Abstract
The use of the tracheoesophageal (T-E) silicone rubber voice prosthesis is the most effective and well-established procedure to restore the voice in patients after laryngectomy. The prosthesis is usually well-tolerated with only minor complications. Severe complications are rare. In this article we present our experience with the prosthetic technique at the Clinic of Otorhinolaryngology and Head and Neck Surgery in University Hospital in Martin, Slovakia between the years 2005–2013 and report a case of a 48-year-old man with secondary prosthesis inserted through a T-E shunt 16 months after laryngectomy. On the 6th day after the insertion, the shunt decayed. After prosthesis removal the tissue defect was sutured. Due to repetitive tissue decay, reconstruction of the trachea and esophagus became necessary. On the 10th day, peritracheoesophageal fistula developed and gastrostomy was performed. Because of intense fibrotic and inflammatory changes, further reconstruction was not indicated. After 6 months, esophageal stenosis occurred and endoscopic dilation under local anaesthesia was performed. The T-E voice prosthesis has become one of the choices for voice rehabilitation following total laryngectomy and may improve the patient’s long-term quality of life. The overall risk of severe complications seems relatively low. Nonetheless, some complications might be challenging and might require specific management.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
1 Introduction
Total laryngectomy is the best approach in patients with transglottic tumours. Surgical removal of the larynx affects the major laryngeal functions such as phonation, airway control, swallowing, and coughing. However, removal of the larynx also results in the loss of laryngeal voice and necessitates a permanent tracheostoma for respiration. The loss of voice is considered a dominant problem after total laryngectomy and an effective voice restoration is critical for prevention of psychosocial consequences (Leonhard and Schneider-Stickler 2015).
Three voice restoration methods after total laryngectomy are currently available: electrolarynx, esophageal voice, and tracheoesophageal puncture. Alaryngeal communication through artificial larynges has a disadvantage of mechanical sound production and has control problems of the laryngeal device with one or both hands. Also, visual distractions to the listener, while the device is being used, may be considered as a disturbance for interactive communication (Wu et al. 2013). Oesophageal speech has an advantage of not necessitating finger closure, but a disadvantage of a long-lasting, complicated learning process. Compared with normal laryngeal speech, esophageal speech has the inherent limitations of slower rate, decreased intensity, lower pitch, stoma blast, and clunking on air intake (Rosso et al. 2012).
Tracheoesophageal puncture (TEP) with voice prosthesis placement is considered a gold standard in alaryngeal patients. Currently, it is the method of choice in Europe and the use of esophageal and electrolarynx voice is in decline (van der Molen et al. 2013). Singer and Blom (1980) have described for the first time one-way silicon voice prosthesis across the tracheoesophageal fistula, thus introducing the most used voice restoration technique. The prosthesis valve protects the airways during deglutition and allows a unidirectional airflow from the trachea across the tracheoesophageal mucosa to produce voice with the vibration of neoglottis. Several voice prostheses have been developed for TEP performed the time of laryngectomy or as a secondary procedure at a later stage (Boscolo-Rizzo et al. 2008; van Weissenbruch and Albers 1993). The prosthesis is usually well-tolerated with only minor complications, e.g. leakage, fungal colonisation, granulation tissue formation, cervical cellulitis, necrosis of the TEP, tracheostomal stenosis, and swallowing impairment. Severe complications are very rare (Laccourreye et al. 1997).
The aim of this article was to present our experience with the prosthetic technique at the Clinic of Otorhinolaryngology and Head and Neck Surgery in University Hospital in Martin, Slovakia between the years 2005–2013 and to report a case of a 48-year-old man with rare complications encountered with secondary prosthesis inserted through T-E shunt 16 months after laryngectomy.
2 Case Report
Between the years 2005–2013, 216 patients with laryngeal cancer were admitted to the Clinic of Otorhinolaryngology and Head and Neck Surgery at the University Hospital in Martin, Slovakia. Of those, 96 underwent total laryngectomy and in 31 patients tracheoesophageal prosthesis was inserted. The study group consists of 28 males and 3 females, with average age of 49 years. The most common complication after puncture was a short-term localized inflammation of varying degrees, requiring treatment with intravenous antibiotics and parenteral nutrition for about 4–5 days (n = 25). Among the long-term mild complications, granulation around voice prosthesis due to soft tissue irritation was present in 13 patients.
