Abstract
Prostaglandins (PGs) are highly bioactive fatty acids. PGs, especially prostaglandin E2 (PGE2), are abundantly produced by cells of both the bone-forming (osteoblast) lineage and the bone-resorbing (osteoclast) lineage. The inducible cyclooxygenase, COX-2, is largely responsible for most PGE2 production in bone, and once released, PGE2 is rapidly degraded in vivo. COX-2 is induced by multiple agonists – hormones, growth factors, and proinflammatory factors – and the resulting PGE2 may mediate, amplify, or, as we have recently shown for parathyroid hormone (PTH), inhibit responses to these agonists. In vitro, PGE2 can directly stimulate osteoblast differentiation and, indirectly via stimulation of RANKL in osteoblastic cells, stimulate the differentiation of osteoclasts. The net balance of these two effects of PGE2 in vivo on bone formation and bone resorption has been hard to predict and, as expected for such a widespread local factor, hard to study. Some of the complexity of PGE2 actions on bone can be explained by the fact that there are four receptors for PGE2 (EP1–4). Some of the major actions of PGE2 in vitro occur via EP2 and EP4, both of which can stimulate cAMP signaling, but there are other distinct signaling pathways, important in other tissues, which have not yet been fully elucidated in bone cells. Giving PGE2 or agonists of EP2 and EP4 to accelerate bone repair has been examined with positive results. Further studies to clarify the pathways of PGE2 action in bone may allow us to identify new and more effective ways to deliver the therapeutic benefits of PGE2 in skeletal disorders.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
1 Introduction
Prostaglandins (PGs) are highly bioactive unsaturated fatty acids. PGs are not stored but are synthesized and released, as needed, and rapidly metabolized. This chapter will focus on prostaglandin E2 (PGE2), which is abundantly produced by cells of both the bone-forming and bone-resorbing lineages. Production of PGs depends on the availability of substrate; one of two cyclooxygenases (COXs), constitutively expressed COX-1 or inducible COX-2; and a specific downstream synthase. Most PGE2 in bone is produced by COX-2. COX-2 is induced by multiple hormones and proinflammatory factors, and the resulting PGE2 can mediate or modify responses to the agonist, sometimes in very unexpected ways, as we discuss for the COX-2 agonist, parathyroid hormone (PTH). PGE2 can act on four G-protein-coupled receptors whose signaling pathways have not been fully elucidated in bone cells. It has been 50 years since PGE2 in bone was first shown to stimulate cyclic AMP (cAMP) production and resorption in bone organ cultures (Klein and Raisz 1970). The early studies in cell and organ cultures led to the conclusion that PGE2 could increase both bone formation and resorption, and this has led to continuing interest in the potential for therapeutic manipulation of PGE2 or its receptors.
2 PGE2 Production
Eicosanoids are bioactive lipids derived from arachidonic acid (AA) and other 20-carbon polyunsaturated fatty acids (PUFAs) (Buczynski et al. 2009; Smith et al. 2011). The term “prostanoid” refers to products of the COX pathway: PGE2, prostaglandin D2 (PGD2), prostaglandin F2a (PGF2a), prostacyclin (PGI2), and thromboxane (TXA2). PGs are 20-carbon fatty acids with a cyclopentane ring. Although TXAs have an oxane ring, they are generally discussed under the “PG” heading. The subscript for prostanoids denotes the number of double bonds (e.g., PGE1, PGE2, and PGE3). The two series of prostanoids are the most abundant and the best characterized.
There are three steps in the production of PGs (Fig. 1). The first is the mobilization of AA from membranes by phospholipases. The second step is catalyzed by a bifunctional enzyme that converts free AA to prostaglandin G2 (PGG2), first by a cyclooxygenase (hence, the name COX) reaction and then a peroxidase reaction, to prostaglandin H2 (PGH2). PGH2 is then converted by terminal synthases to the various prostanoids.
Major prostanoids generated from arachidonic acid. Free arachidonic acid, released from membrane phospholipids by phospholipases, is converted by a bifunctional enzyme, called cyclooxygenase, to prostaglandin G2 (PGG2) in a cyclooxygenase reaction followed by reduction of PGG2 to prostaglandin H2 (PGH2) in a peroxidase reaction. PGH2 is then converted to specific prostanoids by the terminal synthases
AA Release
Phospholipase A2 (PLA2) enzymes catalyze the hydrolysis of membrane phospholipids, from membrane glycerophospholipids, releasing free fatty acids, such as AA. The PLA2 superfamily has 16 groups and many subgroups (Dennis et al. 2011; Murakami et al. 2011, 2015; Vasquez et al. 2017). The most important PLAs for PG production are probably the Ca2+-independent PLA2s (iPLA2), the Ca2+-dependent cytosolic PLA2s (cPLA2), and the secreted PLA2s (sPLA2). As a general summary, iPLA2 is the primary PLA2 in cells, producing low levels of free fatty acids, some of which may be AA, needed for daily cellular functions; cPLA2 is the major inducible enzyme hydrolyzing AA-containing phospholipids during infection or inflammation; sPLA2 is also inducible and augments cPLA2 function (Dennis and Norris 2015).
COX Enzymes
The bifunctional enzyme is formally named prostaglandin endoperoxide H synthase or prostaglandin G/H synthase (PGHS), and the gene name is ptgs. However, because the COX reaction site is inhibited by nonsteroidal anti-inflammatory drugs (NSAIDs), the interest in developing new inhibitors selective for COX-2 led to calling PGHS simply COX and the inhibitors coxibs. The two enzymes for COX, COX-1 and COX-2, are encoded by separate genes (Herschman 1994; Smith et al. 2000). Both COX-1 and COX-2 are N-glycosylated dimeric proteins inserted into the luminal face of the ER and the contiguous inner membrane of the nuclear envelope (Smith et al. 2011).
Despite having similar catalytic mechanisms, COX-1 and COX-2 are independently functioning pathways (Simmons et al. 2004; Smith and Langenbach 2001). COX-2 is rapidly and transiently inducible by multiple factors in many tissues (Kang et al. 2007). COX-1 is expressed at relatively low, stable levels in most tissues and is considered to be “constitutive.” The half-life of COX-2 protein is reported to be 2–7 h in various tissues, while the half-life of COX-1 protein is much longer (Kang et al. 2007; Mbonye et al. 2006). However, it is now evident that COX-2 mRNA is also expressed constitutively at low levels in many tissues and cells. A recent study examined signaling pathways underlying constitutive expression of COX-2 in the kidney, gastrointestinal tract, and brain (Kirkby et al. 2016). It is still unclear how much this expression contributes to PG production. Another difference is that COX-2 is much more efficient at using low AA concentrations (below 5 μM) than COX-1 (Swinney et al. 1997). This difference may explain why osteoblasts from COX-2 KO mice make little or no measurable PGE2 in culture despite the constitutive expression of COX-1 (Chikazu et al. 2005; Choudhary et al. 2003; Okada et al. 2000a; Xu et al. 2007).
It was initially hypothesized that COX-2 was responsible for acute pathological PG responses, while COX-1 produced prostanoids for ongoing “housekeeping” functions, such as maintenance of renal blood flow, platelet aggregation, and gastric cytoprotection. Once highly selective inhibitors of COX-2 activity were available, it became apparent that COX-2 also has physiologic functions and COX-2 selective NSAIDs turned out to have serious adverse side effects, especially on the cardiovascular system, that would limit their use (Grosser et al. 2017a, b).
