried J (1974) Mass fragmentography of dopamine and 6-hydroxydopamine. Application to the determination of dopamine in human brain biopsies from the caudate nucleus. J Chromatogr 99:529–540
D’Alimonte I, Ciccarelli R, Di Iorio P, Nargi E, Buccella S, Giuliani P, Rathbone MP, Jiang S, Caciagli F, Ballerini P (2007) Activation of P2X(7) receptors stimulates the expression of P2Y(2) receptor mRNA in astrocytes cultured from rat brain. Int J Immunopathol Pharmacol 20:301–316
Damier P, Kastner A, Agid Y, Hirsch EC (1996) Does monoamine oxidase type B play a role in dopaminergic nerve cell death in Parkinson’s disease? Neurology 46:1262–1269
Dauer W, Przedborski S (2003) Parkinson’s disease: mechanisms and models. Neuron 39:889–909
Di Iorio P, Ballerini P, Traversa U, Nicoletti F, D’Alimonte I, Kleywegt S, Werstiuk ES, Rathbone MP, Caciagli F, Ciccarelli R (2004) The antiapoptotic effect of guanosine is mediated by the activation of the PI 3-kinase/AKT/PKB pathway in cultured rat astrocytes. Glia 46:356–368
Fitzgerald LW, Kaplinsky L, Kimelberg HK (1990) Serotonin metabolism by monoamine oxidase in rat primary astrocyte cultures. J Neurochem 55:2008–2014
Fujita KA, Ostaszewski M, Matsuoka Y, Ghosh S, Glaab E, Trefois C, Crespo I, Perumal TM, Jurkowski W, Antony PM, Diederich N, Buttini M, Kodama A, Satagopam VP, Eifes S, Del Sol A, Schneider R, Kitano H, Balling R (2013) Integrating pathways of Parkinson’s disease in a molecular interaction map. Mol Neurobiol 49:88–102
Giuliani P, Ballerini P, Ciccarelli R, Buccella S, Romano S, D’Alimonte I, Poli A, Beraudi A, Peña E, Jiang S, Rathbone MP, Caciagli F, Di Iorio P (2012a) Tissue distribution and metabolism of guanosine in rats following intraperitoneal injection. J Biol Regul Homeost Agents 26:51–65
Giuliani P, Romano S, Ballerini P, Ciccarelli R, Petragnani N, Cicchitti S, Zuccarini M, Jiang S, Rathbone MP, Caciagli F, Di Iorio P (2012b) Protective activity of guanosine in an in vitro model of Parkinson’s disease. Panminerva Med 54(1 Suppl 4):43–51
Häcker G (2000) The morphology of apoptosis. Cell Tissue Res 301:5–17
Han BH, Holtzman DM (2000) BDNF protects the neonatal brain from hypoxic-ischemic injury in vivo via the ERK pathway. J Neurosci 20:5775–5781
Hansson E, Sellstrom A (1983) MAO, COMT, and GABA-T activities in primary astroglial cultures. J Neurochem 40:220–225
Inazu M, Kubota N, Takeda H, Zhang J, Kiuchi Y, Oguchi K, Matsumiya T (1999a) Pharmacological characterization of dopamine transport in cultured rat astrocytes. Life Sci 64:2239–2245
Inazu M, Takeda H, Ikoshi H, Uchida Y, Kubota N, Kiuchi Y, Oguchi K, Matsumiya T (1999b) Regulation of dopamine uptake by basic fibroblast growth factor and epidermal growth factor in cultured rat astrocytes. Neurosci Res 34:235–244
Jin K, Mao XO, Zhu Y, Greenberg DA (2002) MEK and ERK protect hypoxic cortical neurons via phosphorylation of Bad. J Neurochem 80:119–125
Jin CM, Yang YJ, Huang HS, Kai M, Lee MK (2010) Mechanisms of L-DOPA-induced cytotoxicity in rat adrenal pheochromocytoma cells: implication of oxidative stress-related kinases and cyclic AMP. Neuroscience 170:390–398
Kulich SM, Chu CT (2001) Sustained extracellular signal‐regulated kinase activation by 6‐hydroxydopamine: implications for Parkinson’s disease. J Neurochem 77:1058–1066
Lee C, Park GH, Jang JH (2011) Cellular antioxidant adaptive survival response to 6-hydroxydopamine-induced nitrosative cell death in C6 glioma cells. Toxicology 283:118–128