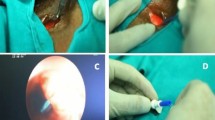
In the study group, one patient experienced a severe complication. A 48-year-old man with carcinoma on the left hemilarynx, classified as T3 N0 M0 III stage G2 was first admitted to the Clinic in November of 2010. He underwent suprahyoid laryngectomy with revision of the cervical lymphatic system followed by radiation therapy in December of 2010. In February of 2012, 16 months later, the secondary tracheoesophageal prosthesis Provox No. 6 was inserted. Because of prosthesis dislocation on the 1st post-operative day, it was replaced by Provox No. 8. In March of 2012, the prosthesis had to be extracted because of saliva and food leakage through treacheoesophageal shunt (Fig. 1). The shunt was closed to 60 % of its original size. Two weeks later, surgical revision followed, with mobilization of the trachea and suture of the defect at the hypopharyngoesophageal junction (Fig. 2). Subsequently, a new defect of ~10 mm in diameter occurred at the upper pole of tracheostomy. Currently, a tracheohypopharyngeal fistula of 2 mm in diameter persists at the upper pole of treacheostomy (Fig. 3).
In April of 2012, the patient underwent the Witzel gastrostomy. The swallowing difficulties developed 6 months later. The esophageal X-ray contrast passage revealed a stenosis at the hypopharyngeal junction. In November of 2012, flexible gastroscopy confirmed the presence of stenosis without mucosal fold in the upper third of the esophagus. Direct repeat esophagoscopy uncovered circular stenosis with ∅ 2 mm approximately 4 cm above the tracheostomy. The stenosis was gradually dilated up to the probe No. 32. Because of inflammation and edema at the site of stenosis, dilation was discontinued and parenteral anti-inflammatory and anti-edematous treatment was initiated. The patient complained of dyspepsia caused by delay in gastric emptying. He lost 23 kg of body weight between April and November of 2012. The patient’s condition improved after introduction of gastric prokinetics. He was finally released in stable condition for outpatient care. Further re-dilation of the stenosis was performed in December of 2012 up to the probe No. 34, after which the swallowing of solid food significantly improved. However, a leak of liquids persisted. A rarely diagnosed material intolerance was suggested as a source of the patient’s problems.
3 Discussion
The prosthetic voice rehabilitation developed after a failure of laryngectomized patients to use esophageal voice or electrolarynx (Singer and Blom 1980). The basic condition of successful voice restoration in these patients is an adequate opening pressure in the pharyngoesophageal segment. It seems that anatomical conditions are more important than the patient’s mental need to talk (Sebova-Sedenkova 2010).
The insertion of a tracheoesophageal prosthesis may be followed by different adverse effects. A minor consequence is tissue granulation around the puncture site (Imre et al. 2013). Treatment includes antibiotics, antifungals, chemical or electrocautery, and surgical excision of the granulation tissue. Another common complication is biofilms formation. Voice prostheses are usually made of silicon rubber. A continuous exposure to saliva, food, drinks, and oropharyngeal microflora contributes to the rapid colonization of the prosthesis by biofilms consisting of mixed bacteria and yeast strains leading to failure and frequent replacement (Talpaert et al. 2014). Microbial colonization and biofilm formation can lead to salivary leakage through voice prosthesis and deterioration of the prosthesis due to the blocking of a valve mechanism. Valve failure as well as compromised speech may result in aspiration pneumonia, and repeat valve replacement may lead to the tract stenosis or insufficiency. Prevention and control of biofilm formation will therefore be beneficial not only for the life span of the prosthesis, but also for the general patient’s health. A number of different approaches have been suggested to inhibit or minimize biofilm formation (for review see Talpaert et al. 2014).
A circumferential enlargement of the tracheoesophageal puncture is a challenging complication as it results in a leakage around the voice prosthesis into the airway and may eventually lead to aspiration pneumonia and respiratory complications (Mobashir et al. 2014). Several treatment alternatives have been proposed to manage the enlarged tracheoesophageal puncture, with varying success. Surgical options include a submucosal purse-string suture around the enlarged tracheoesophageal puncture and its complete closure. Conservative methods, such as customization of the tracheoesophageal voice prosthesis (Lewin et al. 2012), temporary removal of the voice prosthesis (VP) to facilitate stenosis of the tracheoesophageal tract and tracheoesophageal puncture site injections have often been preferred over surgery (Shuaib et al. 2012).