PG Synthases
PGH2 is converted to each PG by specific PG terminal synthases (Fig. 1), and the synthases may determine the major PG synthesized in a tissue. Prostaglandin E synthase (PGES), which converts PGH2 to PGE2, occurs in multiple forms (Hara et al. 2010; Hara 2017). The predominant PGES, mPGES-1, is inducible, located in ER and perinuclear membranes, and regulated similarly to COX-2. mPGES-1 may also be located in the Golgi apparatus, and because COX-2 and cPLA2 may also be located there, the Golgi apparatus may be a dedicated PGE2 synthesis site (Leslie 2015; Yuan and Smith 2015). mPGES-2 is constitutively expressed and functionally coupled with both COX-1 and COX-2. A third form, cytosolic PGES (cPGES), is preferentially coupled to COX-1 and thought to maintain PGE2 production for cellular homeostasis (Tanioka et al. 2000). Knockout (KO) mice for the synthases are reviewed in Hara et al. (2010) and Hara (2017). Mice deficient for mPGES-1 have reduced inflammatory and pain responses, and potential inhibitory drugs have been developed (Psarra et al. 2017). Mice deficient for mPGES-2 have no specific phenotype, and deficiency of cPGES in mice is perinatal lethal.
PGE2 Degradation
Degradation of circulating PGE2 occurs rapidly (Ferreira and Vane 1967), and measurement of PGE2 metabolites in the urine may be the preferred way to track changes in PGE2 production in vivo. The first step in degrading PGE2 is mediated by the enzyme 15-hydroxyprostaglandin dehydrogenase (HPGD, also known as 15-PGDH), which generates metabolites that are orders of magnitude less potent than PGE2 itself. Many tissues make HPGD, but it is not clear how quickly bone cells degrade PGE2. It is common practice to follow PGE2 production in vitro by measuring PGE2 accumulation in osteoblastic or marrow stromal cell cultures over 2–3 days between medium changes, suggesting shared knowledge of some stability in culture.
In humans, mutations in HPGD are associated with a rare genetic disorder called idiopathic hypertrophic osteoarthropathy, characterized by chronically elevated PGE2, coarse or thickened skin, and periostosis in bone (Uppal et al. 2008). In mice, inhibition of HPGD increases PGE2 and potentiates recovery in marrow transplant models and accelerates tissue generation in models of colon and liver injury (Antczak et al. 2017; Desai et al. 2018; Zhang et al. 2015b). Although the known associations of elevated PGE2 with increased inflammation and tumorigenesis might be thought to limit the usefulness of inhibiting HPGD, initial studies in animal models suggest that a small molecule inhibitor can promote transplant recovery without limiting side effects (Desai et al. 2018).
3 PGE2 Receptors
There are four G-protein-coupled receptors (GPCRs), called EP1, EP2, EP3, and EP4, mediating actions of PGE2 (Fig. 1) (Woodward et al. 2011). The EP1 receptor is known to increase Ca2+ and may couple to Gαq because studies have reported involvement of the PLC/PKC pathway (Tang et al. 2005). The major signaling pathway for EP3 receptors is Gαi-induced adenylate cyclase inhibition. EP2 and EP4 are the receptors most extensively studied in bone. Mice deficient in each EP receptor subtype have been generated, and highly selective agonists for the receptors have been developed (Sugimoto and Narumiya 2007; Woodward et al. 2011).
The first major pathway for PGE2 signaling identified in bone was cAMP (Klein and Raisz 1970). Both EP2 and EP4 can stimulate Gαs to activate adenylyl cyclases (ACs) and produce cAMP, which can then activate protein kinase A (PKA) or a PKA-independent pathway mediated by EPAC (exchange protein directly activated by cAMP). The PKA pathway is able to crosstalk with other pathways that regulate cell growth, motility, migration, and apoptosis, including the Wnt/β-catenin signaling pathway (Buchanan and DuBois 2006; Castellone et al. 2006; Estus et al. 2016; Hino et al. 2005; Shao et al. 2005). EP2 and EP4 may also transactivate the epidermal growth factor receptor (EGFR) signaling pathway, leading to multiple signaling pathways, including PI3K/Akt/β-catenin. The recruitment of β-arrestin by EP receptors may also activate c-Src, resulting in EGFR transactivation (O’Callaghan and Houston 2015). There was much interest in studying EP receptors in bone in the early days because of the possibility of developing drugs that could target a specific receptor to increase bone mass and fracture healing without the side effect of inhibiting COX. In more recent years, most of the data on EP signaling has come from studies on other tissues.
4 Bone Remodeling and PGE2
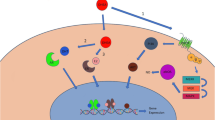
Bone remodeling, the cycle of bone resorption followed by bone formation, occurs throughout our adult life. The net bone balance of these cycles determines whether bone is lost, gained, or maintained. Agents used to prevent or treat osteoporosis, that is, skeletal fragility associated with a high risk of fracture, are aimed at manipulating this cycle. Exogenously applied PGE2 has been shown to stimulate both resorption and formation in bone, but the role of endogenous PGE2 in remodeling is still being defined (Blackwell et al. 2010). The potential involvement of endogenous PGE2 is shown in Fig. 2.
Potential roles of PGE2 in bone resorption and formation. (a) Agonists of resorption, including PGE2, act on osteoblastic cells to induce RANKL, which then binds with its receptor, RANK, on bone marrow macrophages (BMMs) and drives them to differentiate into osteoclasts. These agonists are often also inducers of COX-2 expression in osteoblastic cells, as well. The PGE2 can act back on osteoblasts to induce more RANKL. (RANKL can also induce COX-2 in BMMs.) (b) Some stimulators of osteoblastic differentiation also induce COX-2 and produce PGE2. PGE2 can then act on the osteoblastic precursors to stimulate osteoblastic differentiation. In some cases, such as serum and strontium ranelate (see text), the major stimulatory effect in cell culture is due to PGE2
Bone Resorption
Early work adding PGs in organ culture showed that exogenous PGs of the E series were potent activators of resorption (Klein and Raisz 1970). Studies with inhibitors of PG production showed that the resorptive effects of many agonists were mediated in part by PGs (Pilbeam et al. 2008). In the early 1990s, the inducible COX-2 was identified (O’Banion et al. 1991; Kujubu et al. 1991; Xie et al. 1991). Subsequently, many resorption agonists were shown to induce COX-2 expression and PGE2 production in osteoblastic cells that contributed to increasing osteoclasts, including interleukin-1 (IL-1) (Kawaguchi et al. 1994; Sato et al. 1996; Lader and Flanagan 1998; Min et al. 1998), IL-6 (Tai et al. 1997), tumor necrosis factor-α (TNF-α) (Lader and Flanagan 1998), parathyroid hormone (PTH) (Kawaguchi et al. 1994; Inoue et al. 1995; Okada et al. 2000a), and 1,25(OH)2D3 (Okada et al. 2000a). PGE2 can amplify its own production by inducing COX-2 (Pilbeam et al. 1994). PGE2 has receptors on both osteoblastic and osteoclastic lineage cells, but stimulates osteoclast differentiation largely indirectly via upregulation of expression of receptor activator of NFκB ligand (RANKL) and inhibition of expression of the decoy RANKL receptor, osteoprotegerin (OPG), in osteoblastic lineage cells (Li et al. 2000) (Fig. 2a). Although both EP2 and EP4 may be involved in PGE2-stimulated resorption, a number of in vitro studies have suggested that EP4 is the more important receptor for resorption (Miyaura et al. 2000; Suzawa et al. 2000; Raisz and Woodiel 2003; Zhan et al. 2005).
Bone Formation
Many studies have shown that PGE2 stimulates osteoblastic differentiation in murine or rat bone marrow stromal cell and primary osteoblast/calvarial cell cultures (Choudhary et al. 2013; Flanagan and Chambers 1992). In cultured marrow stromal cells or primary osteoblasts from mice with deletion of ptgs2 or treated with NSAIDs to inhibit COX-2 activity, osteoblastic differentiation is decreased (Choudhary et al. 2013, Okada et al. 2000b, Xu et al. 2007, Zhang et al. 2002). Systemic injections of PGE2 can increase both periosteal and endosteal bone formation in the rat and produce substantial increases in bone mass (Jee and Ma 1997; Lin et al. 1994; Suponitzky and Weinreb 1998). Systemic administration of PGE2 in humans (Faye-Petersen et al. 1996; Ueda et al. 1980) and dogs (Norrdin and Shih 1988) has also been shown to increase cortical and cancellous bone mass. Local infusion of PGE2 has been shown to increase bone in mice (Yoshida et al. 2002).