Leist M, Single B, Castoldi AF, Kuhnle S, Nicotera P (1997) Intracellular adenosine triphosphate (ATP) concentration: a switch in the decision between apoptosis and necrosis. J Exp Med 185:1481–1486
Makar TK, Nedergaard M, Preuss A, Gelbard AS, Perumal AS, Cooper AJL (1994) Vitamin E, ascorbate, glutathione, glutathione disulfide, and enzymes of glutathione metabolism in cultures of chick astrocytes and neurons: evidence that astrocytes play an important role in antioxidative processes in the brain. J Neurochem 62:45–53
Mayo JC, Sainz RM, Antolín I, Rodriguez C (1999) Ultrastructural confirmation of neuronal protection by melatonin against the neurotoxin 6-hydroxydopamine cell damage. Brain Res 818:221–227
McGeer PL, McGeer EG (2008) Glial reactions in Parkinson’s disease. Mov Disord 23:474–483
McNaught KS, Perl DP, Brownell AL, Olanow CW (2004) Systemic exposure to proteasome inhibitors causes a progressive model of Parkinson’s disease. Ann Neurol 56:149–162
Mena MA, García de Yébenes J (2008) Glial cells as players in parkinsonism: the ‘good’, the ‘bad’, and the ‘mysterious’ glia. Neuroscientist 14:544–560
Parkinson FE, Ferguson J, Zamzow CR, Xiong W (2006) Gene expression for enzymes and transporters involved in regulating adenosine and inosine levels in rat forebrain neurons, astrocytes and C6 glioma cells. J Neurosci Res 84:801–808
Pelton EW, Kimelberg HK, Shipherd SV, Bourke RS (1981) Dopamine and norepinephrine uptake and metabolism by astroglial cells in culture. Life Sci 28:1655–1663
Pettifer KM, Kleywegt S, Bau CJ, Ramsbottom JD, Vertes E, Ciccarelli R, Caciagli F, Werstiuk ES, Rathbone MP (2004) Guanosine protects SH-SY5Y cells against beta-amyloid-induced apoptosis. Neuroreport 15:833–836
Pettifer KM, Jiang S, Bau C, Ballerini P, D’Alimonte I, Werstiuk ES, Rathbone MP (2007) MPP(+)-induced cytotoxicity in neuroblastoma cells: antagonism and reversal by guanosine. Purinergic Signal 3:399–409
Sagara JI, Miura K, Bannai S (1993) Maintenance of neuronal glutathione by glial cells. J Neurochem 61:1672–1676
Su C, Elfeki N, Ballerini P, D’Alimonte I, Bau C, Ciccarelli R, Caciagli F, Gabriele J, Jiang S (2009) Guanosine improves motor behavior, reduces apoptosis, and stimulates neurogenesis in rats with parkinsonism. J Neurosci Res 87:617–625
Timmons S, Coakley MF, Moloney AM, O’ Neill C (2009) Akt signal transduction dysfunction in Parkinson’s disease. Neurosci Lett 467:30–35
Traversa U, Bombi G, Di Iorio P, Ciccarelli R, Werstiuk ES, Rathbone MP (2002) Specific [(3)H]-guanosine binding sites in rat brain membranes. Br J Pharmacol 135:969–976
Traversa U, Bombi G, Camaioni E, Macchiarulo A, Costantino G, Palmier C, Caciagli F, Pellicciari R (2003) Rat brain guanosine binding site. Biological studies and pseudo-receptor construction. Bioorg Med Chem 11:5417–5425
Acknowledgments
PG and PB contributed to this work equally.
Conflicts of Interest
The authors declare no conflicts of interest in realtion to this article.
Author information
Authors and Affiliations
Corresponding authors
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2014 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Giuliani, P. et al. (2014). Guanosine Protects Glial Cells Against 6-Hydroxydopamine Toxicity. In: Pokorski, M. (eds) Neurotransmitter Interactions and Cognitive Function. Advances in Experimental Medicine and Biology(), vol 837. Springer, Cham. https://doi.org/10.1007/5584_2014_73
Download citation
DOI: https://doi.org/10.1007/5584_2014_73
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-10005-0
Online ISBN: 978-3-319-10006-7
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)