Imre et al. (2013) have retrospectively analyzed 47 patients with secondary tracheoesophageal prosthesis. Tracheoesophageal puncture and speech valve related complications were observed in 20 patients. Minor complications included granulation tissue formation (2 patients), deglutition of prosthesis (6 patients) and tracheoesophageal puncture enlargement/leakage around the prosthesis (9 patients). Major complications were observed in three patients. Two patients developed life-threatening complications: a mediastinitis and paraesophageal abscess, both in the first month of the postoperative period. The overall complication rate was 42.6 % during a mean follow-up of 15.3 months. Tracheoesophageal fistula enlargement was the most common minor complication and the most common cause of complete closure of tracheoesophageal puncture in that study.
Another retrospective study analyzed 103 patients who underwent total laryngectomy or pharyngolaryngectomy (Bozec et al. 2010). Functional outcomes were recorded 6 months postoperatively. A total of 87 patients (84 %) underwent tracheoesophageal puncture and speech valve placement (79 primary and 8 secondary punctures). A high level of comorbidity was correlated to speech rehabilitation failure. Minor leakage around the valve occurred in 26 % of patients. Late complications occurred in 14 patients, including severe enlargement of the fistula (3 patients), prosthesis displacement (7 patients), and granulation tissue-formation (4 patients).
In the present study, out of the 31 patients with voice restoration by secondary tracheoesophageal puncture, 25 (80.6 %) developed inflammation and 13 (41.9 %) developed granulation, which are considered mild complications. No mediastinitis, bleeding, or prosthesis deglutition were recorded.
Despite short-term complications, the prostheses are considered to be well-tolerated in the long-term view. In a cohort of 100 patients (Lukinović et al. 2012), rehabilitation was successful in 75.8 % of patients. The early complication rate was 4.4 %, and 10.9 % of patients had late complications. Statistical analysis failed to substantiate any differences regarding the complication rate and success rate of rehabilitation between the groups of patients stratified according to age, irradiation status, or timing of prosthesis insertion.
Severe complications, such as bleeding, abscess, or prosthesis aspiration have rarely been reported (Bozzo et al. 2014; Birk et al. 2009; Denholm and Fielder 1994; Spiro and Spiro 1990; Ruth et al. 1985). In the present study, in a group of 31 patients with tracheoesophageal prosthesis, we observed one severe complication with the secondary prosthesis inserted through a T-E shunt 16 months after laryngectomy. The patient developed shunt decay on the 6th day after the insertion. After prosthesis removal, the tissue defect was sutured and gastrostomy was performed. Due to persisting tissue decay on the 7th postoperative day, reconstruction of the trachea and esophagus was necessary. On the 10th day, peritracheoesophageal fistula developed. Because of intense fibrotic and inflammatory changes, reconstruction was not indicated. After 6 months, esophageal stenosis was revealed and endoscopic dilation in local anesthesia had to be performed. Material intolerance was suggested as a source of the patient’s problems, which is a kind of complication not yet reported in the literature on the subject.
4 Conclusions
The tracheoesophageal voice prosthesis has become one of the choices for voice rehabilitation following total laryngectomy and may improve the patient’s long-term quality of life. Even the overall risk of severe complications seems relatively low, some of them might be challenging and require specific management.