Similar to resorption agonists, many osteogenic factors induce COX-2 (Fig. 2b), including transforming growth factor β (TGFβ) (Pilbeam et al. 1997), basic fibroblast growth factor (FGF-2) (Kawaguchi et al. 1995), bone morphogenetic protein (BMP-2) (Chikazu et al. 2005), strontium (Choudhary et al. 2007), and fluid shear stress or mechanical loading (Klein-Nulend et al. 1997; Pavalko et al. 1998; Wadhwa et al. 2002). Serum is also a potent inducer of COX-2 expression and PGE2 production in cultured osteoblasts (Pilbeam et al. 1993). For some osteogenic factors, such as serum, BMP-2, and strontium ranelate, their ability to stimulate osteoblast differentiation in vitro is due largely to their induction of COX-2 produced PGs (Pilbeam et al. 1993; Chikazu et al. 2005; Choudhary et al. 2007).
Both EP2 and EP4 receptors have been positively implicated in the osteogenic and anabolic effects of PGE2 (Alander and Raisz 2006; Choudhary et al. 2008; Li et al. 2007), while mice deficient in EP1 receptors have enhanced fracture healing, higher trabecular bone volume, increased bone formation, and accelerated osteoblastic differentiation compared to WT mice (Zhang et al. 2011, 2015a). It has been difficult to study EP4 receptors in vivo because EP4 KO murine neonates in a pure C57Bl/6 background die shortly after birth due to patent ductus arteriosus (Segi et al. 1998). Reduced bone mass and impaired fracture healing were found in aged EP4 receptor KO mice compared to WT mice (Li et al. 2005) in contrast to another study which did not find any difference in bone formation between aged WT and EP4 KO mice (Gao et al. 2009). Both of these studies were done in mice with mixed backgrounds to circumvent the patent ductus arteriosus problem, and the difference in phenotypes might be due to variability in backgrounds.
Agonists of EP2 and EP4 can increase fracture healing in animals. Local application of an EP2 agonist and local and systemic application of EP4 agonists have been shown to accelerate bone repair (Li et al. 2003; Paralkar et al. 2003; Tanaka et al. 2004; Yoshida et al. 2002). Clinical studies have not been done with these agonists, perhaps because increased PG can have adverse effects (Markovic et al. 2017).
5 Skeletal Phenotypes of Mice with COX-2 Deficiency
Disruption of genes for PG production has given us some indications of the role of endogenous PGs in vivo. It was clear in early studies that COX-1 KO mice were healthy and survived normally, while COX-2 KO mice had more profound effects (Dinchuk et al. 1995; Langenbach et al. 1995, 1999; Morham et al. 1995). However, one study reported 35% of neonatal COX-2 KO mice died with a patent ductus arteriosus and the mortality increased to 100% when both genes for COX-1 were inactivated, indicating the dependence of COX-2 effects on levels of COX-1 expression (Loftin et al. 2001). Other studies found 20% of COX-2 KO mice dying between 7 and 23 weeks of age secondary to renal dysplasia, despite normal renal development at birth (Morham et al. 1995; Norwood et al. 2000). COX-2 KO female mice were infertile, with multiple failures in female reproductive processes, including ovulation, fertilization, and implantation (Lim et al. 1997). Initial studies of skeletal phenotypes in the C57Bl/6,129 background also reported early death in COX-2 KO mice, gave variable phenotypic results, and suggested that older COX-2 KO mice might have primary hyperparathyroidism (HPTH) (Alam et al. 2005; Xu et al. 2005; Robertson et al. 2006).
Effects of Background Strain
Mice for all these initial studies were in the C57Bl/6 inbred strain or mixed C57Bl/6 and 129 inbred strains. Both C57Bl/6 and 129sv mice have been shown to have a natural mutation that results in lack of the gene for the serum phospholipase (GIIA sPLA2) that is important for releasing AA (Kennedy et al. 1995; MacPhee et al. 1995). Hence, COX-2 KOs in these backgrounds are really double KOs, and this may impair the ability of COX-1 to produce PGs and compensate for absent COX-2. The MC3T3-E1 osteoblastic cell line, commonly used to study osteoblastic cells in vitro, was derived from C57Bl/6 mice and may also lack GIIA PLA2.
Mice in the outbred strain, CD-1, were reported to be heterozygous for the GIIA sPLA2 mutation (Kennedy et al. 1995). We bred COX-2 KO mice into the CD-1 background and found that COX-2 KO mice had no increased mortality and no renal dysfunction and that COX-2 KO females were fertile (Xu et al. 2010). Despite being healthy, 5-month-old male COX-2 KO mice had twofold elevated serum PTH compared to WT mice. COX-2 KO mice also had increased serum markers of bone formation and resorption, decreased femoral BMD by DXA (dual-energy X-ray absorptiometry) and cortical bone thickness by μCT, and small but nonsignificant decreases in trabecular bone volume by μCT or dynamic histomorphometry. We concluded that this bone phenotype could be due to hyperparathyroidism, COX-2 deficiency, or both.
PGE2 and Sympathetic Activity
Recently it was reported that PGE2 secreted by osteoblastic cells activated EP4 in sensory nerves to increase bone formation by inhibiting sympathetic activity through the central nervous system (Chen et al. 2019). They found that EP4 KO targeted to sensory nerves or COX-2 KO targeted to mature osteoblasts in 3-month-old mice significantly reduced bone volume in adult mice. They postulate that low bone mineral density is sensed by osteoblasts, perhaps because of increased mechanical stresses and stimulated PGE2 production by osteoblasts. PGE2 then acts via EP4 on sensory nerves to downregulate sympathetic tone, which then leads osteoblast to increase bone formation. Because so many different genetically engineered mice were subjected to so many different protocols, it is difficult to assess reproducibility. If these results are confirmed, it would mean that targeted COX-2 KO in mature osteoblasts has a larger effect than global COX-2 KO on bone phenotype in mice. Part of the argument for doing this study was the skeletal effects in congenital disorders with insensitivity to pain, disorders caused by several mutations (Nahorski et al. 2015). However, it seems likely that most skeletal problems involving fractures and joint disorders in these patients initially arise from repeated injury due to the lack of pain sensitivity and not from bone loss (Zhang and Haga 2014; Phatarakijnirund et al. 2016; Kayani et al. 2017).
6 COX-2 and PTH: A Special Relationship
PTH is the major hormone responsible for maintenance of calcium homeostasis. It is a major stimulator of bone resorption, acting via a GPCR, which is highly expressed by osteoblast lineage cells and activates both Gαs and Gαq signaling pathways (Vilardaga et al. 2011; Mahon 2012). PTH stimulates bone resorption by increasing RANKL and decreasing osteoprotegerin (OPG) (Boyce and Xing 2008). When PTH is injected intermittently, bone formation is increased more than resorption resulting in bone gain. Intermittent PTH was the first anabolic agent approved for osteoporosis therapy in the USA (Potts and Gardella 2007; Augustine and Horwitz 2013).
Intermittent PTH
Both PTH and PGE2 stimulate cAMP signaling, and both can induce both resorption and formation. We hypothesized that PGE2 might mediate some of the anabolic effects of PTH but found instead that the anabolic effects of intermittent PTH were increased in COX-2 KO mice (Xu et al. 2010). This led us to consider that PGE2 might inhibit the osteogenic effects of PTH in vitro. We found that continuous PTH inhibited or had no effect on osteoblastic differentiation in WT marrow stromal cultures but stimulated osteoblastic differentiation in COX-2 KO cultures (Choudhary et al. 2013). The COX-2-dependent inhibition of the osteogenic effects of PTH was shown to be due to a factor secreted by the hematopoietic lineage (bone marrow macrophage) cells in the cultures in response to a combination of RANKL, from osteoblastic lineage cells, and PGE2, produced by either osteoblastic or hematopoietic lineage cells, acting via the EP4 receptor (Choudhary et al. 2013). We subsequently identified the COX-2-dependent secreted inhibitor in vitro as serum amyloid A3 (SAA3) (Choudhary et al. 2016) and showed that secreted SAA3 acted back on osteoblastic cells to inhibit PTH-stimulated cAMP signaling.
Continuous PTH
In contrast to intermittent PTH, continuous PTH infusion causes bone loss (Iida-Klein et al. 2005; Robling et al. 2011). It was generally thought that this difference was due to increased resorption when PTH was given continuously. We examined effects of continuous PTH infusion in COX-2 KO mice, which did not express SAA3 in bone marrow macrophage cells when stimulated by PTH-induced RANKL, and in SAA3 KO mice, which have a normal COX-2 response to PTH (Choudhary et al. 2015, 2018). Continuous PTH increased bone formation in both COX-2 KO mice and SAA3 KO mice but suppressed bone formation in WT mice. There was no effect of COX-2 KO or SAA3 KO on PTH-stimulated bone resorption. Because the PTH stimulated increase in bone formation was greater than the PTH stimulated increase in bone resorption, continuous PTH was anabolic in both COX-2 KO and SAA3 KO mice. Hence, our data suggest that the effects of continuous PTH on bone are due to the PGE2-dependent secretion of SAA3, which suppresses bone formation, and not due to increased bone resorption. Our working hypothesis is shown in Fig. 3.
Role of PGE2-dependent SAA3 in blocking the osteoblastic response to continuous PTH. (1) PTH acts on osteoblastic precursors to induce cAMP, which causes them to differentiate into mature, bone-forming osteoblasts. PTH also induces COX-2/PGE2 and RANKL. (2) RANKL acts on bone marrow macrophages (BMMs) to induce them to become osteoclast precursors. RANKL also induces COX-2/PGE2. RANKL combined with PGE2 causes the osteoclastic precursors to produce and secrete SAA3. (3) SAA3 acts on the osteoblastic cells to block PTH-stimulated cAMP and suppress osteoblastic differentiation
7 Effects of NSAIDS on Bone
Early studies in animals suggested that NSAIDs impaired fracture healing (Einhorn 2003; Brown et al. 2004; Simon and O’Connor 2007). However, other studies proposed that the effects of NSAIDs on fracture healing were dose and duration dependent and reversible after discontinuation of brief treatment (Gerstenfeld et al. 2007). Recent reviews of animal studies indicate that loss of COX-2 activity primarily affects fracture healing via callus chondrogenesis or endochondral ossification (Geusens et al. 2013; O’Connor et al. 2014; Janssen et al. 2017). Recent reviews of fracture healing in humans conclude that short-term use of NSAIDs does not impair fracture healing (Kurmis et al. 2012; Marquez-Lara et al. 2016; Pountos et al. 2012) or spinal fusion surgery (Sivaganesan et al. 2017). On the other hand, 6 weeks of indomethacin increased risk for non-union after acetabular fracture surgery (Sagi et al. 2014), and chronic use of NSAIDs increased risk for a second hip fracture after hip fracture surgery (Huang et al. 2015). Hence, NSAIDs should probably be used at low dose and for a short duration in situations of bone repair.
It is difficult to obtain data in humans on the effects of NSAIDs on bone loss, given the wide range of NSAID dose, drug adherence, physical activity, inflammatory conditions, and considerable variability at an individual level in the degree of COX-2 inhibition and selectivity attained by selective COX-2 inhibitors (Fries et al. 2006). In a study of men age 65 and older, daily COX-2 inhibitor use in men was associated with lower hip and spine bone mineral density (BMD) compared to nonusers (Richards et al. 2006). In postmenopausal women not on estrogen replacement therapy, it was associated with a higher BMD. There was no effect of COX-2 inhibitor in women on estrogen replacement. A review of the literature on controlled randomized clinical trials with bone remodeling outcomes found some evidence for increased BMD and decreased rate of resorption and no evidence for increased bone formation in NSAID users, but the data were too limited for firm conclusions (Konstantinidis et al. 2013).
8 Summary
PGs are highly bioactive fatty acids, produced by most cells in the body and rapidly released and rapidly degraded. PGE2 is abundantly produced by both the mesenchymal lineage cells and the hematopoietic cell lineages, which give rise to the bone-forming osteoblasts and the bone-resorbing osteoclasts, respectively, as well as multiple other cells in the bone environment. The production of PGE2 in bone is highly regulated by multiple factors that induce COX-2. Cell and organ culture studies, as well as in vivo studies of animals given exogenous PGE2, have demonstrated that PGE2 can stimulate both bone resorption and bone formation. However, studies of mice with globally absent COX-2 have not shown a major skeletal phenotype. PGE2 acts at four G-protein-coupled receptors, EP1–4, with distinct signaling pathways. Many of the actions of PGE2 in bone have been attributed to increasing cAMP via the EP2 and EP4 receptors, and agonists of the EP2 and EP4 receptors have been investigated for their ability to stimulate bone formation and enhance fracture repair. Because COX-2 is induced by multiple hormones, growth factors, and proinflammatory factors, PGE2 may integrate, amplify, or actually mediate, the responses to these factors, a possibility that is often overlooked. Recent studies have shown that when PTH is given continuously, PTH-stimulated COX-2/PGE2 leads to the production of a factor that blocks the osteogenic effects of PTH in vitro and the anabolic effects of PTH in vivo.
As might be expected for a local factor with widespread production, regulated by many factors, and acting at multiple receptors, it has been difficult to define specific functions of PGE2 in bone as therapeutic targets. As the signaling pathways in bone are better characterized in physiologic and pathologic conditions, it may be possible to identify therapeutic applications of manipulating PGs in skeletal disorders.