References
Birk S, Michaeli P, Kapsreiter M, Alexiou C (2009) [Dislocation of voice prostheses. Interdisciplinary management of diagnostics and treatment][Article in German]. HNO 57(11):1126–1130
Boscolo-Rizzo P, Zanetti F, Carpene S, Da Mosto MC (2008) Long-term results with tracheoesophageal voice prosthesis: primary versus secondary TEP. Eur Arch Otorhinolaryngol 265:73–77
Bozec A, Poissonnet G, Chamorey E, Demard F, Santini J, Peyrade F, Ortholan C, Benezery K, Thariat J, Sudaka A, Anselme K, Adrey B, Giacchero P, Dassonville O (2010) Results of vocal rehabilitation using tracheoesophageal voice prosthesis after total laryngectomy and their predictive factors. Eur Arch Otorhinolaryngol 267(5):751–758
Bozzo C, Meloni F, Trignano M, Profili S (2014) Mediastinal abscess and esophageal stricture following voice prosthesis insertion. Auris Nasus Larynx 41(2):229–233
Denholm SW, Fielder CP (1994) Submental abscess: an unusual delayed complication of primary Blom-Singer valve insertion. J Laryngol Otol 108(12):1093–1094
Imre A, Pınar E, Callı C, Sakarya EU, Oztürkcan S, Oncel S, Katılmış H (2013) Complications of tracheoesophageal puncture and speech valves: retrospective analysis of 47 patients. Kulak Burun Bogaz Ihtisas Dergisi 23(1):15–20
Laccourreye O, Ménard M, Crevier-Buchman L, Couloigner V, Brasnu D (1997) In situ lifetime, causes for replacement, and complications of the Provox voice prosthesis. Laryngoscope 107(4):527–530
Leonhard M, Schneider-Stickler B (2015) Voice prostheses, microbial colonization and biofilm formation. Adv Exp Med Biol 830:123–136
Lewin JS, Hutcheson KA, Barringer DA, Croegaert LE, Lisec A, Chambers MS (2012) Customization of the voice prosthesis to prevent leakage from the enlarged tracheoesophageal puncture: results of a prospective trial. Laryngoscope 122(8):1767–1772
Lukinović J, Bilić M, Raguz I, Zivković T, Kovac-Bilić L, Prgomet D (2012) Overview of 100 patients with voice prosthesis after total laryngectomy-experience of single institution. Coll Antropol 36(Suppl 2):99–102
Mobashir MK, Basha WM, Mohamed AE, Anany AM (2014) Management of persistent tracheoesophageal puncture. Eur Arch Otorhinolaryngol 271(2):379–383
Rosso M, Sirić L, Tićac R, Starcević R, Segec I, Kraljik N (2012) Perceptual evaluation of alaryngeal speech. Coll Antropol 36(Suppl 2):115–118
Ruth H, Davis WE, Renner G (1985) Deep neck abscess after tracheoesophageal puncture and insertion of a voice button prosthesis. Otolaryngol Head Neck Surg 93(6):809–811
Sebova-Sedenkova I (2010) Primary prosthetic voice rehabilitation in patients after laryngectomy – part II. Otorhinolaryngol Head Neck Surg 4(1):15–18
Shuaib SW, Hutcheson KA, Knott JK, Lewin JS, Kupferman ME (2012) Minimally invasive approach for the management of the leaking tracheoesophageal puncture. Laryngoscope 122(3):590–594
Singer MI, Blom ED (1980) An endoscopic technique for restoration of voice after laryngectomy. Ann Otol Rhinol Laryngol 89(6 Pt 1):529–533
Spiro JD, Spiro RH (1990) Retropharyngeal abscess and carotid hemorrhage following tracheoesophageal puncture and voice prosthesis insertion: a case report. Otolaryngol Head Neck Surg 102(6):762–763
Talpaert MJ, Balfour A, Stevens S, Baker M, Muhlschlegel FA, Gourlay CW (2014) Candida biofilm formation on voice prostheses. J Med Microbiol. doi:10.1099/jmm.0.078717-0. [Epub ahead of print]
van der Molen L, Kornman AF, Latenstein MN, van den Brekel MW, Hilgers FJ (2013) Practice of laryngectomy rehabilitation interventions: a perspective from Europe/the Netherlands. Curr Opin Otolaryngol Head Neck Surg 21(3):230–238
van Weissenbruch R, Albers FWJ (1993) Vocal rehabilitation after total laryngectomy using the Provox voice prosthesis. Clin Otolaryngol Allied Sci 18:359–364
Wu L, Wan C, Wang S, Wan M (2013) Improvement of electrolaryngeal speech quality using a supraglottal voice source with compensation of vocal tract characteristics. IEEE Trans Biomed Eng 60(7):1965–1974
Acknowledgements
The study was supported by VEGA No. 1/0416/12 and Project Virtual and Simulation Tuition as a New Form of Education at JFM CU in Martin (ITMS 26110230071).
Conflicts of Interest
The authors declare no conflicts of interest in relation to this article.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2014 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Calkovsky, V., Hajtman, A. (2014). Primary Prosthetic Voice Rehabilitation in Patients After Laryngectomy: Applications and Pitfalls. In: Pokorski, M. (eds) Respiratory Carcinogenesis. Advances in Experimental Medicine and Biology(), vol 852. Springer, Cham. https://doi.org/10.1007/5584_2014_104
Download citation
DOI: https://doi.org/10.1007/5584_2014_104
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-16921-7
Online ISBN: 978-3-319-16922-4
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)