References
Alam I, Warden SJ, Robling AG, Turner CH (2005) Mechanotransduction in bone does not require a functional cyclooxygenase-2 (COX-2) gene. J Bone Miner Res 20:438–446
Alander CB, Raisz LG (2006) Effects of selective prostaglandin E2 receptor agonists on cultured calvarial murine osteoblastic cells. Prostaglandins Other Lipid Mediat 81:178–183
Antczak MI, Zhang Y, Wang C, Doran J, Naidoo J, Voruganti S, Williams NS, Markowitz SD, Ready JM (2017) Inhibitors of 15-prostaglandin dehydrogenase to potentiate tissue repair. J Med Chem 60:3979–4001
Augustine M, Horwitz MJ (2013) Parathyroid hormone and parathyroid hormone-related protein analogs as therapies for osteoporosis. Curr Osteoporos Rep 11:400–406
Blackwell KA, Raisz LG, Pilbeam CC (2010) Prostaglandins in bone: good cop? bad cop? Trends Endocrinol Metab 21:294–301
Boyce BF, Xing L (2008) Functions of RANKL/RANK/OPG in bone modeling and remodeling. Arch Biochem Biophys 473:139–146
Brown KM, Saunders MM, Kirsch T, Donahue HJ, Reid JS (2004) Effect of COX-2-specific inhibition on fracture-healing in the rat femur. J Bone Joint Surg Am 86-A:116–123
Buchanan FG, DuBois RN (2006) Connecting COX-2 and Wnt in cancer. Cancer Cell 9:6–8
Buczynski MW, Dumlao DS, Dennis EA (2009) Thematic review series: proteomics. An integrated omics analysis of eicosanoid biology. J Lipid Res 50:1015–1038
Castellone MD, Teramoto H, Gutkind JS (2006) Cyclooxygenase-2 and colorectal cancer chemoprevention: the beta-catenin connection. Cancer Res 66:11085–11088
Chen H, Hu B, Lv X, Zhu S, Zhen G, Wan M, Jain A, Gao B, Chai Y, Yang M, Wang X, Deng R, Wang L, Cao Y, Ni S, Liu S, Yuan W, Chen H, Dong X, Guan Y, Yang H, Cao X (2019) Prostaglandin E2 mediates sensory nerve regulation of bone homeostasis. Nat Commun 10:181
Chikazu D, Li X, Kawaguchi H, Sakuma Y, Voznesensky OS, Adams DJ, Xu M, Hoshi K, Katavic V, Herschman HR, Raisz LG, Pilbeam CC (2005) Bone morphogenetic protein 2 induces cyclooxygenase 2 in osteoblasts via a Cbfa1 binding site: role in effects of bone morphogenetic protein 2 in vitro and in vivo. 2002. J Bone Miner Res 20:1888–1898
Choudhary S, Wadhwa S, Raisz LG, Alander C, Pilbeam CC (2003) Extracellular calcium is a potent inducer of cyclooxygenase-2 in murine osteoblasts through an ERK signaling pathway. J Bone Miner Res 18:1813–1824
Choudhary S, Halbout P, Alander C, Raisz L, Pilbeam C (2007) Strontium ranelate promotes osteoblastic differentiation and mineralization of murine bone marrow stromal cells: involvement of prostaglandins. J Bone Miner Res 22:1002–1010
Choudhary S, Alander C, Zhan P, Gao Q, Pilbeam C, Raisz L (2008) Effect of deletion of the prostaglandin EP2 receptor on the anabolic response to prostaglandin E2 and a selective EP2 receptor agonist. Prostaglandins Other Lipid Mediat 86:35–40
Choudhary S, Blackwell K, Voznesensky O, Deb RA, Pilbeam C (2013) Prostaglandin E2 acts via bone marrow macrophages to block PTH-stimulated osteoblast differentiation in vitro. Bone 56:31–41
Choudhary S, Canalis E, Estus T, Adams D, Pilbeam C (2015) Cyclooxygenase-2 suppresses the anabolic response to PTH infusion in mice. PLoS One 10:e0120164
Choudhary S, Goetjen A, Estus T, Jacome-Galarza CE, Aguila HL, Lorenzo J, Pilbeam C (2016) Serum amyloid A3 secreted by preosteoclasts inhibits parathyroid hormone-stimulated cAMP signaling in murine osteoblasts. J Biol Chem 291:3882–3894
Choudhary S, Santone E, Yee S-P, Lorenzo J, Adams DJ, Goetjen A, McCarthy MB, Mazzocca A, Pilbeam C (2018) Continuous PTH in mice causes bone loss because it induces serum amyloid A (SAA). Endocrinology 159:2759–2776
Dennis EA, Norris PC (2015) Eicosanoid storm in infection and inflammation. Nat Rev Immunol 15:511–523
Dennis EA, Cao J, Hsu YH, Magrioti V, Kokotos G (2011) Phospholipase A2 enzymes: physical structure, biological function, disease implication, chemical inhibition, and therapeutic intervention. Chem Rev 111:6130–6185
Desai A, Zhang Y, Park Y, Dawson DM, Larusch GA, Kasturi L, Wald D, Ready JM, Gerson SL, Markowitz SD (2018) A second-generation 15-PGDH inhibitor promotes bone marrow transplant recovery independent of age, transplant dose, and G-CSF support. Haematologica 103:1054–1064
Dinchuk JE, Car BD, Focht RJ, Johnston JJ, Jaffee BD, Covington MB, Contel NR, Eng VM, Collins RJ, Czerniak PM (1995) Renal abnormalities and an altered inflammatory response in mice lacking cyclooxygenase II. Nature 378:406–409
Einhorn TA (2003) Cox-2: where are we in 2003? the role of cyclooxygenase-2 in bone repair. Arthritis Res Ther 5:5–7
Estus TL, Choudhary S, Pilbeam CC (2016) Prostaglandin-mediated inhibition of PTH-stimulated beta-catenin signaling in osteoblasts by bone marrow macrophages. Bone 85:123–130
Faye-Petersen OM, Johnson WH Jr, Carlo WA, Hedlund GL, Pacifico AD, Blair HC (1996) Prostaglandin E1-induced hyperostosis: clinicopathologic correlations and possible pathogenetic mechanisms. Pediatr Pathol Lab Med 16:489–507
Ferreira SH, Vane JR (1967) Prostaglandins: their disappearance from and release into the circulation. Nature 216:868–873
Flanagan AM, Chambers TJ (1992) Stimulation of bone nodule formation in vitro by prostaglandins E1 and E2. Endocrinology 130:443–448
Fries S, Grosser T, Price TS, Lawson JA, Kapoor S, DeMarco S, Pletcher MT, Wiltshire T, Fitzgerald GA (2006) Marked interindividual variability in the response to selective inhibitors of cyclooxygenase-2. Gastroenterology 130:55–64
Gao Q, Zhan P, Alander CB, Kream BE, Hao C, Breyer MD, Pilbeam CC, Raisz LG (2009) Effects of global or targeted deletion of the EP4 receptor on the response of osteoblasts to prostaglandin in vitro and on bone histomorphometry in aged mice. Bone 45:98–103
Gerstenfeld LC, Al-Ghawas M, Alkhiary YM, Cullinane DM, Krall EA, Fitch JL, Webb EG, Thiede MA, Einhorn TA (2007) Selective and nonselective cyclooxygenase-2 inhibitors and experimental fracture-healing. Reversibility of effects after short-term treatment. J Bone Joint Surg Am 89:114–125
Geusens P, Emans PJ, de Jong JJ, van den Bergh J (2013) NSAIDs and fracture healing. Curr Opin Rheumatol 25:524–531
Grosser T, Ricciotti E, FitzGerald GA (2017a) The cardiovascular pharmacology of nonsteroidal anti-inflammatory drugs. Trends Pharmacol Sci 38:733–748
Grosser T, Theken KN, FitzGerald GA (2017b) Cyclooxygenase inhibition: pain, inflammation, and the cardiovascular system. Clin Pharmacol Ther 102:611–622
Hara S (2017) Prostaglandin terminal synthases as novel therapeutic targets. Proc Jpn Acad Ser B Phys Biol Sci 93:703–723
Hara S, Kamei D, Sasaki Y, Tanemoto A, Nakatani Y, Murakami M (2010) Prostaglandin E synthases: understanding their pathophysiological roles through mouse genetic models. Biochimie 92:651–659
Herschman HR (1994) Regulation of prostaglandin synthase-1 and prostaglandin synthase-2. Cancer Metastasis Rev 13:241–256
Hino S, Tanji C, Nakayama KI, Kikuchi A (2005) Phosphorylation of beta-catenin by cyclic AMP-dependent protein kinase stabilizes beta-catenin through inhibition of its ubiquitination. Mol Cell Biol 25:9063–9072
Huang KC, Huang TW, Yang TY, Lee MS (2015) Chronic NSAIDs use increases the risk of a second hip fracture in patients after hip fracture surgery: evidence from a STROBE-compliant population-based study. Medicine (Baltimore) 94:e1566. https://doi.org/10.1097/MD.0000000000001566
Iida-Klein A, Lu SS, Kapadia R, Burkhart M, Moreno A, Dempster DW, Lindsay R (2005) Short-term continuous infusion of human parathyroid hormone 1-34 fragment is catabolic with decreased trabecular connectivity density accompanied by hypercalcemia in C57BL/J6 mice. J Endocrinol 186:549–557
Inoue H, Tanaka N, Uchiyama C (1995) Parathyroid hormone increases the number of tartrate-resistant acid phosphatase-positive cells through prostaglandin E2 synthesis in adherent cell culture of neonatal rat bones. Endocrinology 136:3648–3656
Janssen MP, Caron MM, van Rietbergen B, Surtel DA, van Rhijn LW, Welting TJ, Emans PJ (2017) Impairment of the chondrogenic phase of endochondral ossification in vivo by inhibition of cyclooxygenase-2. Eur Cell Mater 34:202–216
Jee WS, Ma YF (1997) The in vivo anabolic actions of prostaglandins in bone. Bone 21:297–304
Kang YJ, Mbonye UR, Delong CJ, Wada M, Smith WL (2007) Regulation of intracellular cyclooxygenase levels by gene transcription and protein degradation. Prog Lipid Res 46:108–125
Kawaguchi H, Raisz LG, Voznesensky OS, Alander CB, Hakeda Y, Pilbeam CC (1994) Regulation of the two prostaglandin G/H synthases by parathyroid hormone, interleukin-1, cortisol and prostaglandin E2 in cultured neonatal mouse calvariae. Endocrinology 135:1157–1164
Kawaguchi H, Pilbeam CC, Gronowicz G, Abreu C, Fletcher BS, Herschman HR, Raisz LG, Hurley MM (1995) Transcriptional induction of prostaglandin G/H synthase-2 by basic fibroblast growth factor. J Clin Invest 96:923–930
Kayani B, Sewell MD, Platinum J, Olivier A, Briggs TWR, Eastwood DM (2017) Orthopaedic manifestations of congenital indifference to pain with anhidrosis (hereditary sensory and autonomic neuropathy type IV). Eur J Paediatr Neurol 21:318–326
Kennedy BP, Payette P, Mudgett J, Vadas P, Pruzanski W, Kwan M, Tang C, Rancourt DE, Cromlish WA (1995) A natural disruption of the secretory group II phospholipase A2 gene in inbred mouse strains. J Biol Chem 270:22378–22385
Kirkby NS, Chan MV, Zaiss AK, Garcia-Vaz E, Jiao J, Berglund LM, Verdu EF, Ahmetaj-Shala B, Wallace JL, Herschman HR, Gomez MF, Mitchell JA (2016) Systematic study of constitutive cyclooxygenase-2 expression: role of NF-kappaB and NFAT transcriptional pathways. Proc Natl Acad Sci U S A 113:434–439
Klein DC, Raisz LG (1970) Prostaglandins: stimulation of bone resorption in tissue culture. Endocrinology 86:1436–1440
Klein-Nulend J, Burger EH, Semeins CM, Raisz LG, Pilbeam CC (1997) Pulsating fluid flow stimulates prostaglandin release and inducible prostaglandin G/H synthase mRNA expression in primary mouse bone cells. J Bone Miner Res 12:45–51
Konstantinidis I, Papageorgiou SN, Kyrgidis A, Tzellos TG, Kouvelas D (2013) Effect of non-steroidal anti-inflammatory drugs on bone turnover: an evidence-based review. Rev Recent Clin Trials 8:48–60
Kujubu DA, Fletcher BS, Varnum BC, Lim RW, Herschman HR (1991) TIS10, a phorbol ester tumor promoter-inducible mRNA from Swiss 3T3 cells, encodes a novel prostaglandin synthase/cyclooxygenase homologue. J Biol Chem 266:12866–12872
Kurmis AP, Kurmis TP, O’Brien JX, Dalen T (2012) The effect of nonsteroidal anti-inflammatory drug administration on acute phase fracture-healing: a review. J Bone Joint Surg Am 94:815–823
Lader CS, Flanagan AM (1998) Prostaglandin E2, interleukin 1alpha, and tumor necrosis factor-alpha increase human osteoclast formation and bone resorption in vitro. Endocrinology 139:3157–3164
Langenbach R, Morham SG, Tiano HF, Loftin CD, Ghanayem BI, Chulada PC, Mahler JF, Lee CA, Goulding EH, Kluckman KD (1995) Prostaglandin synthase 1 gene disruption in mice reduces arachidonic acid-induced inflammation and indomethacin-induced gastric ulceration. Cell 83:483–492
Langenbach R, Loftin C, Lee C, Tiano H (1999) Cyclooxygenase knockout mice: models for elucidating isoform-specific functions. Biochem Pharmacol 58:1237–1246
Leslie CC (2015) Cytosolic phospholipase A(2): physiological function and role in disease. J Lipid Res 56:1386–1402
Li J, Sarosi I, Yan XQ, Morony S, Capparelli C, Tan HL, McCabe S, Elliott R, Scully S, Van G, Kaufman S, Juan SC, Sun Y, Tarpley J, Martin L, Christensen K, McCabe J, Kostenuik P, Hsu H, Fletcher F, Dunstan CR, Lacey DL, Boyle WJ (2000) RANK is the intrinsic hematopoietic cell surface receptor that controls osteoclastogenesis and regulation of bone mass and calcium metabolism. Proc Natl Acad Sci U S A 97:1566–1571
Li M, Ke HZ, Qi H, Healy DR, Li Y, Crawford DT, Paralkar VM, Owen TA, Cameron KO, Lefker BA, Brown TA, Thompson DD (2003) A novel, non-prostanoid EP2 receptor-selective prostaglandin E2 agonist stimulates local bone formation and enhances fracture healing. J Bone Miner Res 18:2033–2042
Li M, Healy DR, Li Y, Simmons HA, Crawford DT, Ke HZ, Pan LC, Brown TA, Thompson DD (2005) Osteopenia and impaired fracture healing in aged EP4 receptor knockout mice. Bone 37:46–54
Li M, Thompson DD, Paralkar VM (2007) Prostaglandin E(2) receptors in bone formation. Int Orthop 31:767–772
Lim H, Paria BC, Das SK, Dinchuk JE, Langenbach R, Trzaskos JM, Dey SK (1997) Multiple female reproductive failures in cyclooxygenase 2-deficient mice. Cell 91:197–208
Lin BY, Jee WSS, Ma YF, Ke HZ, Kimmel DB, Li XJ (1994) Effects of prostaglandin E2 and risedronate administration on cancellous bone in older female rats. Bone 15:489–496
Loftin CD, Trivedi DB, Tiano HF, Clark JA, Lee CA, Epstein JA, Morham SG, Breyer MD, Nguyen M, Hawkins BM, Goulet JL, Smithies O, Koller BH, Langenbach R (2001) Failure of ductus arteriosus closure and remodeling in neonatal mice deficient in cyclooxygenase-1 and cyclooxygenase-2. Proc Natl Acad Sci U S A 98:1059–1064
MacPhee M, Chepenik KP, Liddell RA, Nelson KK, Siracusa LD, Buchberg AM (1995) The secretory phospholipase A2 gene is a candidate for the Mom1 locus, a major modifier of ApcMin-induced intestinal neoplasia. Cell 81:957–966
Mahon MJ (2012) The parathyroid hormone receptorsome and the potential for therapeutic intervention. Curr Drug Targets 13:116–128
Markovic T, Jakopin Z, Dolenc MS, Mlinaric-Rascan I (2017) Structural features of subtype-selective EP receptor modulators. Drug Discov Today 22:57–71
Marquez-Lara A, Hutchinson ID, Nunez F Jr, Smith TL, Miller AN (2016) Nonsteroidal anti-inflammatory drugs and bone-healing: a systematic review of research quality. JBJS Rev. https://doi.org/10.2106/JBJS.RVW.O.00055
Mbonye UR, Wada M, Rieke CJ, Tang HY, DeWitt DL, Smith WL (2006) The 19-amino acid cassette of cyclooxygenase-2 mediates entry of the protein into the endoplasmic reticulum-associated degradation system. J Biol Chem 281:35770–35778
Min YK, Rao Y, Okada Y, Raisz LG, Pilbeam CC (1998) Regulation of prostaglandin G/H synthase-2 expression by interleukin-1 in human osteoblast-like cells. J Bone Miner Res 13:1066–1075
Miyaura C, Inada M, Suzawa T, Sugimoto Y, Ushikubi F, Ichikawa A, Narumiya S, Suda T (2000) Impaired bone resorption to prostaglandin E2 in prostaglandin E receptor EP4-knockout mice. J Biol Chem 275:19819–19823
Morham SG, Langenbach R, Loftin CD, Tiano HF, Vouloumanos N, Jennette JC, Mahler JF, Kluckman KD, Ledford A, Lee CA (1995) Prostaglandin synthase 2 gene disruption causes severe renal pathology in the mouse. Cell 83:473–482
Murakami M, Taketomi Y, Miki Y, Sato H, Hirabayashi T, Yamamoto K (2011) Recent progress in phospholipase A(2) research: from cells to animals to humans. Prog Lipid Res 50:152–192
Murakami M, Sato H, Miki Y, Yamamoto K, Taketomi Y (2015) A new era of secreted phospholipase A(2). J Lipid Res 56:1248–1261
Nahorski MS, Chen YC, Woods CG (2015) New Mendelian disorders of painlessness. Trends Neurosci 38:712–724
Norrdin RW, Shih MS (1988) Systemic effects of prostaglandin E2 on vertebral trabecular remodeling in beagles used in a healing study. Calcif Tissue Int 42:363–368
Norwood VF, Morham SG, Smithies O (2000) Postnatal development and progression of renal dysplasia in cyclooxygenase-2 null mice. Kidney Int 58:2291–2300
O’Banion MK, Sadowski HB, Winn V, Young DA (1991) A serum- and glucorticoid-regulated 4-kilobase mRNA encodes a cyclooxygenase-related protein. J Biol Chem 266:23261–23267
O’Callaghan G, Houston A (2015) Prostaglandin E2 and the EP receptors in malignancy: possible therapeutic targets? Br J Pharmacol 172:5239–5250
O’Connor JP, Manigrasso MB, Kim BD, Subramanian S (2014) Fracture healing and lipid mediators. Bonekey Rep 3:517. https://doi.org/10.1038/bonekey.2014.12
Okada Y, Lorenzo JA, Freeman AM, Tomita M, Morham SG, Raisz LG, Pilbeam CC (2000a) Prostaglandin G/H synthase-2 is required for maximal formation of osteoclast-like cells in culture. J Clin Invest 105:823–832
Okada Y, Tomita M, Gronowicz G, Kawaguchi H, Sohn J, Tanaka Y, Morimoto I, Nakamura T, Raisz L, Pilbeam C (2000b) Effects of cyclooxygenase-2 gene disruption on osteoblastic function. J Bone Miner Res 15:S217
Paralkar VM, Borovecki F, Ke HZ, Cameron KO, Lefker B, Grasser WA, Owen TA, Li M, Silva-Jardine P, Zhou M, Dunn RL, Dumont F, Korsmeyer R, Krasney P, Brown TA, Plowchalk D, Vukicevic S, Thompson DD (2003) An EP2 receptor-selective prostaglandin E2 agonist induces bone healing. Proc Natl Acad Sci U S A 100:6736–6740
Pavalko FM, Chen NX, Turner CH, Burr DB, Atkinson S, Hsieh YF, Qiu J, Duncan RL (1998) Fluid shear-induced mechanical signaling in MC3T3-E1 osteoblasts requires cytoskeleton-integrin interactions. Am J Physiol 275:C1591–C1601
Phatarakijnirund V, Mumm S, McAlister WH, Novack DV, Wenkert D, Clements KL, Whyte MP (2016) Congenital insensitivity to pain: fracturing without apparent skeletal pathobiology caused by an autosomal dominant, second mutation in SCN11A encoding voltage-gated sodium channel 1.9. Bone 84:289–298
Pilbeam CC, Kawaguchi H, Hakeda Y, Voznesensky O, Alander CB, Raisz LG (1993) Differential regulation of inducible and constitutive prostaglandin endoperoxide synthase in osteoblastic MC3T3-E1 cells. J Biol Chem 268:25643–25649
Pilbeam CC, Raisz LG, Voznesensky O, Alander CB, Delman BN, Kawaguchi K (1994) Autoregulation of inducible prostaglandin G/H synthase in osteoblastic cells by prostaglandins. J Bone Miner Res 10:406–414
Pilbeam C, Rao Y, Voznesensky O, Kawaguchi H, Alander C, Raisz LG, Herschman H (1997) Transforming growth factor-β1 regulation of prostaglandin G/H syntase-2 expression in osteoblastic MC3T3-E1 cells. Endocrinology 138:4672–4682
Pilbeam CC, Choudhary S, Blackwell KA, Raisz LG (2008) Prostaglandins and bone metabolism. In: Bilezikian JP, Raisz LG, Martn TJ (eds) Principles of bone biology, 3rd edn. Elsevier/Academic Press, San Diego
Potts JT, Gardella TJ (2007) Progress, paradox, and potential: parathyroid hormone research over five decades. Ann N Y Acad Sci 1117:196–208
Pountos I, Georgouli T, Calori GM, Giannoudis PV (2012) Do nonsteroidal anti-inflammatory drugs affect bone healing? A critical analysis. ScientificWorldJournal 2012:606404. https://doi.org/10.1100/2012/606404
Psarra A, Nikolaou A, Kokotou MG, Limnios D, Kokotos G (2017) Microsomal prostaglandin E2 synthase-1 inhibitors: a patent review. Expert Opin Ther Pat 27:1047–1059
Raisz LG, Woodiel FN (2003) Effects of selective prostaglandin EP2 and EP4 receptor agonists on bone resorption and formation in fetal rat organ cultures. Prostaglandins Other Lipid Mediat 71:287–292
Richards JB, Joseph L, Schwartzman K, Kreiger N, Tenenhouse A, Goltzman D (2006) The effect of cyclooxygenase-2 inhibitors on bone mineral density: results from the Canadian Multicentre Osteoporosis Study. Osteoporos Int 17:1410–1419
Robertson G, Xie C, Chen D, Awad H, Schwarz EM, O’Keefe RJ, Guldberg RE, Zhang X (2006) Alteration of femoral bone morphology and density in COX-2-/- mice. Bone 39:767–772
Robling AG, Kedlaya R, Ellis SN, Childress PJ, Bidwell JP, Bellido T, Turner CH (2011) Anabolic and catabolic regimens of human parathyroid hormone 1-34 elicit bone- and envelope-specific attenuation of skeletal effects in Sost-deficient mice. Endocrinology 152:2963–2975
Sagi HC, Jordan CJ, Barei DP, Serrano-Riera R, Steverson B (2014) Indomethacin prophylaxis for heterotopic ossification after acetabular fracture surgery increases the risk for nonunion of the posterior wall. J Orthop Trauma 28:377–383
Sato T, Morita I, Sakaguchi K, Nakahama KI, Smith WL, DeWitt DL, Murota SI (1996) Involvement of prostaglandin endoperoxide H synthase-2 in osteoclast-like cell formation induced by interleukin-1 beta. J Bone Miner Res 11:392–400
Segi E, Sugimoto Y, Yamasaki A, Aze Y, Oida H, Nishimura T, Murata T, Matsuoka T, Ushikubi F, Hirose M, Tanaka T, Yoshida N, Narumiya S, Ichikawa A (1998) Patent ductus arteriosus and neonatal death in prostaglandin receptor EP4-deficient mice. Biochem Biophys Res Commun 246:7–12
Shao J, Jung C, Liu C, Sheng H (2005) Prostaglandin E2 stimulates the beta-catenin/T cell factor-dependent transcription in colon cancer. J Biol Chem 280:26565–26572
Simmons DL, Botting RM, Hla T (2004) Cyclooxygenase isozymes: the biology of prostaglandin synthesis and inhibition. Pharmacol Rev 56:387–437
Simon AM, O’Connor JP (2007) Dose and time-dependent effects of cyclooxygenase-2 inhibition on fracture-healing. J Bone Joint Surg Am 89:500–511
Sivaganesan A, Chotai S, White-Dzuro G, McGirt MJ, Devin CJ (2017) The effect of NSAIDs on spinal fusion: a cross-disciplinary review of biochemical, animal, and human studies. Eur Spine J 26:2719–2728
Smith WL, Langenbach R (2001) Why there are two cyclooxygenase isozymes. J Clin Invest 107:1491–1495
Smith WL, DeWitt DL, Garavito RM (2000) Cyclooxygenases: structural, cellular, and molecular biology. Annu Rev Biochem 69:145–182
Smith WL, Urade Y, Jakobsson PJ (2011) Enzymes of the cyclooxygenase pathways of prostanoid biosynthesis. Chem Rev 111:5821–5865
Sugimoto Y, Narumiya S (2007) Prostaglandin E receptors. J Biol Chem 282:11613–11617
Suponitzky I, Weinreb M (1998) Differential effects of systemic prostaglandin E2 on bone mass in rat long bones and calvariae. J Endocrinol 156:51–57
Suzawa T, Miyaura C, Inada M, Maruyama T, Sugimoto Y, Ushikubi F, Ichikawa A, Narumiya S, Suda T (2000) The role of prostaglandin E receptor subtypes (EP1, EP2, EP3, and EP4) in bone resorption: an analysis using specific agonists for the respective EPs. Endocrinology 141:1554–1559
Swinney DC, Mak AY, Barnett J, Ramesha CS (1997) Differential allosteric regulation of prostaglandin H synthase 1 and 2 by arachidonic acid. J Biol Chem 272:12393–12398
Tai H, Miyaura C, Pilbeam CC, Tamura T, Ohsugi Y, Koishihara Y, Kubodera N, Kawaguchi H, Raisz LG, Suda T (1997) Transcriptional induction of cyclooxygenase-2 in osteoblasts is involved in interleukin-6-induced osteoclast formation. Endocrinology 138:2372–2379
Tanaka M, Sakai A, Uchida S, Tanaka S, Nagashima M, Katayama T, Yamaguchi K, Nakamura T (2004) Prostaglandin E2 receptor (EP4) selective agonist (ONO-4819.CD) accelerates bone repair of femoral cortex after drill-hole injury associated with local upregulation of bone turnover in mature rats. Bone 34:940–948
Tang CH, Yang RS, Fu WM (2005) Prostaglandin E2 stimulates fibronectin expression through EP1 receptor, phospholipase C, protein kinase Calpha, and c-Src pathway in primary cultured rat osteoblasts. J Biol Chem 280:22907–22916
Tanioka T, Nakatani Y, Semmyo N, Murakami M, Kudo I (2000) Molecular identification of cytosolic prostaglandin E2 synthase that is functionally coupled with cyclooxygenase-1 in immediate prostaglandin E2 biosynthesis. J Biol Chem 275:32775–32782
Ueda K, Saito A, Nakano H, Aoshima M, Yokota M, Muraoka R, Iwaya T (1980) Cortical hyperostosis following long-term administration of prostaglandin E1 in infants with cyanotic congenital heart disease. J Pediatr 97:834–836
Uppal S, Diggle CP, Carr IM, Fishwick CW, Ahmed M, Ibrahim GH, Helliwell PS, Latos-Bielenska A, Phillips SE, Markham AF, Bennett CP, Bonthron DT (2008) Mutations in 15-hydroxyprostaglandin dehydrogenase cause primary hypertrophic osteoarthropathy. Nat Genet 40:789–793
Vasquez AM, Mouchlis VD, Dennis EA (2017) Review of four major distinct types of human phospholipase A2. Adv Biol Regul 10. https://doi.org/10.1016/j.jbior.2017.10.009
Vilardaga JP, Romero G, Friedman PA, Gardella TJ (2011) Molecular basis of parathyroid hormone receptor signaling and trafficking: a family B GPCR paradigm. Cell Mol Life Sci 68:1–13
Wadhwa S, Choudhary S, Voznesensky M, Epstein M, Raisz L, Pilbeam C (2002) Fluid flow induces COX-2 expression in MC3T3-E1 osteoblasts via a PKA signaling pathway. Biochem Biophys Res Commun 297:46–51
Woodward DF, Jones RL, Narumiya S (2011) International Union of Basic and Clinical Pharmacology. LXXXIII: classification of prostanoid receptors, updating 15 years of progress. Pharmacol Rev 63:471–538
Xie WL, Chipman JG, Robertson DL, Erikson RL, Simmons DL (1991) Expression of a mitogen-responsive gene encoding prostaglandin synthase is regulated by mRNA splicing. Proc Natl Acad Sci U S A 88:2692–2696
Xu M, Choudhary S, Goltzman D, Ledgard F, Adams D, Gronowicz G, Koczon-Jaremko B, Raisz L, Pilbeam C (2005) Do cyclooxygenase knockout mice have primary hyperparathyroidism? Endocrinology 146:1843–1853
Xu Z, Choudhary S, Okada Y, Voznesensky O, Alander C, Raisz L, Pilbeam C (2007) Cyclooxygenase-2 gene disruption promotes proliferation of murine calvarial osteoblasts in vitro. Bone 41:68–76
Xu M, Choudhary S, Voznesensky O, Gao Q, Adams D, Diaz-Doran V, Wu Q, Goltzman D, Raisz LG, Pilbeam CC (2010) Basal bone phenotype and increased anabolic responses to intermittent parathyroid hormone in healthy male COX-2 knockout mice. Bone 47:341–352
Yoshida K, Oida H, Kobayashi T, Maruyama T, Tanaka M, Katayama T, Yamaguchi K, Segi E, Tsuboyama T, Matsushita M, Ito K, Ito Y, Sugimoto Y, Ushikubi F, Ohuchida S, Kondo K, Nakamura T, Narumiya S (2002) Stimulation of bone formation and prevention of bone loss by prostaglandin E EP4 receptor activation. Proc Natl Acad Sci U S A 99:4580–4585
Yuan C, Smith WL (2015) A cyclooxygenase-2-dependent prostaglandin E2 biosynthetic system in the Golgi apparatus. J Biol Chem 290:5606–5620
Zhan P, Alander C, Kaneko H, Pilbeam CC, Guan Y, Zhang Y, Breyer MD, Raisz LG (2005) Effect of deletion of the prostaglandin EP4 receptor on stimulation of calcium release from cultured mouse calvariae: impaired responsiveness in heterozygotes. Prostaglandins Other Lipid Mediat 78:19–26
Zhang Y, Haga N (2014) Skeletal complications in congenital insensitivity to pain with anhidrosis: a case series of 14 patients and review of articles published in Japanese. J Orthop Sci 19:827–831
Zhang X, Schwarz EM, Young DA, Puzas JE, Rosier RN, O’Keefe RJ (2002) Cyclooxygenase-2 regulates mesenchymal cell differentiation into the osteoblast lineage and is critically involved in bone repair. J Clin Invest 109:1405–1415
Zhang M, Ho HC, Sheu TJ, Breyer MD, Flick LM, Jonason JH, Awad HA, Schwarz EM, O’Keefe RJ (2011) EP1(−/−) mice have enhanced osteoblast differentiation and accelerated fracture repair. J Bone Miner Res 26:792–802
Zhang M, Feigenson M, Sheu TJ, Awad HA, Schwarz EM, Jonason JH, Loiselle AE, O’Keefe RJ (2015a) Loss of the PGE2 receptor EP1 enhances bone acquisition, which protects against age and ovariectomy-induced impairments in bone strength. Bone 72:92–100
Zhang Y, Desai A, Yang SY, Bae KB, Antczak MI, Fink SP, Tiwari S, Willis JE, Williams NS, Dawson DM, Wald D, Chen WD, Wang Z, Kasturi L, Larusch GA, He L, Cominelli F, Di ML, Djuric Z, Milne GL, Chance M, Sanabria J, Dealwis C, Mikkola D, Naidoo J, Wei S, Tai HH, Gerson SL, Ready JM, Posner B, Willson JK, Markowitz SD (2015b) Inhibition of the prostaglandin-degrading enzyme 15-PGDH potentiates tissue regeneration. Science 348:aaa2340
Acknowledgments
This effort was supported by National Institute of Health Grants NIAMS award AR060286.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2019 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Pilbeam, C. (2019). Prostaglandins and Bone. In: Stern, P.H. (eds) Bone Regulators and Osteoporosis Therapy. Handbook of Experimental Pharmacology, vol 262. Springer, Cham. https://doi.org/10.1007/164_2019_332
Download citation
DOI: https://doi.org/10.1007/164_2019_332
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-57377-5
Online ISBN: 978-3-030-57378-2
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)